Authors: Katherine Stolper, DO (EM Resident at SAUSHEC, USA) and Brit Long, MD (@long_brit, EM Chief Resident at SAUSHEC, USAF) // Edited by: Jennifer Robertson, MD, MSEd and Alex Koyfman, MD (@EMHighAK, EM Attending Physician, UTSW / Parkland Memorial Hospital)
Case Presentation
You are working in the emergency department (ED) when you overhear the emergency medical services (EMS) report of an incoming 89 yo female with chief complaint of “fall from standing” with no apparent injuries. She is presenting to your ED as a trauma resuscitation secondary to a brief episode of unresponsiveness in the ambulance. Her unresponsiveness resolved with four chest compressions.
Upon arrival, she has a Glasgow Coma Scale (GCS) of 15 with her airway, breathing and circulation intact. Her initial vital signs are heart rate (HR) 56, blood pressure (BP) 176/72, respiratory rate (RR) 20, oxygen saturation 97% on room air (RA), temperature 98.1°F, and glucose of 89.
The primary and secondary surveys are unremarkable. However, while the patient is waiting for a computed tomography (CT) scan, her monitor demonstrates several seconds of asystole. She becomes unresponsive but has rapid return of circulation after a sternal rub.
The electrocardiogram (ECG) above shows a third degree (complete) atrioventricular (AV) block. This article will review third degree AV blocks and their management.
THIRD DEGREE OR COMPLETE ATRIOVENTRICULAR (AV) BLOCK:
Complete AV block is a complete dissociation between the atria and the ventricles. This means that the electrical impulses generated in the atria do not propagate to the ventricles. An ECG will show P waves and QRS complexes that are independent of each other, as seen in the ECG. Since none of the atrial impulses are propagating, you will see an escape rhythm that is either junctional (rate 40-60 beats per minute (bpm) or ventricular (rate 20-40 bpm) depending on the level of the block. Of note, junctional escape rhythms tend to be more stable than ventricular escape rhythms. The etiologies of complete heart block include both reversible and irreversible causes but the most common cause is coronary ischemia.
| Reversible Causes | Irreversible Causes |
| -Medications: Calcium channel blockers, Beta blockers, Amiodarone, Adenosine, Digitalis | -Idiopathic degeneration of the conducting system – Lenegre’s or Lev’s disease |
| -Hyperkalemia | -Congenital – maternal lupus |
| -Inferior Myocardial Infarction | -Amyloidosis/Sarcoidosis |
| -Increased vagal tone | -Lyme disease |
| -Hypothyroidism | -Structural defect: Myocardial infarction (anterior), heart failure |
| -Heart valve surgeries |
Is atropine indicated in bradycardic patients with complete heart block?
According to the American Heart Association (AHA) Advanced Cardiac Life Support (ACLS) guidelines, atropine is indicated as a first line agent for patients with unstable bradycardia. It works by inhibiting vagal stimulation. Atropine is given as 0.5mg intravenously (IV) every 3-5 minutes with a maximum dose of 3 mg. Atropine administration, however, should not interfere with cardiac pacing. If there is a favorable response to atropine, the conduction abnormality is likely in the AV node. However, if the escape rhythm is originating at or below the bundle of His, there is unlikely to be a response to atropine as the more distal conducting system is not as sensitive to vagal stimulation. [1,2]
Response to atropine can be predicted by looking at the QRS morphology on a 12 lead ECG. If the AV block occurs in the AV node or the Bundle of His, the escape rhythm will have a narrow QRS and will likely respond to atropine. Conversely, if the AV block occurs below the bundle of His, the escape rhythm results in a sub-junctional escape rhythm which has a wide QRS and is unlikely to respond to atropine [3].
NOTE: Because atropine can increase cardiac demand, it is contraindicated in patients with complete heart block secondary to myocardial infarction or ischemia.
Titrating to patient response, epinephrine (2-10 mcg/min) or dopamine (2-10 mcg/kg/min) should be considered while waiting for a pacemaker or if pacing is ineffective.
TEMPORARY CARDIAC PACING
The two types of temporary cardiac pacing that you will encounter in the ED are transcutaneous and transvenous. Temporary cardiac pacing is indicated for patients with symptomatic bradycardic dysrhythmias, most frequently due to AV nodal block. [7] Remember that bradycardia is not always due to primary cardiac issues such as sick sinus syndrome, atrioventricular block, or myocardial ischemia. Always consider secondary causes of bradycardia such as hyperkalemia, hypothyroidism, hypothermia, or overdose with beta-blockers, calcium channel blockers, digitalis, clonidine, or other antiarrhythmics.
Transcutaneous Pacing
Transcutaneous pacing is a great option for an unstable patient in whom central venous access has not been established yet for a transvenous pacemaker. Unfortunately, patient discomfort and high pacing thresholds are significant clinical barriers to transcutaneous pacing. Patient discomfort is secondary to skeletal muscle contraction, however, research shows that less electricity can be used due to the newer technology available with larger surface area pads. With the new technology, most patients can tolerate > 15 minutes of transcutaneous pacing [5]. However, in patients who cannot tolerate it, sedation and analgesia can be provided to mitigate any discomfort.
Procedure:
- Pad Placement and set up: Recommended pad placement for the best capture is anterior/posterior, as shown below. The positive pad is placed posteriorly to the left of the spine, beneath the left scapula. The negative pad is placed anteriorly between the xiphoid process and the left nipple.
Alternatively, the pads may both be placed anteriorly, with the negative electrode placed in the V6 position and the positive electrode to the right of the sternum, under the clavicle.
- Select Mode: Select the pacemaker button on the box and choose between fixed and demand modes. Fixed mode means that the pacemaker will fire at whatever rate you choose, regardless of the patient’s intrinsic rhythm. Demand mode will sense the patient’s intrinsic rhythm and pace only if needed. Most often you will start in fixed mode.
- NOTE: If in demand mode, the leads should be placed for continuous ECG so that the pacemaker can sense the patient’s intrinsic rate to pace accordingly (double set up). This prevents the “R on T” phenomenon.
- Set rate and output: The initial pacing rate should be set to 80 bpm with the current set to 30 milliamperes (mA). Beware that initially, pacemaker spikes may be visualized without resultant cardiac depolarization.
The current can be increased by 5-10 mA at a time until capture is seen as a definite QRS complex and T wave following each pacemaker spike. Once capture is achieved, check the patient’s pulse or correlate with the pulse oximeter to ensure that a perfusing rhythm is present.[8] Final output should be set to 5-10 mA above threshold level to ensure continued capture.
Human studies have shown that the average current necessary to achieve capture is between 65-100 mA in unstable bradycardias and about 50-70 mA in hemodynamically stable patients. [5]
Transvenous Pacing
There are no absolute contraindications to transvenous pacing. However, some relative contraindications to transvenous pacing include: patients with mild or rare intermittent symptoms with a stable escape rhythm, patients with prosthetic tricuspid valves, and patients with myocardial infarctions who are receiving thrombolytic agents or aggressive anti-platelet therapy.
NOTE: Also use caution in patients with digitalis toxicity as the myocardium is extremely sensitive to irritation from the transvenous wire and can cause the rhythm to degenerate into ventricular fibrillation.
Supplies:
- Venous sheath (6 French (Fr))
- Pacing wire/catheter
- Pacing generator
- Extension cable
- Sterile precautions
Procedure:
- Achieve Access: Insert a 6 Fr catheter. Note the internal diameter of the catheter sheath needs to match the external diameter of the pacemaker wire. Most balloon tip catheters are 5 Fr and will fit into a 6 Fr catheter. The ideal site selection for the venous catheter is the right internal jugular vein or the left subclavian vein, as these veins give you the most direct route to the right ventricle.
- Hook up your pacing generator: Put a fresh battery in the generator (usually a 9 volt (V) battery) and turn it on. There will be an extension cable with the connector terminals, and the pacing catheter with two electrode connectors at the end. The electrode connectors will need to be connected to the 2 terminals. The proximal (positive) electrode on the catheter plugs into the positive connector terminal and the distal (negative) electrode plugs into the negative connector terminal. You can remember this as “PP” for “Positive Proximal.” Finally, plug the extension cable into the top of the generator box.
Note: If you have a dual chamber pacemaker, make sure it is plugged into the ventricular port.
- Initial pacemaker settings: As shown above, there are three things that need to be set on your generator. These include rate, output, and sensitivity.
- Rate: Rate should be set above the patient’s native rate and above the rate of your transcutaneous pacemaker Set pacing at 80-100 bpm initially so it is easy to tell when capture is obtained, and then turn the rate down to approximately 60 bpm to avoid demand ischemia after capture has been confirmed.
- Output: This is the amount of current that is being sent to the heart and is measured in mA. This is initially set to the maximum which will usually be 20 mA. Note: If pacing is dual chamber, atrial output should be set to zero mA and ventricular output to maximum mA.
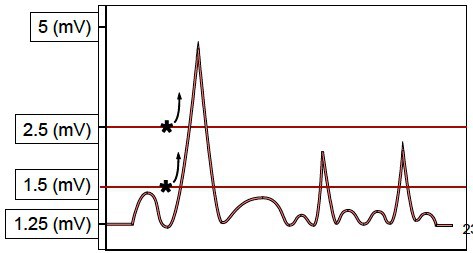
- Sensitivity This is the pacemaker’s ability to see the electrical activity coming from the heart as measured in millivolts (mV). The lower the sensitivity number, the more sensitive the pacemaker is at detecting intrinsic cardiac activity.

- Start with the sensitivity set to “asynchronous” which means the generator will fire at the set rate, no matter what the intrinsic activity of the heart is. This makes it easier to determine once capture occurs.Once you have capture, you can switch to synchronous (or demand) mode. This avoids the “R on T” phenomenon. To find the sensitivity threshold, turn down the rate below the patient’s intrinsic rate and start with the sensitivity dial on the lowest number. Dial up until the pacemaker fails to sense any activity and starts firing. The sensitivity threshold is usually more than 5 mV. The sensitivity setting should be half the sensitivity threshold, meaning the pacemaker should be twice as sensitive as the sensitivity threshold.
- Insert the pacing catheter and determine capture:
- Inflate the balloon once it is at least 20 cm inserted (to ensure it is past the end of the catheter), turn the stopcock to ensure the balloon stays inflated, and advance the wire. The balloon works like a sail to guide the wire into the right ventricle (RV). Make sure to use the 1.5 ml syringe that comes in the kit to avoid overinflating the balloon.
- Running IV fluids through the catheter while floating the wire can also help guide the balloon into the RV.
- Ideal placement of the catheter should be at a depth of approximately 40-45cm.
- Ultrasound guidance using either a parasternal long or subxiphoid view can be helpful to visualize the catheter tip in the RV.
- If you overshoot and need to pull back the wire, make sure the balloon is deflated to avoid tearing the tricuspid valve leaflets
- Once you achieve capture, pacemaker spikes will become apparent and will be soon followed by a widened QRS. This will have a similar appearance to a left bundle branch block as the electrode contacts the wall of the RV. Make sure you check a pulse to ensure that you have a perfusing rhythm. You can also use the pulse oximetry to correlate the QRS complexes with a pulse.
- Deflate the balloon, decrease the output until you lose capture then double the output, typically between 1-5 mA.
- Obtain a chest x-ray for placement confirmation.
PEARL: Defibrillation and cardioversion are safe in patients who have temporary pacemakers.
TROUBLESHOOTING A TRANSVENOUS PACEMAKER
- Failure to Pace/Output failure – The pacemaker does not produce a stimulus when it shuld. Check your wire connections and the battery in the pacemaker box. Check for breaks or kinks in the wires. To exclude other causes, turn the sensitivity to asynchronous and the output to maximum
Switch back to transcutaneous pacing until a new wire can be floated
.

2. Undersensing (risk of R on T) – The pacemaker fires with no regard for the patient’s intrinsic rhythm. Turn down the sensitivity. Remember the lower the number the more sensitive the pacemaker is.
3. Oversensing (risk of failure to pace) – the pacemaker thinks it detects an intrinsic QRS and inhibits itself from firing. This is common with skeletal muscle contraction from shivering or seizures or from a tall T wave. To solve this, turn up the sensitivity to make the pacemaker less sensitive. Also turn the pacemaker to asynchronous.

4. Failure to Capture – You will see pacemaker spikes with no associated QRS complex as in the figure below Turn up the current until you regain capture, check for electrolyte abnormalities, reposition the wire or roll the patient from one side to anothe, or try changing the polarity – which wire is in the positive and negative port.

References / Further Reading
- “ACLS Drugs for Bradycardia.” ACLS Algorithms. Web. Nov.-Dec. 2015
- Link, M. S., D. L. Atkins, R. S. Passman, et al. “Part 6: Electrical Therapies: Automated External Defibrillators, Defibrillation, Cardioversion, and Pacing * 2010 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care.” Circulation 122.18_suppl_3 (2010): S706-S719
- Saure, William, et. al. “Third degree (complete) atrioventricular block” UptoDate. Web 18 Nov 2015
- Neumar RW, Otto CW, Link MS, et al. Part 8: adult advanced cardiovascular life support: 2010 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation 2010; 122:S729.
- Boehm, Judy. “Tried and True: Noninvasive Cardiac Pacing.” Zoll. N.p., n.d Web. Nov.-Dec. 2015
- Flower, Oliver. “Temporary Pacemakers in Critical Care.” Intensive Care Network. N.p., 20 Aug. 2015. Web. 10 Dec. 2015.
- Hayes, David. et.al. “Temporary cardiac pacing” UptoDate. Accessed 07Dec15
- Deal, Nathan, et. al “Focus On: Transcutaneous and Transvenous cardiac pacing. American College of Emergency Physicians. Web. 12 Dec. 2015
- Wood, Mark A., and Kenneth A. Ellenbogen. “Temporary Cardiac Pacing.” Cardiac Pacing and ICDs (2005): 163-95. University of Ottawa Heart Institute. Web. 20 Dec. 2015.
- Insert the pacing catheter and determine capture:










4 thoughts on “Identifying Complete Heart Block and the use of Temporary Cardiac Pacing in the Emergency Department”
Pingback: Emergent Cardiac Pacing – First10EM
Pingback: Complete heart block (3rd degree AV block) : What should you do? – edhsredu
really useful article.thanks a lot
Pingback: PODCAST: Shortness of Breath / Bradycardia | האיגוד הישראלי לרפואה דחופה