Author: Liang Liu, MD (EM Chief Resident, UT Southwestern / Parkland Hospital) // Edited by: Courtney Cassella, MD (@Corablacas, EM Resident Physician, Icahn SoM at Mount Sinai) and Alex Koyfman, MD (@EMHighAK, EM Attending Physician, UTSW / Parkland Memorial Hospital)
A 20-year-old female presents with abdominal pain. She is gravid 2, para 1 at 18 weeks gestation confirmed by ultrasound dating. She has had an uncomplicated pregnancy but has had one day of gradual onset abdominal pain with nausea, vomiting and anorexia. How should this patient be managed? What should be considered for the fetus?
Introduction
Though many obstetric complications occur during pregnancy, the pregnant woman is still a woman with all her other organs that can be at risk, regardless of her pregnancy status. Typically, patients with obstetric complications will complain of uterine tenderness, vaginal bleeding and may have abnormal fetal heart tones on monitoring. When signs and symptoms do not support an obstetric cause for the patient’s abdominal pain, it is imperative that the differential is still wide for all other causes.
The gravid uterus is considered an abdominal organ at 12-week gestation, and this (in conjunction to natural physiologic changes in pregnancy) can complicate and confuse presentations of non-obstetric medical emergencies.1 The expanding uterus can delay the recognition of acute pain and may mask typical findings of peritonitis. Due to a naturally occurring increase in white blood cells during pregnancy, leukocytosis no longer provides as much information in the diagnosis of acute pathology. Additionally, a relative increase in blood volume can delay the development of tachycardia and hypotension in the truly ill patient.1
Appendicitis

The incidence of appendicitis in young women is 1 in every 1500 regardless of pregnancy status.2 It is one of the most common indication for operative management of a non-obstetric condition in the pregnant woman with acute abdomen. Additionally, pregnancy is associated with a two to three times increased rate of appendiceal rupture when comparing pregnant to nonpregnant women.3 Perforation increases both maternal and fetal morbidity, including peritonitis, sepsis, preterm labor, and fetal demise.4 In fact, fetal morbidity and mortality rates increase from 0% to 1.5% in uncomplicated appendicitis to as high as 20% to 35% with perforation.5 This increased rate of complications can be attributed to a delay in diagnosis as many of the symptoms of appendicitis are common during pregnancy including nausea, vomiting and anorexia. Additionally, with the growth of the uterus, the appendix will also move cephalad resulting in an atypical location of pain. The gravid uterus can lift and stretch the anterior abdominal wall away from the inflamed appendix resulting in less direct contact between the area of inflammation and the peritoneum which would result in a muted guarding or rebound tenderness.1,6 Oftentimes, the inflamed appendix is actually in contact with a ureter or renal pelvis resulting in pyuria without bacteriuria and urinary symptoms.7
Though the gold standard for diagnosis of appendicitis is CT in the general population, physicians must weigh the risk of delayed diagnosis and rupture with the risk of exposing the fetus to radiation. Ultrasound, where possible, can confirm diagnosis without exposing the fetus to this risk. Like in the nonpregnant patient, diagnosis is based on first identifying the appendix, a blind ended aperistaltic tubular structure that originates from the base of the cecum. The normal appendix has a wall thickness of 2 mm or less. Appendicitis is diagnosed upon seeing an incompressible, blind ended tubular structure with wall thickness of 3 mm or more and an outer anterior-posterior diameter of 6 mm or more.8 Other findings suggestive of appendicitis include presence of fecalith, hyperechoic periappendicular fat, or a peritoneal fluid collection. However, evaluation of the compressibility of the appendix is less sensitive after 35-week gestation due to the gravid abdomen.9 If the appendix is not visualized due to operator experience, body habitus, intraluminal air or distortion of normal anatomy as seen in pregnancy, an ultrasound is equivocal for the diagnosis. MRI has also been recommended by several studies in place of CT to minimize risk of radiation exposure.1 If US is equivocal and MRI can be obtained without delaying care then proceed to MRI rather than CT.
Definitive management upon diagnosis is early appendectomy within 24 hours of diagnosis to minimize risk of perforation. Perioperative antibiotic treatment should be given in the case of acute appendicitis without peroration to cover gram negatives aerobes and anaerobes as outline in the table below.4 In the case of perforated appendicitis, patients will appear septic and an empiric broad-spectrum antibiotic selection is important and should be continued until cultures can aid in narrowing the agents.4
Cholestasis and Cholecystitis
Progesterone during pregnancy not only slows gastric motility through smooth muscle relaxation but also causes bile stasis. 1 Additionally, elevated levels of estrogen cause aggregation of cholesterol crystals and increased bile concentration.1 Together, these two hormones result in an increased incidence of cholelithiasis and puts patients at risk for acute cholecystitis. Acute cholecystitis is the second most common surgical problem during pregnancy and has an incidence of 0.05% to 0.8%.10
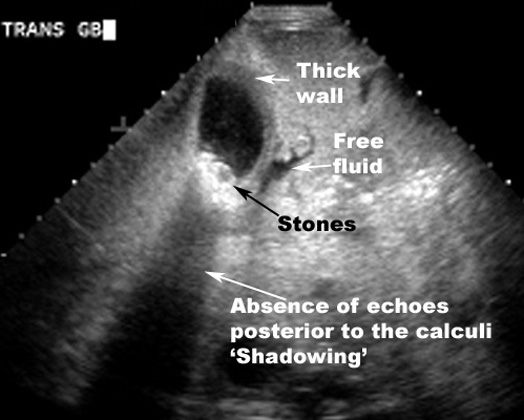
Presentation of the pregnant versus the nonpregnant female with cholecystitis is identical. Laboratory values may not be useful, however, as an increase in white blood cell count, elevated amylase and elevated alkaline phosphatase are all normal during pregnancy.1 Diagnosis is with ultrasound and is confirmed with a gallbladder wall thickness greater than 3 mm, presence of pericholecystic fluid, presences of gallstones and a positive sonographic Murphy’s sign. Management of cholecystitis in pregnancy is identical to that in the nonpregnant patient: cholecystectomy or conservative management with IV fluids, supportive care, and antibiotics (ampicillin-sulbactam, piperacillin-tazobactam, ticarcillin-clavulanate OR ceftriaxone plus metronidazole).11
Pyelonephritis
Nulliparous, young pregnant women, especially in their second trimester, are at highest risk for acute pyelonephritis, and it is most often caused by Escherichia coli.12 Pregnant women are susceptible to pyelonephritis due to the ureteral dilatation that occurs early during pregnancy and persists until delivery due to increased progesterone levels that relax the smooth muscles of the ureters and the direct compression of the ureters by the uterus. This slowed peristalsis and dilatation of the ureters result in urinary stasis and places pregnant women at increased risk of kidney stone formation and infections.2 The IDSA recommends screening for bacteriuria during the early stages of pregnancy and treating for asymptomatic bacteriuria with nitrofurantoin (100 mg BID) or a cephalosporin (generally, Cephalexin 500 mg BID, even though it does not cover enterococci) for 3-7 days with confirmatory test of cure.13 Typically, imaging is not necessary but when complications of pyelonephritis are suspected, renal ultrasounds can be helpful. All pregnant females with pyelonephritis require admission for intravenous antibiotics, and all women in their third trimester with cystitis need admission due to the risk of pre‐term labor.1
Pancreatitis
Acute pancreatitis occurs in 1% of pregnant women and is often self-limited and conservatively managed.1 Presentation is identical to that in nonpregnant patients and diagnosis is based on elevated lipase and clinical picture. Most commonly, this occurs during the third trimester or immediately postpartum. It is thought that the increased incidence in the third trimester is due to increased intra-abdominal pressure by the gravid uterus on the biliary ducts.6 Ultrasound can be useful in identifying complications associated with pancreatitis including common bile duct dilation, cholelithiasis, pancreatic pseudocysts, and abscesses. Generally, a CT is not necessary unless the clinical course is complicated by suspected extensive necrotic pancreatitis or severe pancreatitis. Mainstay of management is no different than pancreatitis in the nonpregnant patient and is primarily supportive care including analgesia, antiemetics, advancing diets as tolerated and maintaining volume status with intravenous hydration.
Adnexal Torsion

Adnexal torsion is a rare problem but does complicate 1 in every 1,800 pregnancies.14 This is more likely during the first and early second trimester, typically involves the right side, and most commonly is due to the presence of the corpus luteum cyst.14 Presentation will be similar to that of nonpregnant patients and ultrasound is the imagining modality of choice for diagnosis. The transabdominal approach can be used initially for evaluation and becomes more useful at later stages of pregnancy as the ovaries are brought out of the pelvis by the enlarging uterus.15 A transvaginal approach may be needed if the adnexal structures are not well visualized in the transabdominal approach. Doppler flow should be used to evaluate for torsion though the presence of flow does not exclude the diagnosis. Management is surgical and requires consultation with OBGYN.
Intestinal Obstruction
Intestinal obstruction occurs in 1 in 1,500 to 3,000 pregnancies.2 Adhesions contribute to 60-70% of small bowel obstructions in pregnancy and are attributed primarily to previous abdominal procedures and prior pelvic inflammatory disease.14 Intestinal obstructions most commonly occur in the third trimester due to the mechanical effects of a rapidly growing uterus on the gastrointestinal tract.1 It is also seen immediately postpartum with the rapid decrease in size of the uterus.1 The maternal mortality rate associated with bowel obstructions during pregnancy can be as high as 6% and fetal mortality as high as 26%.1,14 This risk then increases in the third trimester with maternal mortality rate of 10-20%.1,14
Diagnosis is dependent on serial physical exams and imaging. Serial abdominal films obtained 4-6 hours apart showing air fluid levels and bowel dilatation is diagnostic for intestinal obstruction.6 Absent typical findings on plain films, a CT with contrast is needed for diagnosis in the patient with high clinical suspicion.6 Like in the nonpregnant patient, management is initially conservative: fluid and electrolyte replacement, nasogastric decompression, fetal monitoring and close monitoring.6 However, in the setting of clinical deterioration and worsening symptoms, management regardless of pregnancy status is surgical.6
HELLP Syndrome
In the second half of pregnancy, HELLP (Hemolysis, Elevated Liver enzymes and Low Platelets) syndrome, a complication of preeclampsia, can present with many of the similar symptoms as described for an acute abdomen including nausea, vomiting, and abdominal pain. While some women will have previously documented hypertension and proteinuria in previous pregnancies, 20% of pregnant women will present with HELLP syndrome as their first presentation of pre-eclampsia.16 Patients may complain of acute onset right upper quadrant or epigastric abdominal pain or have other symptoms concerning for development of eclampsia including headache, visual disturbances, altered consciousness or irritability. Workup in these patients will show elevated blood pressures, peripheral smear with schistocytes and burr cells, elevated lactate dehydrogenase, elevated liver enzymes including bilirubin and low platelets.16
Mainstays of management include blood pressure control, prevention of seizures, correction of coagulopathy and delivery of the fetus. A number of antihypertensive medications have been described in the literature for the management of preeclampsia and eclampsia including hydralazine, labetalol, sodium nitroprusside, alpha blockers, calcium channel blockers, and methyldopa.17 Hydralazine and labetalol are the most commonly used. Hydralazine is given initially as a 5 mg IV bolus then repeated at 20 minute intervals of 5 to 10 mg IV bolus depending on response until blood pressure is controlled and then repeat dosing to maintain blood pressure control every 3 hours.17 Labetalol is given as an initial 20 mg IV bolus and then doubled every 10 minutes until blood pressure controlled with a maximum dose of 220 mg.17 (Summary see Table 2.) Magnesium is also given for its vasodilatation role and to prevent seizures.17, 20 For dosing of magnesium, see Table 3.20

Hepatic rupture is a rare complication in these patient, and patients will present with severe abdominal pain and in hemorrhagic shock.16 Fetal outcomes in these patients are devastating with mortality rates ranging from 40% to 60% in both the mother and the fetus regardless of gestational age due to delays in diagnosis and the critically ill state of the mother.18 Emergency laparotomy with bleeding control, termination of the pregnancy and correction of the coagulopathy is paramount in the management of these patients to save the mother’s life.19
Conclusion
Delays in care of the pregnant female with non-obstetric emergencies arise both from delays in diagnosis due to vague symptoms and atypical presentation and also from delays in obtaining appropriate and definitive diagnostic imaging. Though radiation exposure does place risk on the development of the fetus and future cancer risks of the child, a fetus absorbs 3.5 rad when exposed to a typical CT scan of the abdomen and pelvis and 0.02 to 100 mrad with conventional chest and abdomen radiographs.19 These levels are much lower than the radiation dose threshold thought to cause morbidity and mortality to the fetus.1,19 As such, with good clinical gestalt, delays in diagnosis and in obtaining definitive workup should be avoided to improve outcomes for the pregnant woman.
Take Home Points
- The gravid uterus can mask the signs of peritoneal irritation (guarding, rigidity and rebound tenderness) by preventing the inflamed organ from contacting the peritoneum.
- Due to increased white blood cells that naturally occur during pregnancy, leukocytosis is not helpful in identifying acute pathology.
- A relative increase in blood volume can delay the development of tachycardia and hypotension in the truly ill patient.
- Consider appendicitis in the patient complaining of typical signs and symptoms of appendicitis even if confounded by right middle and upper quadrant abdominal pain, pyuria, urinary symptoms and subtle signs of peritonitis.
- HELLP syndrome is managed with blood pressure control, prevention of seizures, correction of coagulopathy, and delivery of the fetus.
- Radiological investigations, including abdominal plain films, can be safely undertaken during pregnancy and should always be considered so as to avoid delays and failures in diagnosing potentially life-threatening conditions.
References / Further Reading
- Diegelmann L. Nonobstetric abdominal pain and surgical emergencies in pregnancy. Emerg Med Clin North Am. 2012 Nov;30(4):885-901. doi: 10.1016/j.emc.2012.08.012.
- Kilpatrick CC, Monga M. Approach to the acute abdomen in pregnancy. Obstet Gynecol Clin North Am 2007; 34: pp. 389-402
- Gilo NB, Amini D, Landy HJ. Appendicitis and cholecystitis in pregnancy. Clin Obstet Gynecol 2009; 52: pp. 586-596
- Young BC, Hamar BD, Levine D, Roqué H. Medical management of ruptured appendicitis in pregnancy. Obstet Gynecol. 2009 Aug;114(2 Pt 2):453-6. doi: 10.1097/AOG.0b013e3181998424
- Guttman R, Goldman R, and Koren G. Appendicitis during pregnancy. Can Fam Physician 2004; 50: pp. 355-357
- Augustin G, Majerovic M. Non-obstetrical acute abdomen during pregnancy. Eur J Obstet Gynecol Reprod Biol 2007; 131: pp. 4-12
- Kennedy A. Assessment of acute abdominal pain in the pregnant patient. Semin Ultrasound CT MR. 2000 Feb;21(1):64-77. doi:10.1016/S0887-2171(00)90014-3
- Wild JRL, Abdul N, Ritchie JE, Rud B, Freels S, Nelson RL. Ultrasonography for diagnosis of acute appendicitis (Protocol). Cochrane Database of Systematic Reviews 2013, Issue 2. Art. No.: CD010402. doi: 10.1002/14651858.CD010402
- Vissers R.J., and Lennarz W.B.: Pitfalls in appendicitis. Emerg Med Clin North Am 2010; 28: pp. 103-118
- Date R.S., Kaushal M., and Ramesh A.: A review of the management of gallstone disease and its complications in pregnancy. Am J Surg 2008; 196: pp. 599-608
- Brooks D.: Gallstone disease in pregnant women. Wolters Kluwer Health, 2012.
- Sharma P., and Thapa L.: Acute pyelonephritis in pregnancy: a retrospective study. Aust N Z J Obstet Gynaecol 2007; 47: pp. 313-315
- Nicolle LE, Bradley S, Colgan R, Rice JC, Schaeffer A, and Hooton TM. Infectious Diseases Society of America Guidelines for the Diagnosis and Treatment of Asymptomatic Bacteriuria in Adults. CID 2005; 40: pp. 643-654
- Cappell M.S., and Friedel D.: Abdominal pain during pregnancy. Gastroenterol Clin North Am 2003; 32: pp. 1-58
- Graham L.: ACOG releases guidelines on management of adnexal masses. Am Fam Physician 2008; 77: pp. 1320-1323
- Chandraharan, E., Arulkumaran, S. Acute abdomen and abdominal pain in pregnancy. Obstet Gynaecol Reprod Med. 2008;18: pp. 205–212.
- Neligan PJ and Laffey JG. Clinical review: Special populations – critical illness and pregnancy. Crit Care. 2011; 15(4): 227. Epub 2011 Aug 12. doi: 10.1186/cc10256
- Augustin G, Majerovic M. Non-obstetrical acute abdomen during pregnancy. Eur J Obstet Gynecol Reprod Biol. 2007 Mar;131(1):4-12. Epub 2006 Sep 18. doi: 10.1016/j.ejogrb.2006.07.052
- Devarajan S, Chandraharan E. Abdominal pain in pregnancy: a rational approach to management. Obstet Gynaecol Reprod Med. 2011;21:198–206. doi: 10.1016/j.ogrm.2011.04.001
- Lew M, Klonis E. Emergency Management of eclampsia and severe pre-eclampsia. Emerg Med (Fremantle). 2003 Aug; 15(4):361-8.
- Calhoun DA, Oparil S. Treatment of hypertensive crisis. N Engl J Med. 1990 Oct 25;323(17):1177-83.









