Author: Brit Long, MD (@long_brit, EM Chief Resident, SAUSHEC, USAF) // Edited by: Jennifer Robertson, MD and Alex Koyfman, MD (@EMHighAK)
Case 1:
A 28 year-old female with a history of HIV presents to the emergency department (ED) with chest pain and shortness of breath. Her only medications include highly active antiretroviral therapy (HAART) and simvastatin. Besides HIV, her other comorbidities include hyperlipidemia. Her chest X-ray is normal, and her electrocardiogram (ECG) shows nonspecific T-wave inversions. The patient’s pain is controlled with a GI cocktail, and she is discharged home with primary care follow-up.
Case 2:
A 54 year-old male with chronic renal disease and hypertension presents with shortness of breath. His initial ECG is normal. He had a recent treadmill stress test five months ago, and states that he thinks it was “normal”. The patient’s pain resolves after one 0.4mg tab of sublingual nitroglycerin, and he is discharged.
Both patients return with crushing chest pain to a different ED, where both patients’ ECGs show ST elevation with reciprocal changes.
What was missed on the first visit? Could the initial ED physician have done anything differently?
Discussion
Chest pain is the presenting complaint of 5-8% of ED visits. With over 8 million patient visits per year to EDs for chest pain, about 15% of patients will be diagnosed with acute coronary syndrome (ACS), which is broken into unstable angina, non ST elevation myocardial infarction (NSTEMI), and ST elevation myocardial infarction (STEMI).1,2
Myocardial infarction (MI) is defined as the clinical event caused by myocardial ischemia with evidence of myocardial injury/necrosis. To meet criteria for MI, there must be a rise in cardiac biomarkers above the 99th percentile upper reference limit along with typical symptoms, suggestive ECG changes such as new Q waves, new ST segment / T wave changes, identification of an intracoronary thrombus by angiography, or new loss of viable myocardium/new regional wall motion abnormality.3,4
Many of us were taught that large, stenotic plaques are the cause of symptoms. However, a recent New England Journal of Medicine (NEJM) publication demonstrates the importance of plaque composition, rather than size, as being the most important factor.5 It is important to note that approximately 50% of plaques that cause MI obstruct less than 2/3 of the vessel lumen before acute occlusion. Plaques can rupture at any size, including those considered non-obstructive. Plaques with a thin fibrous cap, large fatty lipid core, and inflammation in the lipid core are most susceptible to rupture due to immaturity. As plaques grow in size, they may extend outward rather than inward, causing wall bulging. The lumen remains patent with good perfusion, until the plaque ruptures.5
Classically, the quoted percentage of missed MI is 2%. However, closer inspection of an article by Pope, et al. reveals that the rate is closer to 0.2%, as discussed by Dr. David Newman on SMART EM.6,7 The range of lawsuit payout for missed myocardial infarction ranges from 10% to 30% (though closer to 10%).8 Who are the patients most at risk for missed MI? These patients usually have fewer typical risk factors (hypertension, hyperlipidemia, diabetes, coronary disease, family history), the young, females, and those with less typical presentations. Several reasons account for why physicians miss MI: 1) Patient factors, 2) ECG findings, and 3) Testing factors.
1) Patient factors:
First, not all patients with MI have chest pain. Up to 1/3 of patients will have silent or atypical symptoms such as shortness of breath, malaise, fatigue, pre-syncope/syncope, or nausea/vomiting.9,10 The Global Registry of Acute Coronary Events (GRACE) trial found 8.4% of patients did not have chest pain, and dyspnea was actually the dominant symptom in more than half of patients.3 Females, older patients, diabetics, and patients with heart failure more often present atypically. Unfortunately, those patients who present atypically often receive suboptimal treatment and have increased morbidity and mortality. Mortality has been shown to be 13% in those presenting with atypical symptoms as compared to 4% presenting with typical symptoms.9,10
Traditional factors are for population use only and not for individual patients
The presence of classic cardiac risk factors such as hypertension, smoking, hyperlipidemia, and diabetes are helpful for predicting long-term risk of coronary artery disease (CAD) in a population, but they are limited in ruling out ACS. If the story is good for ACS but the patient has no risk factors, clinicians should still consider it as a diagnosis. One study demonstrated that 10.5% of patients with non-STEMI had none of the traditional risk factors.11 A separate study by Body showed that 12% of patients with no risk factors ruled in for acute MI.12 In younger patients who died of “non-natural causes” with average age of 36 years, over 80% of patients had coronary disease at autopsy, with 8% having significant coronary obstruction.13 Thus, be wary of discounting ACS risk based on patients with no classic risk factors or just because the patient is young!1
Consider nontraditional risk factors in younger patients with chest pain. Patients with HIV/AIDS have higher risks of MI due to HAART therapy and chronic inflammation, which both can cause increased thrombus and platelet plug formation. In particular, protease inhibitors may cause hyperglycemia, hyperlipidemia, and central obesity.15 A higher prevalence of hyperlipidemia, arteriosclerosis, left ventricular hypertrophy, and heart failure are also present in patients with chronic kidney disease. Dialysis patients have a 10 to 30 times higher mortality from coronary disease as compared to the general population.16 Lupus is another important risk factor, as women with lupus aged 35 to 44 years have 50 times greater risk of MI. The mean age of lupus patients with first MI is 20 years younger than those without lupus. This disease causes premature atherosclerosis due to chronic steroid use, inflammation, hyperlipidemia, and renal disease.17 Long-term steroid use is itself a risk factor due to increased insulin resistance, hyperlipidemia, central obesity formation, and hypercoagulability.18 Pregnancy is also a risk factor for acute MI, with risk increased four-fold. This risk is even higher in women over 40 years (30 fold risk). Heart disease is now one of the largest non-obstetric related causes of death in pregnant women in the developed world.19
Elderly patients present several challenges for emergency physicians. They often present atypically with dyspnea, fatigue, and/or nausea with vomiting. Chest pain is present in 50% of cases of MI in the elderly. They are also less likely to have diagnostic ECGs, with ST depression and/or subtle changes more common. The proportion of patients over 85 years with NSTEMI who have non-diagnostic ECG is over 40%! Baseline abnormalities are often present on the ECG including left bundle branch block (LBBB), paced rhythms, left ventricular hypertrophy, and prior MI. Due to the often atypical presentations and non-diagnostic ECGs, the elderly are at tremendous risk of death from MI due to under diagnosis and under treatment. The 30-day mortality after MI in patients less than 65 years is 3%, 65-74 years 10%, 75-84 years 20%, and over 85 years 30%. Elderly patients account for over 80% of deaths from MI. The older patient warrants a closer evaluation for ACS.20,21
Beware of the patient presenting with anxiety and recent emotional events. These patients are at higher risk of ACS, as a stressful event effectively functions as a stress test. An ECG should be obtained in the anxious patient, especially if he or she has chest pain. Wars, earthquakes, sport games, family arguments, or even road rage can all increase catecholamine release, which may result in unstable plaque rupture and platelet aggregation.22
The physical exam for patients with chest pain is important. Always consider other chest pain causes (pulmonary embolism (PE), pneumothorax, esophageal rupture, pericarditis, myocarditis, pneumonia, tamponade, and aortic dissection). Pain that radiates to the bilateral shoulders or right shoulder, chest pain with exertion, chest pain with diaphoresis, and chest pain with nausea/vomiting increase the likelihood of ACS. Chest pain described as pressure surprisingly does not increase the likelihood of ACS. Factors that decrease the likelihood include pleuritic pain, positional pain, sharp pain, pain at rest, and reproducible pain. However, none of these will rule out ACS, as up to 16% of patients with ACS will have atypical pain. For example, 20% of patients have upper abdominal pain or reflux symptoms instead of chest pain. One third of patients have pressure, while 20% will call the pain indigestion. Only 1/3 of patients have pain with exertion, 8% have pain with eating, and 7% have pain with emotional stress. Anywhere from 30% to 50% will have no chest pain. ACS can and will present atypically. You cannot rule out ACS based on the absence of typical symptoms and signs.23-25
One of the most common misdiagnoses in cases of missed MI is reflux esophagitis. Up to 20% of patients present with “indigestion” or “burning” pain. Almost 50% of patients with acute MI report increase in belching, 15% obtain some relief with antacids, and 7% obtain complete relief with antacids.23-25 Do not use a gastrointestinal (GI) cocktail as a diagnostic tool. Patients with documented coronary disease and those without have similar pain relief from GI cocktails. An Annals of Emergency Medicine study demonstrated that patients with chest pain and abdominal pain had similar frequencies of responses to GI cocktails.26 If you are going to use a GI cocktail to treat a patient’s pain, then know that it should not be used for diagnosis! Before you discharge a patient with “reflux,” consider ACS.
Women experience higher mortality rates and more adverse outcomes, even with less obstructive disease. Women actually have more coronary remodeling of vessels, which means plaques grow into the vessel wall, causing bulging outward. Coronary angiography often misses these lesions. Women will more often have false negative stress tests and angiograms (that will show normal or non-significant disease). Do not rely on stress testing or angiography in these patients.27,28
2) ECG findings:
Be systematic during your evaluation of the ECG. Look at each lead for ST depression, elevation, and T wave changes. Look through the five MI patterns on the ECG: anterior (V1-V6), inferior (II, III, aVF), lateral (I, aVL, V5-V6), RV infarct (ST depression in V2, elevation in V1), and posterior (large R waves in V1-V3 with ST depression). Closely evaluate for ST changes (depression and elevation) and T wave changes.
Do not just get one ECG. Initially normal or non-specific ECGs can occur in patients with acute MI. A 2001 JAMA study showed that 7.9% of patients had initially normal ECGs, 35.1% had non-specific ECG abnormalities, and 57% had diagnostic changes on their ECGs. With a normal ECG, in-hospital mortality was 5.7%!29 A separate study by Riley demonstrated that in over 41,000 patients, 11% had initially non-diagnostic ECGs. One third converted to STEMI by 30 minutes, 50% converted to STEMI by 45 minutes, and 75% converted by 90 minutes.30 In patients with concerning symptoms and/or if their pain changes, repeat ECGs should be obtained. Obtaining an ECG every 15 minutes in patients with a concerning history can be helpful. Remember that the ECG is good at ruling in MI, but not ruling out ACS.31
Evaluate for ST depression, reciprocal changes, and T wave changes. ST depression does not localize ischemia if present without ST elevation, as ST depression may only denote reciprocal changes. Using the pneumonic PAILS (Posterior, Anterior, Inferior, Lateral, Septal) can be helpful for anatomical reciprocal changes. For example, ST elevation in anterior leads should produce depression in inferior leads, and elevation in lateral leads should produce depression in septal leads. However, do not rely on reciprocal changes to diagnose STEMI. Some cases may only have ST elevation with no reciprocal changes. T wave inversions that are new or anatomical warrants repeat ECG for evolution and evaluation of prior ECG. Hyperacute T waves are often “fat and wide” with poor R wave progression and blunt peaks, while hyperkalemic T waves are more often sharp with narrow base. These ischemic T waves morph quickly into ST segment elevation, so evaluate closely for these large T waves.32,33
Always obtain an old ECG, which gives you a baseline to evaluate for changes in the new ECG. This is a vital step in the evaluation of the ACS patient and can help prevent misdiagnosis and missing an acute event.32,33
Be wary of Non-ACS causes of ST elevation. Mimics of STEMI include benign early repolarization, pericarditis, left ventricular aneurysm, Brugada syndrome, LVH, LBBB, paced rhythms, and hyperkalemia. To help differentiate a STEMI vs. a mimic, first look for ST depression as LVH, LBBB, paced rhythms, and hyperkalemia can present with ST depression. Next, repeat the ECG and look for evolving changes, which may point towards a STEMI. With the exceptions of leads aVR/VI, the diagnosis of MI is more commonly seen in ECGs with ST depressions. Additionally, MI is also commonly seen in ECGs with horizontal or convex upwards ST elevations, evolving ST/T waves, new ST changes when compared with old ECGs, new Q wave development, or ST elevations that follow coronary anatomy (ST elevation limited to inferior leads, lateral leads, etc.).32,33
Pericarditis vs. STEMI: Pericarditis should not have ST depressions, but may have PR depressions in multiple leads. A friction rub (specific but not sensitive for pericarditis) may be present, and concave ST elevations as well as ST elevation in lead II greater than in III may be present. If ST elevation is greater in III than II, ST depression is present in any lead besides aVR and V1, or ST elevation is convex or straight upwards, then a STEMI should be considered. 32,33
Ventricular aneurysm vs. STEMI: A STEMI should demonstrate ST depressions, also known as reciprocal changes. An ECG showing large T waves in leads with Q waves and ST elevations is more consistent with a STEMI. A ventricular aneurysm will usually present with blunted or flat T waves in the leads with Q waves on the ECG. Also, this is where serial ECGs can be helpful. ECGs in patients with ventricular aneurysms should not change from prior ECGs, while STEMI ECG’s often do evolve over the course of 1 hour. Aneurysms usually involve the anterior wall, while STEMI can involve the anterior, lateral, posterior, or inferior leads. Aneurysms will almost always have Q waves, while STEMs may or may not show Q waves. 32,33
Benign Early Repolarization (BER) vs. STEMI: Differentiating BER from STEMI can be difficult. Again, it is vital to obtain repeat ECG’s and evaluate for change. BER always has concave ST elevations (never horizontal, straight, or convex). ST elevations on ECGs in BER are usually largest in the precordial leads, and large R waves in the precordial leads should also be present. The ECG in BER can demonstrate ST elevation in the inferior leads, but the elevation should not be isolated to the inferior leads. ST elevation should never be greater than 5mm in BER, and BER ECGs should not show ST depressions, except perhaps in aVR and VI. ST elevation in inferior leads III greater than II points to STEMI. 32,33
Posterior STEMI: Approximately 4% of acute STEMIs will be isolated posterior in location. These can be easily misdiagnosed as reciprocal changes, so the ECG should `be examined closely. The diagnosis of posterior STEMI is made with the following: ST depressions in leads V1-V3, upright T waves in V1-V3, and tall R waves (R>S) in V1-V3 that develop over several hours (similar to Q waves). These R waves many not be present acutely. If any ECG shows ST depressions in V1-V3, a repeat the ECG with posterior leads V7-V9 should be obtained. ST elevations of ≥ 0.5mm in the posterior leads meet criteria for reperfusion. 32,33
Paced Rhythms/Left Bundle Branch Block (LBBB): The criteria for diagnosing STEMI in the presence of paced rhythms and LBBBs have been recently updated. The diagnosis of STEMI in the setting of a LBBB is met with the following algorithm:34,35
3) Testing factors:
A recent “negative” angiogram does not definitely rule out ACS. Coronary arteriography remains the gold standard for coronary disease, with stenosis > 70% usually resulting in intervention. Why 70%? In general, at 70% stenosis an epicardial vessel is maximally dilated and can no longer accommodate for a decrease in flow. This is hypothesized to cause cardiac ischemia and chest pain. At 90%, it is thought that patients will experience pain at rest. Lesion severity can be calculated via computer analysis or manually. Manual calculations are conducted by comparing the diameter of the vessel at the location of tightest stenosis with normal vessel size. This method is performed by the interventional cardiologist. Quantitative coronary angiography is done by a computer that analyzes and compares the diseased segment (s).36,37
Calculating disease severity can be problematic for multiple reasons. First, if there are no lesions greater than 70%, the report may read “non-obstructive.” This is not “normal.” The disease may have progressed from the time of the angiogram, with lesions progressing 10-20% per year and even faster in patients with diabetes or inflammatory disease.38 Also, an angiogram is two dimensional and may have difficulty evaluating eccentric plaques. The angiogram focuses on larger epicardial vessels, while vessels smaller than 1.5mm may be missed or not reported on. Additionally, microvasculature is often not assessed at all.39,40 Most importantly, many STEMIs result from plaques that are less than 60% the diameter of the vessel but are unstable in composition.41 And as discussed above, it is not size that is important, but the composition. Thus, a lesion that is described as “non-obstructive” or “non-flow limiting” may actually be the one that ruptured, causing ischemia and infarction. Unfortunately, the angiogram does not evaluate plaque composition.
Another point regarding the negative angiogram is that ischemic events can occur in patients in the absence of coronary disease (due to vasospasm, myocardial vessel dissection, vessel trauma, vasculitis, myocardial bridging, coronary vessel tortuosity, and microvascular dysfunction).42,43 One study found that 9% of NSTEMIs had non-obstructive disease, with 50% of those showing no disease on angiogram, yet these patients had a 2% rate of death/MI and a 12.1% event rate (revascularization, MI, UA death, stroke) in one year. Thus, “non-significant” disease is not reassuring!44
Never assume that a recent negative stress test rules out ACS. Many patients who present with chest pain have had some prior stress testing. The goal of stress testing is to screen for CAD and identify a fixed obstruction (usually plaque greater than 50%). The sensitivity for exercise stress tests is only in the range of 68%-77% for single vessel disease. The sensitivity is better for multivessel disease.
Remember that the underlying pathophysiology of ACS is plaque rupture (usually in plaques less than 50%) with thrombus formation and platelet aggregation. These plaques will not always cause a positive stress test.45,46 In one study, 20.7% of patients presenting to the ED with a negative stress test in the last three years had positive cardiac markers, cardiac catheterization requiring intervention, or death due to cardiac arrest within 30 days of ED visit.47
If the history is concerning, do not obviate your concern for the patient because of a recent negative stress test. These tests may identify large occlusions, but they cannot tell us about recent rupture or composition of the plaque. Remember that stress tests neither assess unstable plaques, nor predict or assess for disease in the individual in front of you.
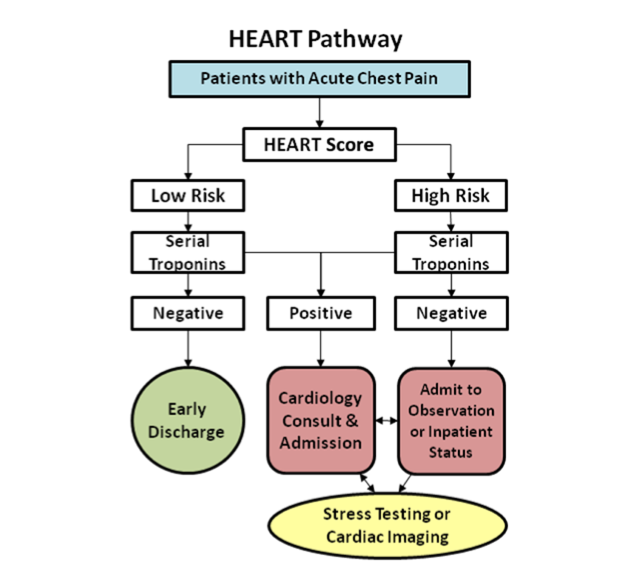
Use clinical pathways and troponin testing wisely. Many institutions utilize a specific pathway for chest pain patients in conjunction with troponin testing. First, know what pathway is used in your institution. An evaluation of the HEART (History, ECG, Age, Risk factors, Troponin) pathway found that it helped decrease hospitalizations and interventions with no major cardiac adverse events. The HEART pathway is shown below. A score of 0-3 is deemed low risk for cardiac events.48-50 Know what your institution utilizes and what your internal medicine and cardiology colleagues will want for follow up in these patients.
Finally, and most importantly, discuss with the patient your workup and findings. If you are going to discharge him or her, talk about the risks and benefits of discharge. Give him or her a diagram or visual aid (shown below from University of Maryland) that provides an overview of his or her cardiac risks. Ensure that you document your discussion, the patient’s agreement and consensus on the risk/benefits of the plan, the patient’s follow up plans, and return precautions.50
Summary
– Be aware of the complaints of dyspnea, pre-syncope/syncope, nausea/vomiting, diaphoresis, or fatigue in older patients, diabetics, women, and heart failure patients and check an ECG.
– Traditional risk factors are for population use only, not for the patient in front of you.
– Patients with HIV/AIDS, CKD, dialysis, lupus, long-term steroid use, and pregnancy are at higher risk for MI.
– Pain that radiates to the bilateral shoulders or right shoulder, chest pain with exertion, chest pain with diaphoresis, and chest pain with nausea/vomiting are associated with increased likelihood of ACS
– Carefully evaluate elderly, women, and those presenting with chest pain in the setting of emotional stress. Elderly and women more often present atypically.
– Systematically evaluate the ECG, obtain an old ECG, and repeat ECGs. Look for ST depression/elevations and hyperacute T waves and know STEMI mimics.
– A recent “negative” angiogram or stress test does not rule out disease.
– Know what clinical pathway your institution uses, and ensure you have cardiology and internal medicine agreement and follow up
-Always discuss with the patient the plan and ECG/test results. Provide a visual aid for risk.
-Discuss and document this discussion on the plan for follow-up with return precautions.
References/Further Reading
- Kontos, KC. Evaluation of the Emergency Department chest pain patient. Cardiol Rev 2001;9(5):266-275.
- Lai C, Noeller TP, et al. Short-term risk after initial observation for chest pain. J Emerg Med 2003;25(4):357-62.
- Fox KA, Goodman SG, Klein W, et al. Management of acute coronary syndromes. Variations in practice and outcome; findings from the Global Registry of Acute Coronary Events (GRACE). Eur Heart J 2002;23:1177-89.
- Thygesen K, Alpert JS, Jaffe AS, et al. Third universal definition of myocardial infarction. Circulation 2012;126:2020-35.
- Libby P. Mechanisms of acute coronary syndromes and their implications for therapy. N Engl J Med 2013 May 23;368(21): 2004-13.
- Pope JH, et al. Missed diagnoses of acute cardiac ischemia in the emergency department. N Engl J Med 2000 Apr 20;342(16):1163-70.
- Newman D. Stress testing. SMART EM. 25 January, 2012. http://www.smartem.org/podcasts/stress-testing-moment-clarity
- Glenn C, et al. Medicolegal aspects of acute myocardial infarction. 2001 May 01;19(2):511-21.
- Brieger D, et al. Acute coronary syndromes without chest pain, an underdiagnosed and undertreated high-risk group. Insights from the Global Registry of Acute Coronary Events. Chest 2004;126(2):461-9.
- Dorsh MF, et al. Poor prognosis of patients presenting with symptomatic myocardial infarction but without chest pain. Heart 2001;86(5):494-8.
- Roe MT, Halabi AR, Mehta RH, et al. Documented traditional cardiovascular risk factors and mortality in non-ST-segment elevation myocardial infarction. Am Heart J 2007;153:507-514.
- Body R, McDowell G, Carley S, et al. Do risk factors for chronic coronary heart disease help diagnose acute myocardial infarction in the Emergency Department? Resuscitation 2008;79:41-45.
- Nemetz PN, et al. Recent trends in the prevalence of coronary disease: a population-based autopsy study of non-natural deaths. Arch Intern Med 2008;168:264-270.
- Arbab-Zadeh A, et al. Acute coronary events. Circ 2012;125:1147-1156.
- Khunnawat C, Mukerji S, Havlichek D, et al. Cardiovascular Manifestations in Human Immunodeficiency Virus-Infected Patients. Am J Cardiol 2008;102:635-642.
- Sarnak MJ, et al. Kidney disease is a risk factor for development of cardiovascular disease: A statement from the American Heart Association councils on kidney in cardiovascular disease, high blood pressure research, clinical cardiology, and epidemiology and prevention. Hypertension 2003;42(5):1050-65.
- Mattu A, Petrini J, Swencki S, et al. Premature atherosclerosis and acute coronary syndrome in systemic lupus erythematosus. Am J Emerg Med 2005;23:696-703.
- Maxwell SR, et al. Corticosteroids: Do they damage the cardiovascular system? Postgrad Med J 1994;70(830):863-70.
- Roos-Hesselink, et al. Pregnancy in high risk cardiac conditions. Heart 2009;95:680-686.
- Alexander KP, et al. Acute coronary care in the elderly, part I: Non-ST-segment elevation acute coronary syndromes. Circulation 2007;115:2549-2569.
- Samaras, N, Chevalley, T, et al. Older patients in the emergency department: a review. Ann Emerg Med 2010;56:261-269.
- Wittstein IS, et al. Neurohumoral features of myocardial stunning due to emotional stress. N Engl J Med 2008;358(5):475-83.
- Swap CJ, Nagurney JT. Value and limitations of chest pain history in the evaluation of patients with suspected acute coronary syndromes. JAMA 2005;294:2623-2629.
- Body R, Carley S, Wibberley C, et al. The value of symptoms and signs in the emergent diagnosis of acute coronary syndromes. Resuscitation 2010;81:281-286.
- Panju AA, Hemmelgarn BR, Guyatt GH, et al. Is this patient having a myocardial infarction? JAMA 1998;280:1256-1263.
- Wrenn K, Slovis CM, Gongaware J. Using the “GI cocktail”: a descriptive study. Ann Emerg Med 1995;26(6):687-90.
- Della Rocca DG, Pepine CJ. What causes myocardial infarction in women without obstructive coronary artery disease? Circulation 2011;124:1404-1406.
- Reynolds HR, Srichai MB, Iqbal SN, et al. Mechanisms of myocardial infarction in women without angiographically obstructive coronary artery disease. Circulation 2011;124:1414-1425.
- Welch RD, Zalenski RJ, et al. Prognostic Value of a Normal or Nonspecific Initial Electrocardiogram in Acute Myocardial Infarction. JAMA 2001;286(16):1977-1984.
- Riley RF, et al. Diagnostic time course, treatment, and in- hospital outcomes for patients with ST-segment elevation myocardial infarction presenting with nondiagnostic initial electrocardiogram: a report from the American Heart Association Mission: Lifeline program. Am Heart J 2013 Jan;165(1):50-6.
- Turnipsee SD, Trythall WS, Diercks DB, et al. Frequency of acute coronary syndrome in patients with normal electrocardiogram performed during presence or absence of chest pain. Acad Emerg Med 2009;16:495-9.
- Smith SW. Dr. Smith’s ECG Blog. http://hqmeded-ecg.blogspot.com.
- Weingart SC. Who needs an acute PCI with Steve Smith (Parts I and II). EMCrit. http://emcrit.org/podcasts/who-needs-acute-pci/
- Cai Q, et al. The left bundle-branch block puzzle in the 2013 ST-elevation myocardial infarction guideline: from falsely declaring emergency to denying reperfusion in a high-risk population. Are the Sgarbossa Criteria ready for prime time? Am Heart J 2013 Sep;166(3):409-13.
- Smith SW, et al. Diagnosis of ST-elevation myocardial infarction in the presence of left bundle branch block with the ST-elevation to S-wave ratio in a modified Sgarbossa rule. Ann Emerg Med 2012 Dec;60(6):766-76.
- Fischer JJ, et al. Comparison between visual assessment and quantitative angiography versus fractional flow reserve for native coronary narrowings of moderate severity. Am J Cardiol 2002;90:210-5.
- Klocke FJ. Measurements of coronary blood flow and degree of stenosis: Current clinical implications and continuing uncertainties. JACC 1983;1:31-41.
- Glaser R, et al. Clinical progression of incidental, asymptomatic lesions discovered during culprit vessel coronary intervention. Circulation 2005;111(2):143-9.
- Topol EJ, Nissen SE. Our preoccupation with coronary luminology. The dissociation between clinical and angiographic findings in ischemic heart disease. Circulation. 1995 Oct 15;92(8):2333-42.
- Yamagishi M, et al. Morphology of vulnerable coronary plaque: insights from follow-up of patients examined by intravascular ultrasound before an acute coronary syndrome. J Am Coll Cardiol 2000 Jan;35(1):106-11.
- Hackett D, et al. Pre-existing coronary stenoses in patients with first myocardial infarction are not necessarily severe. Eur Heart J 1988 Dec;9(12):1317-23.
- Galzio et al. Myocardial infarction with normal coronary arteries: Ten-year follow up. Ital Heart J 2004;5(10):732-8.
- Gaibazzi N1, Rigo F, et al. Severe coronary tortuosity or myocardial bridging in patients with chest pain, normal coronary arteries, and reversible myocardial perfusion defects. Am J Cardiol 2011 Oct 1;108(7):973-8.
- Bugiardini R1, Badimon L, et al. Angina, “normal” coronary angiography, and vascular dysfunction: risk assessment strategies. PLoS Med 2007 Feb;4(2):e12.
- Selker HP, et al. ECG exercise stress test. Ann Emerg Med 1997;29(1):33-8.
- Ioannidis JP, et al. Accuracy of imaging technologies in the diagnosis of acute cardiac ischemia in the emergency department: A meta-analysis. Ann Emerg Med 2001;37(5):471-7.
- Walker J, Galuska M, Vega D. Coronary Disease in Emergency Department Chest Pain Patients With Recent Negative Stress Test. West JEM Sep 2010;40(4).
- Mahler SA, et al. The Heart Pathway Randomized Trial: Identifying Emergency Department Patients with Acute Chest Pain for Early Discharge. Circ Cardiovasc Qual Outcomes March 2015;82:195.
- Backus BE, et al. Chest pain in the emergency room: a multicenter validation of the HEART Score. Crit Pathw Cardiol 2010 Sep;9(3):164-9.
- University of Maryland. Low Risk Chest Pain Evaluation and Disposition Guideline. http://ec.libsyn.com/p/d/c/d/dcdd1ccf2e26506d/Feb_2015_Low_Risk_Chest_Pain_Evaluation_and_Disposition__Guideline-final-1.pdf?d13a76d516d9dec20c3d276ce028ed5089ab1ce3dae902ea1d06cb8e33d8ce5e14b8&c_id=8383156








1 thought on “Missed Myocardial Infarction in the Emergency Department”
Pingback: emDOCs.net – Emergency Medicine EducationNon-Traditional ACS Risk Factors: A Snake in the Grass - emDOCs.net - Emergency Medicine Education