Author: David Cisewski, MD (@PainProfiles – EM Resident Physician, Icahn School of Medicine at Mount Sinai) // Edited by: Manpreet Singh, MD (@MPrizzleER), Alex Koyfman, MD (@EMHighAK), and Brit Long, MD (@long_brit)

No, not Detroit…. I’m referring to Dilaudid, aka hydromorphone. This terrifying 8-letter word may make people take three steps back when they hear it in the ED. However, this article is not a condemnation of opioid use in the ED. To the contrary, opioids serve a distinct purpose in the ED, and it is essential that health care providers take an evidence-based approach to their use. The objective of this article is to provide an overall understanding of hydromorphone, how it is used effectively in the emergency setting, and what evidence we have to supports this – much of which is hot off the press.
Let’s start with the basics: what is hydromorphone?
Hydromorphone (HM), as many know, is a highly lipophilic opioid with rapid, potent CNS activation [1, 2]. At approximately 7-times the potency of morphine sulfate (MS) but 13-times less potent than fentanyl, HM is the middle-child of the opioid family [2, 3]. Nevertheless, it is an incredibly powerful analgesic that can result in significant adverse effects if incorrectly dosed in the ED.
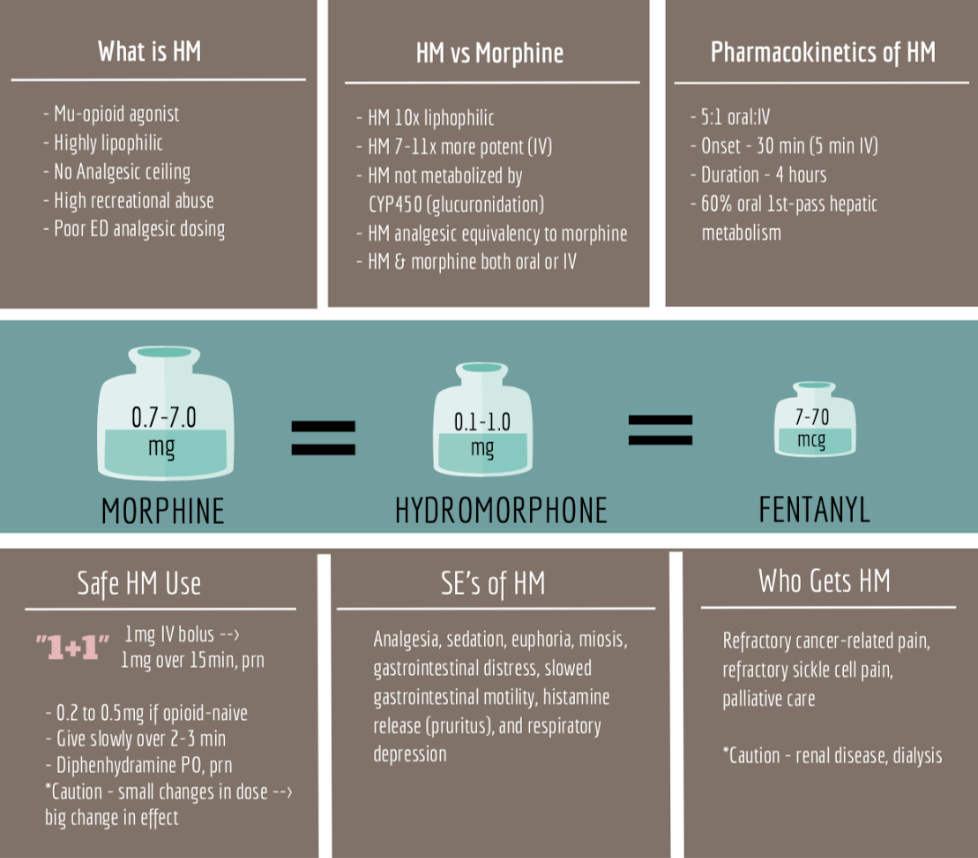
How should we be dosing HM in the ED?
This is slightly controversial until you take a look at the evidence. Most agree that HM should be limited to moderate and severe pain. Typical recommendations are to start at 0.75 – 1.5 mg IV based on equianalgesicdosing (based on 0.1 mg/kg IV morphine equianalgesic dosing). However, in opioid-naïve patients, dosing as low as 0.25-0.5 mg IV administered over 2-3 minutes may be used to avoid nausea, pruritus, and rapid (over) sedation [2, 4-6]. Onset of HM is approximately 15 min IV (30 min PO) and lasts approximately 4-6 hours, leaving time for corrective dosing in acute pain presentations [5, 7].
What if the patient is in severe pain? Should I start at a higher?
It’s important to remember that although analgesic control is the goal, this must be balanced with the risk of respiratory depression and over-sedation. Fortunately, there is a “1+1 Protocol”, which has been studied when treating moderate/severe pain. The “1+1” protocol indicates that a 1 mg HM IV bolus is given at baseline with a repeat 1 mg HM IV bolus at 15 minutes as needed based on pain severity. This protocol has shown analgesic efficacy with limited adverse effects in nonelderly patients in the ED presenting in moderate to severe acute pain [8]. The “1+1” protocol is also supported by a follow-up study comparing the protocol to a baseline 2 mg IV bolus. In this study, though both arms provided similar analgesic efficacy, the “1+1” arm had an opioid-sparing effect, as only one-third of the patients required the second dose at 15 minutes [9].
What are the major side effects we have to worry about with HM?
Side effects of HM are dose-dependent and similar to general opioids [2]. These include respiratory depression, miosis, cardiovascular depression (hypotension, bradycardia), pruritus (through histamine release), urinary retention, and constipation/gastrointestinal motility depression [10-12]. Respiratory depression is prominent among patients with obesity and sleep apnea, and opioids should be used cautiously among this population [13, 14]. If pruritus becomes intolerable, PO diphenhydramine can be administered (avoid IV diphenhydramine as this can worsen sedation, while offering limited pruritic relief) [15].
Respiratory depression is the leading preventable adverse side effect seen in the emergency setting secondary to inaccurate dosing [16, 17]. Doses as low as 1 mg IV HM have shown transient, self-resolving desaturations (<95% O2 saturation) though without the need for intervention [8]. 2 mg IV HM has been shown to cause desaturations (<95% O2 saturation) in up to one-third of patients, though this is successfully offset when co-administered with oxygen via nasal cannula [18]. Age is directly correlated with risk of desaturation, suggesting caution with higher dose usage in elderly populations [18].
How is HM metabolized? Can it be used in patients with renal disease?
Similar to oxymorphone and morphine sulfate, HM is independent of hepatic CYP450 metabolism, avoiding these drug-drug interactions [19, 20]. HM undergoes hepatic glucuronidation producing the primary metabolite, hydromorphone-3-glucuronide (H3G). H3G is neuroexcitatory, and excessive buildup can lead to myoclonus and seizure activity [7, 19, 21].
HM and its metabolites are renally excreted and should be avoided in patients with renal disease or dialysis [2, 22, 23]. However, HM metabolites are more efficiently dialyzed than morphine metabolites and thus better tolerated among patients who are to receive dialysis soon after administration [22, 23].
Can HM be used during pregnancy?
Opioids during pregnancy and lactation are considered relatively safe when used for short-term pain relief and under close observation [24]. Opioids can cross the placental barrier in small amounts, creating the particular concern for neonatal abstinence syndrome (NAS) when maternal administration occurs in the peripartum period [24-26]. In comparison, acetaminophen is listed as a Category B FDA rating for the first through third trimester of pregnancy secondary to a favorable safety profile [27, 28]. In mild to moderate pain, acetaminophen is considered the safest first line analgesic for pregnancy and lactation and should be considered over opioids [28].
A patient on my last shift told me they were allergic to morphine. Should I be worried?
Many patients report suspected ‘opioid allergies’ due the past production of symptoms such as hypotension and urticaria consistent with anaphylactoid reactions [29]. Though always a concern – particularly in the setting of swallowing difficulties, bronchospasm, and severe hypotension – true opioid anaphylaxis is rare, occurring in less than 2% of patients [29, 30]. With that said, consider alternatives if concerned for an allergic reaction.
We’re in the midst of an ‘opioid epidemic’. Are we talking about HM now?
Some very important ED research came out last week involving HM that we need to understand. With the upcoming patent expirations of IV acetaminophen, many researchers and ED providers believe this may be a feasible option for the treatment of acute pain in the ED. We discussed this a few months back on Pain Profiles in a comparison of IV and oral paracetamol. Unfortunately, prior literature has been poor comparing IV acetaminophen to opioids, which remain the preferable choice for moderate to severe pain. However, Barnaby, et al (Jacobi/Montefiore, Bronx NY) did just that in their RCT published last week comparing IV HM with IV acetaminophen in adult ED patients presenting with acute pain. 220 patients presenting in moderate/severe acute pain were randomized to receive either 1g acetaminophen or 1.0 mg hydromorphone, with primary outcome being a decrease in NRS (numerical rating scale, 0 to 10) at one hour. Their conclusion was that IV HM provides both clinically and statistically greater analgesia than IV acetaminophen, though with more nausea and vomiting (see infographic below).
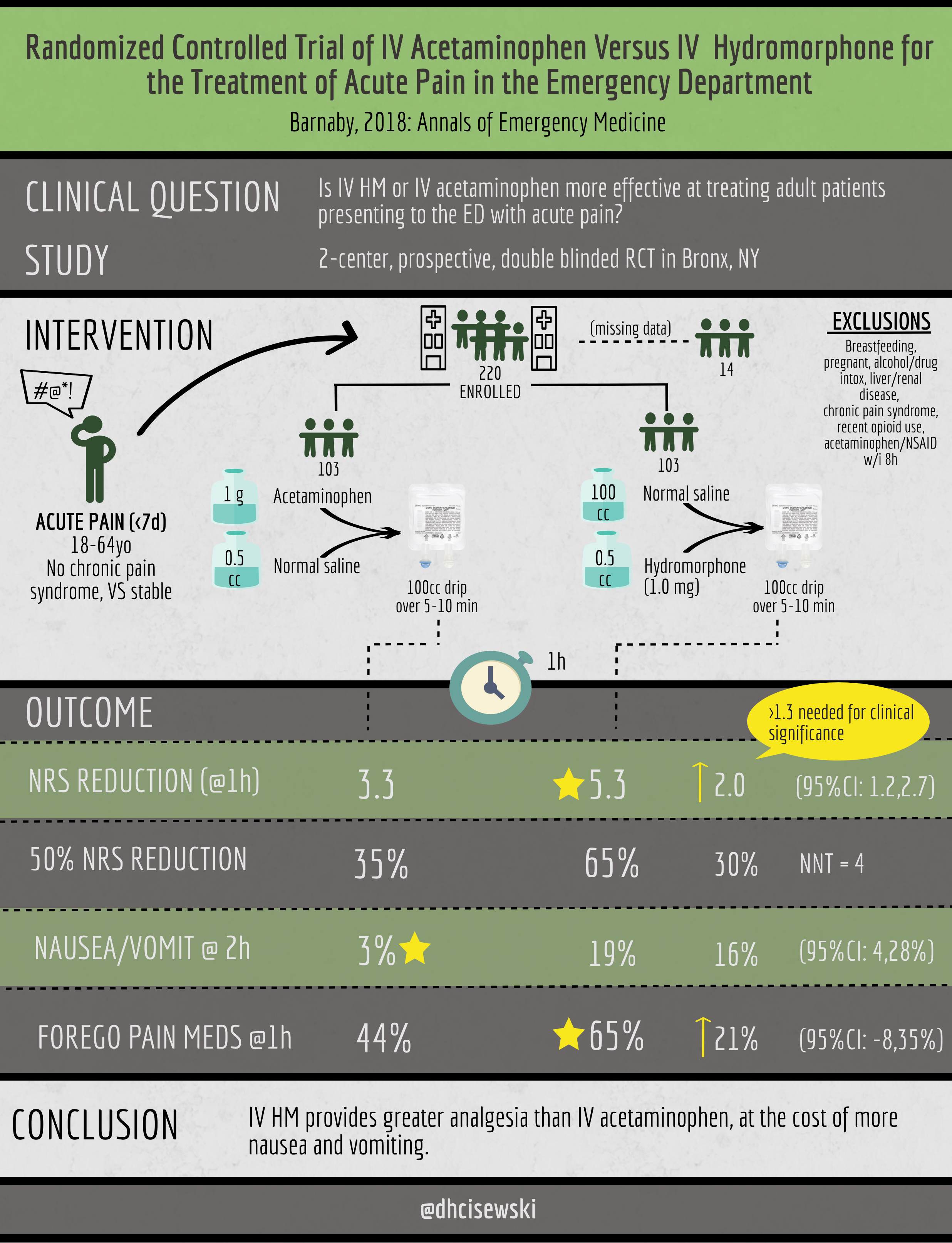
The importance of this study is that although IV acetaminophen may be a useful analgesic, it remains inferior to IV HM and should be considered when patients are presenting with moderate/severe pain.
The authors do note that this RCT included all patients with acute pain and may have therefore failed to identify particular subsets of patients presenting with acute pain who may have responded more or less favorably to hydromorphone or acetaminophen.
Interesting, you say, but this only looks at younger adults (<65yo) – What about older adults/geriatrics in which we worry about opioid side effects?
Fortunately, Chang, et al also just published research addressing this exact question (also out of the Bronx). They evaluated adults >64yo presenting to the ED with moderate/severe acute pain to see whether IV acetaminophen as an adjunct to IV HM was more effective at treating adult patients presenting to the ED with acute pain than IV HM alone. All patients were given 0.5 mg IV HM, and half were randomized to receive 1g IV acetaminophen. Primary outcome was a decrease in NRS (numerical rating scale, 0 to 10) at one hour. The outcome showed that IV acetaminophen as an adjunctive analgesic for acute, severe, pain in older adults provided neither clinically nor statistically superior pain relief when compared to HM alone for acute pain relief (see infographic below).

Speaking of acute pain… What about HM for migraines?
Of the 1 million patients presenting to the ED each year for migraine treatment, opioids are used in many treatment plans, with HM being the analgesic of choice in approximately one-fourth of the cases [31]. However, this is predominantly based on anecdotal evidence, and recent research by Friedman, et al has demonstrated non-opioid analgesics (prochlorperazine) have superior analgesic relief (see infographic below) [32]. Patients in this study were randomized to receive either 10 mg prochlorperazine + 25 mg diphenhydramine or 1 mg hydromorphone + normal saline (NS) placebo delivered in a 500cc NS bag over 5 minutes. Primary outcome was whether patients had a headache of mild/none at 2 hours and did not have a headache relapse at 48 hours. The study was terminated after 127 patients due to superiority of the prochlorperazine over hydromorphone treatment arm. The primary outcome of sustained 48-hour headache relief was achieved in 60% of the prochlorperazine arm vs 31% in the hydromorphone arm. Both groups had a similar ED length of stay, rate of headache relapse following discharge, and frequency of functional impairment.

Bottom line – between metoclopramide, prochlorperazine, occipital nerve blocks, etc, we have a sufficient tool box to avoid opioid use. See Dr. Friedman’s rundown on Headache Management at painandpsa for further discussion.
The Upshot
In the July 2018 EMA, Reflections of a Skeptic, Jerry Hoffman, MD reflected on the ‘abomination of an opioid-free ED’, pointing out opioids remain extremely effective analgesics in the ED and that the current opioid epidemic is not the result of opioid administration for patients in pain while in the ED. In August, 2018 EM:RAP, Al Sacchetti, MD made a similar ‘opioid rant’, pointing out that our focus on opioid addiction is minimalizing the indications for treatments with opioids. As Dr. Sacchetti points out, ‘don’t let patients suffer because you’re afraid to give opioids’. Be aware of equianalgesic dosing and remember that a “1+1” is not for everyone. Although hydromorphone is not for all pain presentations, it is effective for moderate and severe pain when used at appropriate doses.
Further Reading
- Emergency Physicians Monthly: Dilaudid in Detail: The Problem with Hydromorphone
References
- Sarhill, N., D. Walsh, and K.A. Nelson, Hydromorphone: pharmacology and clinical applications in cancer patients. Support Care Cancer, 2001. 9(2): p. 84-96.
- Mazer-Amirshahi, M., S. Motov, and L.S. Nelson, Hydromorphone use for acute pain: Misconceptions, controversies, and risks. J Opioid Manag, 2018. 14(1): p. 61-71.
- Knotkova, H., P.G. Fine, and R.K. Portenoy, Opioid rotation: the science and the limitations of the equianalgesic dose table. J Pain Symptom Manage, 2009. 38(3): p. 426-39.
- Choo, E.K., et al., The Prescription Opioid Epidemic: Social Media Responses to the Residents’ Perspective Article. Ann Emerg Med, 2016. 67(1): p. 40-8.
- PAMI. Pain Management and Dosing Guide. 2016; Available from: http://pami.emergency.med.jax.ufl.edu/.
- Ricket, A., et al., A pilot evaluation of a hydromorphone dose substitution policy and the effects on patient safety and pain management. J Pain Palliat Care Pharmacother, 2015. 29(2): p. 120-4.
- Trescot, A.M., et al., Opioid pharmacology. Pain Physician, 2008. 11(2 Suppl): p. S133-53.
- Chang, A.K., et al., Safety and efficacy of rapid titration using 1mg doses of intravenous hydromorphone in emergency department patients with acute severe pain: the “1+1” protocol. Ann Emerg Med, 2009. 54(2): p. 221-5.
- Chang, A.K., et al., Randomized clinical trial of the 2 mg hydromorphone bolus protocol versus the “1+1” hydromorphone titration protocol in treatment of acute, severe pain in the first hour of emergency department presentation. Ann Emerg Med, 2013. 62(4): p. 304-10.
- Mayer, D.J. and D.D. Price, Central nervous system mechanisms of analgesia. Pain, 1976. 2(4): p. 379-404.
- Wood, J.D. and J.J. Galligan, Function of opioids in the enteric nervous system. Neurogastroenterol Motil, 2004. 16 Suppl 2: p. 17-28.
- Holzer, P., Opioid receptors in the gastrointestinal tract. Regul Pept, 2009. 155(1-3): p. 11-7.
- Patanwala, A.E., et al., Should morphine dosing be weight based for analgesia in the emergency department? J Opioid Manag, 2012. 8(1): p. 51-5.
- Casati, A. and M. Putzu, Anesthesia in the obese patient: pharmacokinetic considerations. J Clin Anesth, 2005. 17(2): p. 134-45.
- Kumar, K. and S.I. Singh, Neuraxial opioid-induced pruritus: An update. J Anaesthesiol Clin Pharmacol, 2013. 29(3): p. 303-7.
- PPSA, Adverse drug events with hydromorphone: How preventable are they?, P.P.S. Advisory, Editor. 2010. p. 69-75.
- Beaudoin, F.L., et al., Preventing iatrogenic overdose: a review of in-emergency department opioid-related adverse drug events and medication errors. Ann Emerg Med, 2015. 65(4): p. 423-31.
- Chang, A.K., et al., Two milligrams i.v. hydromorphone is efficacious for treating pain but is associated with oxygen desaturation. J Opioid Manag, 2009. 5(2): p. 75-80.
- Smith, H.S., Opioid metabolism. Mayo Clin Proc, 2009. 84(7): p. 613-24.
- Vallejo, R., R.L. Barkin, and V.C. Wang, Pharmacology of opioids in the treatment of chronic pain syndromes. Pain Physician, 2011. 14(4): p. E343-60.
- Smith, M.T., Neuroexcitatory effects of morphine and hydromorphone: evidence implicating the 3-glucuronide metabolites. Clin Exp Pharmacol Physiol, 2000. 27(7): p. 524-8.
- Dean, M., Opioids in renal failure and dialysis patients. J Pain Symptom Manage, 2004. 28(5): p. 497-504.
- Ishida, J.H., et al., Opioid Analgesics and Adverse Outcomes among Hemodialysis Patients. Clin J Am Soc Nephrol, 2018. 13(5): p. 746-753.
- Wunsch, M.J., V. Stanard, and S.H. Schnoll, Treatment of pain in pregnancy. Clin J Pain, 2003. 19(3): p. 148-55.
- Baka, N.E., et al., Colostrum morphine concentrations during postcesarean intravenous patient-controlled analgesia. Anesth Analg, 2002. 94(1): p. 184-7, table of contents.
- Tolia, V.N., et al., Increasing incidence of the neonatal abstinence syndrome in U.S. neonatal ICUs. N Engl J Med, 2015. 372(22): p. 2118-26.
- Black, R.A. and D.A. Hill, Over-the-counter medications in pregnancy. Am Fam Physician, 2003. 67(12): p. 2517-24.
- de Fays, L., et al., Use of paracetamol during pregnancy and child neurological development. Dev Med Child Neurol, 2015. 57(8): p. 718-24.
- Baldo, B.A. and N.H. Pham, Histamine-releasing and allergenic properties of opioid analgesic drugs: resolving the two. Anaesth Intensive Care, 2012. 40(2): p. 216-35.
- Li, P.H., et al., Opioid Hypersensitivity: Predictors of Allergy and Role of Drug Provocation Testing. J Allergy Clin Immunol Pract, 2017. 5(6): p. 1601-1606.
- Friedman, B.W., et al., Current management of migraine in US emergency departments: an analysis of the National Hospital Ambulatory Medical Care Survey. Cephalalgia, 2015. 35(4): p. 301-9.
- Friedman, B.W., et al., Randomized study of IV prochlorperazine plus diphenhydramine vs IV hydromorphone for migraine. Neurology, 2017. 89(20): p. 2075-2082.






4 thoughts on “Pain Profiles: The “Dirty D” – Hydromorphone Use in The Emergency Setting”
In the UK, IV hydromorphone isn’t available and its PO indication is solely for “severe pain in cancer”. It is formulated as a standard tablet and a ‘modified release’ capsule.
What does this medication add, in its IV form, to an ED where morphine and fentanyl are already available?
Does it have a useful niche or is it part of the reason for the opioid epidemic in the US?
Fantastic visual abstracts!
These are all great questions, Dean. I would first point out that when compared to non-ED settings, emergency department opioid prescriptions have shown to be shorter in duration with less long-acting formulations, and associated with a lower risk of long-term opioid use progression (Jeffery, 2018; Ann of Emergency Medicine). That is to say, i don’t believe the ED was a major culprit in the opioid epidemic. Acute pain in an ED setting is a unique presentation and requires focused attention.
The interesting thing about Dilaudid is that the reason people argue against it now is the same reason many were arguing for it a decade ago. If you take a look at Chang, 2006 (Safety and Efficacy of Hydromorphone as an Analgesic Alternative to Morphine in Acute Pain: A Randomized Clinical Trial) you will see that it was studied specifically because morphine was being continually under-dosed in the ED setting resulting in poor pain control. Interestingly, health care providers who had an aversion to prescribing 7-10 mg IV morphine showed no qualms about 1mg hydromorphone (despite equianalgesic equivalency). Additionally, these authors pointed out that up to two-thirds of patients have been shown to have insufficient reduction of pain at 30 minutes post-administration (defined as pain reduction >50% of the baseline pain level) despite using the 0.1mg/kg IV dosing standard . Yet 1mg hydromorphone was resulting in superior pain relief and these researchers wanted something that successfully treated pain in the emergency setting. As stated by Chang, 2006, “Because morphine has been used in EDs for so many years, its inappropriately low dosing has been ingrained in the minds of emergency physicians and nurses. We believe that it will be easier to attack oligoanalgesia through introduction of another parenteral opioid with the proper dosing than to try to educate clinicians to use higher, more appropriately therapeutic doses of morphine.”
But a decade later, many are now concerned with how freely 1-2 mg of hydromorphone is given (because it sounds like a small dose – whereas few are willing to go above 7mg morphine), resulting in (over) sedation. Hence, the objective of this article – to provide an understanding of equianalgesic hydromorphone dosing and it’s role in acute pain setting. Could other medications be sufficient? Sure. Could hydromorphone be misused by providers who don’t understand it’s effects? Absolutely. But that’s not to say it can’t also be used to effectively treat acute pain in the acute, EMERGENCY setting. Our job as ED physicians is to understand the full armament of analgesics we have available in our toolbox and when to use them appropriately to optimally treat patients in pain.
To add one more point. The current concern re inappropriate hydromorphone is rightfully justified and excellently explained in the ‘further reading’ article by Dr. Motov who provides a thorough explanation of these mis-dosing concerns. ” Emergency Physicians Monthly: Dilaudid in Detail: The Problem with Hydromorphone”