Author: Lana Shaker, Emergency Medicine Resident (Rutgers New Jersey Medical School, Newark NJ) and Cynthia Santos MD (Assistant Professor Emergency Medicine, Medical Toxicology, Rutgers New Jersey Medical School) // Edited by: Alex Koyfman, MD (@EMHighAK, EM Attending Physician, UTSW / Parkland Memorial Hospital), and Brit Long, MD (@long_brit, EM Attending Physician, San Antonio Military Medical Center)

Case Presentation:
A 4-year-old girl is brought to the ED by parents with the complaint of chest pain and abnormal behavior, consisting of not talking and refusing PO intake. On exam, vital signs: BP 105/75 HR 122/min, RR 26/min, Pulse ox 98%. The child was restless, irritable, and held her neck in extension. Neck, chest, and abdomen x-rays were obtained.
Fig 1: Antero-posterior and lateral chest x-rays showing a radiopaque foreign body in the esophagus.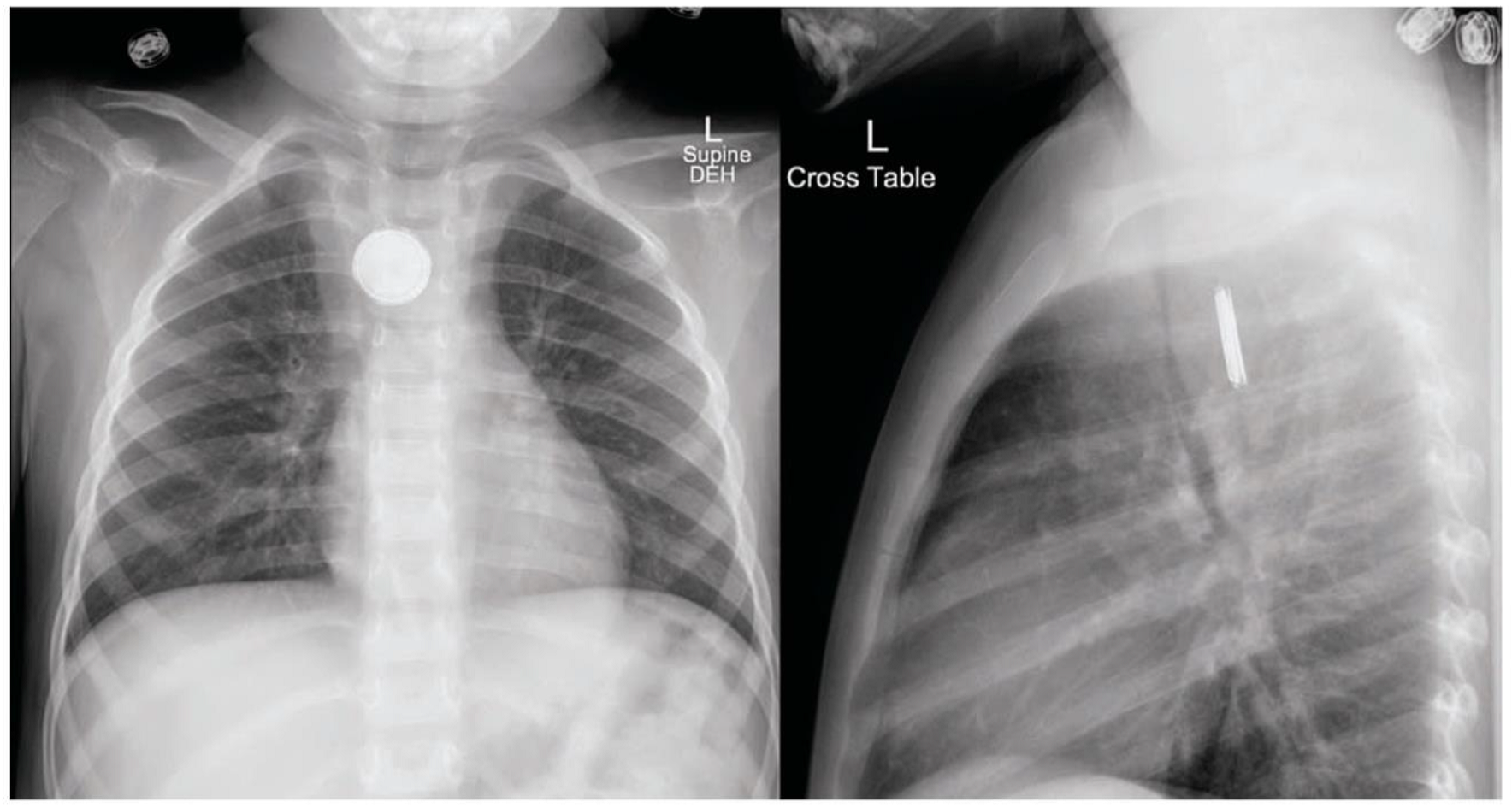
Image Reference: Tiedeken, SH., Shaffer SE., Worrisome chronic cough in a 3-year old girl. Contemporrary Pediatrics, 2014.
Questions
- When should button battery ingestion be suspected?
- How do button batteries cause tissue damage?
- How should these cases be managed??
- What are the long term sequelae of button battery ingestion?
Signs & Symptoms
- Signs and symptoms that any foreign body ingestion may have occurred, including button batteries, include chest or abdominal discomfort, dysphagia, drooling, difficulty swallowing, nausea and vomiting, decreased appetite or refusing to eat, coughing, choking, or gagging when attempting to eat, fever, irritability and listlessness. Signs of airway obstruction can include coughing, wheezing, stridor, increased work of breathing, and refusing to speak.[1]
Mechanism of Toxicity
- An electric current is generated when the battery comes in contact with mucosa, leading to localized burn injury.
- If the alkaline battery leaks, corrosive injury and liquefactive necrosis can occur. This is more common with non-lithium batteries and is usually not the cause of tissue damage that is seen to occur within 2 hours.
- The negative terminal, which is on the narrower side of the battery, generates hydroxide ions and is where necrosis occurs. A button battery moving freely does not generate enough hydroxide ions to produce focal damage. However, when the button battery becomes lodged (particularly in the esophagus and nostril) it can generate a focal collection of alkaline caustic material in a confined region that results in tissue necrosis.[1] This can be remembered as “narrow-negative-necrotic.”
- Batteries lodged in the esophagus may cause serious burns in as little as 30 minutes and the patient might be asymptomatic initially.[1]
- Certain button batteries carry greater risk than others. Patients with lithium battery ingestions have worse outcomes, as these have the potential to generate a higher current than other batteries and cause greater damage.[2, 3]
- Most batteries made in the USA do not contain added mercury since the “Mercury-Containing and Rechargeable Battery Management Act” was enacted in 1996 so mercury poisoning is not a concern.[4]
Management
- The airway should be stabilized if there are signs of airway compromise or obstruction.
- Particular care should be taken to examine the nose and bilateral ears for possible additional button battery insertions in these locations, as children may inadvertently place them in their ears or noses and tissue destruction can also occur in the ear or nasal mucosa.[5-8]
- DO NOT place a nasogastric tube, unless placed under direct visualization during endoscopy.
- Patients suspected of a button battery ingestion should be kept NPO and x-rays should be obtained of the neck, chest (AP and lateral), and abdomen as soon as possible. Infants can have a whole body x-ray, known colloquially as a “baby-gram.”
- Some research has shown that honey and sucralfate have protective effects in button battery ingestion due to neutralization of tissue pH leading to more localized and superficial injuries, which may reduce injury severity and improve outcomes. This research was only done on cadaveric pigs and although recommended by some poison control centers, it is still controversial and has not been widely adopted and/or recommended.[9]
- Look for the “double shadow” or “halo” appearance on X-ray (shown in Figure 2). These findings support the diagnosis of disc battery ingestion rather than a coin, though the absence of a “halo” does not rule out battery ingestion.Figure 2: Antero-posterior chest x-rays showing the “double shadow” or “halo” sign of a button battery on the left versus a coin on the right with the absence of the “halo”.
Figure 2: Antero-posterior chest x-rays showing the “double shadow” or “halo” sign of a button battery on the left versus a coin on the right with the absence of the “halo”.

Image Reference: Jatana, KR., Button Battery Injuries in Children: A Growing Risk. Everything Matters in Patient Care, 2013.
- Button batteries co-ingested with a magnet can attract and appose one another through walls of bowel loops, leading to injury, entrapment, or twisting of the bowel loops. There is no consensus on timing and manner of foreign body removal in these settings but these children should be admitted for observation with consultation to GI and/or pediatric surgery and there should be a low threshold for FB removal.[13]
- Batteries beyond the esophagus will pass usually without complications.[1-3,10-12]
- However if the child is symptomatic or it was co-ingested with a magnet – there is a low threshold to remove the battery no matter where it is.
- If the battery is in the stomach and child is asymptomatic, they can be discharged with expectant management and monitored with repeat x-rays.
- Batteries located in the esophagus must be endoscopically removed immediately (within 2 hours) and require emergent GI consultation.[1-3,10-12]
- Endoscopy is preferred over magnet retrieval mechanisms or balloon catheter. Endoscopy allows a direct assessment of injury severity and nasogastric tube placement under direct visualization.
- Endoscopy or surgery should not be delayed even if the child has recently eaten.
- During removal of the battery, note the position of the battery and direction of the negative pole during removal. Blind battery removal should not be performed.
- Ipepac, laxatives, and polyethylene glycol electrolyte solution administration should be avoided.
- Blood and urine concentrations of mercury, lithium or other battery contents is not needed.

Reference: Litovitz T, et al. Emerging battery-ingestion hazard: Clinical implications. Pediatrics 2010;125:1168-1177.
Complications
- Complications of button battery ingestions include severe GI and airway sequela like perforation, strictures, tracheoesophageal fistula, aorto-esophageal fistulas, vocal cord paralysis, mediastinitis, tracheal stenosis, tracheomalacia, aspiration pneumonia, empyema, lung abscess, pneumothorax, spondylodiscitis, or hemorrhage from vessel perforation.
- Management questions can also be directed to your regional poison center at 800-222-1222 and/or the National Battery Ingestion Hotline at 800-498-8666.

Reference: NBIH Button Battery Ingestion Triage and Treatment Guideline. National Capital Poison Control 2016; Available from: https://www.poison.org/battery/guideline.
Main Point:
There should be a high index of suspicion for button battery ingestions given the significant sequelae. Button batteries in the esophagus should be removed endoscopically immediately as necrosis can occur within 2 hours.
References:
- NBIH Button Battery Ingestion Triage and Treatment Guideline. National Capital Poison Control 2016; Available from: https://www.poison.org/battery/guideline.
- Litovitz, T., Whitaker, N., Clark, L., White, NC., Marsolek, M. Emerging battery-ingestion hazard: Clinical implications. Pediatrics 2010.
- JS, R., Coin-size lithium batteries can cause serious injury, death in a matter of hours if swallowed. AAP News, 2013.
- United States Environmental Protection Agency, “The Mercury Containing and Rechargeable Battery Management Act: Public Law 104-142”, 1996.
- McRae, D., Premachandra, DJ., Gatland, DJ. Button Batteries in the ear, nose, and cervical esophagus: a destructive foreign body. J Otolaryngol. 1989.
- Lin, YW., Daniel, SJ., Papsin, BC. Button batteries in the ear, nose, and upper aerodigestive tract. Otorhinolaryngology. 2004.
- Katana, KR. Button Batteries: Damaging if Swallowed, Put in Ears or Nose. American Academy of Pediatrics and American Society of Pediatric Otolaryngology. 2017.
- Tong, MC., Van Hasselt, CA., Woo, JK. The hazards of button batteries in the nose. J Otorlarnygol. 1992.
- Anfang, RR., Jatana, KR., Linn RL., Rhoades, K., Fry, J., Jacobs, IN., pH-Neutralizing Esophageal Irrigations as a Novel Mitigation Strategy for Button Battery Injury. The Laryngoscope, 2018.
- Tiedeken, SH., Shaffer SE., Worrisome chronic cough in a 3-year old girl. Contemporrary Pediatrics, 2014.
- Jatana, KR., Button Battery Injuries in Children: A Growing Risk. Everything Matters in Patient Care, 2013.
- Lee, JH., Shim, JO., Eun, BL., Yoo, KH., Foreign Body Ingestion in Children: Should Button Batteries in the Stomach Be Urgently Removed? Pediatr Gastroenterol Hepatol Nutr, 2016.
- Teague,WJ., Vaughan, EM., McHoney, M., McCabe, AJ., Swallowed Magnets and Batteries: A Dangerous but Not Unexpected Attraction. BMJ Case Reports,2013.









1 thought on “TOXCard: Button Battery Ingestions”
Pingback: Nursing FOAMed Review #5 (Sept 23rd - Oct 12th) - Code Blue LLC