Author: Chuck Pilcher, MD, FACEP (Editor, Med Mal Insights) // Editors: Alex Koyfman, MD (@EMHighAK) and Brit Long, MD (@long_brit)
Welcome to this month’s case from Medical Malpractice Insights – Learning from Lawsuits, a monthly email newsletter for ED physicians. The goal of MMI-LFL is to improve patient safety, educate physicians, and reduce the cost and stress of medical malpractice lawsuits. To opt in to the free subscriber list, click here.
Chuck Pilcher, MD, FACEP
Editor, Med Mal Insights
Knee dislocation: A vascular emergency
Patient loses leg due to delayed recognition, disorganized care
Facts (presented as timeline in hours:minutes post injury):
- Time zero: An adult female in her 30’s falls in her rural community and sustains a dislocated L knee. EMS transports her to the small local hospital.
- 0:20-1:40: Arrives in the ED and is seen by a PA. Distal pulses are present. An x-ray confirms the dislocation. The PA calls the family physician on call for the ED. An orthopedic surgeon at a distant second hospital is consulted. Recommendations include reduction, followed by transfer to a third hospital (closer to this ED) for vascular studies. Family physician comes to the ED.
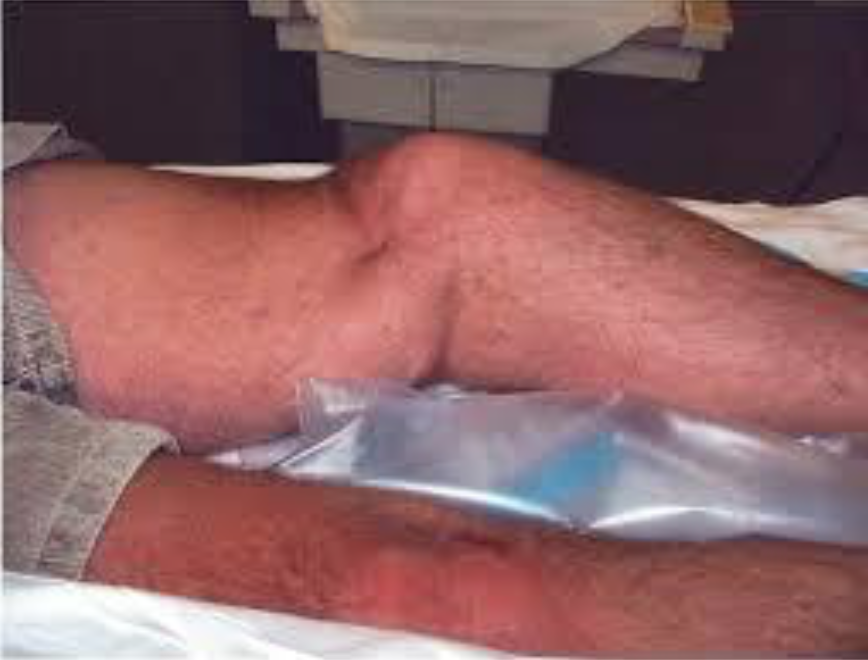
- 2:10: Reduction by the PA and family physician is completed under procedural sedation, after which distal pulses are absent. Transfer to the third hospital (not affiliated with the consulting orthopedic surgeon) is arranged.
- 4:53: Patient arrives at third hospital, now unable to wiggle toes or move L foot. Distal pulses are variably documented as present at triage but not present by subsequent Doppler.
- 6:00: Seen by the ED physician. A doppler ultrasound of the leg is ordered.
- 6:40: ED learns that no vascular surgeon is available in the community. Distal pulses and motor/sensory function variably documented as present and absent.
- 7:20: The Level I trauma center is contacted, heparin is begun, and transport arrangements are started.
- 7:45: Ultrasound is reported as abnormal. L foot is “white.”
- 8:28: Sensation decreased, motor absent.
- 9:23: Patient departs ED for major trauma center.
- 11 hours 30 minutes after injury, patient arrives at trauma center and is taken to the OR for vascular repair.
An amputation is eventually necessary. A lawsuit is filed against everyone involved.
Plaintiff: Every one of you dawdled around with my knee while my leg was dying. An orthopedic surgeon advised you that I needed vascular studies immediately, but you sent me to a hospital that had no available vascular surgeon. I needed my circulation restored within 6 hours. Because of you – all of you – and your substandard care, I lost my leg.
Defense: Each defendant pointed the finger at every other defendant.
“It was YOUR fault.”
“No, it was YOUR fault.”
“No, it was that OTHER doctor’s fault.”
“The knee should NOT have been reduced.”
“YES, it should have.”
“THEY transferred you to the wrong place.”
“YOU said you had a vascular surgeon.”
“YOU didn’t tell us she needed one.”
“She HAD pulses.”
“No, she DIDN’T.”
“We all did the best we could under the circumstances. Even if we did everything perfect, it wouldn’t have mattered.”
Etc., etc., etc…
Result: Settlement for undisclosed amount split amongst the various defendants.
Takeaways:
- Make sure all consultants and referral hospitals understand the patient’s injury and needs.
- Don’t become focused on how awful the joint looks. The danger lies in what you can’t see.
- It’s not about the bones. Whether pulses are present or not, whether reduction is done or not, a total knee dislocation is an orthopedic and vascular emergency.
- Admission is strongly advised. Continuous monitoring of the distal circulation is mandatory.
- Six hours is generally considered the maximum time a leg can survive with compromised circulation.
References:
- Knee Dislocation Clinical Presentation. Kelleher HB. Medscape eMedicine. Updated 8.24.2015 https://emedicine.medscape.com/article/823589-clinical#a0217
- EM Cases: Occult Knee Injuries Pearls and Pitfalls. Helman A. emDocs, Dec 29, 2017 http://www.emdocs.net/em-cases-occult-knee-injuries-pearls-pitfalls/
- Knee Dislocation: Pearls and Pitfalls. Singh M. emDocs, Apr 7, 2015 http://www.emdocs.net/knee-dislocation-pearls-and-pitfalls/
- Med Mal Insights case story of another knee dislocation: https://madmimi.com/p/ebcde5
“Be big enough to admit your mistakes, smart enough to profit from them, and strong enough to correct them.”
John C. Maxwell





