Originally published on Ultrasound G.E.L. on 5/20/17 – Visit HERE to listen to accompanying PODCAST! Reposted with permission.
Follow Dr. Michael Prats, MD (@PratsEM), Dr. Creagh Bougler, MD (@CreaghB), and Dr. Jacob Avila, MD (@UltrasoundMD) from Ultrasound G.E.L. team!
Point-of-care ultrasonography for evaluation of acute dyspnea in the emergency department
Chest Epub February 2017 – Pubmed Link
Take Home Points
1. POCUS in isolation had good correlation with diagnosis determined by emergency physician for patients with undifferentiated dyspnea.
2. POCUS lead to decreased time to diagnosis although limitations to the comparison.
3. POCUS showed overall high specificity and lower sensitivities for etiologies of acute dyspnea in the emergency department.
Background
Dyspnea as a presenting complaint to the ED is so common it’s not even funny. Point of care ultrasound can diagnose pulmonary edema, pneumothorax, pneumonia, pleural effusion, and pulmonary embolism by looking at the lungs. Then it can turn around and diagnosis right heart strain, global cardiac dysfunction, focal wall motion abnormalities, and pericardial fluid with echocardiography. Add in the IVC – and you probably have at least an idea of what is causing that patient’s symptoms. This paper takes a look at how accurate POCUS is in these patients in the emergency department.
Question
How accurate is combined heart, lung, and IVC ultrasound in determining diagnosis in an undifferentiated dyspneic patient in the emergency department?
Population
Inclusion
- Acute dyspnea (“acute” is not specified, possibly meant any dyspnea presenting to emergency department)
- adults > 18 years old
Exclusion
- Dyspnea from trauma
- Discharged from ED after evaluation
- Died in ED
- Did not consent
Design
Prospective, blinded, observational study
Consecutive patients enrolled
Study sonographer blinded to tests (aside from history, exam, and ecg potentially) compared to treating physician (blinded to POCUS). Both had to determine diagnosis which was compared to gold standard final diagnosis as determined by two emergency medicine experts by chart and diagnostic review including POCUS and any inpatient testing.
Up to two diagnoses could be selected
Calculated test characteristics of POCUS-informed diagnosis and compared to traditional ED work up.
Note: this is not the test characteristics of the POCUS exam for specific diseases – it is using the ultrasound to choose the most likely diagnoses (for example, if multiple findings like consolidation plus bilateral b lines but also enlarged right ventricle – they had to pick the most likely two diagnoses)
Intervention
All patients received:
(1). Routine evaluation (history, physical exam, electrocardiogram)
(2). POCUS performed
(3). As Needed:
– Chest xray
– Chest CT
– Cardiologist performed echo
– ABG
– Other blood tests
(4). Then the sonologist filled out a standardized form specifying what was most likely diagnosis (up to 2). The options were:
– Heart failure
– Acute coronary syndrome
– Pneumonia
– Pleural effusion
– Pericardial effusion
– COPD/Asthma
– Pulmonary embolism
– Pneumothorax
– ARDS/ALI
– Other: cancer, interstitial lung disease, psychogenic dyspnea, metabolic disorder, neurological disorder, musculoskeletal chest pain
Who did the scans?
10 EP sonographers
Professional course training of 80 hours
150 Lung US
150 echos
At least 2 years experience
The Scans
4-8 MHz linear probe
2.5- 3.5 MHz “curved array” probe


Their Protocol Order
- Lung ultrasound (LUS)
- Echo
- IVC
LUS
Long and oblique scans of anteriolateral and posterior thorax
Patient supine or near-supine, sitting if possible or lateral decubitus
Definitions
Pulmonary edema = diffuse interstitial syndrome
Pneumonia = lung consolidation and air bronchograms with or without focal interstitial syndrome
Pleural effusion = anechoic space between pleura
PE = two or more triangular or rounded pleural based lesions
COPD/asthma = absence of other findings with suggest medical history
Pneumothorax = no lung sliding, b-lines, or lung pulses AND lung point
ARDS = anterior subpleural consolidations with absence or reduction of lung sldiing, spared areas of normal parenchyma, pleural line abnormalities (irregularly thickened or fragmented, non homogenous distribution of blines)
Echo – two views
Apical four chamber – looking at ejection fraction (EF) and right ventricular dilation
Subcostal long axis – checking for effusion and evaluate EF also
Definitions
Low EF = < 50%
RV dilation = end diastolic diameter R:L >1 at level of AV valve annulus
IVC
Collapsibility index in subcostal view using Mmode 2 cm from RA junction
Definition
Reduced <50%, if 50 or above – normal or increased
They had a lot of focused questions in this study so there is not one video that captures every scan. That being said, here a bunch of them from 5 minute sono
Results
3487 patients with dyspnea from 1/2013 to 12/2013
- 734 discharged
- 57 trauma
- 7 no consent
- 6 died in ED
n = 2683
Patients
- Mean age 71.2
- Overall characteristics – on average not hypotensive, normal heart rate, RR 22.6
- 98% had CXR
- 11% had Chest CT
- 15% had comprehensive echo
Most Common Final Diagnoses:
- Pneumonia – 37.6%, n = 1086
- COPD/Asthma – 26.3%, n = 759
- Heart failure – 20.2%, n = 585
Primary Outcomes
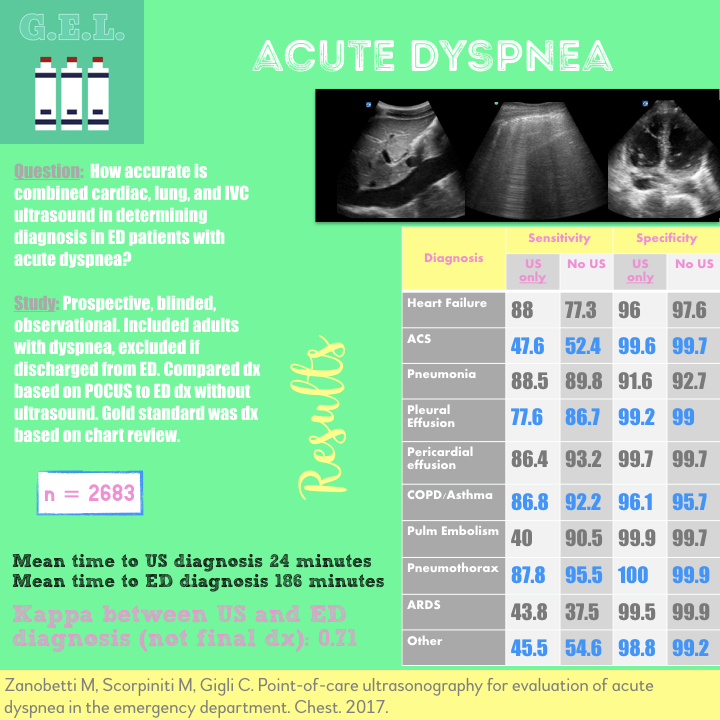
Concordance between US and ED diagnosis (not final diagnosis): Overall (from all diagnoses) kappa – 0.71 (“good”)
Kappa 0.8 was considered optimal in this study. The concordance was therefore optimal for heart failure, pericardial effusion, COPD/asthma, PTX. It was “good” for ACS, PNA, pleural effusion. It was “moderate” for PE and “poor” for ARDS/ALI.
My thought: who cares if it correlates with ED diagnosis if its not an accurate diagnosis? I think the authors were just trying to make a comparison to two diagnostic strategies here, but keep this in mind.
Test Characteristics of Ultrasound (blinded to most other clinical information) versus ED diagnosis (blinded to POCUS results)

That’s a lot of numbers. Here are points to notice from this data:
US significantly more sensitive for HF (88% vs 77,3%) and only slightly less specific (96% vs 97.6%
US less sensitive for COPD/asthma (87% vs 92%) and PE (40% vs 91% (likely because most got CT and ultrasound was only looking for RH strain and subpleural consolidations)
US less specific for ARDS/ALI but both were good (99.5% vs 99.9%)
All other differences not significant
Summary: US usually less sensitive but comparable specificity (and usually reasonably high specificity)
Other Findings
Mean time to US diagnosis 24 minutes
Mean time to ED diagnosis 186 minutes (p = 0.025)
- This was not exactly a fair comparison – see limitations.
Mean study time: 7±2 minutes (3 for Lung, 4 for echo)
97% of the PE patients (n=40) had RV dilation, only 66% had “pulmonary infarction” on CT. No false positives with RV dilation but 3 cases (5% of PE) of false positives with subpleural consolidations (patients had subpleural consolidation but no PE).
Ultimately 7.2% had two diagnosis by final diagnosis determination. Most commonly heart failure and pneumonia (36.2% of double diagnosis, 75 cases)
Limitations
Main limitation is that this is not how you are supposed to use diagnostic POCUS. The whole point is that the person performing the ultrasound is also caring for the patient and is therefore able to use ultrasound information in conjunction with clinical and other diagnostic tests. This study tests isolated ultrasound information (blinded to patient’s clinical information) and ED providers who were blinded to POCUS findings. Ideally, these are combined and therefore this study does not necessarily reflect conditions of clinical practice. A completely unblinded approach would have been more relevant information. If the POCUS clinicians had been able to see other diagnostics and response to treatment, they likely would have been more accurate than the EP diagnosis. It is unlikely that adding ultrasound would actually make your test characteristics worse (as it did in COPD and PE in this data).
There could have been a POCUS first arm versus not POCUS arm to determine if there was decrease in other diagnostics and overall decreased time to admission (or other patient centered outcomes).
Very experienced providers performing ultrasound (more than usual)
Blinding not complete – could have influenced POCUS providers decision for diagnosis; on the other hand (as mentioned above), this more accurately represents the clinical use of POCUS.
Excluded those discharged – probably because difficult to determine definitive diagnosis and the fact that they would be less likely to have most of the diagnoses assessed here. However, this is important in applying this data.
Did not look for DVT – did not want exam to be too time consuming. This could have improved test characteristics for PE.
Low prevalence of ARDS (n=16, 0.55%), can’t draw conclusions from this subset of the data.
US was included in the “Final diagnosis” assessment – this is practical, but may have biased the results towards supporting the US findings
The time comparison was not really a fair comparison. The ultrasonologists only had to complete the study on a single patient and make a diagnosis to stop the clock. The emergency physicians in the study presumably had more patients and other duties to attend to prior to deciding on a diagnosis.
Take Home Points
1. POCUS in isolation had good correlation with diagnosis determined by emergency physician for patients with undifferentiated dyspnea.
2. POCUS lead to decreased time to diagnosis although limitations to the comparison.
3. POCUS showed overall high specificity and lower sensitivities for etiologies of acute dyspnea in the emergency department.
Our score





1 thought on “Ultrasound G.E.L. – Acute Dyspnea”
Pingback: CRACKCast E213 – Dyspnea - CanadiEM