Welcome back to the “52 in 52” series. This collection of posts features recently published must-know articles. Our nineteenth post looks at the relationship between pediatric temperature and heart rate.

Author: Brannon Inman (Chief Resident, Emergency Medicine Physician, San Antonio, TX) // Reviewed by: Alex Koyfman, MD (@EMHighAK); Brit Long, MD (@long_brit)
Relationship Between Body Temperature and Heart Rate in Children With No Other Apparent Cause of Tachycardia
Question:
What is the normal heart rate range at various temperatures for children with no other apparent source of tachycardia?
Design: Retrospective observational cohort trial
PICO
Population:
- Retrospectively enrolled patients presenting to a single pediatric ED in Tokyo between April 2014 – March 2017
- The study attempted to select generally well patients (i.e., those less likely to have another driving cause of tachycardia)
- Included
- Otherwise well neonates to 18-year-olds
- Excluded
- No triage or no triage vital signs available
- Pt overstimulated or screaming in triage (documented by nurse as a standard in this hospital)
- Any patients requiring blood work (other than febrile 0-3 months old, which in this study period universally received blood work)
- Patients who were ultimately admitted
- The pediatric assessment triangle determined the patient was sick
- Triaged as emergent or needs resuscitation
- Hypoxia <94 %
- Cardiovascular complaints (palpitations, chest pain, etc.)
- Environmental/psychosocial stressors
- Drug overdose
- Ortho trauma/complaint
- Psych problems
- Bounce back in 7 days
- Severe disease as adjudicated by the physician
- Included

Intervention:
- No intervention evaluated, as this is a purely observational, retrospective evaluation
Comparator:
- Enrolled patients were compared to age-matched patients with a similar temperature
Outcome:
- Heart rate curves were sigmoidal for all age groups except the 0-3 month-old age group which was linear
- The 0-3 month-old age group also included the narrowest temperature range (36-38ºC)
- In most age groups, heart rate increased 4-10bpm/1ºC between 36-37ºC
- In all age groups, heart rate increased the steepest between 37-38ºC (increased 20bpm/1ºC)
- In most age groups, heart rate increased the increased 10-15bpm/1ºC between 38-39ºC
- In most age groups, heart rate increased the increased 13-10bpm/1ºC between 39-40ºC

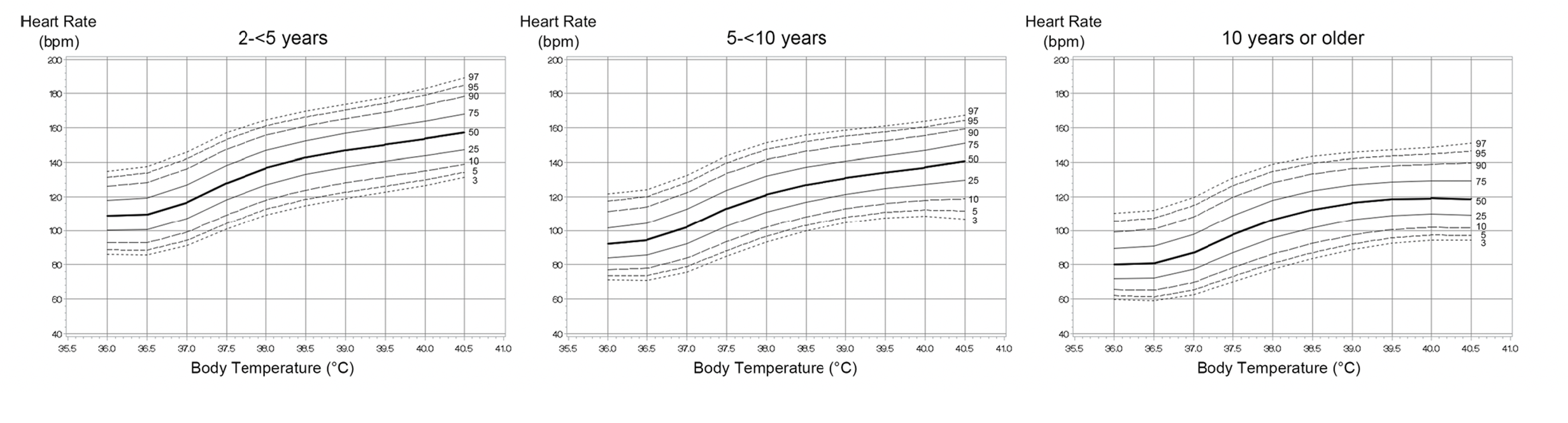
Take Aways:
- Overall, this was a fairly well-done look at the trends of heart rate and temperature with a large sample size. Pediatric patients of all ages were well represented.
- This was a single center in Japan and may not represent the patients in other countries.
- Most age groups displayed sigmoidal heart rate variability, except the youngest group. This may have been due to the differences in observed temperatures.
- This study focuses on otherwise well children. I think this is useful since when we look at the heart rate and decide if it’s proportional to the fever, it’s normally in patients we would like to discharge.
- Unfortunately, it appears many of the temperatures were obtained as axillary temperatures as this was the primarily reported triage method. While I understand this, it called in to question accuracy. Axillary temperatures are notorious for discrepant measurements. However, to this paper’s credit, this is how (reportedly) all triage measurements were obtained.
My Take:
- Contrary to the traditional teaching that the heart rate increases about 10 bpm for each degree Celsius above normal, the heart rate and temperature relationship appears to be sigmoidal (at least based on this study).
Please the AAP pediatric fever update on emDOCs Pediatric Small Talk.
References:
- Matsumura O, Morikawa Y, Kaneko T, Sakakibara H, Hagiwara Y. Relationship Between Body Temperature and Heart Rate in Children With No Other Apparent Cause of Tachycardia [published online ahead of print, 2022 Jan 18].Pediatr Emerg Care. 2022;10.1097/PEC.0000000000002617. doi:10.1097/PEC.0000000000002617





