Authors: Saran S. Pillai, MBBS (Medical Officer and Research Associate, Critical Care Medicine, KIMS hospital Trivandrum, Kerala, India) and Sameer Desai, MD, FACEP (@sameerdesai00, EM Attending Physician, University of Kentucky, Department of Emergency Medicine) // Edited by: Alex Koyfman, MD (@EMHighAK) and Brit Long, MD (@long_brit)
Case
A 32-year-old male presents with headache and intermittent clear discharge from the right nostril, not relieved by antihistamines or analgesics. Has a history of fall from height 2 days ago with no loss of consciousness, and he was evaluated at another hospital and discharged on pain meds. No further details areavailable. On examination, clear fluid is dripping from the right nostril, and the right ear examination using an otoscope shows hemotympanum.
Introduction
Basilar Skull Fracture (BSF) involving one of the five bones that form the base of the skull represents a life-threatening condition with high morbidity and mortality. They are relatively less common due to the resilience of the skull base (occurring in 4% serious head injury cases and up to 21% of all skull fractures)1 and need significant blunt trauma to occur.
They are mostly caused by high-impact blunt trauma such as motor vehicle accidents, with assaults, falls, andgunshot injuries being less common causes2,3. BSFs are most commonly found in younger males due to differences in high-riskactivity between sexes and age groups.
While most BSFs are managed conservatively in view of anticipated complications, it is important for the emergency physician to have a clearpicture of the management guidelines specifically with regard to presentation, evaluation, andcomplications.

Fig. 1: Fracture through the temporal bone on the right with associated opacification of the mastoid air cells. Image courtesy of Dr. Bruno Di Muzio. Radiopaedia.org rID: 12973.
Associations:
BSFs have a high risk for extra-axial hematomas, commonly epidural hematoma. This is due to the relative weakness of the temporal bone (most commonly affected bone in BSF) and its proximity to the middle meningeal artery and vein.
The likelihood of having BSF is significantly increased with a comorbid facial or skull fractures with the incidence of BSF directly linked to the number of facial fractures in the patient4–6. Similarly,50% of cases of BSF will have another intracranial injury, and 5-15% have an associated C-spine fracture7.
The most common BSFs involve the petrous portion of the temporal bone, the tympanic membrane, and the external auditory canal7,8.
Presentation
Clinical exam signs are relatively specific for BSFs in comparison to other skull fractures, due to the proximity of the skull base to cranial nerves, vessels, and dura that lie in its vicinity. Loss of consciousness and GCS score variesdepending on the bone that is fractured, but also on the degree of the associated brain injury.
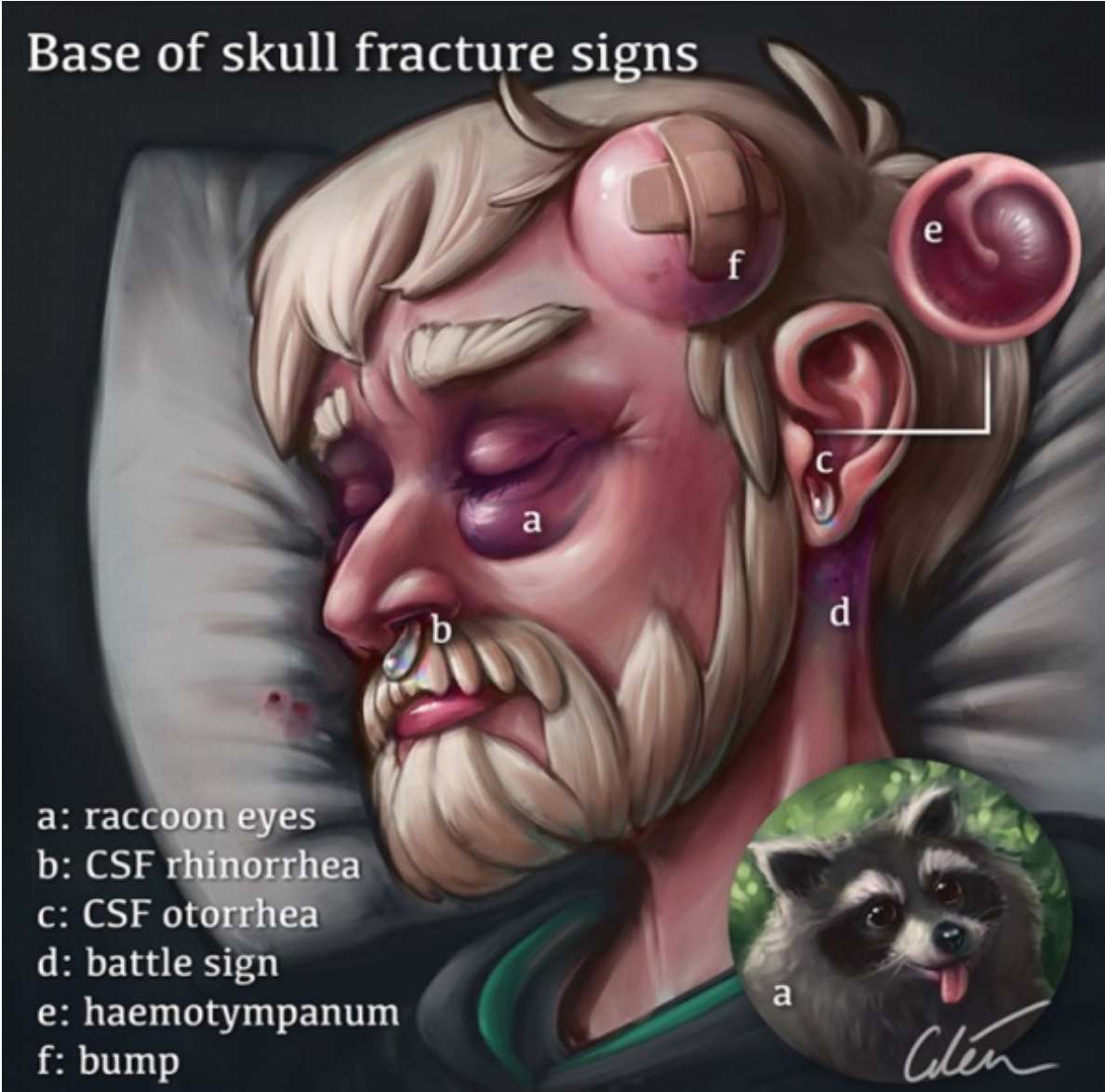
Fig. 2: Medical Illustration by Dr.Ciléin Kearns (Artibiotics).
The features most commonly associated with BSFs are:
- Hemotympanum
- Bloody Otorrhea
- CSF Rhinorrhea
- CSF Otorrhea
- Battle’s sign (mastoid ecchymosis)
- Raccoon eyes (periorbital ecchymosis)
- Cranial nerve deficits
- Decreased auditory acuity
- Tinnitus
- Dizziness
- Nystagmus
The positive predictive value in detecting a BSF is 100% for the Battle sign, 90% for a unilateral raccoon eye, and 70% for both bilateral raccoon eye and bloody otorrhea9. Some specific signs of BSF may also be considered as predictive for intracranial hematomas in patients with GCS of 13-15 with a PPV of 78% for Raccoon eyes, 66% for Battle’s sign, and 41% for bloody otorrhea9.
Hemotympanum recognized as a purple hue behind the tympanic membrane generally appears within hours of injury and is usually the first finding that could be seen in the ED10. One must consider the possibility of this being obscured by cerumen.
Battle sign and raccoon eye both typically may appear within 6 to 12 hours to 3 days after the fracture is sustained, and hence are not commonly found during initial ED presentation11. Dr. Battle reported his eponymous sign in 1890 and also found that when mastoid ecchymosis is present, the patient is more likely to have a slower course of recovery from head injury than expected12,13.
CSF leaks, considered pathognomonic for a BSF and associated dural tear, manifest as either otorrhea or rhinorrhea and occur in 2% of all head traumas and 12% to 30% of all BSF14,15. These leaks can develop within one to several days following injury with the patient often complaining of clear discharge from the nose or ears. 50% of cases appear within the first 2 days, 70% in one week, and almost all seen within 3 months14. Intermittent leaks are common and thus are often missed on evaluation in the ED. Thorough history regarding nature, consistency, and precipitating and relieving factors of CSF leak can assist.
Middle/Inner ear injury follows in up to 33% of patients with serious head trauma and over 50% ofpatients with temporal bone fractures15,16. These injuries include hemotympanum, hearing loss, disruption of the ear ossicles, cerebrospinal fluid (CSF) fistula, otic capsule injury etc.17,18. Hemotympanum or CSF middle ear effusion following a BSF can cause a conducting hearing loss while damage to the otic ganglion and cranial nerve can cause a sensorineural hearing loss19.
Cranial nerve and vascular lesions can occur according to the part of the skull base that is fractured and the nerves and vessels that lie in its vicinity.

Fig. 3: Associations of Basilar Skull fracture by the location of the defect. (Cranial nerve deficits are in italics).
Complications:
Complications associated with BSF include:
- Cerebrospinal fluid leak/fistula
- Meningitis
- Pneumocephalus
- Hearing loss
- Vertigo
- Cranial Nerve Injury
- Cavernous sinus thrombosis
- CerebroVascularInjury (CVI)
- Carotid-cavernous fistula
- Intracranial hemorrhage (ICH)
Delayed development of complications associated with BSF like cranial nerve deficits, CSF leak, carotid/vertebral artery injury are the norm and typically present after 48 hours.
85% of traumatic CSF leaks resolve spontaneously within a week,but some rarely can persist for as long as several months. Less than 5% of patients with BSF develop meningitis, but the risk is related to the duration of the CSF leak with a prevalence of 3% if the leak lasts less than 1 week, and 50% if it persists for more than 2 weeks20–22. Meningitis and CSF leak following isolated skull base fractures are rare in both children and adults, with low rates of meningitis (0.48% and 0.64%) and CSF leak (2.33% and 1.75%), respectively. The median time between the traumatic CSF leak and the onset of meningitis approaches 11 days22–24.
In 10-50% cases of BSF, a pneumocephalus may occur immediately or arise chronically as a sequelaof a CSF fistula20,25. Rarely, progressive accumulation of air, especially after delivery of positive airway pressure during resuscitation can lead to a tension pneumocephalus with mass effect and increased intracranial pressure26.
Temporary conductive deafness that resolves in 1-3 weeks is due to hemotympanum or mucosal edema in the middle ear cavity. Classifying temporal bone fractures into ‘Otic capsule sparing’ (OCS) and ‘Otic capsule violating’ (OCV) correlates well with the severity of the hearing loss, the prognosis of the patient, and residual disability27. 60.5% of patients with temporal bone fractures reported hearing loss, with OCS accounting for 91.5% of fractures and OCV accounting for 8.5%18,28 of temporal bone fractures. OCS usually causes a conductive or mixed hearing loss, while OCV fractures will almost always lead to a sensorineural hearing loss.
Cranial nerve deficits, as described in Figure 3, are most commonly due to entrapment rather than transection of the nerve. Anosmia due to CN I damage occurs in as many as 7% of anterior skull-base fractures. Only 10% of these patients will recover their sense of smell, usually in a delayed fashion of months to years29. Traumatic facial nerve palsy can either be immediate and complete due to nerve transection or delayed and incomplete due to neuropraxia. Delayed facial nerve paralysis is associated with normal or near normal recovery within months to a year in most patients and can be treated with corticosteroids18,30.
Approximately 50% of patients with BSF can present with delayed ischemic brain damage due to an associated evolving ICH over 12-24 hours31. 50% of patients with BSF will have another intracranial injury on CT28.
Central skull base fractures are usually associated with vascular complications, with a predisposition for the internal carotid and basilar arteries (Carotid>basilar) due to their course close to the temporal bone and sphenoid sinuses. Carotid artery injury is seen in 2-35% of patients with BSF32,33. Vascular complications include occlusion, compression, dissection or transectionof the carotid artery by fracture fragments, or formation of a pseudoaneurysmor a carotid cavernous fistula (CCF) secondary to injury. With an overall incidence of 3.8 % in BSF, CCF can result in blindness, stroke, or even death34. Acute injury to the internal carotid artery may be either asymptomatic or result in fatal bleeding. Although only a minority of carotid canal fractures result in vascular injury14, injury to the internal carotid artery are nearly always observed when the carotid canal is fractured35. Carotid artery injury, when overlooked, is associated with severe permanent neurologic deficit or death in up to 50% cases. Carotid artery injuries can also lead to a stroke due to arterial dissection in up to 31% of cases33.
Diagnosis
Physical examination findings suggestive of a BSF have a sensitivity of 71.2% and specificity of 90.1% for the diagnosis of BSF36. Research performed to validate the Canadian Head CT rule and other smaller observational studies showed that the signs of BSF (ie, Battle sign, raccoon eyes, hemotympanum, otorrhea/rhinorrhea) collectively are highly predictive of a clinically important head injury9,37,38. However, physical exam misses 14-35% of radiographically visible temporal bone fractures9,39,40.
Plain Xray can miss as many as 70-80% of fractures and are not recommended to evaluate for basilar skull fracture5.
CT is considered to be the imaging modality of choice. The sensitivity of CT scan for basilar skull fractures is low with CT scans with 5-mm axial sections having sensitivities of 50% to 71% for identifying BSF41,42. A high spatial resolution CT scan with 1-1.5 mm thin sliced bone windows with reconstruction is the fastest and best method to delineate a BSF with a 25% improved sensitivity41,43. Multidetector CT scans (MDCT) with multi-planar reconstructions may be required for the diagnosis of BSF and its associated complications, especially maxillofacial, head, and cervical reconstructions which are studies that are routinely done in patients with polytrauma in the ED44. Helical CT scan is helpful in occipital condylar fractures45. A key concern with BSF imaging is to differentiate them from accessory sutures as both can appear very similar. In comparison to fractures, accessory sutures are usually less than 2 mm in width, have a uniform thickness throughout, and are lighter radiologically.
A CT angiogram is advised in a patient with an already established BSF, if the chances for a cerebrovascular injury (CVI) are high as listed in fig. 546.
MRI also plays a role in BSF imaging due to its better soft tissue imaging detail, which is used to highlight CSF leaks or fistulas or arachnoid herniations (T2 fat sat), and cranial nerves (heavily T2 weighted thin slice images)47. MR cisternography has a sensitivity of 90% for traumatic CSF leaks, compared to 60-80% for the more invasive CT cisternography which requires an intrathecal administration of radiopaque contrast during the procedure48,49. However, MRI is often not available in the ED.
CSF from a suspected CSF otorrhea/rhinorrhea placed on a piece of filter paper will result in separation of blood and CSF (central blood with a clearing around) which is known as the halo/ring sign. However, it lacks specificity as it will return a positive result with blood mixed with water, saline, and mucus50.
Crude methods of detecting CSF leak like analysis of glucose and protein content of secretions is a safe noninvasive method, with a limited diagnostic value due to contamination with blood, lacrimal secretion or saliva51. An elevated glucose value and lower protein level supports CSF leak, rather than other sources of nasal discharge. However, these tests have variable sensitivity/specificity and require further study before they are routinely used to diagnose CSF leak.
Fluid suspicious for CSF may be collected and sent for analysis for identification of β transferrin, the β2 transferrin isoform found only in CSF52. The high sensitivity and specificity of this test are unmatched by other noninvasive methods, and the test can be performed easily even for intermittent leaks53. However,it can be impractical in the ED due to the volume of CSF needed (0.5 cc) and the delay in test results (up to 4 hours)46.
Management:
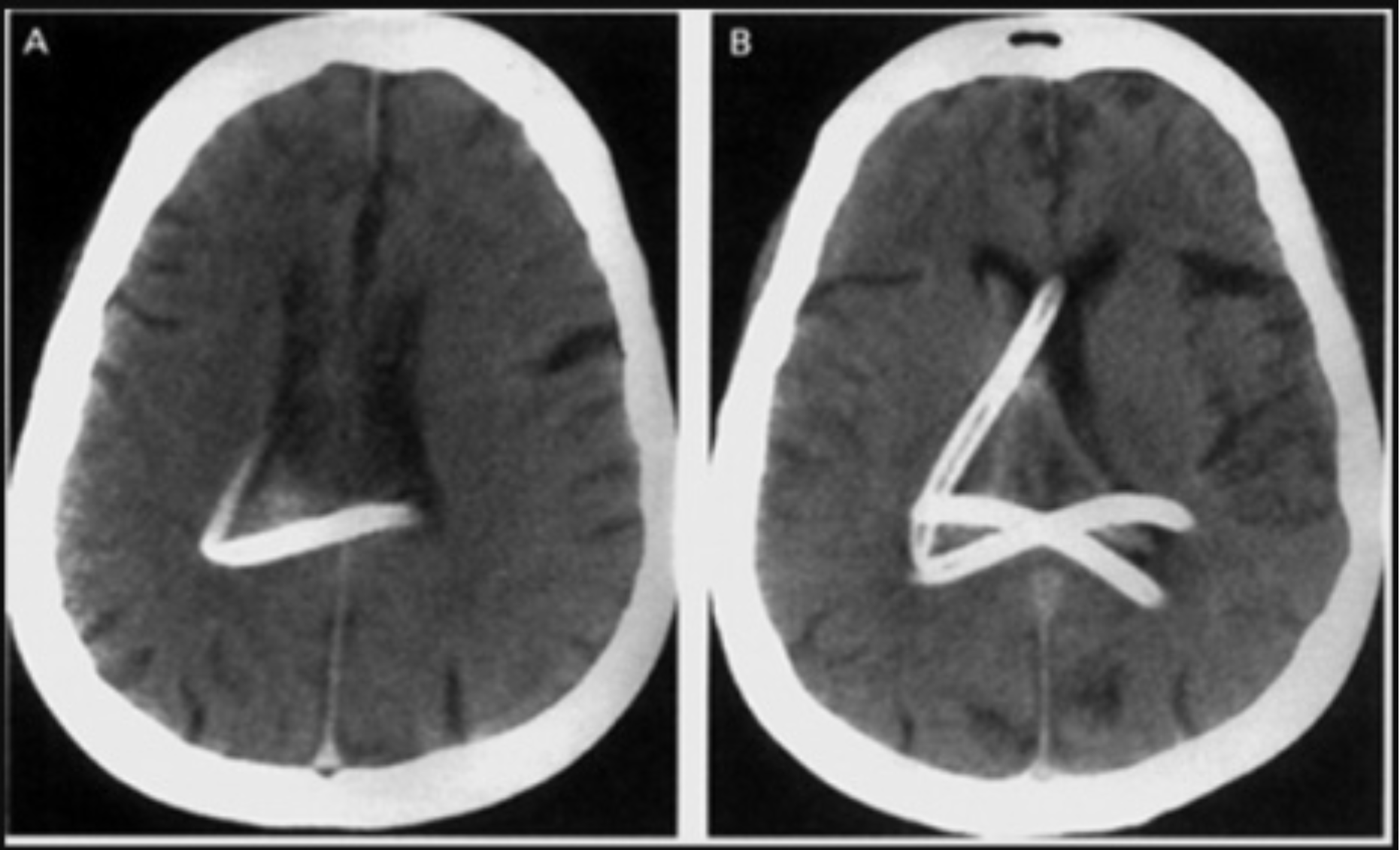
Fig. 4: ‘Food for thought’ – Avoid nasogastric intubation in BSF patients. https://jordynredwood.files.wordpress.com/2013/08/d15e8-ngct.jpg.
When there is facial trauma or evidence of BSF, nasogastric intubation and nasopharyngeal suction are not recommended54. Gastric decompression with the orogastrictube is a better choice55. NIPPV should likely be avoided as well in patients with potential BSF due to the risk of pneumocephalus7. In asymptomatic patients with radiological evidence of pneumocephalus, bed rest with 100% oxygen to wash out nitrogen and decrease intracranial gas has been proposed29.
Definitive treatment measures typically begin with conservative treatment for a non-displaced fracture, with surgical intervention saved for severe or persistent disease. Conservative management for CSF leaks includes strict bed rest, head of bed elevation >30 degrees, and sinus precautions (avoiding coughing, sneezing or straining), which has resolution rates of 85% after 1 week. A Cochrane review analysis concluded that there is not enough evidence for prophylactic antibiotics in BSF, with or without evidence of CSF leakage56. Patients with a CSF leak should receive both the pneumococcal conjugate vaccine and the pneumococcal polysaccharide vaccine57. Tetanus vaccination should be offered if the patient has not received immunization within the last 5 years58. Patients should be treated with broad-spectrum antibiotics if they have an open wound or if the presentation has been delayed.
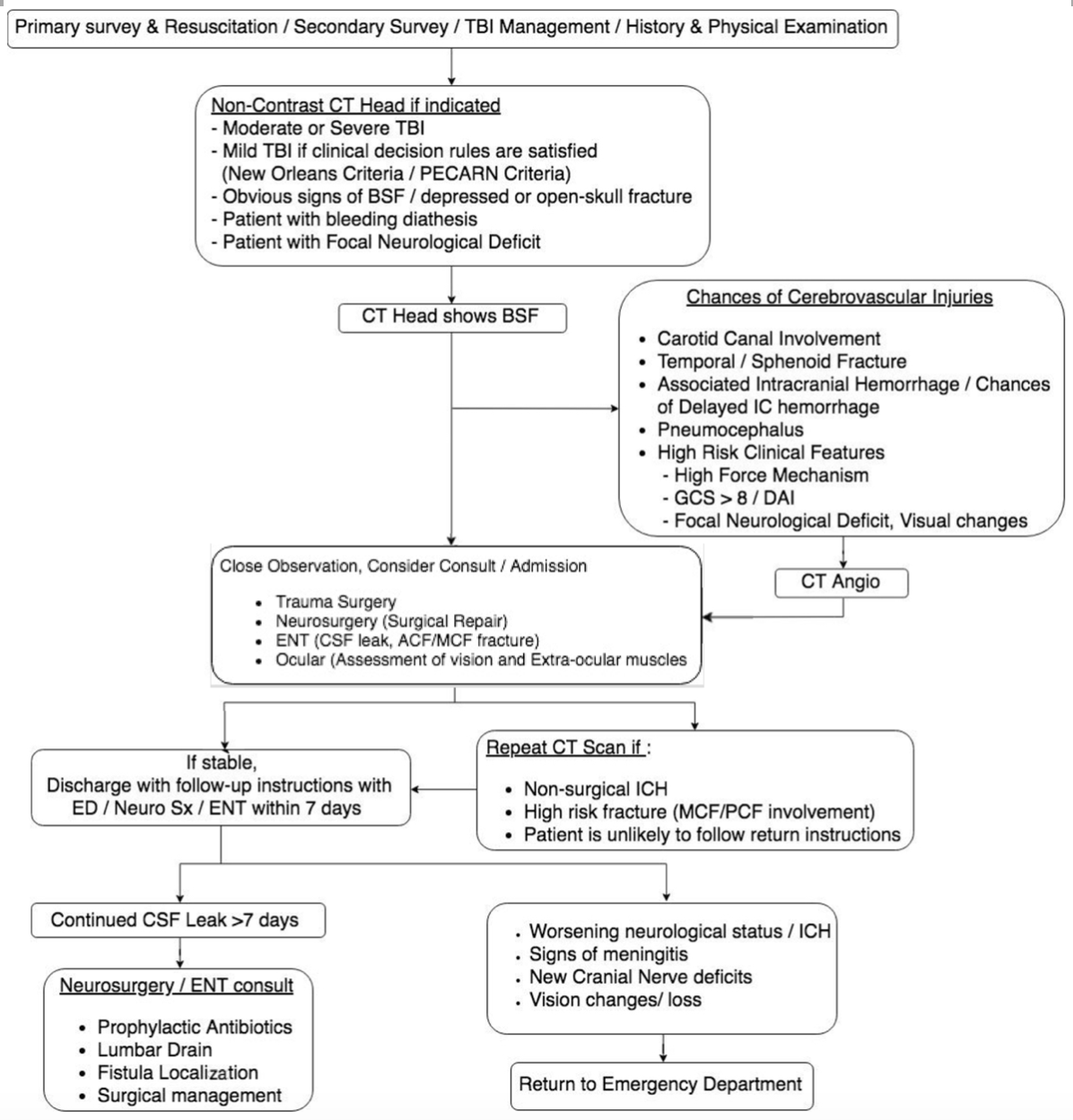
Fig. 5: Flowchart to the management of a BSF at the ED with guidelines to imaging, consultation, and follow-up.
The following are some guidelines that could help the emergency physician in decision making regarding admission/consult/disposition46.
When to consider consult/hospital admission?
Patient has been sufficiently evaluated and there is evidence of:
- Altered level of consciousness compared to patients baseline
- Presence of associated non-surgical ICH
- Presence of any other high-risk clinical features (eg. high impact mechanism of injury, alteration of the GCS, Diffuse axonal injury, middle or posterior fossa involvement, suspicion of CVI) that need close observation/ repeat/additional imaging.
- CVI requiring observation/additional management
- Presence of CSF leak or cranial nerve deficits
- Features indicative of meningitis in a settingof suspected CSF leak
- Patient or ED related factors that prevent safe observation/discharge preparation/adequate follow-up
Whom to consult?
All Consults should focus on establishing further imaging, determine the need for transfer/admit/repeat imaging, and also ensure follow-up, especially in case of CSF leaks and CN injury.
ENT consultation is necessitated in cases of CSF leak, and/or ACF/MCF fracture; Ophthalmology consultation for detailed evaluation of vision and extraocular muscles; and Neurosurgery consultation to consider definitive management.
Regarding definitive management, basilar fractures seldom need surgical repair, but when there is the persistent CSF leak, cranial nerve compression, or increased intracranial pressure, operative repair may be indicated39. If the CSF leakage is persistent after 7 days, the surgical treatment of choice is endoscopic endonasal surgical repair, which has a better outcome and lower morbidity compared to the intracranial approach59. Operative repair may be required for persistent cranial nerve injury (hearing loss persisting for >3 months, facial paralysis), but there is little evidence that surgical treatment of facial paralysis is superior to conservative treatment60,61.
Overall, most patients with BSF do have some type of residual functional or neurological deficit which may take months or even years to reverse21,62.
When can you consider discharge?
Patient has been sufficiently evaluated with:
- CT head/CT angiogram
- Cranial nerve examination including visual acuity and olfactory sensation
- C spine injury excluded
And found to have an isolated BSF or a linear skull fracture but no symptoms of CSF leak or cranial nerve deficits, or no radiological evidence of CVI or other associated injuries.
Return instructions must be given for signs/symptoms of:
- Delayed ICH, CVI (focal neurological deficits)
- New onset Visual changes
- New onset Cranial nerve damage
- New onset CSF leak – continuous or intermittent
- Symptoms of meningitis
Reassessment at 7 days for development of any of the above is important either at the level of primary care or consult services.
From Dr. Katy Hanson at Hanson’s Anatomy:

Pearls and Pitfalls:
- Battle sign and raccoon’s eye may be delayed 6-12 hours or not present with BSF.
- Hemotympanum is typically first finding.
- Most complications of BSF like CSF leak, cranial nerve deficits, and sequelae of carotid/vertebral artery injury arise late and present after 48 hours.
- Consider abuse in elderly and children.
- Consider meningitis if prolonged CSF leak.
- No evidence for prophylactic antibiotics regardless of CSF leak.
- Consider CTA to evaluate for carotid artery injury regardless of cervical fracture.
- Missed CVI can lead to permanent neurologic sequelae or mortality in up to 50% cases.
- Avoid nasogastric intubation, nasopharyngeal suction / airway, and NIPPV if potential BSF.
Case Conclusions
On further examination, the patient had neither other neurological deficits or neck stiffness. He was GCS-15, alert oriented and hemodynamically stable. His previous CT scan from 2 days previously was reviewed, which showed a questionable fracture in the petrous part of the temporal bone. He was kept on close observation with strict bed rest, head of the bedelevation, and advised not to cough, stress or sneeze. Clear fluid from the nose was collected and sent for analysis and β transferrin assay. ENT was consulted in view of CSF leakage and Neurosurgery in view of thehigh-risklocation of the fracture. A high-resolutionCT scan of the head was done to rule out a repeat ICH and also to localize the site of the CSF leak. This showed fractures at the level of the cribriform plate, with a fracture at the petrous part of the temporal bone on the right side. There were no associated intracranial hemorrhages or other associated lesions. A Ct angiogram was also done in view of the high-risklocation of the temporal bone fracture, which was normal. Further cranial nerve examination showed that the patient also had anosmia. The β transferrin assay returned positive for CSF. He was observed and discharged with close follow up.
References/Further Reading:
- Potapov AA, Gavrilov AG, Kravchuk AD, et al. [Basilar skull fractures: clinical and prognostic aspects]. Zh Vopr Neirokhir ImN N Burdenko. 2004;(3):17-23; discussion 23-24.
- Wang H, Zhou Y, Liu J, Ou L, Han J, Xiang L. Traumatic skull fractures in children and adolescents: A retrospective observational study. Injury. 2018;49(2):219-225.
- Wani AA, Ramzan AU, Raina T, et al. Skull base fractures: An institutional experience with review of literature. Indian J Neurotrauma. 2013;10(2):120-126.
- Gerbino G, Roccia F, BenechA, Caldarelli C. Analysis of 158 frontal sinus fractures: current surgical management and complications. J Cranio-Maxillo-fac Surg Off Publ Eur Assoc Cranio-Maxillo-fac Surg. 2000;28(3):133-139.
- Johnson F, Semaan MT, Megerian CA. Temporal bone fracture: evaluation and management in the modern era. Otolaryngol Clin North Am. 2008;41(3):597-618, x.
- Slupchynskyj OS, Berkower AS, Byrne DW, Cayten CG. Association of skull base and facial fractures. The Laryngoscope. 1992;102(11):1247-1250.
- Tintinalli’s Emergency Medicine: A Comprehensive Study Guide, 8e | AccessEmergency Medicine | McGraw-Hill Medical. https://accessemergencymedicine.mhmedical.com/book.aspx?bookID=1658. Accessed March 6, 2019.
- Cranial Vault & Skull Base – Diagnosis – AO Surgery Reference. https://www2.aofoundation.org/wps/portal/!ut/p/a1/04_Sj9CPykssy0xPLMnMz0vMAfGjzOKN_A0M3D2DDbz9_UMMDRyDXQ3dw9wMDAx8jYEKIvEocDQnTr8BDuBoQEi_l35Uek5-EtipkY55ScYW6fpRRalpqUWpRXqlRUDhjJKSgmIrVQNVg_Lycr30_Pz0nFS95PxcVQNsWjLyi0v0I1BV6hfkhkZU-aSGAwDYYmkN/dl5/d5/L2dJQSEvUUt3QS80SmlFL1o2XzJPMDBHSVMwS09PVDEwQVNFMUdWRjAwMFE1/?bone=CMF&segment=Cranium&showPage=diagnosis. Accessed March 8, 2019.
- Pretto Flores L, De Almeida CS, Casulari LA. Positive predictive values of selected clinical signs associated with skull base fractures. J Neurosurg Sci. 2000;44(2):77-82; discussion 82-83.
- Hasso AN, Ledington JA. Traumatic injuries of the temporal bone. Otolaryngol Clin North Am. 1988;21(2):295-316.
- Tubbs RS, Shoja MM, Loukas M, Oakes WJ, Cohen-Gadol A. William Henry Battle and Battle’s sign: mastoid ecchymosis as an indicator of basilarskull fracture. J Neurosurg. 2010;112(1):186-188.
- EpperlaN, Mazza JJ, Yale SH. A Review of Clinical Signs Related to Ecchymosis. WMJ Off Publ State Med Soc Wis. 2015;114(2):61-65.
- BattleWH. Three Lectures on Some Points Relating to Injuries to the Head. Br Med J. 1890;2(1540):4-10.
- Lemole M, Behbahani M. Retrospective Study of Skull Base Fracture: A Study of Incidents, Complications, Management, and Outcome Overview from Trauma-One-Level Institute over 5 Years. J Neurol Surg Part B Skull Base. 2013;74(S 1):A239.
- Lee D, Honrado C, Har-El G, Goldsmith A. Pediatric temporal bone fractures. The Laryngoscope. 1998;108(6):816-821.
- Zimmerman WD, Ganzel TM, Windmill IM, Nazar GB, Phillips M. Peripheral hearing loss following head trauma in children. The Laryngoscope. 1993;103(1 Pt 1):87-91.
- Kim SH, Kazahaya K, Handler SD. Traumatic perilymphatic fistulas in children: etiology, diagnosis andmanagement. Int J Pediatr Otorhinolaryngol. 2001;60(2):147-153.
- Brodie HA, Thompson TC. Management of complications from 820 temporal bone fractures. Am J Otol. 1997;18(2):188-197.
- Otic barotrauma from air travel. – PubMed – NCBI. https://www.ncbi.nlm.nih.gov/pubmed?term=15949100. Accessed March 8, 2019.
- Bobinski M, Shen PY, Dublin AB. Basic Imaging of Skull Base Trauma. J Neurol Surg Part B Skull Base. 2016;77(5):381-387.
- McCutcheon BA, Orosco RK, Chang DC, et al. Outcomes of Isolated Basilar Skull Fracture: Readmission, Meningitis, and Cerebrospinal Fluid Leak. Otolaryngol Neck Surg. 2013;149(6):931-939.
- Baltas I, Tsoulfa S, Sakellariou P, VogasV, Fylaktakis M, Kondodimou A. Posttraumatic meningitis: bacteriology, hydrocephalus, and outcome. Neurosurgery. 1994;35(3):422-426; discussion 426-427.
- van de Beek D, Drake JM, Tunkel AR. Nosocomial bacterial meningitis. N Engl J Med. 2010;362(2):146-154.
- Choi D, Spann R. Traumatic cerebrospinal fluid leakage: risk factors and the use of prophylactic antibiotics. Br J Neurosurg. 1996;10(6):571-575.
- Gautschi OP, Zellweger R. Asymptomatic posttraumatic pneumocephalus. Am J Emerg Med. 2006;24(5):628-629.
- Youngblood SC, Baig HR. Images in anesthesiology: pneumocephalus resulting from basilarskull fracture. Anesthesiology. 2015;122(5):1152.
- Maradi N, M SB. Hearing loss following temporal bone fractures- a study on classificationof fractures and the prognosis. Int J Otorhinolaryngol Head Neck Surg. 2017;3(2):390-394.
- Martinez L. Basilar Skull FracturesDecember 2013. Grand Rounds presentation presented at the: 2013.
- Jimenez DF, Sundrani S, Barone CM. Posttraumatic anosmia in craniofacial trauma. J Cranio-Maxillofac Trauma. 1997;3(1):8-15.
- Adegbite AB, Khan MI, Tan L. Predicting recovery of facial nerve function following injury from a basilar skull fracture. J Neurosurg. 1991;75(5):759-762.
- Management of Skull Base Fractures : Neurosurgery Quarterly. https://journals.lww.com/neurosurgery-quarterly/Abstract/2002/03000/Management_of_Skull_Base_Fractures.3.aspx. Accessed March 25, 2019.
- Ringer AJ, Matern E, Parikh S, Levine NB. Screening for blunt cerebrovascular injury: selection criteria for use of angiography. J Neurosurg. 2010;112(5):1146-1149.
- Miller PR, Fabian TC, Bee TK, et al. Blunt cerebrovascular injuries: diagnosis and treatment. J Trauma. 2001;51(2):279-285; discussion 285-286.
- Traumatic carotid cavernous fistula accompanying basilar skull fracture: a study on the incidence of traumatic carotid cavernous fistula in the pat… – PubMed – NCBI. https://www.ncbi.nlm.nih.gov/pubmed?term=17993945. Accessed March 10, 2019.
- Resnick DK, Subach BR, Marion DW. The significance of carotid canal involvement in basilarcranial fracture. Neurosurgery. 1997;40(6):1177-1181.
- OlabinriEO, Ogbole GI, Adeleye AO, Dairo DM, Malomo AO, Ogunseyinde AO. Comparative analysis of clinical and computed tomography features of basal skull fractures in head injury in southwestern Nigeria. J Neurosci Rural Pract. 2015;6(2):139-144.
- Comparison of the Canadian CT Head Rule and the New Orleans Criteria in patients with minor head injury. – PubMed – NCBI. https://www.ncbi.nlm.nih.gov/pubmed?term=16189364. Accessed March 10, 2019.
- Savastio G, Golfieri R, Pastore Trossello M, Venturoli L. [Cranial trauma: the predictability of the presentationsymptoms as a screening for radiologic study]. Radiol Med (Torino). 1991;82(6):769-775.
- Exadaktylos AK, Sclabas GM, Nuyens M, et al. The clinical correlation of temporal bone fractures and spiral computed tomographic scan: a prospective and consecutive study at a level I trauma center. J Trauma. 2003;55(4):704-706.
- Stein SC, Ross SE. The value of computed tomographic scans in patients with low-risk head injuries. Neurosurgery. 1990;26(4):638-640.
- Connor SEJ, Flis C. The contribution of high-resolution multiplanar reformats of the skull base to the detection of skull-base fractures. Clin Radiol. 2005;60(8):878-885.
- Kadish HA, Schunk JE. Pediatric basilar skull fracture: do children with normal neurologic findings and no intracranial injury require hospitalization? Ann Emerg Med. 1995;26(1):37-41.
- RinglH, Schernthaner R, Philipp MO, et al. Three-dimensional fracture visualisationof multidetector CT of the skull base in trauma patients: comparison of three reconstruction algorithms. Eur Radiol. 2009;19(10):2416-2424.
- Zayas JO, Feliciano YZ, Hadley CR, Gomez AA, Vidal JA. Temporal Bone Trauma and the Role of Multidetector CT in the Emergency Department. RadioGraphics. 2011;31(6):1741-1755.
- Tseng W-C, Shih H-M, Su Y-C, Chen H-W, Hsiao K-Y, Chen I-C. The association between skull bone fractures and outcomes in patients with severe traumatic brain injury. J Trauma. 2011;71(6):1611-1614; discussion 1614.
- Basilar Skull Fracture : BC Emergency Medicine Network. https://www.bcemergencynetwork.ca/clinical_resource/basilar-skull-fracture/. Accessed March 18, 2019.
- Morani AC, Ramani NS, Wesolowski JR. Skull base, orbits, temporal bone, and cranial nerves: anatomy on MR imaging. Magn Reson Imaging Clin N Am. 2011;19(3):439-456.
- Tuntiyatorn L, Laothammatas J. Evaluation of MR cisternography in diagnosisof cerebrospinal fluid fistula. J Med Assoc Thail Chotmaihet Thangphaet. 2004;87(12):1471-1476.
- La Fata V, McLean N, Wise SK, DelGaudio JM, Hudgins PA. CSF leaks: correlation of high-resolution CT and multiplanar reformations with intraoperative endoscopic findings. AJNR Am J Neuroradiol. 2008;29(3):536-541.
- The “ring sign”: is it a reliable indicator for cerebral spinal fluid? – PubMed – NCBI. https://www.ncbi.nlm.nih.gov/pubmed/8457102. Accessed March 10, 2019.
- Communications E. Head and Neck Trauma. An Interdisciplinary Approach. https://medone-otolaryngology-thieme-com.ezproxy.cul.columbia.edu/ebooks/1527658#/ebook_1527658_SL63411523. Accessed March 8, 2019.
- Reiber H, Walther K, Althaus H. Beta-trace protein as sensitivemarker for CSF rhinorheaand CSF otorhea. Acta Neurol Scand. 2003;108(5):359-362.
- Warnecke A, Averbeck T, Wurster U, Harmening M, Lenarz T, Stöver T. Diagnostic Relevance of β2-Transferrin for the Detection of Cerebrospinal Fluid Fistulas. Arch Otolaryngol Neck Surg. 2004;130(10):1178-1184.
- Veeravagu A, Joseph R, Jiang B, et al. Traumatic epistaxis: Skull base defects, intracranial complications andneurosurgical considerations. Int J Surg Case Rep. 2013;4(8):656-661.
- Spurrier EJ, Johnston AM. Use of nasogastric tubes in trauma patients–a review. J R Army Med Corps. 2008;154(1):10-13.
- Ratilal BO, Costa J, Pappamikail L, Sampaio C. Antibiotic prophylaxis for preventing meningitis in patients with basilar skull fractures. Cochrane Database Syst Rev. 2015;(4).
- Tunkel AR, Hasbun R, Bhimraj A, et al. 2017 Infectious Diseases Society of America’s Clinical Practice Guidelines for Healthcare-Associated Ventriculitis and Meningitis. Clin Infect Dis Off Publ Infect Dis Soc Am. 14 2017.
- Kim DK. Advisory Committee on Immunization Practices Recommended Immunization Schedule for Adults Aged 19 Years or Older — UnitedStates, 2018. MMWR Morb Mortal Wkly Rep. 2018;67.
- Oh J-W, Kim S-H, Whang K. Traumatic Cerebrospinal Fluid Leak: Diagnosis and Management.Korean J Neurotrauma. 2017;13(2):63-67.
- Nash JJ, Friedland DR, Boorsma KJ, Rhee JS. Management and outcomes of facial paralysis from intratemporalblunt trauma: a systematic review. The Laryngoscope. 2010;120(7):1397-1404.
- Dalgic A, Okay HO, Gezici AR, Daglioglu E, Akdag R, Ergungor MF. An effectiveand less invasive treatment of post-traumatic cerebrospinal fluid fistula: closed lumbar drainage system. Minim Invasive Neurosurg MIN. 2008;51(3):154-157.
- Leibu S, Rosenthal G, Shoshan Y, Benifla M. Clinical Significance of Long-Term Follow-Up of Children with Posttraumatic Skull Base Fracture. World Neurosurg. 2017;103:315-321.