Unstable Sepsis: Airway First? Not Always
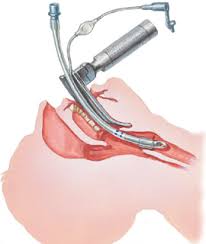
Intubation, especially in the septic and critically ill patient, can, by itself, cause hemodynamic abnormalities and/or hypoxemia and hypercapnea. In some situations, it may be important to make sure that the patient is adequately prepared for intubation, both from hemodynamic and pre-oxygenation standpoints. This is a brief review of some suggestions when intubating the very ill patient in the emergency department.
Unstable Sepsis: Airway First? Not Always Read More »