Authors: Michael J. Yoo, MD (EM Resident, San Antonio, TX), Rachel E. Bridwell, MD (@rebridwell, EM Resident, San Antonio, TX), and Zachary J. Sletten, MD (EM Attending, San Antonio, TX) // Reviewed by Alex Koyfman, MD (@EMHighAK) and Brit Long, MD (@long_brit)
Case
A 33-year-old woman with a history of kidney stones presents to the emergency department (ED) with presyncope gross hematuria from her percutaneous nephrostomy tube. She had a right-sided nephrostomy tube placed 6 days ago by an interventional radiologist for obstruction from a 12 mm proximal ureter stone. The patient states that 36 hours following her procedure, her urine started clearing up but suddenly became cherry-red in color for the past several days. She also notes that during that same time period, her nephrostomy tube has had decreasing output.
Her vital signs are BP 98/65, HR 110, RR 19, 37°C, SpO2 100% RA. The patient looks pale, and you note conjunctival pallor. You inspect her nephrostomy tube site, which is clean and dry, but notice that her nephrostomy collection bag has about 150 mL of gross hematuria with small clots. She endorses mild right-sided costovertebral angle tenderness. What are the next steps in your evaluation and treatment?
Background
The insertion of a percutaneous nephrostomy tube is a minimally invasive and generally well-tolerated procedure in which a small catheter is used to connect the upper urinary tract, typically from the renal pelvis or calyx, to the skin.1 This procedure is performed by interventional radiology or urology, with several indications that can be summarized into 4 broad categories: urinary obstruction, urinary diversion, access for another endourologic procedure, and diagnostic testing.1 However, the majority of nephrostomy tubes are placed for relief of urinary obstruction secondary to a stone, cancer, or stricture, representing up to 90% of total nephrostomy cases.1 Although the technical success of nephrostomy tube placement is reported up to 99%, complications occur in up to 6% of patients.2 The most commonly described complications consist of infection, hemorrhage, and catheter related structural problems—to include misplacement, kinking, and dislodgement.3,4 Other typical post-operative complications such as atelectasis, thrombosis, and pneumonia must also be considered.
General Care, Initial Evaluation, and Minor Complications
Patients with nephrostomy tubes are typically given the following guidelines after their procedure:
- The site should remain completely dry for the first two days.5
- Showering is permitted afterwards, though any submersion such as bathing, hot tubs, and swimming should be avoided.5
- Hydration is essential—patients should drink approximately 2 liters of water per day to maintain tube patency and prevent infection.5
- Patients should inspect the nephrostomy site daily for soiling, external kinking, and leakage.5
- Patients should replace dressings at least twice a week, with soiled dressings replaced immediately.5
- Patients should record the total output into the nephrostomy bag.5
- Patient should replace the drainage bags when it is half to two-thirds full, and the collection bags should be exchanged at least 3 times a week.5

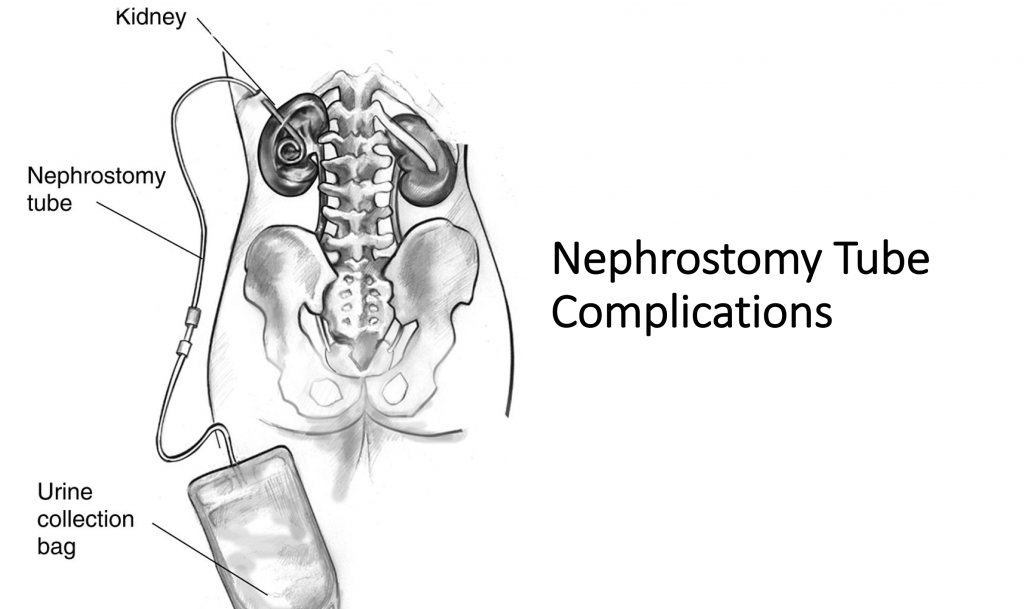
From https://commons.wikimedia.org/wiki/File:N01224_H_nephrostomy.jpg
Any patient with a nephrostomy tube should be assessed for adherence to these recommendations which helps providers evaluate for risk factors for infection or catheter failure. Some common, but minor complaints associated with nephrostomy tubes, their etiologies, and troubleshooting steps that correct the majority of the issues are listed in the table below.

With the exception of concerns for infection, internal catheter failure, or bleeding (all discussed below), patients who present to the emergency department with the chief complaints outlined in the table above can typically be discharged with continued outpatient follow-up with urology, with re-education of nephrostomy care recommendations.
Catheter Blockage Troubleshooting
Data are limited regarding the total incidence of catheter obstructions following nephrostomy tube placement. However, small studies in pregnant women have published post-operative obstructions requiring flushing as high as 45%.6 We extrapolate that any process that can incite hypercalciuria and hyperuricosuria, which are physiologic in pregnancy, may lead to an increased risk of catheter obstruction.6 In the majority of cases, gentle irrigation should relieve the obstruction. The technical aspects of troubleshooting catheter obstructions are listed here:5
- Using sterile technique, disconnect the nephrostomy tube from its collection bag.
- Clean the tip of the tube with alcohol or chlorhexidine.
- Draw up approximately 10 mL of either normal saline or sterile water into a syringe.
- With gentle pressure, flush the nephrostomy tube.
- If resistance is met while flushing, gently pull back on the syringe to dislodge the source of obstruction.
- Re-attempt gentle flushing of the nephrostomy tube.
- Avoid aggressive drawing and flushing to prevent trauma.
If these conservative bedside measures fail, early urology consultation is recommended, especially if the patient is anuric. Simultaneously, workup should be initiated to evaluate for infection (such as abscess), hematoma, and dislodgement causing catheter obstruction or failure. While the specifics of these more serious causes of blockage are discussed below, obtaining labs to include a complete blood cell count, renal function test, and a renal ultrasound (noninvasive, quick, can detect large hematomas and abscesses)is a reasonable approach for a patient with an obstruction that was not relieved with irrigation. The utility of a computed tomography is discussed later.
Infection and Sepsis
The reported rates of post-nephrostomy infections vary widely, occurring in up to 14% of cases.3 Although controversial, most practice guidelines dictate that pre-procedural antibiotics should be administered to prevent infective complications, and that antibiotic regimens should reflect the most recent patient culture data.7 In the absence of culture data, these patients typically receive broad spectrum antibiotics including carbapenems and later generation cephalosporins.3,8 It is worth noting that asymptomatic bacteriuria is common with nephrostomy tubes and can be found in up to 7.5% of patients, though the true rates of asymptomatic bacteriuria is minimally reported and likely underestimated.9 Prophylaxis of asymptomatic bacteriuria with antibiotics is not recommended.9
Patients with post-nephrostomy infectious complications present similarly to non-nephrostomy patients with pyelonephritis. These symptoms include fevers, chills, nausea, vomiting, flank pain, and back pain.8 If the patient is not anuric, some studies suggest urinary changes such as foul-smelling urine or worsening hematuria could be clues to a post-operative infection, although these findings are not specific and generally have little to no evidence supporting their routine use.8 Additionally, pre-nephrostomy pyonephrosis has been shown to be predictive of septicemia, with one study showing that 60% of patients with pyonephrosis progressed to septic shock post-procedurally.11 Nephrostomy tube related infections present at a median time of 42 days after the procedure.10 In an Infectious Disease Society of America study, the most commonly isolated organisms were (in descending order): Pseudomonas (36%), Enterococcus (23%), and E. coli (18%).10 Other studies have identified E.coli, Klebsiella, and Proteus as the most common isolated organisms.11 Importantly, up to half of infections are polymicrobial.10
Unfortunately, no universal guideline currently exists for the optimal empiric antibiotic regimen or timing of catheter exchange in the setting of nephrostomy related infections.12 Further complicating treatment, IDSA guidelines and categorization of catheter related urinary tract infections do not include nephrostomy tubes due to a lack of studies.13 Additionally, as mentioned earlier, nephrostomy tubes are commonly placed for the relief of obstruction, to include cancers. Subsequently, patients on active chemotherapy further complicate the approach to nephrostomy related infections due to the potential for atypical presentations and immunosuppression.
Workup in the ED should include a complete blood cell count (to rule out neutropenia in cancer patients), chemistry (to trend new or worsening renal function), and urine studies, to include a gram stain, urinalysis, and culture to obtain sensitivities. Obtaining a urine sample from patients with nephrostomy tubes may be technically novel to the ED staff. Rather than taking samples from the collection bag, nursing staff should be instructed to use sterile technique, detach the nephrostomy tube from the collection bag, and allow gravity to provide fresh urine into a sterile specimen cup.8 Upon collecting the urine, the nephrostomy tube should be connected to a new, closed bag and anchored to the patient’s body to prevent dislodgement.8 Additionally, in septic or toxic-appearing patients, blood cultures should be added. Imaging to include abdominal computed tomography is often included, which can demonstrate peri-nephrostomy stranding; however, the utility of imaging is greater in the workup of bleeding and catheter misplacement, kinking, and dislodgement (see section on catheter-related complications).14 Furthermore, early engagement of either urology or interventional radiology, depending on which service performed the procedure, is advised.
Despite the limited literature regarding nephrostomy tube infections, we believe that approaching suspected nephrostomy tube infections similarly to complicated cystitis and complicated pyelonephritis is a reasonable strategy (see http://www.emdocs.net/must-know-antimicrobial-regimens-adults/). If the patient presents with sepsis, clinicians should aggressively support blood pressure, oxygenation, and administer broad-spectrum antibiotic therapy, to include antipseudomonal agents.1
Bleeding and Hematuria
Blood tinged urine following nephrostomy tube placement is most common in the hours immediately following the procedure and typically self-resolves within 48 hours.2,15 This is considered a normal clinical course and not a complication of the procedure.2,15 Significant bleeding is a less common but non-negligible complication, occurring between 1% to 4.3% of patients.4 Although this estimate includes intra-operative bleeding complications, other studies document that post-operative hematuria requiring transfusions occurs in up to 2.4% of patients.11 Pre-operative renal failure was found to be the only statistically significant risk factor for post-operative bleeding.16 Cases of significant bleeding present with either continued hematuria beyond 2-3 days postoperatively, or the reappearance of hematuria and clots after a period of clear urine.17 However, delayed presentations up to weeks or months have been reported.17 The etiology of continued hematuria is often a missed, intraoperative vascular injury leading to pseudoaneurysm, arteriovenous fistula, or hematoma formation.17
Clinicians should focus on typical signs and symptoms of clinical anemia—shortness of breath, tachycardia, decreased exercise tolerance, pallor, pre-syncope, and syncope (see http://www.emdocs.net/em3am-anemia/). The initial evaluation for post-operative bleeding includes a complete blood cell count, renal function testing, and a low threshold to obtain coagulation studies and a type and screen. In post-nephrostomy patients, a significant hemoglobin and hematocrit drop out of proportion to the duration and quantity of hematuria should raise suspicion for an intraoperative vascular injury.17 Additional case reports have published that acute renal failure and low nephrostomy tube output were seen in patients who developed post-operative hematomas, likely secondary to the hematoma causing obstructive uropathy.18 Imaging modalities from the ED include renal ultrasound which may diagnose hematoma, though limited by the operator and low sensitivity; in the absence of a clear hematoma on ultrasound, computed tomography with angiography is the recommended imaging modality to identify and characterize hematomas.18,19 If possible, CTA with availability of embolization if needed is recommended.
Management of significant post-operative bleeding includes correction of coagulopathy, if present, and blood transfusions, though a universal transfusion levels remains controversial and may vary based on the patient’s comorbidities. Although there are case reports that non-operative management with transfusions alone is successful in select patients, all patients who present to the ED with significant post-nephrostomy tube hematuria, anemia, or evidence of hematoma requires emergent consultation with either urology or interventional radiology. Ultimately, these patients may require angiography and evaluation for embolization.
Catheter Dislodgment and Kinking
Nephrostomy tube dislodgement is an uncommon but serious post-operative complication, with the largest study published to date reporting rates in up to 5% of patients.20 In this study, the authors found that body mass index was a significant risk factor for dislodgement and theorize that increased skin laxity and subcutaneous tissue allow for movement of the nephrostomy tube anchor point.20 Depending on the initial indication for the procedure, patients with dislodgment (and similarly kinking and catheter failure) can present with a variety of pre-operative symptoms, ranging from flank pain, decreased nephrostomy tube output, urine leak, fever, and bleeding.20 A CT of the abdomen is the imaging modality of choice to confirm placement or dislodgement.21 Ultimately, if dislodgement or kinking is confirmed, emergency physicians should consult urology or interventional urology to coordinate catheter exchange.
Pleural Injury
Pleural injury is possible during nephrostomy tube placement. Complications include pneumothorax, hydrothorax, and pleural effusions. The incidence of these complications increases when the approach for renal access is intercostal (i.e. between the 11th and 12th ribs) versus subcostal, though overall, remains exceedingly rare.3 In fact, the majority of large studies document pleural injury complication in less than 0.3% of cases.8 Although pain from the nephrostomy tube may limit a patient’s inspiration, typical signs and symptoms to include decreased breath sounds, pleuritic chest pain, and hypoxia suggest pleural injury, especially in the days immediately following the procedure. Management of a pneumothorax, hydrothorax, or pleural effusion does not change in the setting of a nephrostomy tube. While some case reports report spontaneous resolution with conservative measures (oxygen supplementation, pulmonary hygiene), ultimately patients may need a chest tube or thoracostomy.3
Key Points
- The majority of nephrostomy tubes are placed for relief of urinary obstruction, and failure of catheters manifest with symptoms similar to what led to nephrostomy tube placement.
- Treat nephrostomy tube infections as complicated cystitis or complicated pyelonephritis, but avoid treating asymptomatic bacteriuria, which is common.
- Be mindful that nephrostomy tubes are often placed for obstructions caused by cancers—make sure the patient is not neutropenic if on chemotherapy.
- Obtain fresh urine from the nephrostomy tube to send off for studies, rather than obtaining urine from the collection bag.
- If an obstruction is suspected, try bedside troubleshooting with gentle irrigation of the catheter.
- Hematuria is common in the first 2 days, but always consider a vascular injury or hematoma formation if hematuria persists or re-occurs after the urine initially clear.
- In patients with decreased breath sounds or pleuritic chest pain ipsilateral to a recently placed nephrostomy tube, always consider pleural injury in your differential diagnosis.
Case Resolution
A CBC reveals a hemoglobin of 6.5 g/dL, which is a 4 point drop from her pre-operative baseline. You transfuse her 2U of pRBC with hemodynamic improvement. CTA reveals a large right-sided hematoma at the renal pelvis, for which she undergoes embolization by interventional radiology. She is admitted for monitoring.
References/Further Reading:
1 Dagli M, Ramchandani P. Percutaneous nephrostomy: technical aspects and indications. Seminars Interventional Radiology. 2011;28(4):424–437.
2 Farrell TA, Hicks ME. A Review of Radiologically Guided Percutaneous Nephrostomies in 303 Patients. Journal of Vascular and Interventional Radiology. 1997;8(5):769–774.
3 Radecka E, Magnusson A. Complications associated with percutaneous nephrostomies. a retrospective study. Acta radiologica. 2004;45(2):184–188.
4 Skolarikos A, Alivizatos G, Papatsoris A, Constantinides K, Zerbas A, Deliveliotis C. Ultrasound-guided percutaneous nephrostomy performed by urologists: 10-year experience. Urology. 2006;68(3):495–499.
5 Nephrostomy and Biliary Tube Management: A Review of the Clinical Evidence and Guidelines. Ottawa (ON): Canadian Agency for Drugs and Technologies in Health; 2014 Sep 4. APPENDIX 2, Summary of Clinical Care Pathways & Patient Information Sheets. Available from: https://www.ncbi.nlm.nih.gov/books/NBK242385/
6 Khoo L, Anson K, Patel U. Success and short-term complication rates of percutaneous nephrostomy during pregnancy. Journal of vascular and interventional radiology. 2004;15(12):1469–73.
7 Nicolle LE, Bradley S, Colgan R, Rice JC, Schaeffer A, Hooton TM. Infectious Diseases Society of America guidelines for the diagnosis and treatment of asymptomatic bacteriuria in adults. Clinical Infectious Diseases. 2005;40(5):643–654.
8 Zagoria RJ, Dyer RB. Do’s and don’t’s of percutaneous nephrostomy. Academic radiology. 1999;6(6):370–377.
9 Bahu R, Chaftari AM, Hachem RY, Ahrar K, Shomali W, El Zakhem A, Jiang Y, AlShuaibi M, Raad II.Nephrostomy tube related pyelonephritis in patients with cancer: epidemiology, infection rate and risk factors. The Journal of urology. 2013;189(1):130–135.
10 El Haddad H, Viola G, Jiang Y, Raad I, Rolston K, Szvalb A. Percutaneous Nephrostomy Tube-related Infections. Open Forum Infectious Diseases. 2017;4(1):S349-S349.
11 Turo R, Horsu S, Broome J, Das S, Gulur DM, Pettersson B, Doyle G, Awsare N. Complications of percutaneous nephrostomy in a district general hospital. Turkish Journal of Urology. 2018;44(6):478–483.
12 McDevitt JL, Acosta-Torres S, Zhang N, Hu T, Odu A, Wang J, Xi Y, Lamus D, Miller DS, Pillai AK. Long-Term Percutaneous Nephrostomy Management of Malignant Urinary Obstruction: Estimation of Optimal Exchange Frequency and Estimation of the Financial Impact of Patient Compliance. Journal of Vascular and Interventional Radiology. 2017;28(7):1036–1042.
13 Hooton TM, Bradley SF, Cardenas DD, Colgan R, Geerlings SE, Rice JC, Saint S, Schaeffer AJ, Tambayh PA, Tenke P, Nicolle LE. Diagnosis, Prevention, and Treatment of Catheter-Associated Urinary Tract Infection in Adults: 2009 International Clinical Practice Guidelines from the Infectious Diseases Society of America. Clinical Infectious Diseases. 2010;50(5):625–663.
14 Lewis S, Patel U. Major complications after percutaneous nephrostomy-lessons from a department audit. Clinical Radiology. 2004;59(2):171–179.
15 Von der Recke P, Nielsen MB, Pedersen JF. Complications of Ultrasound-Guided Nephrostomy: a 5-year Experience. Acta Radiologica. 1994;35(5):452–454.
16 Lee WJ, Patel U, Patel S, Pillari GP. Emergency Percutaneous Nephrostomy: Results and Complications. Journal of vascular and interventional radiology. 1994;5(1):135–139.
17 Cope C, Zeit RM. Pseudoaneurysms after nephrostomy. American Journal of Roentgenology. 1982;139:255–261.
18 Stewart JK, Smith TP, Kim CY. Clinical implications of acute pelvicaliceal hematoma formation during percutaneous catheter nephrostomy insertion. Clinical imaging. 2017;43:180–183.
19 Dayal: Dayal M, Gamanagatti S, Kumar A. Imaging in renal trauma. World Journal of Radiology. 2013;5(8):275–284.
20 Bayne D, Taylor ER, Hampson L, Chi T, Stoller ML. Determinants of nephrostomy tube dislodgment after percutaneous nephrolithotomy. Journal of endourology. 2015;29(3):289–292.
21 Jones CD, McGahan JP. Computed tomographic evaluation and guided correction of malpositioned nephrostomy catheters. Abdominal imaging. 1999;24(4):422–425.