Author: David Bussé, MD, MBA (EM Resident Physician, UTSW / Parkland Memorial Hospital) // Edited by: Jamie Santistevan, MD (@jamie_rae_EMdoc – EM Physician, Presbyterian Hospital, Albuquerque, NM); Manpreet Singh, MD (@MPrizzleER – Assistant Professor of Emergency Medicine / Department of Emergency Medicine – Harbor-UCLA Medical Center); and Brit Long, MD (@long_brit – EM Attending Physician, San Antonio, TX)
Welcome to this edition of ECG Pointers, an emDOCs series designed to give you high yield tips about ECGs to keep your interpretation skills sharp. For a deeper dive on ECGs, we will include links to other great ECG FOAMed!
The Case:
A 65-year-old male with a PMH of ICM s/p PCI and ICD placement and presents to your ED stating that his ICD has shocked him multiple times since he attempted to fall asleep earlier yesterday evening. Of note, he returned yesterday morning from a brief cruise line Caribbean vacation with his grandchildren. He states he had been noticing increased leg swelling and exertional shortness of breath over the past 2 days, but figured he could wait to see his PCP at his next scheduled appointment, as this is not uncommon. His triage vitals are T 36.5C, HR 94, BP 187/123, and O2 Sat 91% on room air.

This ECG shows sinus rhythm with a left bundle branch block.
Function of Implantable Cardioverter-Defibrillators (ICDs)
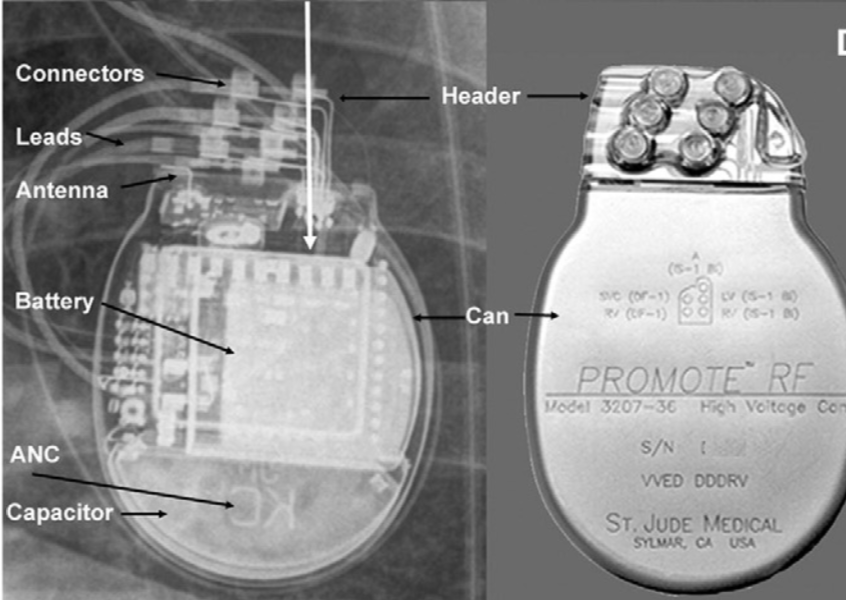
ICDs serve to disrupt cardiac dysrhythmias. In addition to anti-tachycardia pacing and shock delivery, most newly implanted ICDs also have pacing functionality [1]. A CXR will distinguish an ICD from a pacemaker, as the leads of an ICD include the thick coil of the shocking electrode [4, 7]. As with pacemakers, plain radiography also identifies the manufacturer’s logo.
ED Approach to ICD Malfunction
Single Shock
- Patients who receive a single shock of their ICD should be seen by their cardiologist for urgent interrogation [1, 7] . They are actually instructed not to visit the ED.
- Should they come to the ED, a medically appropriate work-up may be limited to a focused H&P [1, 7]. The provider should identify symptoms that preceded the shock/lasted after the shock.
- An ECG, electrolyte studies, and a CXR are appropriate tests [1]. Interrogation with the patient’s cardiologist should be arranged.
Multiple Shocks

- A patient presenting with multiple shocks, however, is a different story.
- If a patient with an ICD experiences cardiac arrest, do not deviate from standard ACLS therapies [7].
- External defibrillator pads should be placed in the anterior-posterior configuration.
- ICD shocks do not pose a danger to others, but to avoid an unpleasant tingle, wear gloves [7].
- When the patient is hemodynamically stable, differentiate between appropriate and inappropriate shocks by interrogating the device. Interrogation can confirm true shocks vs. phantom shocks by accessing the device’s stored ECGs [7].
- If shocks are deemed appropriate in the stable patient, external defibrillation pads should be placed on the patient. Do NOT place a magnet in this circumstance [7].
- Occasionally, ICD shocks are delivered for tachydysrhythmias that are not hemodynamically significant (Afib, Aflutter) [7]. If the shocks are distressing to the patient, place a magnet over the ICD.
- An ECG and a continuous rhythm strip should be obtained on all symptomatic patients in order to identify the underlying dysrhythmia. Electrolytes, cardiac biomarkers (in certain circumstances), and a CXR are also warranted [1].
- Transient ST-segment changes following defibrillation are common but should normalize within 5-15 minutes [3, 7].
- Defibrillation alone can also cause an increase in troponin levels [1, 3, 7]. Therefore, only those with symptoms consistent with ACS should undergo such evaluation.
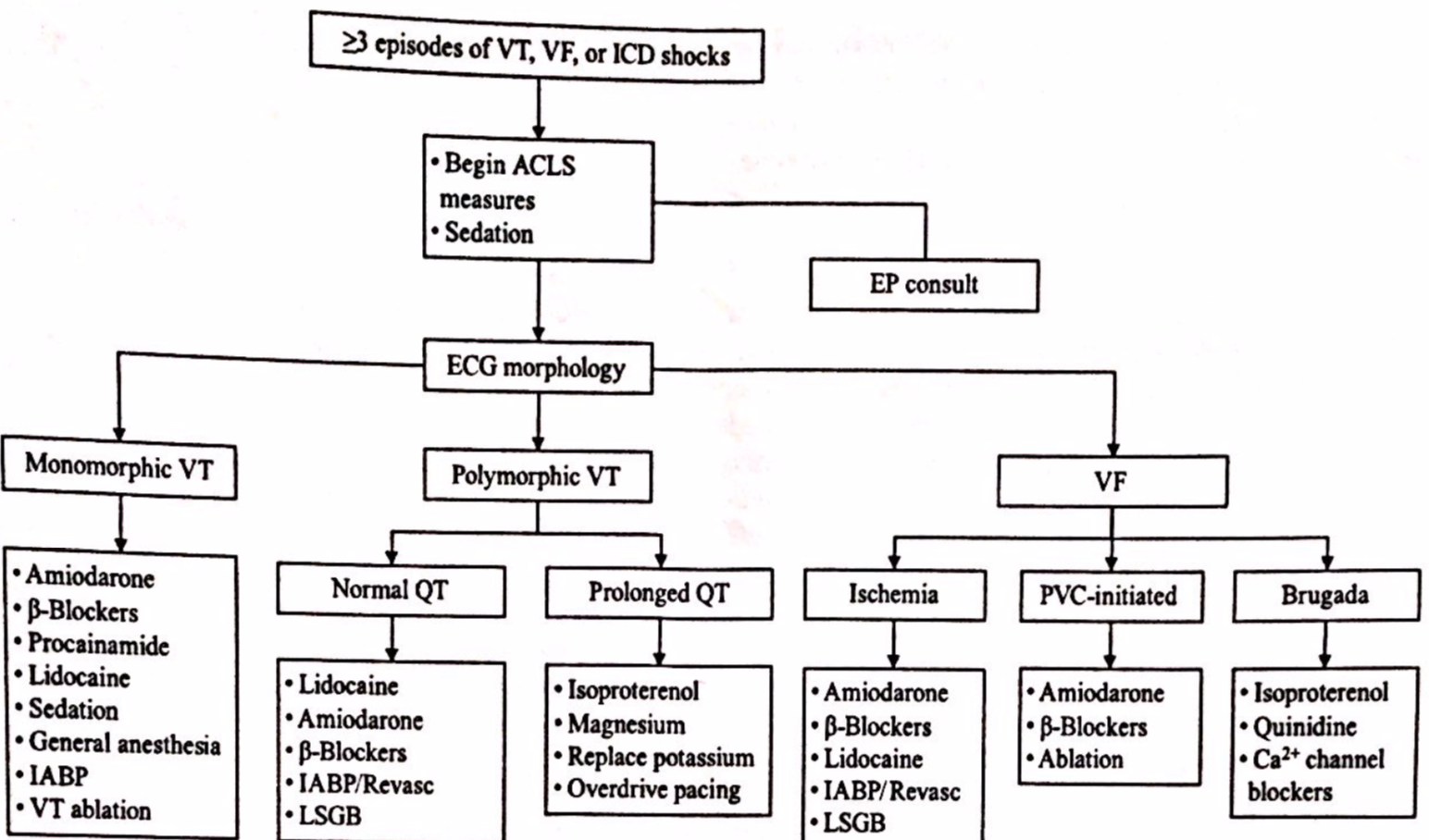
- Three distinct episodes of ventricular tachycardia, ventricular fibrillation, or appropriate shocks from an ICD in 24 hours defines electrical storm [1, 3, 7]. Specific precipitants include acute ischemia, worsening heart failure, hypokalemia, hypomagnesemia, arrhythmogenic drug therapy, hyperthyroidism, and infection/fever [3, 7].
- Monomorphic VT tends to be associated with worsening structural heart disease, most commonly scar tissue following MI [3]. Acute myocardial ischemia almost always presents with polymorphic VT [3].
- Amiodarone is the anti-arrhythmic drug of choice for appropriate shocks [1, 3].
- Consider adding IV metoprolol, propranolol, or esmolol [1, 3].
- Propranolol consistently decreases the incidence of fatal VF during acute MI and sudden cardiac death after MI [3].
- Propranolol blunts the pro-dysrhythmic effect of catecholamines (epinephrine, vasopressin) and is advocated under current ACLS guidelines in cases of pulseless VT or VF [3].
- Magnesium is unlikely to be effective in polymorphic VT associated with a normal QT interval, but it should be given for those with long QT interval [3].
- If other measures fail, general anesthesia is warranted [1]. IV analgesics and sedatives should be given early and aggressively to patients who sustain multiple ICD shocks [3].
- Patients experiencing electrical storm should be admitted to an ICU for aggressive monitoring with electrophysiology consult [7].
Additional Considerations
- Valid DNR orders do not preclude ICD therapy [7]. ICDs should not be deactivated by the emergency practitioner based on this document.
- The femoral vein is the safest access site in an emergent situation for placement of a central venous catheter. The subclavian or internal jugular veins contralateral to the ICD can be accessed with care [7].
- ICDs are susceptible to infections in the same manner as pacemakers. Vancomycin is the antibiotic of choice, but if the patient is septic/ill appearing, broad-spectrum coverage is needed [7].
- Non-depolarizing neuromuscular blockade agents are preferred for RSI. Inappropriate therapy has been attributed to oversensing of muscle fasciculations following succinylcholine administration [7].
- Contact the device manufacturer prior to obtaining an MRI. Magnetic fields can disable or reprogram devices, cause spurious therapies, or cause burns and other injuries [7].
Application of a clinical magnet to an ICD
Placement of a clinical magnet over a defibrillator causes the device to temporarily stop delivering shocks without affecting its pacing functionality [1, 3, 5, 7]. This measure is confirmed by an auditory/vibratory alert. Except when dealing with St. Jude and Sorin ICDs, place the magnet directly over the device. With these exceptions, it is best to place the magnet just proximal to the device [5].
This feature is useful in the setting of recurrent, distressing, inappropriate shocks. Place external defibrillation pads on a patient’s chest and back prior to applying a magnet. Keep in mind that not all ICDs will resume their actions once the magnet is removed [5, 7]. Lastly, interrogate all ICDs before external monitoring and therapies are discontinued.
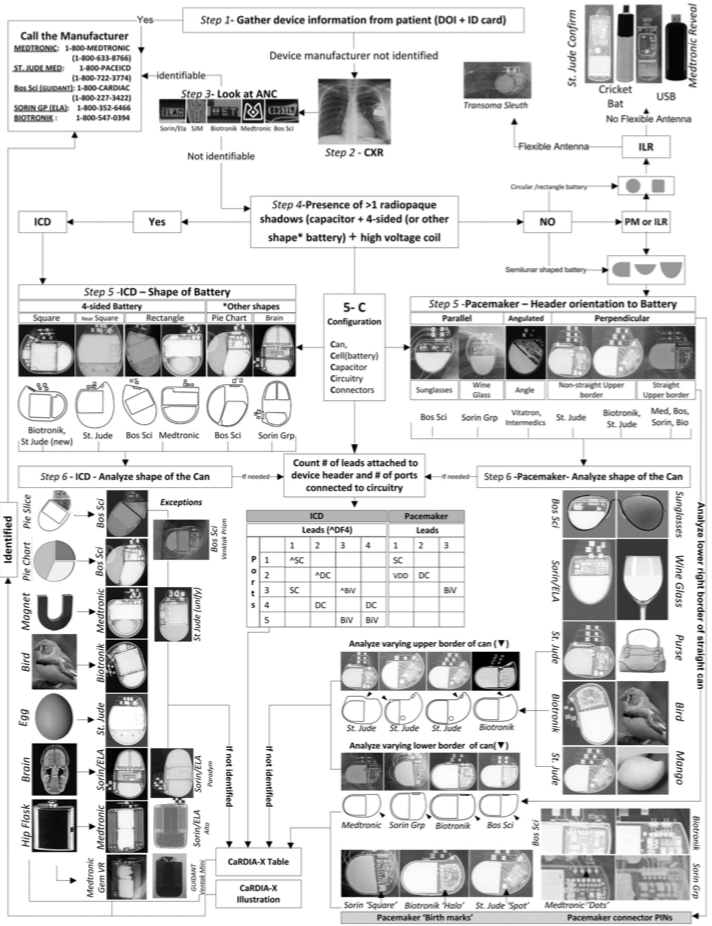
Cardiac Rhythm Device Identification Algorithm Using X-Rays [4]
References/Further Reading:
- Allison, Michael G., and H. A. Mallemat. Emergency Care of Patients with Pacemakers and Defibrillators. Emergency Medicine Clinics of North America. 2015. 33(3). 653-667.
- Cardall, Taylor Y., et al. Permanent Cardiac Pacemakers: Issues Relevant to the Emergency Physician, Part I. The Journal of Emergency Medicine. 1999. 17(3). 479-489.
- Eifling, Michael, M. Razavi, and A. Massumi. The Evaluation and Management of Electrical Storm. Texas Heart Institute Journal. 2011. 38(2). 111-121.
- Jacob, Sony, et al. Cardiac Rhythm Device Identification Algorithm Using X-rays: CaRDIA-X. Heart Rhythm Society. 2011. 8(6). 915-922.
- Jacob, Sony, et al. Clinical Applications of Magnets on Cardiac Rhythm Management Devices. Europace. 2011. 13. 1222-1230.
- Madhavan, Malini, et al. Advances and Future Directions in Cardiac Pacemakers. Journal of the American College of Cardiology. 2017. 69(2). 211-235.
- McMullan, Jason, et al. Care of the Pacemaker/Implantable Cardioverter Defibrillator in the ED. American Journal of Emergency Medicine. 2007. 25. 812-822.
- Mulpuru, Siva, et al. Cardiac Pacemakers: Function, Troubleshooting, and Management. Journal of the American College of Cardiology. 2017. 69(2). 189-210.







4 thoughts on “ECG Pointers: ICDs and when they malfunction”
Pingback: Nursing FOAMed Review #11 (May 3rd - May 25th) - Code Blue LLC
Great review ! Only after reading did I realize it was written by an excellent resident from my home institution. Great job!
Pingback: Akut kardiologi – Kurs Lund 2019 – Mind palace of an ER doc
Pingback: Pacemaker – Översikt – Mind palace of an ER doc