Author: Manpreet Singh, MD (@MPrizzleER – Assistant Professor of Emergency Medicine / Department of Emergency Medicine – Harbor-UCLA Medical Center) // Edited by: Jamie Santistevan, MD (@jamie_rae_EMdoc – EM Physician, Presbyterian Hospital, Albuquerque, NM) and Brit Long (@long_brit – EM Attending Physician, San Antonio, TX)
Welcome to this edition of ECG Pointers, an EMDocs series designed to give you high yield tips about ECGs to keep your interpretation skills sharp. For a deeper dive on ECGs, we will include links to other great ECG FOAMed!
The Case:
While working during your busy overnight shift, an EKG tech hands you the following patient’s screening EKG that is being triaged for chest pain. They ask for your quick signature so they can get back to the front.
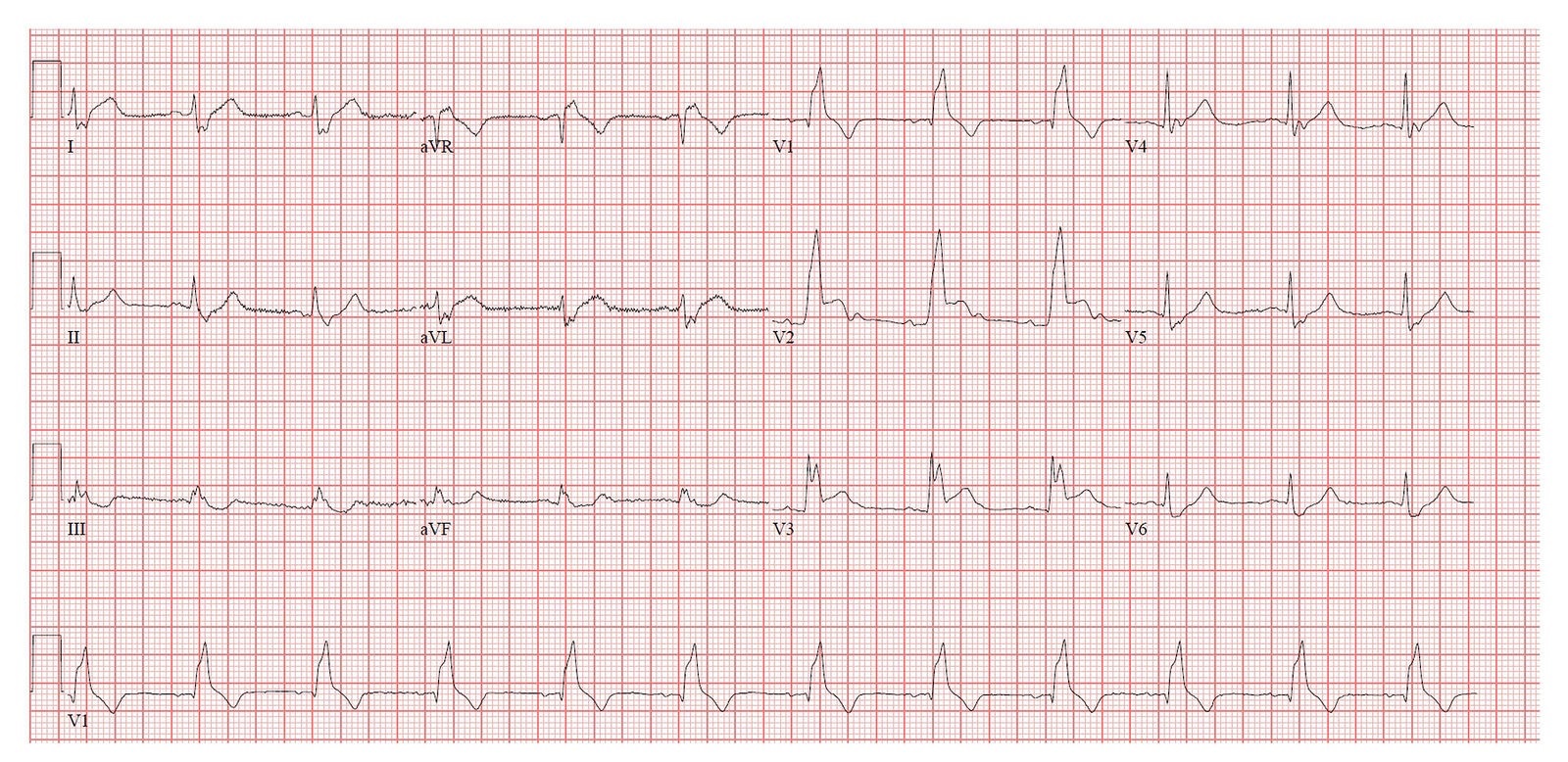
You are tempted to put your initials down and continue with your work, but you pause and notice something is off.
Often, when we see a RBBB in a chest pain patient, looking for ischemic changes may sound difficult as secondary repolarization abnormalities may be normal findings in V1-V3. So what can we do to help us in picking up ACS changes on the EKG in the setting of a RBBB?
What is a right bundle branch block (RBBB)?
A RBBB is a block at the right bundle branch leading to delayed right ventricle depolarization. It can develop from various reasons (structural, function, iatrogenic), most commonly due to age, DM, and anterior wall infarctions (note – more perfusion from LAD though dual blood supply).
The RBBB ECG Diagnostic Criteria includes the following:
- QRS complex > 0.12 seconds
- rSR’ QRS complex in anterior pre-cordial leads (V1-V3) – The classic ‘M-shaped QRS complex’
- Widened or “slurred” S wave in leads I, aVL and V5/V6

Can a RBBB obscure diagnosis of ACS?
Unlike a LBBB, a RBBB should not pose a diagnostic challenge in interpretation of ST-segment elevation. As mentioned earlier, a positive QRS is normally associated with ST depressions and T wave inversions (secondary repolarization abnormalities), which is violated in ACS. In that case, we can potentially note ST-segment elevations. T waves findings in ACS are usually variable, as they may still be inverted or lost / hidden within the ST-segment.
There are also two key points to remember when looking for ischemic changes:
- There is normally an appropriate discordance between the QRS complex and ST-T.
- Find the terminal portion of the QRS located at the J-point (isoelectric baseline) and look for subtle ST-segment elevations.
What does a RBBB in the setting of ACS mean to your patient?
A RBBB in an ACS patient can be a marker of significant potential cardiovascular risk in this sub-group with quite a high short- and long-term risk of morbidity and mortality.1 These patients are more likely to experience acute CHF, hypotension, A-V blocks requiring pacemaker placement, cardiogenic shock, and cardiac arrest.1,2 A RBBB was found to be a more important independent predictor of in-hospital mortality than LBBB.3
What are the main ECG pointers for RBBB in ACS?
- Look for appropriate discordance between the QRS complex and ST-T.
- Look for subtle ST-segment findings after the J-point (isoelectric baseline).
- A RBBB in setting of ACS is an independent predictor of 30-day mortality, so definitely keep an eye on these patients when they are in your ED.
But wait, here’s some more ECG FOAMed:
- http://hqmeded-ecg.blogspot.com/2015/09/pseudostemi-and-true-st-elevation-in.html – Great tip by Dr. Smith. Find the end of the QRS and draw a line at beginning of ST segment (J-point).
- http://www.ems12lead.com/2011/02/09/an-unusual-case-of-right-bundle-branch-block-discussion/ – Tom Bouthillet highlights an unusual case of RBBB.
Special thanks to Dr. James T. Niemann for reviewing this write-up for me!
References
- Horton, Cheryl Lynn, and William J. Brady. “Right bundle-branch block in acute coronary syndrome: diagnostic and therapeutic implications for the emergency physician.” The American journal of emergency medicine9 (2009): 1130-1141.
- Hazem, A., Sharma, S., Sharma, A., Leitch, C., Sharadanant, R., Uriell, M., … & Sorita, A. (2014). Is right bundle branch block associated with poor outcomes in the setting of an acute coronary syndrome? A systematic review and meta-analysis.
- Chan, William K., et al. “Clinical Characteristics, Management, and Outcomes of Acute Coronary Syndrome in Patients With Right Bundle Branch Block on Presentation.” The American journal of cardiology5 (2016): 754-759.






