Author: Brit Long, MD (@long_brit, EM Attending Physician, San Antonio, TX) // Edited by: Alex Koyfman, MD (@EMHighAK, EM Attending Physician, UTSW / Parkland Memorial Hospital)
Welcome to EM@3AM, an emDocs series designed to foster your working knowledge by providing an expedited review of clinical basics. We’ll keep it short, while you keep that EM brain sharp.
A 52-year-old male with a history of severe liver disease, cirrhosis, and hepatitis C presents with altered mental status. He presents with his wife, and the only major pertinent history is the patient has not had a bowel movement in 5 days. His vital signs are normal, and he displays asterixis on exam. His neurologic exam is otherwise nonfocal. His ECG, head CT, and labs are normal.
What should you consider, and what are your next steps?
Answer: Hepatic encephalopathy
Background: This is primarily a diagnosis of exclusion that occurs in patients with severe liver disease, primarily due to nitrogen waste accumulation and increased metabolism of ammonia to glutamine in the CNS. It occurs with increased nitrogen load, decreased toxin clearance, and alteration in neurotransmitters.
Precipitants include GI bleed, high dietary protein, infection (SBP, UTI), low potassium, alkalosis, constipation, dehydration, vomiting, opioids, benzodiazepines, alcohol, and others.
Hepatic encephopathy is a diagnosis of exclusion. Consider intracerebral hemorrhage/subdural hematoma, hypoglycemia, hyper/hyponatremia, renal failure, sepsis/SBP, intoxication/overdose, Wernicke-Korsakoff syndrome, etc.
The condition is characterized by a progression from AMS to hyperreflexia, spasticity, seizure, and coma. Patients may present with stigmata of hepatic disease including jaundice, pedal edema, ascites, palmar erythema, gynecomastia, spider angiomata, sequelae of portal hypertension (ascites, varices), and asterixis. Asterixis is not specific for hepatic encephalopathy. It results from loss of postural control and is not a true tremor.

Evaluate with CBC, renal function and liver function panels, coagulation panel, urinalysis, ECG, and chest x-ray. Low threshold for Head CT is recommended. Paracentesis should be completed if ascites is present. Ammonia is typically elevated, though this should not be used for definitive diagnosis.
Management: Identify and correct precipitating cause(s) thorough history, exam, labs, and imaging as indicated to evaluate for GI bleed, infection (SBP), hypoglycemia, intravascular hypovolemia, renal failure (hepato-renal syndrome), electrolyte derangement, hepatocellular CA, or hepatic/portal vein thrombosis.
Treat underlying cause and lower serum NH3: Lactulose for acute portal systemic encephalopathy: 20-30g (30-45cc) every hour to bowel movement, reduce to TID/QID, and titrate to 2-3 soft stools QD. Rifaximin for those intolerant of lactulose or failing to improve after 48 hours of therapy (off-label: 400mg q 8hrs for 5-10 days) can be used, as can neomycin (associated with nephrotoxicity and ototoxicity). Treat hypokalemia, which contributes to renal ammonia production.
Other treatments include polyethylene glycol, flumazenil, L-carnitine, acarbose, sodium benzoate, melatonin, serotonin antagonists, and opioid antagonists.
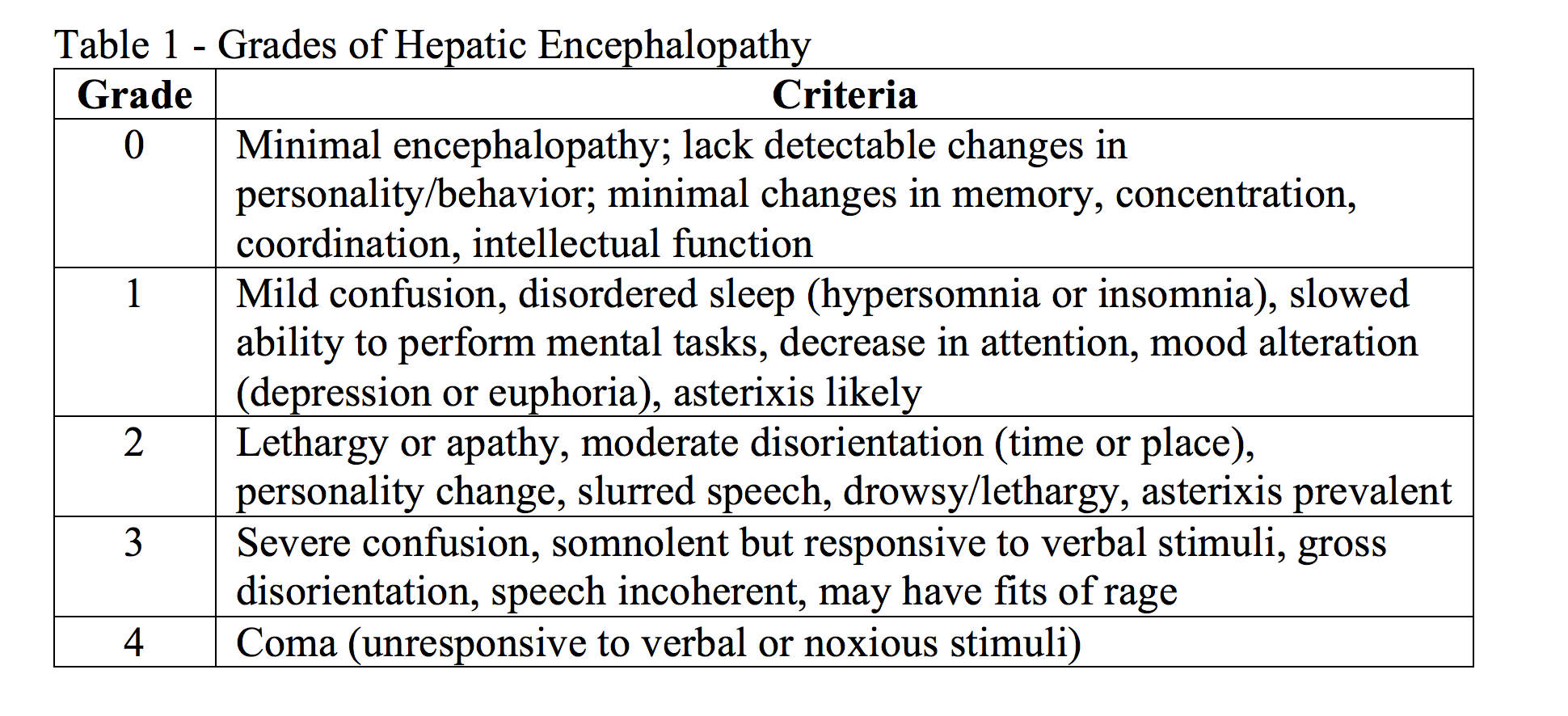
Disposition: Recommendations are based upon grade of overt hepatic encephalopathy and evaluation of underlying causes. Patients with grades 0 and I are usually appropriate for discharge. Patients with grade II may need admission depending on patient status and ability to follow-up. Grades III and IV typically require admission to the ICU.
References:
- Vilstrup H, Amodio P, Bajaj J, et al. Hepatic encephalopathy in chronic liver disease: 2014 Practice Guideline by the American Association for the Study of Liver Diseases and the European Association for the Study of the Liver. Hepatology 2014; 60(2): 715-735.
- Poordad FF. Review article: the burden of hepatic encephalopathy. Aliment Pharmacol Ther 2007; 25 Suppl 1: 3-9.
- Ortiz M, Jacas C, Córdoba J. Minimal hepatic encephalopathy: diagnosis, clinical significance and recommendations. J Hepatol 2005; 42 Suppl: S45-S53.
- Khungar V, Poordad F. Hepatic encephalopathy. Clin Liver Dis 2012; 16(2): 301-320.
- Blei AT, Córdoba J. Hepatic Encephalopathy. Am J Gastroenterol 2001; 96: 1968-1976.
- Bajaj JS, Wade JB, Sanyal AJ. Spectrum of neurocognitive impairment in cirrhosis: Implications for the assessment of hepatic encephalopathy. Hepatology 2009; 50: 2014-2021.
- Bajaj JS. Review article: the modern management of hepatic encephalopathy. Aliment Pharmacol Ther 2010; 31: 537-547.