Authors: Russ Burgin (MS4, Bethesda, MD); Rachel Bridwell, MD (EM Attending Physician, WA) // Reviewed by: Sophia Görgens, MD (EM Physician, Northwell, NY); Cassandra Mackey, MD (Assistant Professor of Emergency Medicine, UMass Chan Medical School); Brit Long, MD (@long_brit)
Welcome to EM@3AM, an emDOCs series designed to foster your working knowledge by providing an expedited review of clinical basics. We’ll keep it short, while you keep that EM brain sharp.
A 68-year-old male with a history of poorly controlled diabetes presents to the ED with increasing right-sided ear and facial pain, swelling, and difficulty hearing for two weeks. He says the pain is worse at night and when he is chewing. Today, he noticed his right face looked swollen and he had an unequal smile.
Triage vital signs include BP 130/75 mm Hg, HR 90 bpm, T 37C, RR 15 breaths per minute, SpO2 98% on room air. A point of care glucose is 148 mg/dL. On exam, the right side of the patient’s face is notably swollen. The right ear is anteriorly displaced by surrounding edema and is erythematous with malodorous discharge. There is facial asymmetry that involves the forehead. Otoscopic exam reveals granulation tissue, as shown below.
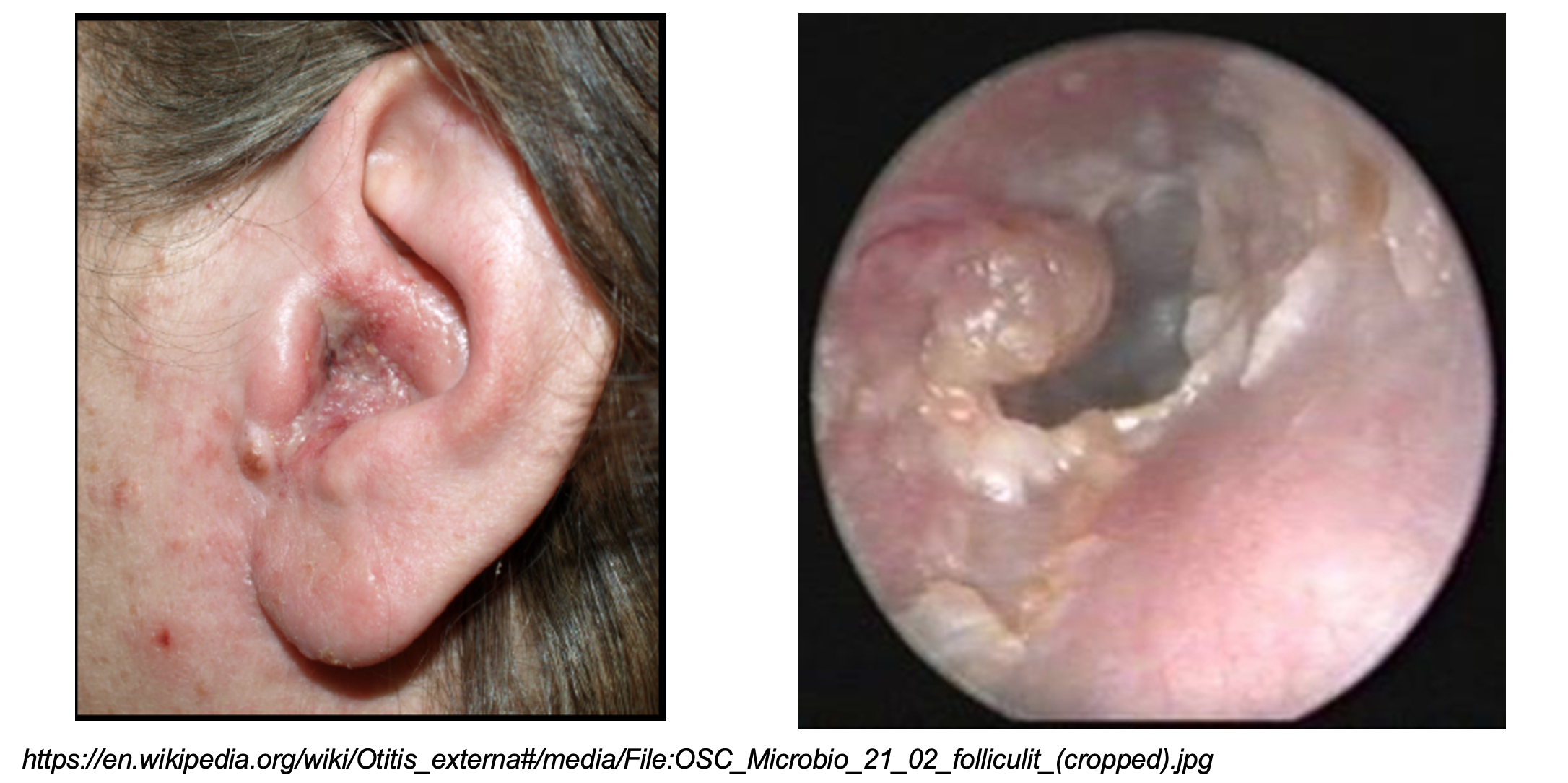
What is the diagnosis?
Answer: Malignant/Necrotizing Otitis Externa (MOE)1-13
Definition:
- Invasive infection of the external ear and surrounding tissue that can spread to the skull base
Pathophysiology: Not fully understood, 90% of cases associated with some form of glucose intolerance in addition to:1
- Microangiopathy of ear canal1
- Elevated pH of cerumen among patients with glucose intolerance which causes impaired immune response2
- Microbiology: 95% of cases caused by Pseudomonas aeruginosa2
- Other organisms more rarely isolated include Proteus mirabilis, Proteus, Klebsiella spp., and Staphylococcus spp.. 2
- Fungal involvement (usually Aspergillus fumigatus), especially in immunocompromised patients.2
Epidemiology/Risk Factors:
- Age > 603
- Rarely occurs in children, although reported in those with diabetes or immunocompromised4
- Diabetes mellitus3
- Immunosuppression3
Evaluation:
- Diagnosis is largely clinical, particularly in the ED, due to non-specific nature of labs and availability of imaging modalities
- Clinical features
- Otalgia (often exquisite, nocturnal, and associated with mastication)4
- Otorrhea non-responsive to typical otitis externa (OE) topicals, e.g. fluroquinolones, corticosteroids5
- Auditory canal edema
- Granulation tissue in floor of ear canal
- CN palsies, most often VII, but can affect IX, X, XI4
- Altered mental status (if intracranial involvement)
- Most lab work will be normal, with the exception of ESR/CRP
- Non-specific, but can be used to monitor progression/response to treatment5
- Negative studies do not rule out MOE4
- May be helpful to distinguish MOE from acute otitis externa6
- Cultures of ear drainage/granulation tissue (bacterial, fungal, mycobacterial)4
- Essential to determine appropriate therapy4
- Antimicrobial sensitivity may change during treatment course8
- Histology of granulation tissue is important to rule out neoplasm (i.e., squamous cell carcinoma)8
- Ideally blood cultures prior to antibiotics, but bacteremia is rare, thus limited yield5
- Check blood glucose level to assess for concomitant diabetic ketoacidosis
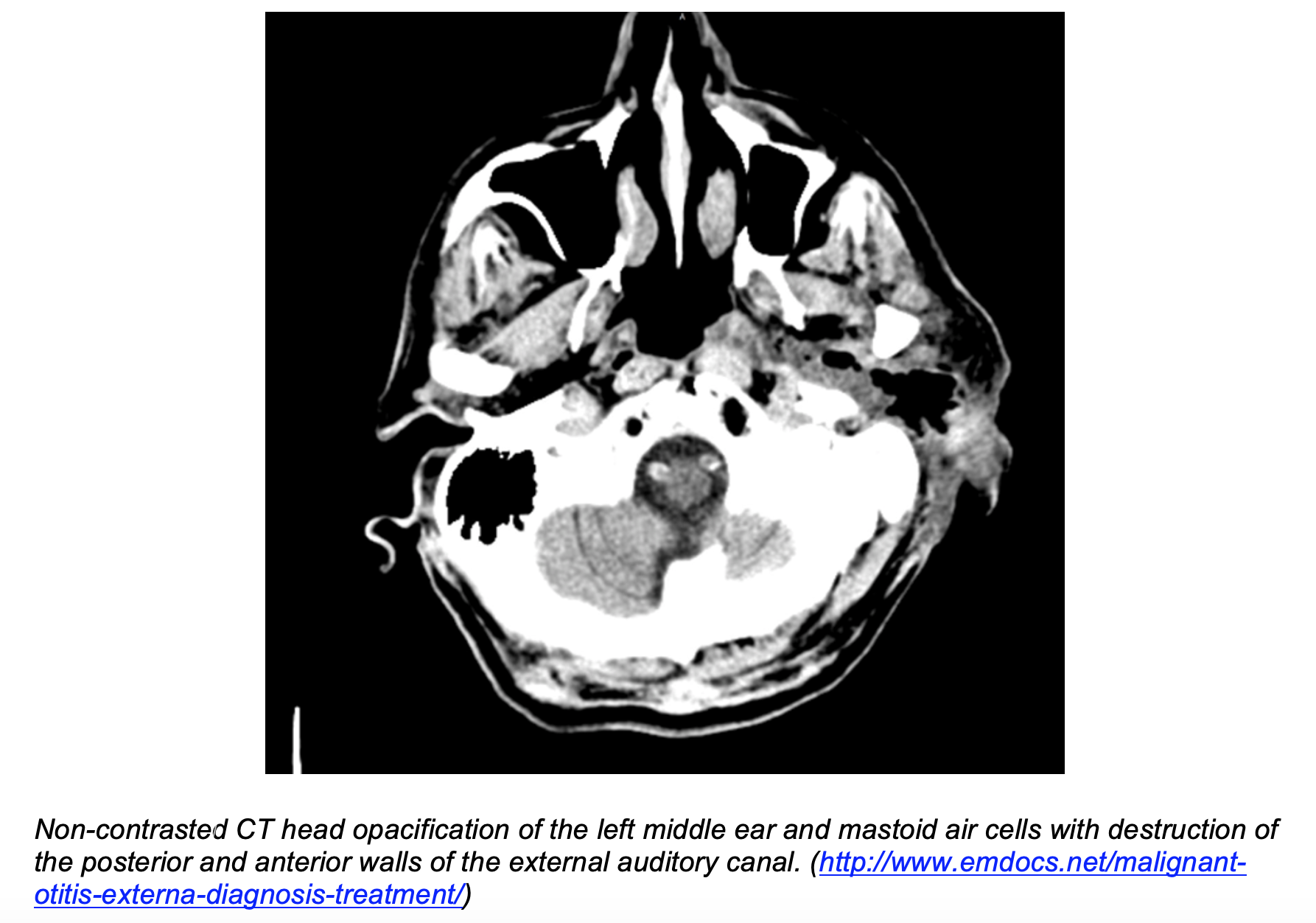
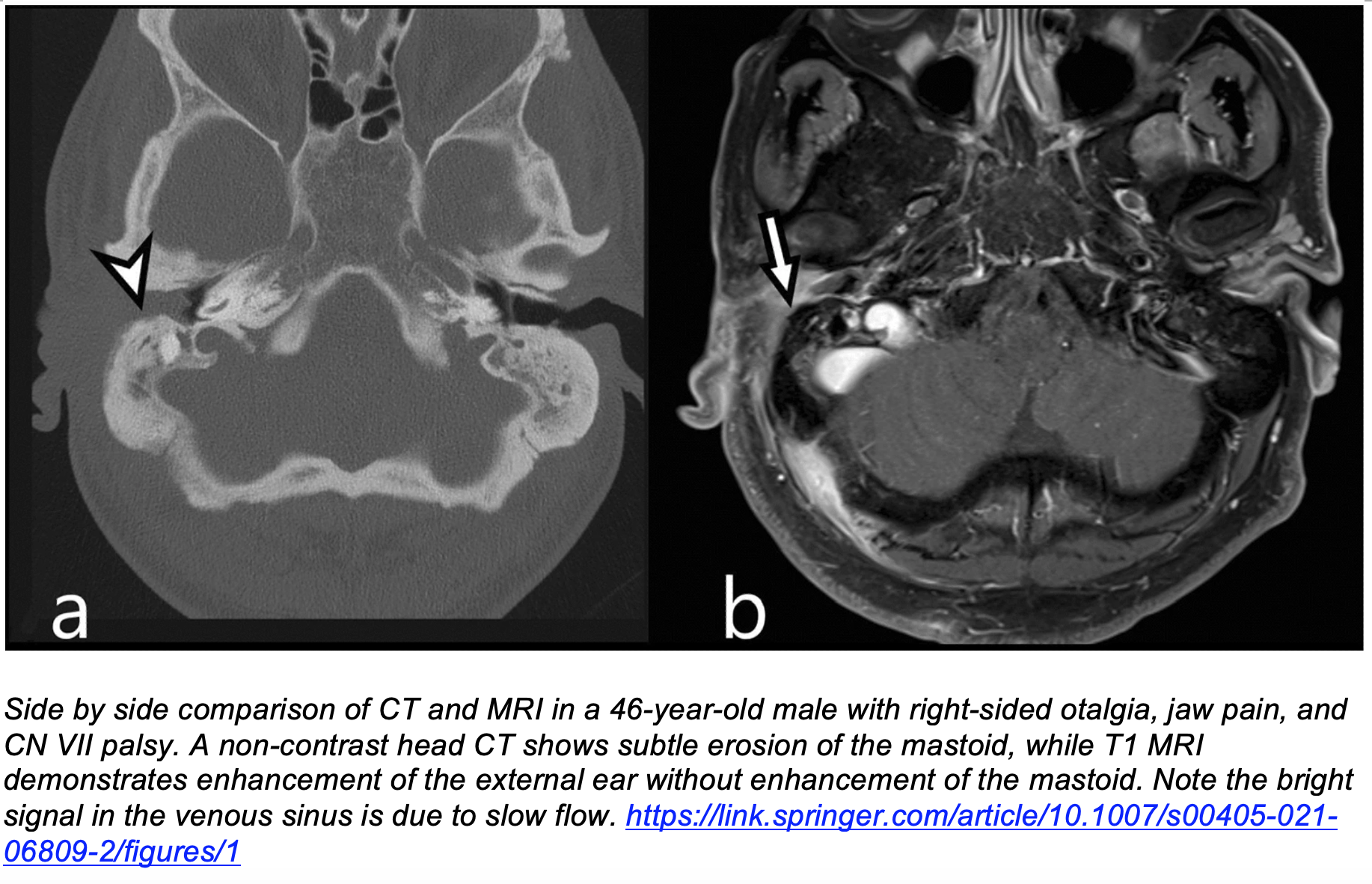
- Imaging: CT vs MRI
- CT is superior for detecting bony erosion (e.g. mastoid), which aids in diagnosis but may not be present in early disease7
- MRI is superior in establishing direction/depth of invasion, disease course, and response to treatment3,7
- Gallium or Technicum-99 may be used once admitted or as test of cure, though this will not occur in the ED9,10
Treatment:
- Consult ENT early for disposition
- Early MOE may be managed in the outpatient setting for a small set of well-appearing patients with close follow-up4
- Consult Infectious Disease for antimicrobial selection4
- Antipseudomonal therapy4,11,12
- Immunocompetent:
- Outpatient: oral ciprofloxacin 750mg BID for 6-8 weeks
- Inpatient: IV ciprofloxacin 400mg q8h until clinical response or decrease in ESR and/or CRP, then transition to oral
- Indications for combination ciprofloxacin and anti-pseudomonal beta-lactam:
- Immunocompromised
- Advanced disease (cranial neuropathies, significant bony erosion)
- High resistance to fluroquinolones in antibiogram
- Choices:
- Piperacillin-tazobactam: IV 4.5g q6h
- Cefepime: IV 2g q12h
- Ceftazidime: IV 2g q8h
- Meropenem: IV 2g q8h
- Pseudomonal resistance to ciprofloxacin is rising
- Immunocompetent:
- Consider muscle relaxants for those with TMJ/mastication symptoms13
Pearls
- MOE is almost always associated with glucose intolerance.
- Pseudomonas aeruginosa is responsible for 95% of cases.
- CT and MRI can be synergistic in diagnosis of management, though CT is the ideal imaging modality in the ED.
- Consult ENT and ID early to determine disposition/appropriate antimicrobial coverage.
- Fluroquinolones +/- anti-pseudomonal beta-lactams are the antimicrobials of choice for initial management.

A 67-year-old man with a history of hypertension and diabetes presents to the emergency department with right ear pain for 2 weeks. His vital signs are normal except for a temperature of 38.2°C and a blood pressure of 158/82 mm Hg. On exam, he has a right-sided facial droop that does not spare his forehead. His right ear is exquisitely painful, even with the slight pulling of his auricle. The ear canal is edematous with granulation tissue across the floor of the canal and pale yellow discharge. He has no pain over his mastoid and his physical exam, including a thorough neurologic exam, is otherwise normal. Given this patient’s most likely diagnosis, what is the most appropriate treatment?
A) Immediate surgical debridement
B) Intravenous piperacillin-tazobactam
C) Oral ciprofloxacin and discharge with close follow-up
D) Placement of a ciprofloxacin-instilled ear wick
Answer: B
This patient’s presentation is consistent with necrotizing otitis externa, a rare complication of acute otitis externa. Acute otitis externa is most commonly seen in young children and those who swim. The diagnosis requires the development of otalgia, ear itching, or ear fullness within the last 3 weeks. This must be associated with at least one of the following: diffuse ear canal edema or erythema or tragus or pinna pain with palpation. Fluoroquinolone otic drops are the mainstay of treatment for uncomplicated cases. If the ear canal is too edematous for drops to reach the deeper portions, an ear wick instilled with ciprofloxacin or ofloxacin should be used. If an ear wick is placed, close follow-up with an otolaryngologist should be arranged in the next 2–3 days.
For immunosuppressed patients (those with diabetes), systemic fluoroquinolones are recommended. The majority of patients improve with these treatments. However, older patients, those with diabetes, and immunocompromised patients with acute otitis externa may progress to the necrotizing form. This presents with similar symptoms to acute otitis externa with the addition of granulation tissue across the floor of the ear canal, purulent discharge, periauricular pain and swelling, headache, or any combination of these. Notably, as the infection spreads toward the base of the skull, cranial nerve palsies may result, with facial nerve involvement being the most common. Treatment depends on the severity of the case and risk factors for worsening infection (e.g., diabetes, immunosuppression, older patient). This patient has diabetes and systemic signs of illness (i.e., fever). He should be treated with intravenous antibiotics with pseudomonal coverage and admission. While these patients may need surgical debridement if the infection does not improve, antibiotics should not be delayed. Healthy individuals with mild infection and without systemic signs of illness may be discharged home with oral ciprofloxacin. However, given the severity of this infection and the potential for meningeal spread, there should remain a low threshold to admit these patients to ensure adequate improvement in the infection.
Immediate surgical debridement (A) was previously the mainstay of care in necrotizing external otitis, a rare complication of acute otitis externa. However, the bioavailability of antipseudomonal antibiotics has improved outcomes, limiting surgery as a confirmatory diagnostic procedure and as needed for granulation tissue removal.
Oral ciprofloxacin and discharge with close follow-up (C) is not appropriate in this patient with diabetes, signs of systemic illness, and evidence of peripheral nerve involvement. Outpatient treatment is reserved for healthy patients with early infection and adequate follow-up.
Placement of a ciprofloxacin-instilled ear wick (D) is a common treatment for acute otitis externa, as noted above, but treatment of necrotizing external otitis requires systemic ciprofloxacin.
Additional FOAM Resources:
- https://wikem.org/wiki/Malignant_otitis_externa#cite_note-3
- https://www.ncbi.nlm.nih.gov/books/NBK556138/
- https://pedemmorsels.com/otitis-externa/
- https://radiopaedia.org/cases/malignant-otitis-externa-4?lang=us
References:
- Rubin Grandis, J., Branstetter, B. F., 4th, & Yu, V. L. (2004). The changing face of malignant (necrotising) external otitis: clinical, radiological, and anatomic correlations. The Lancet. Infectious diseases, 4(1), 34–39. https://doi.org/10.1016/s1473-3099(03)00858-2Rubin Grandis, J., Branstetter, B. F., 4th, & Yu, V. L. (2004). The changing face of malignant (necrotising) external otitis: clinical, radiological, and anatomic correlations. The Lancet. Infectious diseases, 4(1), 34–39. https://doi.org/10.1016/s1473-3099(03)00858-2
- Al Aaraj MS, Kelley C. Malignant Otitis Externa. [Updated 2023 Apr 8]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK556138/
- Byun, Young Jae, Patel, Jaimin; Nguyen, Shaun A.; Lambert, Paul R.. Necrotizing Otitis Externa: A Systematic Review and Analysis of Changing Trends. Otology & Neurotology 41(8):p 1004-1011, September 2020. | DOI: 10.1097/MAO.0000000000002723
- Long, D. A., Koyfman, A., & Long, B. (2020). An emergency medicine-focused review of malignant otitis externa. The American Journal of Emergency Medicine, 38(8), 1671–1678. https://doi.org/10.1016/j.ajem.2020.04.083
- Rubin, J., & Yu, V. L. (1988). Malignant external otitis: insights into pathogenesis, clinical manifestations, diagnosis, and therapy. The American journal of medicine, 85(3), 391–398. https://doi.org/10.1016/0002-9343(88)90592-x
- Hosmer, K: Ear Disorders, in Tintinalli JE, Stapczynski JS, Ma OJ, Yealy DM, Meckler GD, Cline DM (eds): Emergency Medicine, A Comprehensive Study Guide, ed 8. New York, McGraw-Hill, 2016, Ch 242:p 1581-2.
- Al-Noury, K., & Lotfy, A. (2011). Computed tomography and magnetic resonance imaging findings before and after treatment of patients with malignant external otitis. European archives of oto-rhino-laryngology : official journal of the European Federation of Oto-Rhino-Laryngological Societies (EUFOS) : affiliated with the German Society for Oto-Rhino-Laryngology – Head and Neck Surgery, 268(12), 1727–1734. https://doi.org/10.1007/s00405-011-1552-8
- Cooper MA, Andrews JM, Wise R. Ciprofloxacin resistance developing during treatment of malignant otitis externa. J Antimicrob Chemother. 1993;32:163-4.
- Paramsothy, M., Khanijow, V., & Ong, T. O. (1997). Use of gallium-67 in the assessment of response to antibiotic therapy in malignant otitis externa–a case report. Singapore medical journal, 38(8), 347–349.
- Stokkel, M. P., Takes, R. P., van Eck-Smit, B. L., & Baatenburg de Jong, R. J. (1997). The value of quantitative gallium-67 single-photon emission tomography in the clinical management of malignant external otitis. European journal of nuclear medicine, 24(11), 1429–1432. https://doi.org/10.1007/s002590050172
- Carlton, D. A., Perez, E. E., & Smouha, E. E. (2018). Malignant external otitis: The shifting treatment paradigm. American journal of otolaryngology, 39(1), 41–45. https://doi.org/10.1016/j.amjoto.2017.05.010
- Franco-Vidal, V., Blanchet, H., Bebear, C., Dutronc, H., & Darrouzet, V. (2007). Necrotizing external otitis: a report of 46 cases. Otology & neurotology : official publication of the American Otological Society, American Neurotology Society [and] European Academy of Otology and Neurotology, 28(6), 771–773. https://doi.org/10.1097/MAO.0b013e31805153bd
- Trevino Gonzalez, J. L., Reyes Suarez, L. L., & Hernandez de Leon, J. E. (2021). Malignant otitis externa: An updated review. American Journal of Otolaryngology, 42(2), 102894–102894. https://doi.org/10.1016/j.amjoto.2020.102894






