Author: David Ediger, MD (EM Resident Physician, MAMC / Tacoma, WA), Rachel Bridwell, MD (@rebridwell, EM Resident Physician, San Antonio, TX) // Reviewed by: Brit Long, MD (@long_brit, EM Attending Physician, San Antonio, TX); Alex Koyfman, MD (@EMHighAK, EM Attending Physician, UTSW / Parkland Memorial Hospital)
Welcome to EM@3AM, an emDOCs series designed to foster your working knowledge by providing an expedited review of clinical basics. We’ll keep it short, while you keep that EM brain sharp.
A 51-year-old male with diabetes mellitus presents to the Emergency Department with pain in his left foot. The pain has been getting worse over the past week, and he is now having trouble walking. He does not check his blood sugar or see a doctor regularly. He denies drug use, recent surgery, or trauma. Review of systems is positive for fever and chills.
The patient’s vital signs include a blood pressure of 140/81 mmHg, a heart rate of 86 beats per minute, oral temperature of 101.2 F, respiration rate of 14 breaths per minute, with a saturation of 98% on room air. His physical exam is notable for a 3 cm ulcer over the plantar aspect of his left first metatarsophalangeal joint, with considerable surrounding warmth and erythema. Using a sterile instrument, bone was easily probed. His lower extremities have equal strength, though pinprick sensation is decreased in the feet bilaterally.
What is your next step in evaluation and treatment?
Answer: Osteomyelitis1-19
Osteomyelitis (OM) is an infection of bone, either due to direct inoculation or hematogenous spread.
Epidemiology and anatomy
- Bimodal age distribution: <20 years or >50 years1
- Adults: most commonly affects vertebrae, long bones, pelvis, clavicles2
- Intravenous drug use: hip, knee, ankle, sternoclavicular joint, cervical vertebrae, clavicle2,3
- Diabetes: foot, decubitus ulcers4,5
- Dialysis: spine, ribs, large joints3
- Sickle cell disease: long bones3
Microbiology
- OM in children is more commonly due to hematogenous spread6
- Risk factors: endocarditis, indwelling device, hardware, IV drug use, sickle cell disease, hemodialysis3
- Bacteremia allows bacterial biofilm formation in metaphyseal blood supply
- Inflammation causes swelling and formation of sequestrum (disrupted, necrotic bone) and involucrum (peri-sequestral new bone formation)2
- Typically monomicrobial, whereas direct inoculation is typically polymicrobial3
- Vertebral osteomyelitis can occur due to hematogenous spread of tuberculosis (Pott disease)7
- Usually subacute; constitutional symptoms less likely8
- Direct inoculation: contiguous spread from external source to bone; more common in adults7
- In patients with diabetes or vascular disease, compromised sensation, poor blood flow, and skin breakdown promote bacterial colonization of the skin and subsequent spread to bone3
- Other risk factors include surgery, orthopedic hardware, trauma/puncture wounds (consider Salmonella, Pseudomonas), and being bed- or wheelchair-bound7

History
- Typical symptoms of acute OM (onset over two weeks or less): musculoskeletal pain, limited range of motion, erythema, swelling, drainage from sinus tract/ulcer, constitutional symptoms (fever, chills)6,7,9
- Patients with diabetes may not have any signs of inflammation4
- Consider vertebral OM if: new/worsening neck or back pain, bloodstream infection, infective endocarditis, neurologic symptoms10
- Chronic OM (more than six weeks) may have a low-grade fever, nonspecific pain, poor wound healing, malaise, or ulcer drainage6
- Ask about diabetes, IV drug use, sickle cell disease, history of surgery or trauma, and presence of orthopedic hardware, prostheses, or indwelling catheters
- For kids, ask about irritability and changes in behavior or gait3,6
Physical exam
- Vital sign abnormalities (tachycardia, hypotension, tachypnea, fever) indicate severe infection and sepsis
- Intervene with appropriate sepsis management including antibiotics
- Examine for skin breakdown, erythema, swelling, ulcers, and drainage
- Assess range of motion of joints above and below complaint, neurovascular status, sensation
- Probe to bone is most sensitive test in diabetic foot ulcers; can rule in high-risk and rule out low-risk patients (sensitivity 87%, specificity 83%)11
Labs
- Leukocytosis is an unreliable predictor of acute or chronic osteomyelitis5,12
- C-reactive protein most sensitive (97%), decreases faster than ESR to indicate successful treatment
- Combined ESR/CRP in pediatric cases have 98% sensitivity13
- Serum procalcitonin may be a useful marker for acute osteomyelitis (sensitivity 85%, specificity 87% at a cutoff of 0.4ng/mL)14
- Blood cultures are typically low yield; obtain if patient is unstable3
- Positive for causative organism in 50% of hematogenous OM1
- Bone biopsy is the gold standard, though not necessary with positive cultures and radiographic evidence of osteomyelitis6
- Culturing skin or sinus tracts does not typically yield the causative agent; do not base antibiotic choice on superficial skin or wound cultures3
Imaging
- Radiographs
- May be normal early on; findings lag by up to two weeks6,15
- Need 1cm and 30-50% of bone affected to see changes on X-ray15
- Variable sensitivity (43-75%) and specificity (75-83%); cannot rule out acute osteomyelitis15
- May show soft tissue swelling, periosteal thickening/elevation, osteopenia/osteoporosis15
- May be normal early on; findings lag by up to two weeks6,15
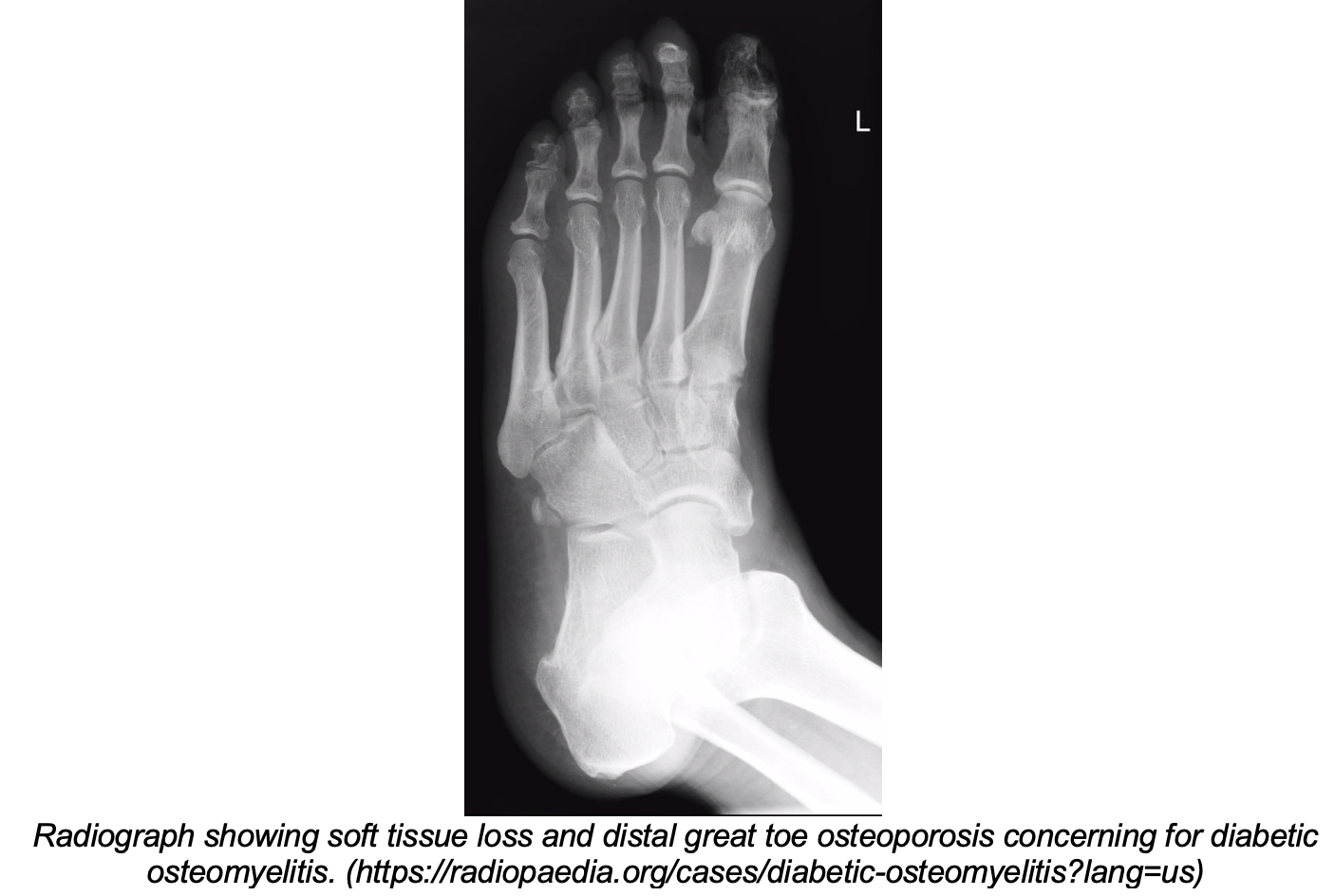
- Computed tomography (CT)
- May show thickened marrow density, intramedullary gas, necrotic bone15
- Poor sensitivity (67%), specificity (50%)15
- Main role is in detecting bone reactions (sequestra, involucra) in chronic osteomyelitis, identifying vertebral osteomyelitis, and surgical planning
- Ultrasound
- May show periosteal elevation earlier than radiographs, especially in children15
- Otherwise, low utility in diagnosis of OM
- Magnetic resonance imaging (MRI)
- Best modality to show early OM (as early as 3-5 days after onset), though often not available in the ED15
- If high suspicion for OM and plain films negative/indeterminate, admission is warranted to obtain MRI
- Sensitivity 82-100%, specificity 75-96%15
- T2/STIR: high signal, bone/soft tissue edema
- T1: ill-defined, low-signal intensity; dark, central abscess surrounded by non-enhancing sclerotic penumbra
- Best modality to show early OM (as early as 3-5 days after onset), though often not available in the ED15

Cierny-Mader classification9
- Osteomyelitis classification system; groups patients by overall health and location of infection
- Lower stages receive antibiotics, higher stages receive surgical intervention in addition to antibiotics

Management
- If clinically unstable, immediate resuscitation for sepsis with fluids, antibiotics, blood cultures
- Consult orthopedics for surgical evaluation and source control3,7
Antibiotic regimen
- Consult local antibiogram for hospital-specific antibiotic recommendations
- Ciprofloxacin has good bone penetration if there is concern for Salmonella16
- Vertebral OM: if treating empirically, consider coverage against MRSA, streptococcus, and Gram negatives (eg, vancomycin 15-20mg/kg IV q12 hours AND cefepime 2g IV q8-12 hours)10
- Prosthetic joint infection: surgical intervention, followed by 2-6 weeks of pathogen-specific IV antibiotics, plus rifampin 300-450mg PO BID17
- Course: 2-8 weeks, depending on surgery and response6,18

- Empiric: based on CA-MRSA rate19
- If <10%: nafcillin, oxacillin, or cefazolin
- If >10%: vancomycin or clindamycin
- If MSSA or GAS suspected: nafcillin 50-100mg/kg/day divided q8 hours OR oxacillin 50-100mg/kg/day divided q8 hours19
- Course: at least four to six weeks in MRSA osteomyelitis18
Disposition7
- Admit if septic or suspect hematogenous osteomyelitis to obtain MRI and additional workup
- Chronic OM: antibiotics (rifampin and fluoroquinolone), outpatient follow-up, local wound care in consultation with orthopedics
Pearls
- Most common organism is aureus; antibiotic regimens should cover MRSA
- Probe to bone is the most sensitive exam finding in diabetic foot ulcers
- C-reactive protein is the most sensitive lab, as well as a marker of successful treatment
- MRI is the gold standard imaging for diagnosing acute osteomyelitis
- If the patient is stable, withhold empiric antibiotics until a definitive microbiologic diagnosis is made

A 4-year-old boy presents to the emergency department with a limp and fever. His mother states that he began limping two days ago, and it has gotten progressively worse. He will no longer walk. His fever started today. His mother denies any known injuries. On physical examination, his temperature is 102.1°F with a heart rate of 130 beats per minute. His right hip is warm to the touch with overlying erythema present. He has limited range of motion of the right hip due to pain. Laboratory analysis reveals a leukocytosis with elevated erythrocyte sedimentation rate and C-reactive protein. X-ray of his right hip reveals periosteal thickening. An ultrasound of the right hip reveals a hip effusion. Which of the following is the most common cause of the patient’s presentation?
A) Bartonella henselae
B) Pseudomonas aeruginosa
C) Staphylococcus aureus
D) Streptococcus pyogenes
Staphylococcus aureus (S. aureus) is the most common cause of osteomyelitis in children, with methicillin-resistant S. aureus (MRSA) being more severe of an infection than methicillin-susceptible S. aureus (MSSA). Osteomyelitis is an infection of the bone. In children, the microorganisms most commonly enter the bone hematogenously. They may also enter the bone by direct inoculation from trauma or by local invasion from a nearby or contiguous infection, such as cellulitis. Clinical features include constitutional symptoms along with focal pain or limited function with a leukocytosis, an elevated erythrocyte sedimentation rate (ESR) and C–reactive protein (CRP), as well as imaging abnormalities. Plain radiographs should be the initial test to rule out other causes of pain, such as bone tumors or fractures. Characteristic findings of osteomyelitis on plain radiographs include periosteal reaction, periosteal elevation, and lytic lesions or sclerosis. If initial plain radiographs are negative and the diagnosis is still suspected, higher-level imaging should be considered. Magnetic resonance imaging (MRI) is the imaging modality of choice. Scintigraphy is recommended if MRI is not readily available. MRI is usually preferred in comparison to computed tomography (CT), however, if plain radiographs suggest significant bone destruction, then CT is better able to delineate changes in the bone. Ultrasonography can be a useful adjunct to evaluate possible fluid collections. The diagnosis is confirmed by bone biopsy and culture. Osteomyelitis is treated with a prolonged course of antibiotics.

Bartonella henselae (A) is incorrect. Bartonella henselae may cause osteomyelitis in children with cat scratch disease. Pseudomonas aeruginosa (B) is incorrect. Pseudomonas aeruginosa may cause osteomyelitis in children with nail puncture wounds to the foot. Streptococcus pyogenes (D) is incorrect. Streptococcus pyogenes may cause osteomyelitis in children as a complication of varicella-zoster infection.
Rosh Review website
Further Reading:
References
- Rauker N, Zink B. Bone and joint infections. In: Walls R, Hockberger R, Gasuche-Hill M, eds. Rosen’s Emergency Medicine: Concepts and Clinical Practice. 2nd ed. Philadelphia, PA: Elsevier; 2018:1693-1704.
- Lew DP, Waldvogel FA. Osteomyelitis. N Engl J Med. 1997;336(14):999-1007.
- Schmitt SK. Osteomyelitis. Infect Dis Clin North Am. 2017;31(2):325-338.
- Newman L, Waller J, Palestro C, et al. Unsuspected Osteomyelitis in Diabetic Foot Ulcers. JAMA. 1991;266(9):1246-1251.
- Ertugrul B, Savk O, Ozturk B, Cobanoglu M, Oncu S, Sakarya S. The diagnosis of diabetic foot osteomyelitis: Examination findings and laboratory values. Med Sci Monit. 2008;15(6):CR307-312.
- Hatzenbuehler J, Pulling TJ. Diagnosis and management of osteomyelitis. Am Fam Physician. 2011;84(9):1027-1033. doi:10.2165/00019053-199916060-00003
- Perron AD, Brady WJ, Miller MD. Orthopedic Pitfalls in the ED: Osteomyelitis. Am J Emerg Med. 2003;21(1):61-67. doi:10.1053/ajem.2003.50013
- Ferrer MF, Torres LG, Ramirez OA, Zarzuelo MR, Gonzalez N del P. Tuberculosis of the spine: A systematic review of case series. Int Orthop. 2012;(36):221-231. doi:10.1007/s00264-011-1414-4
- Carek P, Dickerson L, Sack J. Diagnosis and Management of Osteomyelitis. Am Acad Fam Physicians. 2001;63(12):2413-2420.
- Berbari EF, Kanj SS, Kowalski TJ, et al. 2015 Infectious Diseases Society of America (IDSA) Clinical Practice Guidelines for the Diagnosis and Treatment of Native Vertebral Osteomyelitis in Adults. Clin Infect Dis. 2015;61:26-46. doi:10.1093/cid/civ482
- Lam K, Asten SAV Van, Nguyen T, Fontaine J La, Lavery LA. Diagnostic Accuracy of Probe to Bone to Detect Osteomyelitis in the Diabetic Foot: A Systematic Review. Clin Infect Dis. 2016;63:944-948. doi:10.1093/cid/ciw445
- Armstrong D, LA L, M S, H A. Leukocytosis is a Poor Indicator of Acute Osteomyelitis of the Foot in Diabetes Mellitus. J Foot Ankle Surg. 1996;35(4):280-283.
- Paakkonen M, Kallio MJ, Kallio PE, Peltola H. Sensitivity of Erythrocyte Sedimentation Rate and C-reactive Protein in Childhood Bone and Joint Infections. Clin Orthop Relat Res. 2010;468:861-866. doi:10.1007/s11999-009-0936-1
- Maharajan K, Patro DK, Menon J, et al. Serum Procalcitonin is a sensitive and specific marker in the diagnosis of septic arthritis and acute osteomyelitis. J Orthop Surg Res. 2013;8(1):1. doi:10.1186/1749-799X-8-19
- Pineda C, Espinosa R, Pena A. Radiographic Imaging in Osteomyelitis: The Role of Plain Radiography, Computed Tomography, Ultrasonography, Magnetic Resonance Imaging, and Scintigraphy. Semin Plast Surg. 2009;23(02):080-089. doi:10.1055/s-0029-1214160
- Fong IW, Ledbetter WH, Vandenbroucke AC, Simbul M. Ciprofloxacin Concentrations in Bone and Muscle after Oral Dosing. 1986;29(3):405-408.
- Osmon DR, Berbari EF, Berendt AR, et al. Diagnosis and Management of Prosthetic Joint Infection : Clinical Practice Guidelines by the Infectious Diseases Society of America a. 2013;56:1-25. doi:10.1093/cid/cis803
- Liu C, Bayer A, Cosgrove SE, et al. Clinical practice guidelines by the Infectious Diseases Society of America for the treatment of methicillin-resistant Staphylococcus aureus infections in adults and children: Executive summary. Clin Infect Dis. 2011;52(3):285-292. doi:10.1093/cid/cir034
- Harik N, Smeltzer M. Management of acute hematogenous osteomyelitis in children. Expert Rev Anti Infect Ther. 2010;8(2):175-181. doi:10.1586/eri.09.130.Management






