Today on the emDOCs cast with Brit Long, MD (@long_brit), we cover the evaluation and management of the patient with a burn injury.
Episode 103: Thermal Burn Injury
Initial evaluation of thermal burns
- Range of burn severities and types: minor sunburns to full thickness burns and severe inhalation injury.
- Immediate goals are addressing the airway and hemodynamic instability. Always consider trauma and toxic exposure in the burn patient.
- Around 5% will have a concomitant injury from trauma.
- Most common traumatic injuries are fractures, TBIs, and thoracic or abdominal injuries.
- Try to obtain history on associated trauma including an explosion, substances burned (plastics are associated with cyanide, carbon monoxide toxicity), location (whether the burn occurred outdoors or in an enclosed space).
- Primary and secondary assessment, just like trauma; start with the ABCs.
- Evaluate for respiratory distress and smoke inhalation; fully expose to evaluate entire surface for burns.
- Burn injury assessment: depth, extent of TBSA, location.
- Depth: superficial, or first degree, partial thickness, which can be superficial and deep, full thickness, and 4th degree. Superficial burns are not included in assessment of TBSA.
- Burns are dynamic and will evolve.
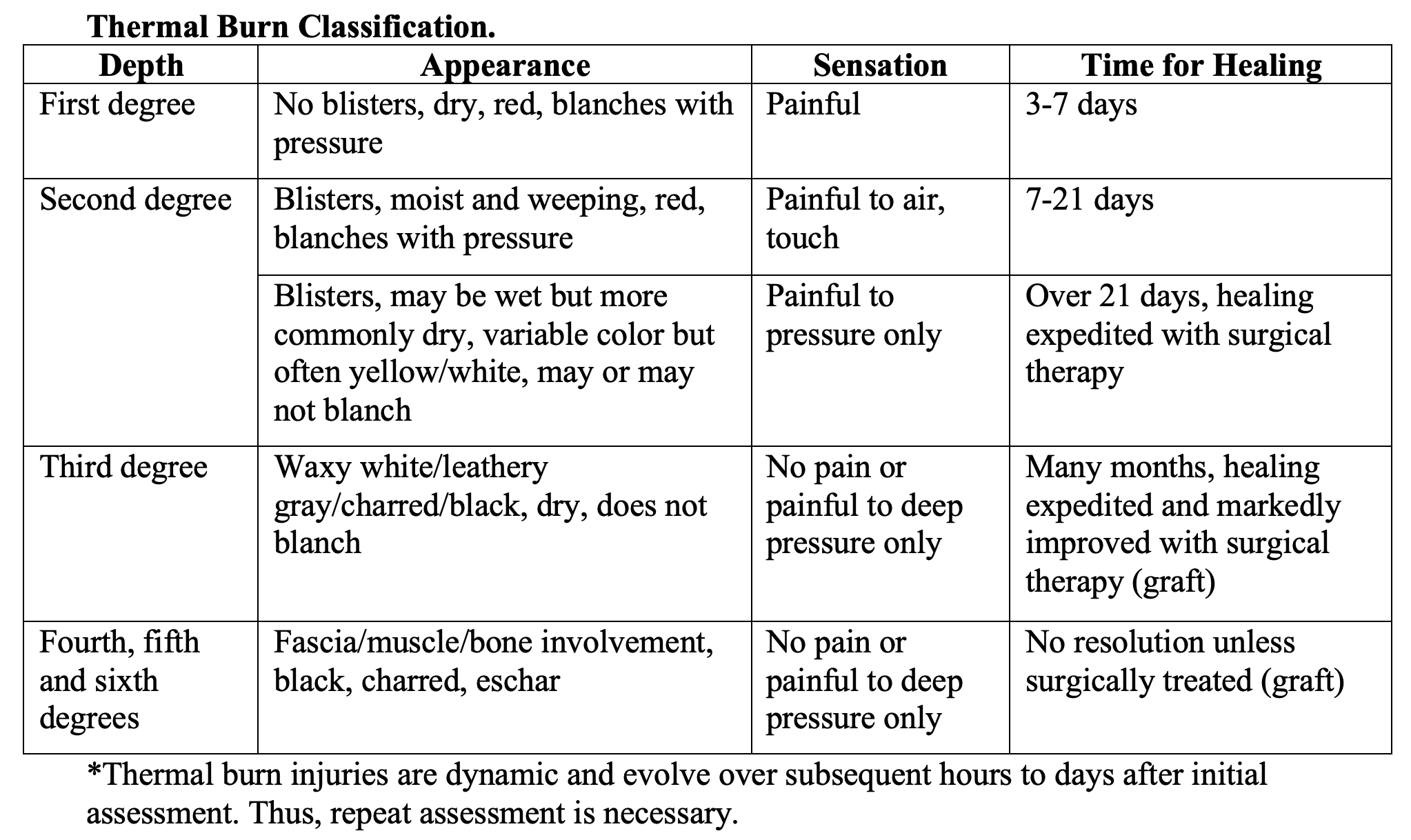
- Estimate TBSA: may use Lund-Browder chart (most accurate assessment in children and adults), Rule of Nines, or palm method (measure the burn by using patient’s entire palmar surface and fingers as 1% TBSA). Palm method likely best for burns < 15% (15 hands) or > 85% (number of hands not involved subtracted from 100%).
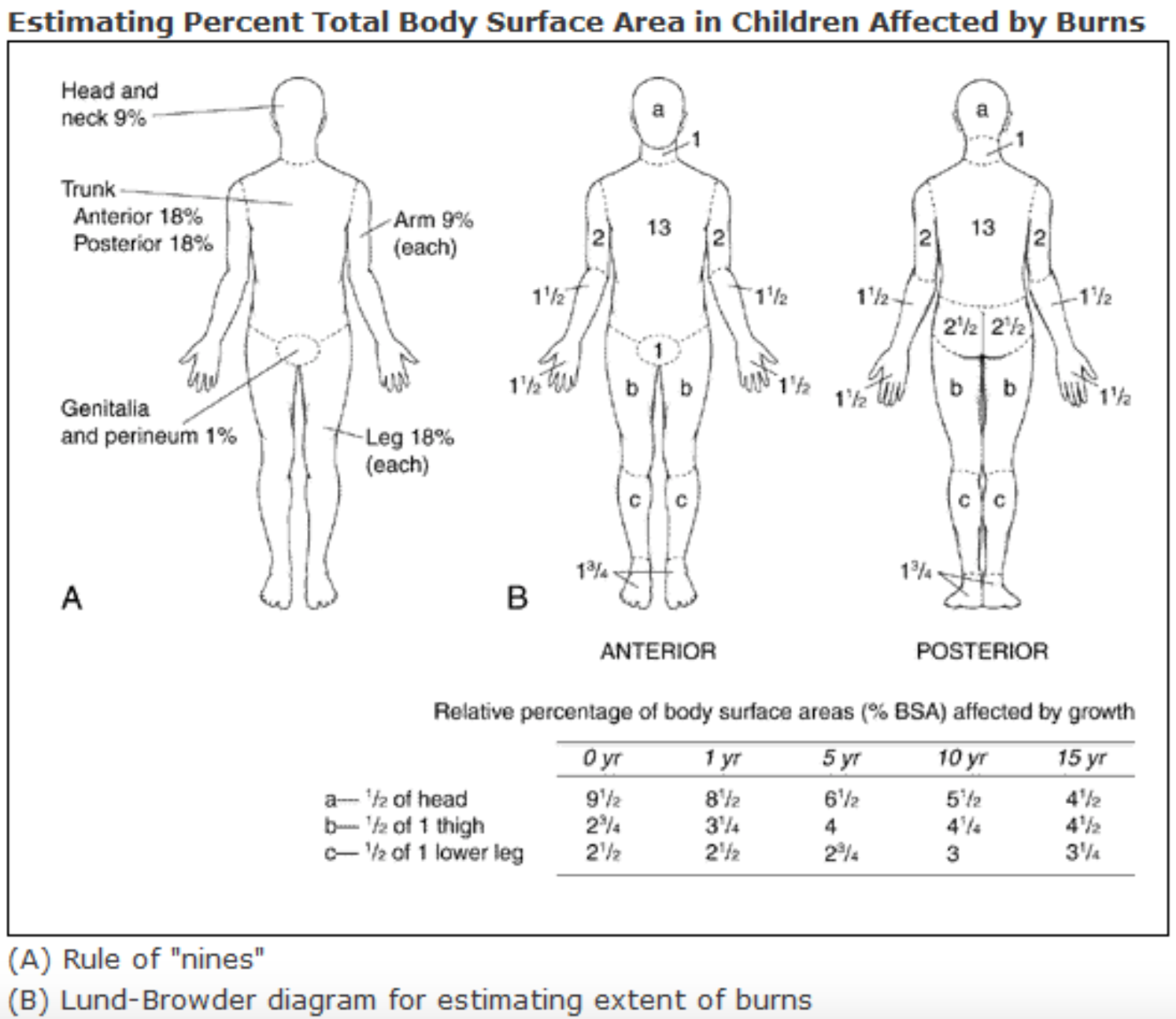
- Location: evaluate the neurovascular status in an extremity with circumferential or near circumferential burn injury. Chest burns/flank/back/abdominal burns may cause issues with ventilation.
- Consider escharotomy if there is any issue with perfusion or neurologic deficit, as well as difficult ventilation in the intubated patient.
Fluid resuscitation target and fluid
- Fluid resuscitation is one of the most important parts of management; goal is to increase intravascular volume and ensure end organ perfusion.
- Typically for adults with a TBSA of at least 20% or 10% in pediatric patients.
- Best option is two large bore IV lines through unburned skin, but may obtain IV access through burned skin if necessary. IOs and central lines are also options.
- Resuscitation is a balance between too little (hypoperfusion) and too much (risks of pulmonary edema, compartment syndrome, and abdominal compartment syndrome).
- Calculating fluid resuscitation:
- Parkland formula: 4 mL X % TBSA X weight in kilograms. Total amount over 24 hours. First half have over 8 hours, second half over 16 hours. May be associated with fluid overload.
- Modified Brooke formula: 2 mL X % TBSA X weight in kilograms. Total amount over 24 hours. First half have over 8 hours, second half over 16 hours. This formula is recommended by the ABA.
- ISR Rule of 10s:

- Must closely monitor vital signs and urine output. Target urine output is 0.3-0.5 mL/kg/hr for adults and 1.0 mL/kg/hr in kids. If lower than this, increase hourly rate.
- Consider using computer decision support software for fluid and urine tracking.
- Fluid choice: If traumatic injury and bleeding, administer blood products. For isolated burn injury, use balanced crystalloids like LR. Avoid normal saline.
- For large burns, consider albumin to lower total volume administration and improve urine output.
Managing the Burn
- Stop the burning process: remove burned clothing and debris from the burned area. Also remove any jewelry (edema).
- Update tetanus immunization if needed.
- Provide analgesia with multimodal approach: opioids, acetaminophen, ketamine.
- Cool burned area. Most effective means is with gentile irrigation using cool running water. Do not use ice, which makes the burn injury worse.
- If transferring, gently clean the wound and cover with a clean, dry sheet.
- If the patient does not need to be transferred, provide wound care.
- May remove ruptured blisters (covering is dead tissue and nonviable).
- If blister is clean and intact, management is more controversial. Do not use needle aspiration. If blister is large or overlies a joint, consider debridement. Other blisters may be left alone.
- Dressings: If available, use nonadherent mesh gauze with a thin layer of a topical antibiotic like bacitracin or mupirocin.
- Silver sulfadiazine used to be a major part of management, but current guidelines no longer recommend it (no clear benefit and may have negative impact on healing).
- Once wound is dressed, patient should be reassessed every 24 hours the first several days to evaluate wound and the burn depth.
- No role for prophylactic antibiotics in burn and inhalation injuries. May increase the risk of fungal infections and resistant organism.
- Severely burned patients have impaired thermoregulation and are at risk of hypothermia. Keep the room warm and cover patient with warm, dry blankets.
Inhalation injury
- Inhalation injury is one of the deadliest issues with burns. Most common in those trapped in an enclosed space for significant time with smoke.
- Mortality increases by 30% with inhalation injury.
- Systemic poisoning from inhaled toxins, obstruction of the upper airway from heat injury and edema, and chemical injury to the lower respiratory system from smoke inhalation.
- If the patient is altered after smoke exposure in an enclosed spaced, consider carbon monoxide or cyanide poisoning.
- CO toxicity: treat with supplemental oxygen.
- Cyanide toxicity: cyanocobalamin 5 g IV over 15 minutes (can be readministered in 15 minute if there’s no improvement). Side effects include red urine, red skin, hypertension, nausea, decreased lymphocytes, injection site reactions, and (rarely) acute renal failure. It may interfere with lab tests (obtain labs prior to administration).
- Inhalation injury presents with soot in posterior oropharynx, singed nasal hairs. Hyperacute presentation with upper airway signs/symptoms (shortness of breath, stridor/hoarseness, burns to face/neck) or lower airway signs/symptoms (shortness of breath, hypoxemia, wheezing, coughing).
- Strongly consider intubation for airway protection. Edema can rapidly worsen.
- Intubate with large ETT (>8.0) to assist with bronchoscopy, which is the gold standard evaluation and will assist with treatment.
- Acute pulmonary edema may occur 48-72 hours after burn.
Burn Center Consultation/Transfer
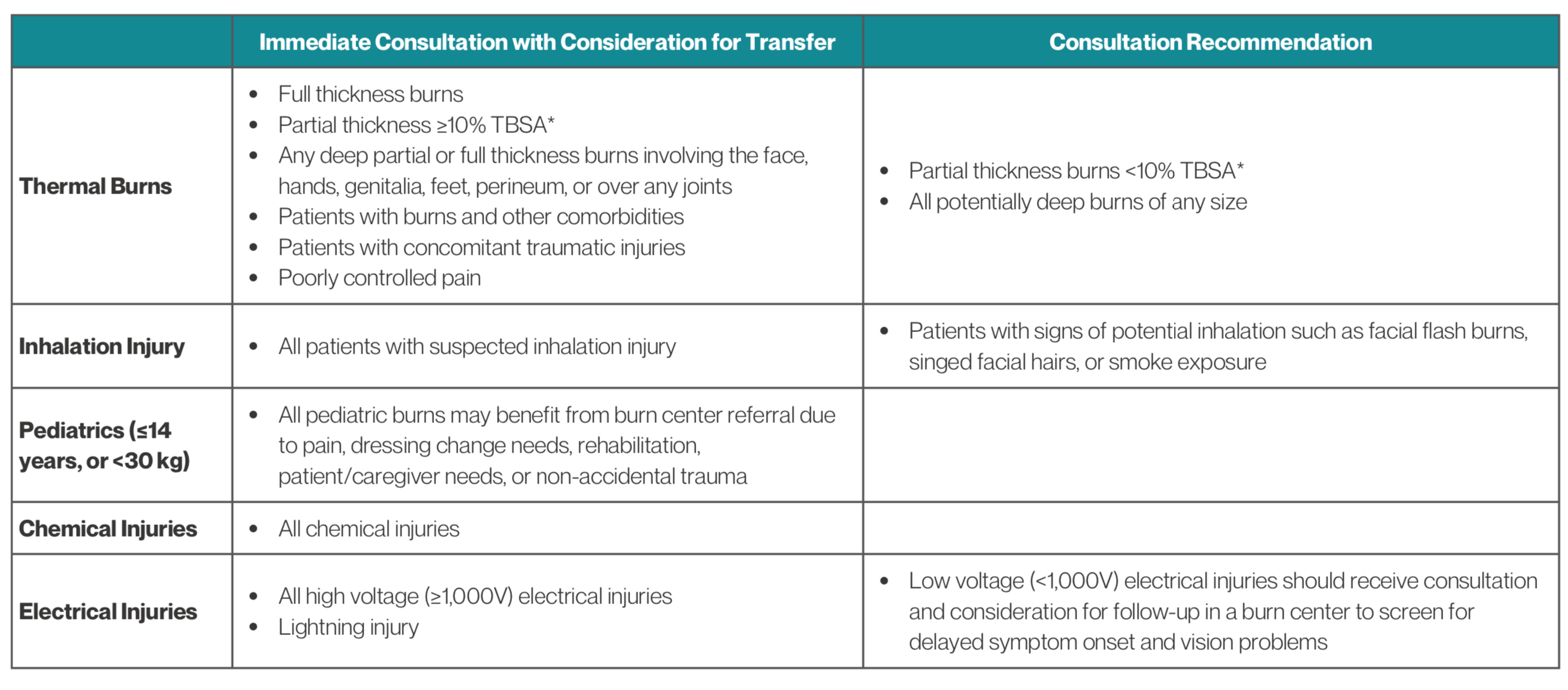
- The American Burn Association have several criteria on when to consider consulting a burn center and transferring.
- Partial thickness burns over 10% TBSA, burns involving the face/hand/feet/major joints/perineum, any third-degree burns, complicated burns like electrical or chemical burns, inhalation injuries, concomitant trauma, and patients with extensive comorbidities.
Summary:
- Patients with thermal burn injury should be assessed for traumatic injury and toxicologic exposure.
- Assessment of the thermal burn injury includes burn depth, extent, and anatomic location. TBSA should be assessed using the Lund-Browder Chart, Rule of Nines, or palm method.
- Fluid resuscitation should be initiated for those with > 20% TBSA according to the modified Brooke formula per the ABA and titrated to the patient’s clinical condition, vital signs, and urine output.
- Evaluate all thermal burn patients for inhalation injury.
- The American Burn Association has established criteria for which burn injuries require transfer to a dedicated burn center.
References
- American Burn Association. National Burn Repository 2019 Update, Report of data from 2009–2018. https://ameriburn.site-ym.com/store/ViewProduct.aspx?id=14191872 (2019).
- Cartotto R, Johnson LS, Savetamal A, Greenhalgh D, Kubasiak JC, Pham TN, Rizzo JA, Sen S, Main E. American Burn Association Clinical Practice Guidelines on Burn Shock Resuscitation. J Burn Care Res. 2024 May 6;45(3):565-589.
- ISBI Practice Guidelines Committee; Steering Subcommittee; Advisory Subcommittee. ISBI Practice Guidelines for Burn Care. Burns. 2016 Aug;42(5):953-1021.
- Hettiaratchy S, Papini R. Initial management of a major burn: II–assessment and resuscitation. BMJ. 2004;329(7457):101-103.
- Brandt CP, Yowler CJ, Fratianne RB. Burns with multiple trauma. Am Surg. 2002 Mar;68(3):240-3; discussion 243-4.
- Rosenkranz KM, Sheridan R. Management of the burned trauma patient: balancing conflicting priorities. Burns. 2002 Nov;28(7):665-9.





