Author: Marina Boushra, MD (EM Resident, Vidant Medical Center) // Edited by: Alex Koyfman, MD (@EMHighAK) and Brit Long, MD (@long_brit)
A 28-year-old G1P1 woman presents to the emergency department with two days of progressive, throbbing headache and blurred vision. Her medical history includes migraine headaches controlled with sumatriptan and an uncomplicated vaginal delivery one week ago. Her vitals upon arrival to the emergency department are HR 95, BP 150/97, RR 24, 94% on room air. Her exam is notable for photophobia and right upper quadrant tenderness to palpation. Neurological examination reveals global hyperreflexia.
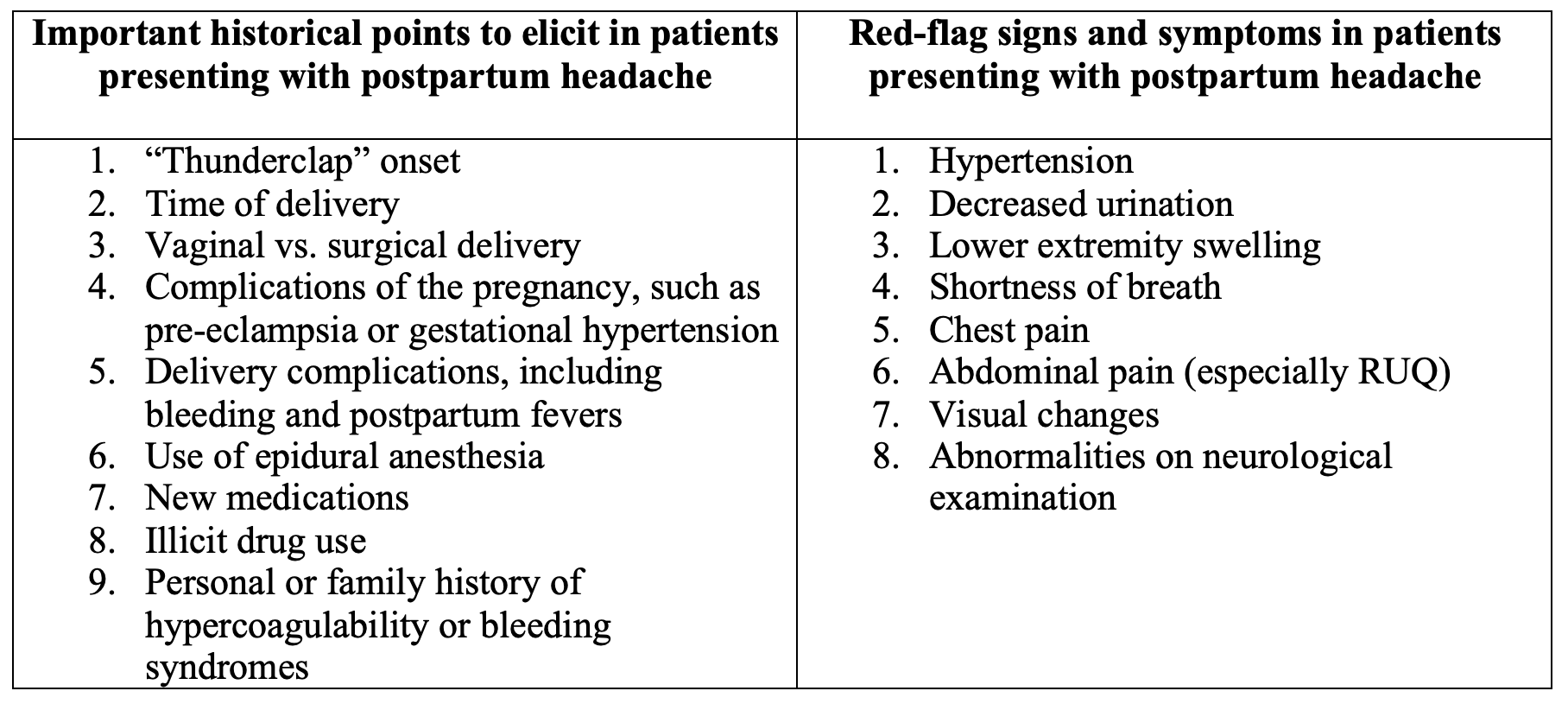
Headache is a common presenting complaint in the emergency department which disproportionally affects women of childbearing age and can be triggered by the sharp chemical and social changes surrounding the postpartum period1,2. Women in pregnancy and the puerperium period represent a diagnostic challenge, as this is typically a young and healthy population with a transient physiologic change that can increase the risk for acutely life-threatening disease. Their young age makes the prompt diagnosis of the life- and limb-threatening disease vital, as it presents an opportunity for acute intervention that accounts for a significant increase in both years lived and disease-free time. It also adds significant social and medicolegal consequences in the case of missed or delayed diagnosis in these patients. Headaches in the puerperium cover a broad diagnostic range from benign and common to rare and acutely life-threatening conditions. Data and research on postpartum headaches are skewed towards severe headaches, as many patients self-medicate with analgesics in the setting of mild or moderate headaches and, as such, never seek medical care. Because the features of many types of postpartum headaches overlap—and indeed, multiple headache syndromes can exist concurrently—differentiation of these diagnoses may be difficult. The threshold for advanced diagnostic testing and imaging is lower in this population than in those in a comparable age group, highlighting the importance of detailed history-taking and physical examination with vigilant attention to elicit red-flag historical features and symptoms as well as neurological findings, which are often subtle and easily overlooked.
Common Causes of Postpartum Headache
The complaint of headache is extremely common in the postpartum period. Prospective studies have shown acute headache syndromes affect more than one third of women in the first six weeks following delivery3. Primary headache disorders such as migraine, tension, cervicogenic, and cluster headaches are the most common cause of postpartum headache3. The most common secondary cause of postpartum headaches is spinal or post-dural puncture headache (PDPH) that results from spinal anesthesia during childbirth3,4. Together, primary headaches and PDPH account for approximately one-half of severe headache presentations in postpartum period3,5.
Primary Headache Disorders (Migraine, Cluster, Tension)
The postpartum period is rife with social and physiologic factors that may exacerbate primary headache disorders. Women in the postpartum period experience sleep deprivation, increased stress levels, disordered sleep cycles, and irregular nutritional intake, all of which may trigger primary headaches. Additionally, the dramatic fluctuations in estrogen, serotonin, and oxytocin levels associated with childbirth and breastfeeding may exacerbate underlying primary headache disorders1. In women with a primary headache disorder, approximately one quarter report acute headache exacerbation in the first postpartum week, and more than half report acute exacerbation in the first four weeks postpartum3. Patients presenting with primary headache typically report the same quality of headache as their baseline and should have no abnormal findings on neurological examination3. A change in the quality or severity of a patient’s baseline headache should trigger consideration for a secondary cause of postpartum headache, especially since women with a history of primary headache syndromes are at increased risk for multiple conditions that may cause secondary headaches5. While exacerbation of a primary headache disorder is the most common cause of headache in the postpartum period, the diagnosis should only be made after careful consideration of secondary causes of headaches. Pharmacologic treatment of acute exacerbations of primary headache disorders typically includes the use of dopamine antagonists6. Patients should be counseled on lifestyle changes to prevent further exacerbations of primary headaches, including rest and regular nutritional intake, though these changes are understandably difficult to achieve in households with a new baby7,8.
Post-Dural Puncture Headache (PDPH)
PDPH develops within five days of dural puncture and should spontaneously remit within one week of onset or within 48 hours of a therapeutic blood patch2. PDPH most commonly presents as a fronto-occipital headache9. The defining feature of PDPH is its positional nature9; these headaches should be exacerbated by sitting or standing and improve with lying flat. PDPH is commonly accompanied by neck stiffness, hypoacusia, photophobia, tinnitus, and nausea9. Neurological examination should be normal. Initial treatment is bedrest, analgesia, intravenous hydration, and caffeine supplementation. Patients who do not respond to this treatment within 48 hours may require a blood patch.
Uncommon but Life-threatening Causes of Postpartum Headache
The life-threatening causes of headache in the postpartum period are all secondary and may result from complications of anesthesia during delivery, primary intracranial pathology, or obstetric complications. The diagnosis of secondary causes of postpartum headaches is difficult and hindered by the fact that women with primary headache disorders are at increased risk for the development of hypertensive disorders of pregnancy as well as intracranial vascular catastrophes, all secondary causes of postpartum headaches10,11. In addition, the imaging modality of choice for the evaluation of headache in the emergency department setting—non-contrasted head CT—is often non-diagnostic of secondary causes of postpartum headache3. The literature on secondary headaches in the postpartum disorders is skewed, with most studies including only women whose headaches did not respond to conventional therapy or those who required hospitalization3. This may overestimate the incidence of secondary headaches in the postpartum population. Nevertheless, delayed or missed diagnosis in this group of likely otherwise healthy individuals has the potential for catastrophic medical, social, and legal outcomes. A high-index of suspicion for secondary causes of headache is, therefore, appropriate for patients in the postpartum period.
Preeclampsia/Eclampsia
Preeclampsia is a hypertensive disorder of pregnancy which may rarely present in the postpartum period and is a significant cause of maternal morbidity and mortality. Preeclampsia in both pregnancy and the puerperium presents as new onset hypertension (defined as two blood pressures greater than 140/90 mmHg taken at least four hours apart) with associated proteinuria or evidence of end-organ damage12. The greatest risk of postpartum preeclampsia is in the first 48 hours postpartum, though this disorder can present as far out as 6 weeks from the time of delivery13. Prodromal symptoms are non-specific and include headache, visual changes, and gastrointestinal symptoms such as abdominal pain and nausea. These are present in greater than 90% of patients14. These symptoms may be ignored by patients or overlooked by healthcare providers, leading to late presentation and diagnostic delay in a significant portion of these patients. Mild elevations in blood pressure—as low as 140/90 mmHg—that may otherwise go unnoticed in the emergency department or may be considered a reactive response to discomfort should trigger a comprehensive workup in pregnant women and those in the postpartum period. This work up should include a urinalysis, a spot urinary protein to creatinine ratio, complete blood count, chemistry, LFTs, uric acid, and a lactate dehydrogenase12. Work up should also include a chest x-ray, given that cardiopulmonary involvement is common in pre-eclampsia with severe features12. The development of seizures marks the transition to eclampsia, the most serious hypertensive disorder of pregnancy.
Posterior Reversible Encephalopathy Syndrome (PRES)
Posterior reversible encephalopathy syndrome (PRES) is a reversible disorder of the parietal and occipital lobes that presents with headache, altered mental status, visual changes, and seizures. Though PRES is most common in patients with hypertension, not all cases of PRES are associated with hypertension. Other risk factors for the development of PRES include autoimmune disorders, use of chemotherapeutic medications, renal disorders, and sepsis15. In the peripartum period, this disorder may easily be misdiagnosed as eclampsia, especially since preeclampsia-eclampsia is a major risk factor for the development of PRES16. The pathophysiology of PRES has not be clearly delineated, but current theories posit failed cerebral autoregulation due to underlying disease (such as the risk factors mentioned above), which leads to hypoperfusion-mediated endothelial injury and vasogenic edema15. Diagnosis is made based on history and neuroimaging, which shows bilateral, symmetric edema in the subcortical regions of the parietal and occipital lobes17. Hemorrhage is uncommon but is a poor prognostic indicator when present17. MRI is more sensitive than CT for the diagnosis of PRES, though CT is typically the first imaging modality used in diagnosis due to its widespread availability15. Like the symptoms, the imaging abnormalities associated with PRES are reversible and typically resolve completely within two weeks with appropriate treatment17. Treatment of PRES centers on identification and management of the underlying disease triggering the disorder, with strict blood pressure control being of utmost importance to prevent spread of edema and permanent cerebral damage15.
Meningitis
Literature on meningitis in the postpartum period is sparse and exists primarily as case reports. The largest and most recent study of meningitis in the postpartum period was conducted in the Netherlands and studied all cases of fatal meningitis in the postpartum period over 23 years (1983-2007)18. In this study, 87% of patients who went on to die from meningitis initially presented with a headache, most with associated altered mental status and/or fever18. Neck stiffness was uncommon, seen in only 5% of the patients in the study18. While antibiotic resistance is not typically an issue in meningitis, delayed diagnosis contributes to the significant mortality of this disease, which is estimated to be approximately 20% in adults19. Cerebral spinal fluid analysis following lumbar puncture is diagnostic. Head imaging prior to lumbar puncture should be done in cases where the patient has alteration in mental status or focal neurological symptoms. Diagnostic studies and imaging should not delay treatment with antibiotics. Though data is limited, the organisms associated with meningitis in the postpartum period are thought to be similar to those associated with meningitis in similarly aged individuals, most commonly Streptococcus pneumoniae, Neisseria meningitidis, and herpes simplex20. Empiric antibiotic treatment should target these organisms, and a common empiric regimen is a combination of vancomycin, ceftriaxone, and acyclovir21.
Strokes (Ischemic, Hemorrhagic)
Estimates of the incidence of postpartum strokes are varied, ranging from 4.3 to 210 per 100,000 women22. The large range for these estimates arises from difference in the populations studied, as well as differences in stroke classifications (ischemic, hemorrhagic, or venous in nature). While the exact rates of postpartum strokes are difficult to ascertain, postpartum strokes are a significant contributor to maternal mortality worldwide, with approximately 40% of survivors experiencing residual neurological sequelae23. Relative risk for all stroke subtypes is increased in the third trimester and the postpartum period24. Ischemic stroke incidence rises due to hypercoagulability in pregnancy reaching its peak in the immediate postpartum period25. Additionally, rising estrogen and progesterone levels lead to vasodilation and increased vascular distensibility, which is thought to contribute to the higher rate of rupture of vascular malformations and intracranial hemorrhages in this period as well25. While headaches are only associated with approximately 10% of strokes, the hallmark of stroke-associated headaches is the presence of abnormalities on neurological examination. While neurological symptoms may be caused by exacerbations of known underlying neurological disorders (ie multiple sclerosis) or a new non-pregnancy related disorder (brain neoplasm), the finding of neurological abnormalities in a patient with postpartum headache should trigger a thorough evaluation for causes of secondary headache, including brain imaging26. Neurological abnormalities are commonly subtle and difficult to elicit. The most common findings include diplopia, gaze palsy, nystagmus, aphasia, apraxia, and ataxia24. Headaches from stroke syndromes occur suddenly and either concurrently or shortly following the development of neurological symptoms24. If stroke is suspected, neurology should be consulted early to aid in patient management and disposition.
Sinus Venous Thrombosis
In the absence of a traumatic mechanism or underlying hypercoagulability disorder, the diagnosis of sinus venous thrombosis is almost entirely exclusive to females in the puerperium and those on estrogen-containing medications27. Symptoms of sinus venous thrombosis occur secondary to increased intracranial pressure due to impaired venous drainage, as well as focal brain injury from ischemia27. Symptoms from impaired venous drainage, which are typically subtle and include diplopia and papilledema, occur before symptoms of ischemic brain injury, and are often easily missed. As such, the presentation of sinus venous thrombosis is dauntingly broad, ranging from mild headache to altered mental status and coma28. Headache is the most common symptom in sinus venous thrombosis, found in approximately 90% of patients29. In one study, isolated headaches without neurological findings were found in 25% of patients, further highlighting the challenge this diagnosis can present to clinicians30. Headaches associated with sinus venous thrombosis are typically insidious in onset and can easily be misattributed to a primary headache disorder28. This diagnosis should be strongly considered in women in the postpartum period presenting with headache and diplopia or papilledema, even in the absence of other neurological symptoms or findings. When present, the most common neurological symptoms of sinus venous thrombosis are aphasia and hemiparesis31. Focal or generalized seizures are common, occurring in approximately 40% of patients31. Non-contrasted head CT, the most common initial imaging modality used in patients with a suspected secondary cause of headache, is only 30% sensitive for the diagnosis of sinus venous thrombosis27. CT venography is much more sensitive and equivalent to MR venography in the diagnosis of cerebral venous thrombosis27. Invasive diagnosis techniques such as angiography exist but are infrequently used. Anticoagulation is the primary therapy of choice for prevention of clot propagation and facilitation of recanalization32,33. Early neurology consultation and involvement is recommended.
Traumatic Intracranial Hemorrhage
The rates of domestic and intimate partner violence increase during pregnancy and the puerperium34. It is imperative to keep trauma with intracranial injury in the differential diagnosis for women presenting with headache in the puerperium, especially if they have no prior headache history. For patients in whom a potential traumatic mechanism is suspected as the cause of their headache, the patient should be interviewed separately from her partner. These patients should be provided with social resources such as safe houses, but if it is their decision to not report the abuse to authorities, this should be respected. Though physicians are not mandated reporters of domestic abuse and intimate partner violence, screening for potential abuse is extremely important in these patients, as the abuser likely presents a danger to the newborn child as well.
Pituitary Apoplexy
Pituitary apoplexy is a neuroendocrine emergency that results from hemorrhagic infarction of the pituitary gland and resultant hormone deficiencies. Pituitary apoplexy is more common in patients with an underlying pituitary mass but also increased incidence in the postpartum period35. This is due to pituitary gland hypertrophy and hyperplasia from the increased estrogen levels associated with pregnancy and the peripartum period35. Enlargement of the gland results in increased pressure in the sella turcica, leading to elevated risk of hemorrhage and thrombosis. Rapid changes in blood pressure—such as those seen in peripartum hemorrhage—further increases the risk for pituitary apoplexy in the puerperium. Headache is the most common presenting symptom and is classically referred retro-orbitally due to irritation of the ophthalmic branch of the trigeminal nerve. Involvement of the optic chiasm or optic nerve results in visual changes or visual field cuts. Cranial nerve palsies are also common, resulting from expansion of the pituitary into the cavernous sinus. Other symptoms may occur from associated hormone deficiencies and include amenorrhea and breastfeeding difficulty.
The most acutely life-threatening hormone deficiency associated with pituitary apoplexy is acute adrenal insufficiency. This condition results from adrenocorticotropic hormone deficiency and is a significant contributor to mortality from pituitary apoplexy. Steroid supplementation and management of electrolyte derangements are the cornerstones of management. Other hormone insufficiencies are more appropriately managed in the outpatient setting under the care of an endocrinologist.
Take Home Points
- Headaches are common in the postpartum period and have a broad differential diagnosis. While most postpartum headaches are benign in nature, secondary and life-threatening headache syndromes are more common in the puerperium.
- Exacerbations of primary headache disorders and post-dural puncture headaches account for more than half of emergency department presentations of headache in the postpartum period.
- Neurological manifestations of secondary headaches are often subtle and difficult to elicit, and any abnormality on neurological examination should lead to advanced imaging in postpartum patients.
- Preeclampsia and eclampsia can present up to six weeks postpartum. A headache may be the only neurological manifestation of severe preeclampsia, so particular attention should be paid to any blood pressure elevation in a postpartum patient.
- Women in the postpartum period are at increased risk for ischemic and hemorrhagic stroke as well as venous sinus thrombosis. CT has poor sensitivity for these conditions in the acute setting, so consider advanced testing with MRI.
References/Further Reading
- Klein AM, Loder E. Postpartum headache. Int J Obstet Anesth. 2010;19:422-430. doi:10.1016/j.ijoa.2010.07.009.
- Headache Classification Committee of the International Headache Society (IHS). The International Classification of Headache Disorders, 3rd edition (beta version). Cephalalgia. 2013;33(9):629-808. doi:10.1177/0333102413485658.
- Goldszmidt E, Kern R, Chaput A, Macarthur A. The Incidence and Etiology of Postpartum Headaches: A Prospective Cohort Study [L’incidence et La Cause Des Céphalées Du Postpartum : Une Étude Prospective]. https://link.springer.com/content/pdf/10.1007%2FBF03022061.pdf. Accessed September 2, 2018.
- Benhamou D, Hamza J, Ducott B. Post Partum Headache after Epidural Analgesia without Dural Puncture. Vol 4.; 1995. https://ac-els-cdn-com.jproxy.lib.ecu.edu/0959289X9582133U/1-s2.0-0959289X9582133U-main.pdf?_tid=611aea24-9fd0-47b5-80a9-6809550eb5c2&acdnat=1541424714_25cc1787d23e2892b8b8bfea90c5cc77. Accessed November 5, 2018.
- Raffaelli B, Siebert E, Körner J, Liman T, Reuter U, Neeb L. Characteristics and diagnoses of acute headache in pregnant women – a retrospective cross-sectional study. J Headache Pain. 2017;18(1):114. doi:10.1186/s10194-017-0823-1.
- Friedman BW, Grosberg BM. Diagnosis and management of the primary headache disorders in the emergency department setting. Emerg Med Clin North Am. 2009;27(1):71-87, viii. doi:10.1016/j.emc.2008.09.005.
- Rasmussen BK. Migraine and tension-type headache in a general population: precipitating factors, female hormones, sleep pattern and relation to lifestyle. Pain. 1993;53(1):65-72. doi:10.1016/0304-3959(93)90057-V.
- Boardman HF, Thomas E, Millson DS, Croft PR. Psychological, Sleep, Lifestyle, and Comorbid Associations With Headache. Headache J Head Face Pain. 2005;45(6):657-669. doi:10.1111/j.1526-4610.2005.05133.x.
- Kwak K-H. Postdural puncture headache. Korean J Anesthesiol. 2017;70(2):136-143. doi:10.4097/kjae.2017.70.2.136.
- Bushnell CD, Jamison M, James AH. Migraines during pregnancy linked to stroke and vascular diseases: US population based case-control study. BMJ. 2009;338:b664. doi:10.1136/bmj.b664.
- Facchinetti F, Allais G, Nappi R, et al. Migraine is a Risk Factor for Hypertensive Disorders in Pregnancy: A Prospective Cohort Study. Cephalalgia. 2009;29(3):286-292. doi:10.1111/j.1468-2982.2008.01704.x.
- ACOG Practice Bulletin No. 202: Gestational Hypertension and Preeclampsia. Obstet Gynecol. 2019;133(1):e1-e25. doi:10.1097/AOG.0000000000003018.
- Gynecology AC of O and. Hypertension in Pregnancy.; 2013. https://www.acog.org/~/media/Task Force and Work Group Reports/public/HypertensioninPregnancy.pdf. Accessed September 2, 2018.
- Yancey LM, Withers E, Bakes K, Abbott J. Postpartum Preeclampsia: Emergency Department Presentation and Management. J Emerg Med. 2011;40(4):380-384. doi:10.1016/J.JEMERMED.2008.02.056.
- Buyukaslan H, Lok U, Gulacti U, et al. Posterior reversible encephalopathy syndrome during the peripartum period: report of four cases and review of the literature. Int J Clin Exp Med. 2015;8(2):1575-1581. http://www.ncbi.nlm.nih.gov/pubmed/25932085. Accessed January 12, 2019.
- Brewer J, Owens MY, Wallace K, et al. Posterior reversible encephalopathy syndrome in 46 of 47 patients with eclampsia. Am J Obstet Gynecol. 2013;208(6):468.e1-468.e6. doi:10.1016/j.ajog.2013.02.015.
- Schweitzer AD, Parikh NS, Askin G, et al. Imaging characteristics associated with clinical outcomes in posterior reversible encephalopathy syndrome. Neuroradiology. 2017;59(4):379-386. doi:10.1007/s00234-017-1815-1.
- Schaap T, Schutte J, Zwart J, Schuitemaker N, van Roosmalen J, Dutch Maternal Mortality Committee. Fatal meningitis during pregnancy in the Netherlands: a nationwide confidential enquiry. BJOG An Int J Obstet Gynaecol. 2012;119(13):1558-1563. doi:10.1111/j.1471-0528.2012.03443.x.
- Thigpen MC, Whitney CG, Messonnier NE, et al. Bacterial Meningitis in the United States, 1998–2007. N Engl J Med. 2011;364(21):2016-2025. doi:10.1056/NEJMoa1005384.
- Lucas S. Acute bacterial meningitis during and after pregnancy. BJOG An Int J Obstet Gynaecol. 2012;119(13):1555-1557. doi:10.1111/1471-0528.12025.
- Brouwer MC, Tunkel AR, van de Beek D. Epidemiology, diagnosis, and antimicrobial treatment of acute bacterial meningitis. Clin Microbiol Rev. 2010;23(3):467-492. doi:10.1128/CMR.00070-09.
- Witlin AG, Mattar F, Sibai BM. Postpartum stroke: A twenty-year experience. Am J Obstet Gynecol. 2000;183(1):83-88. doi:10.1067/mob.2000.105427.
- James AH, Bushnell CD, Jamison MG, Myers ER. Incidence and Risk Factors for Stroke in Pregnancy and the Puerperium. Obstet Gynecol. 2005;106(3):509-516. doi:10.1097/01.AOG.0000172428.78411.b0.
- Camargo EC, Feske SK, Singhal AB. Stroke in Pregnancy. Neurol Clin. 2019;37(1):131-148. doi:10.1016/j.ncl.2018.09.010.
- Too G, Wen T, Boehme AK, et al. Timing and Risk Factors of Postpartum Stroke. Obstet Gynecol. December 2017:1. doi:10.1097/AOG.0000000000002372.
- van Zuthphen SW et al. Postpartum Stroke, a diagnostic challenge. 2008. doi:10.1016/j.ajem.2008.01.045.
- Bousser M-G, Ferro JM. Cerebral venous thrombosis: an update. Lancet Neurol. 2007;6(2):162-170. doi:10.1016/S1474-4422(07)70029-7.
- Saposnik G, Barinagarrementeria F, Brown RD, et al. Diagnosis and Management of Cerebral Venous Thrombosis. Stroke. 2011;42(4):1158-1192. doi:10.1161/STR.0b013e31820a8364.
- Ferro JM, Canhão P, Stam J, Bousser M-G, Barinagarrementeria F. Prognosis of Cerebral Vein and Dural Sinus Thrombosis. Stroke. 2004;35(3):664-670. doi:10.1161/01.STR.0000117571.76197.26.
- Crassard I, Bousser M-G. Céphalées au cours des thromboses veineuses cérébrales. Rev Neurol (Paris). 2005;161(6-7):706-708. doi:10.1016/S0035-3787(05)85124-0.
- Khealani BA, Wasay M, Saadah M, et al. Cerebral Venous Thrombosis. Stroke. 2008;39(10):2707-2711. doi:10.1161/STROKEAHA.107.512814.
- Einhäupl KM, Villringer A, Meister W, et al. Heparin treatment in sinus venous thrombosis. Lancet (London, England). 1991;338(8767):597-600. doi:10.1016/0140-6736(91)90607-Q.
- de Bruijn SFTM, Stam J. Randomized, Placebo-Controlled Trial of Anticoagulant Treatment With Low-Molecular-Weight Heparin for Cerebral Sinus Thrombosis. Stroke. 1999;30(3):484-488. doi:10.1161/01.STR.30.3.484.
- Mumford EA, Liu W, Joseph H. Postpartum Domestic Violence in Homes With Young Children: The Role of Maternal and Paternal Drinking. Violence Against Women. 2018;24(2):144-162. doi:10.1177/1077801216678093.
- Grand’Maison S, Weber F, Bédard M-J, Mahone M, Godbout A. Pituitary apoplexy in pregnancy: A case series and literature review. Obstet Med. 2015;8(4):177-183. doi:10.1177/1753495X15598917.









2 thoughts on “Headaches in the Postpartum Period”
Pingback: Huvudvärk postpartum – Mind palace of an ER doc
Pingback: Nursing FOAMed Review #10 (March 25th - May2nd) - Code Blue LLC