Authors: Carly Rosen, MD (Assistant Vice Chair of EMRA Health Policy Committee, PGY2 Mount Sinai Morningside-West); Gee Yoon S Park, DO (Vice Chair of EMRA Health Policy Committee, Ultrasound Fellow, Hospital of University of Pennsylvania); Summer Chavez, DO, MPH, MPM (University of Houston) // Reviewed by: Alex Koyfman, MD (@EMHighAK); Brit Long, MD (@long_brit)
Policy Playbook returns to emDOCs with a summary of the latest developments in the current procedural terminology (CPT) changes.

What is this about, and why should I care?
In 2019, The Center for Medicare and Medicaid Services adopted the American Medical Association’s proposition for the change in descriptors for CPT codes (Table 1). The changes were reviewed in July 2022 and will go into effect on January 1, 2023 (1, 2). A couple of important notes to keep in mind–First, this is the biggest overhaul to our documentation process in years. These changes will change our daily workflow as gone are the days of needing to count out ROS and physical exam systems. This will affect reimbursement for all. Finally, CMS has delayed “the implementation of the full transition to using only time to determine the substantive portion of a split/shared E/M service until 2024.” (3).

What is changing with ED CPT Coding Guidelines?
In the past, the CPT coding reflected the Emergency Service Index assigned to patients during the triage process as the level of reimbursement is primarily based on severity of the patient’s chief complaint. These current guidelines require strict documentation of History/Review of Systems, Physical Exam, and Medical Decision Making (4). CMS required a specific number of elements in each section to be documented appropriately to meet a level of service (2). This often caused excessive, irrelevant and/or repetitive documentation.
The new CPT guidelines, eliminates the burden of repetitive documentation and over documentation as billing relies solely on medical decision making (MDM). The level of the MDM takes into consideration the number and complexity of issues addressed, the amount of data reviewed, and the risk of morbidity and mortality during patient management (2,3,4). Table 1 displays the descriptors and criteria for each level of level of service based on the three elements of the MDM.
How is the MDM analyzed?
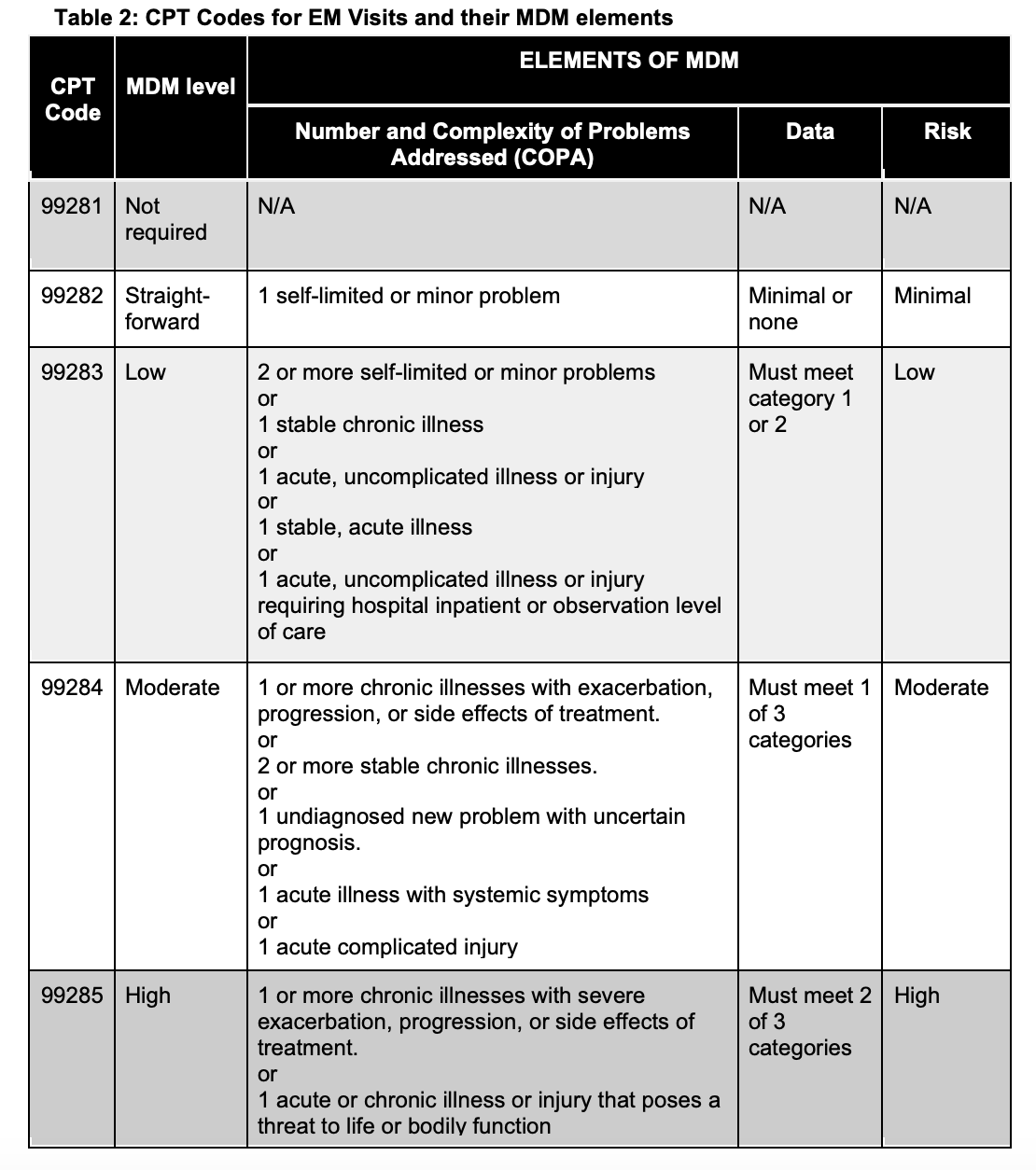
The billing level is determined based on if the complexity of the MDM is: N/A, straightforward, low, moderate, or high. The level of the MDM is based on two of the three elements being met (2,5). The three elements each have a grading system that is broken down further in Table 2. Listed below are some definitions and clarifications of the wording as each word in the CPT guidelines comes with specific criteria for classification (2,5).
- Number and Complexity of Problem(s) Addressed (COPA)
- Self-limited or minor problem: suture removal, dressing change, etc.
- Stable illness: illness at treatment goal
- Acute uncomplicated injury/illness: localized symptoms, minor trauma, no testing required
- Acute complicated injury/illness: requires evaluation of organ system, high mechanism of injury, requires testing/imaging
- Acute on chronic illness: illness with exacerbation, progression of symptoms, side effects of treatment
- Undiagnosed problem
- Acute illness with systemic symptoms: threat to bodily function
- Amount and complexity of data addressed and reviewed
- Category 1: Tests/Documents
- External note review (nursing home records, outpatient office, outside hospital visits)
- Test result review
- Order unique test
- Assessment requiring outside historian (EMS, friend, collateral)
- Category 2: Independent interpretation of tests (EKG, images)
- Category 3: Discussion of Management or Test Interpretation
- Don’t forget to document urine dip, urine HCG, fingerstick-glucose even in low acuity patients!
- Discussion with specialty consultants, social work, pharmacy
- Risk of complications and morbidity/mortality of the patient
- Complicating past medical history (hypertension, diabetes, cancer, substance use disorder including prior injection drug use, psychiatric history)
- Social determinants of health (housing, food insecurity, transportation)
- Category 1: Tests/Documents
What is changing with Critical Care Coding?
A couple of big changes to note with new proposal from CMS: changes of critical care time for 99292 and “Split or shared visits”
Traditionally, 99291 is billed for critical care time 30 minutes to 74 minutes and 99292 is billed for time spent above 75 minutes. 99292 was intended to bill for the first 60 minutes of critical care time. As 99292 had been set to bill for 75 minutes, 99291 included up to 74 minutes due to “Mid-Point Rule”. If you would like further explanation, you could read it here under “Technical Correction for Split (or Shared) Critical Care Services” (6). CMS has now changed the 99292 threshold to 104 minutes instead of 75 minutes, stating that “99292 is reportable for additional, complete 30-minute time increments furnished to the same patient (74 + 30 = 104 minutes)” (7).
Critical care time as of January 1st 2023:
99291: 30 minutes – 74 minutes (no changes)
99292: now requires a minimum of 104 minutes, as opposed to 75 minutes.
So, what do we do for patients we have spent 75-103 minutes on? Document appropriately following the new 99291 and 99292. In short, you could sign out to someone who could bill up to 74 minutes, however beyond that, it needs to be in 30-minute increments (8).
Secondly, CMS has delayed “split or shared visits” until 2024, however under its final policy, only ONE, “who performs the substantive portion of the visit” whether a physician or a non-physician practitioner (NPP), may bill if the patient was seen by both a physician and an NPP. This will be further discussed in the follow up articles as it will not go into effect starting 2023. For now, no changes starting January 1, 2023 for critical care visits when working with a NPP.
How will my documentation change?
Gone are the days of counting your systems and writing out a full story in the HPI. Now, pertinent history, signs/symptoms and physical exam findings are documented at the discretion of the physician and are not necessarily required for billing but should be documented for medical and legal purposes. Thorough documentation can be useful to communicate with other physicians and for lawyers when reviewing past cases. Furthermore, although the information outside the MDM may not be directly counted toward the billing of the case, the HPI and exam can help the coder understand the complexity of the issues at hand (9).
All of these changes may seem overwhelming, but it is relatively simple to meet the highest level of service. One major takeaway to consider is that in order to get “credit” for a medical condition in the COPA, you must specifically state how it is relevant to current patient presentation. An easy way to get extra credit in the data section is to chat with an outside historian (EMS, nursing home, friend, family, etc.). Reviewing patients’ past medical records and test results all count towards the complexity and amount/types data used. These are all things we do already but tend to forget to document. On a positive note, we may be saved from clicking fatigue with the new implementation.
For more in depth information and if you have other questions, check out ACEP’s FAQ.
This post is a collaboration between emDocs and the EMRA Health Policy Committee.

Resources
- https://www.acep.org/globalassets/sites/rc/media/presentations/special-briefing-intro-to-the-2023-documentation-guidelines-dmck-final-sent.pdf
- https://www.acep.org/administration/reimbursement/reimbursement-faqs/2023-ed-em-guidelines-faqs/
- https://www.acep.org/federal-advocacy/federal-advocacy-overview/regs–eggs/regs–eggs-articles/regs–eggs—november-2-2022/
- https://www.cgsmedicare.com/partb/mr/pdf/99285.pdf
- https://www.ama-assn.org/system/files/2023-e-m-descriptors-guidelines.pdf
- https://www.hospitalmedicine.org/policy–advocacy/letters/shm-submits-comments-on-2023-physician-fee-schedule-proposed-rule/
- https://www.federalregister.gov/documents/2022/07/29/2022-14562/medicare-and-medicaid-programs-cy-2023-payment-policies-under-the-physician-fee-schedule-and-other
- https://www.cms.gov/files/document/r11288cp.pdf
- https://www.acep.org/administration/reimbursement/reimbursement-faqs/critical-care-faq








