Author: Mohamed Elfatihi, MD (Senior EM Resident Physician, SUNY Downstate / Kings County Hospital, Brooklyn, NY) // Edited by: Alex Koyfman, MD (@EMHighAK) and Brit Long, MD (@long_brit)
Case: You are overnight in the Pediatrics ED when a 12-year-old male is brought in by EMS with stridor, fever, and cough. The patient is sick appearing, but you remember treating him earlier in the week for URI-like symptoms. He is awake and alert. You recognize that he is in respiratory distress and immediately begin to assess the airway.
Stridor is associated with a large airway obstruction. There are different characteristics to the sound of stridor based on the anatomical location of the obstruction, but harsh high-pitched sound is most common [1]. Inspiratory, expiratory, and biphasic can describe the timing in the respiratory cycle when it can best be heard. Stridor has multiple etiologies ranging from acute life threatening to more chronic and acquired causes. Initial management for stridor in the ED mirrors most other illnesses, starting with Airway, Breathing, and Circulation. History, age, and exam are crucial in generating a likely diagnosis to initiate immediate appropriate treatment.
Pathophysiology
To understand the origin of stridor we need to define the anatomical regions of the airways. The extrathoracic region includes two regions: 1) the supraglottic area consisting of nasopharynx, epiglottis, larynx, aryepiglottic folds, and false vocal cords, and 2) the glottic and subglottic area consisting of the trachea prior to entering the thoracic cavity. The glottic area is less vulnerable to collapse due to support from the cartilage and the tracheal rings that develop. The intrathoracic region consists of the airways that reside in the thoracic cavity [2]. Inspiratory stridor tends to suggest extrathoracic pathology, while expiratory stridor suggests intrathoracic pathology. Biphasic stridor is usually due to a fixed obstruction such as a foreign body [3].
Pediatric airways have many differences from adult airways. As you may recall in Poiseuille’s Equation, resistance is inversely proportional to the radius to the fourth power (r4).

Pediatric airways are narrower, producing a higher resistance in the pediatric airway, and any further strain in the anatomy from a disease entity can significantly lead to airway obstruction [2]. A second important physics phenomenon in pulmonary physiology is the Bernoulli effect. The Bernoulli effect states that fast moving air will have less pressure following it than slow moving air [2]. As you take a breath in (forced inspiration), the pressure in the trachea decreases comparably to atmospheric pressure [4]. In stridor caused by extrathoracic pathology, the Bernoulli effect results in a drop in the airway pressure beyond the obstruction, leading to the collapse of the airway walls and an increase in the obstruction. This collapse limits the airflow and causes increased turbulence and vibration of the airway walls generating the characteristic sound of stridor [2]. The Bernoulli effect occurs in intrathoracic obstruction as well but with forced expiration. In intrathoracic obstruction the pleural pressure is in play instead of the atmospheric pressure [4]. Biphasic stridor usually occurs due to a fixed obstruction from a mass or foreign body and is not dictated by the Bernoulli effect.
Differential Diagnosis
There is a wide differential in stridor. Etiologies can be due to infections, trauma, mechanical, allergic, congenital, and/or acquired syndromes, with several causes falling into multiple categories. Stridor causing pathologies can be acute, subacute or chronic.
Below is a partial list of etiologies that can cause stridor, but this list is not exhaustive of all causes. Etiologies in bold represent etiologies that can require emergent care.

Evaluation and Management
Airway assessment should be your initial focus. Signs of airway obstruction include stridor, tachypnea, retractions, drooling, trismus, dysphagia, patient in tripod or “Sniffing” positions, altered phonation, altered mental status, or severe fatigue [5]. Patients with stridor may be extremely ill appearing, and intervention should proceed diagnostic work up. Certain acute etiologies such as epiglottitis and bacterial tracheitis will likely require immediate airway intervention. If the clinical setting suggests the patient is stable but airway intervention will likely be needed shortly, the patient should be transported to the OR for anesthesia and ENT airway intervention. [6]. Unstable patient will require intubation in the ED. An endotracheal tracheal tube (ETT) size less than the age calculated size is needed to account for the airway edema from the underlying illness [7]. These intubations should be done by the most experienced, proficient provider [8]. It is important to have someone call for Anesthesia and ENT as backup, if possible, in the unstable patient that cannot be brought to the OR. Flex Fiberoptic tools are ideal as it more easily allows you to attempt an upright intubation to maintain an open airway position [9]. A surgical airway kit should also be at the bedside in case of sudden complete airway collapse. Supraglottic airways may worsen the airway obstruction by the pressure they exert on an epiglottis [9]. Pre-oxygenation is important prior to attempting any intubation. Take great care to immediately secure the ETT and initiate proper sedation to avoid the risk of tube dislodgement.
History and exam play important roles in making the appropriate diagnosis and providing the definitive treatment. Neonates and infants are more likely to have stridor as a result of congenital anomalies than adolescents, and toddlers are more likely to have croup than retropharyngeal abscesses [10]. Anaphylaxis can affect all ages. The acuity of onset will also be an important factor in accurate diagnosis. Epiglottitis, bacterial tracheitis, anaphylaxis, and foreign body aspiration are the most common acute causes of stridor. Croup, RPA, and PTA generally have a prodromal and subacute pattern. Other associated symptoms such as fevers, urticaria, dysphagia, and onset during specific activity such as feeding, sleeping, or crying will be important clues [11]. A history of prolonged intubations, trauma, or radiation can suggest more acquired pathologies. As discussed earlier, certain pathologies can be differentiated based on the timing of stridor in the respiratory cycle. Inspiratory stridor is more common and suggests a laryngeal obstruction, while expiratory stridor suggests tracheobronchial obstruction [2]. Some conditions may cause both inspiratory and expiratory stridor but will not necessarily be biphasic since the obstruction may be dynamic and evolving, whereas biphasic stridor is due to a fixed obstruction.

Diagnostic testing is tailored to specific etiologies of stridor. A CBC with WBC and cultures should be obtained if the symptoms are suspected or confirmed to be infectious. Radiographs would be necessary if foreign objects are suspected, or atypical presentations. However, in patients presenting with croup, radiograph is low yield [2]. Neck radiographs can help assess the retrotracheal space or look for a “thumbprint” or “Steeple” sign. Computed Tomography (CT) can be useful in surgical planning for deep space infections [6].

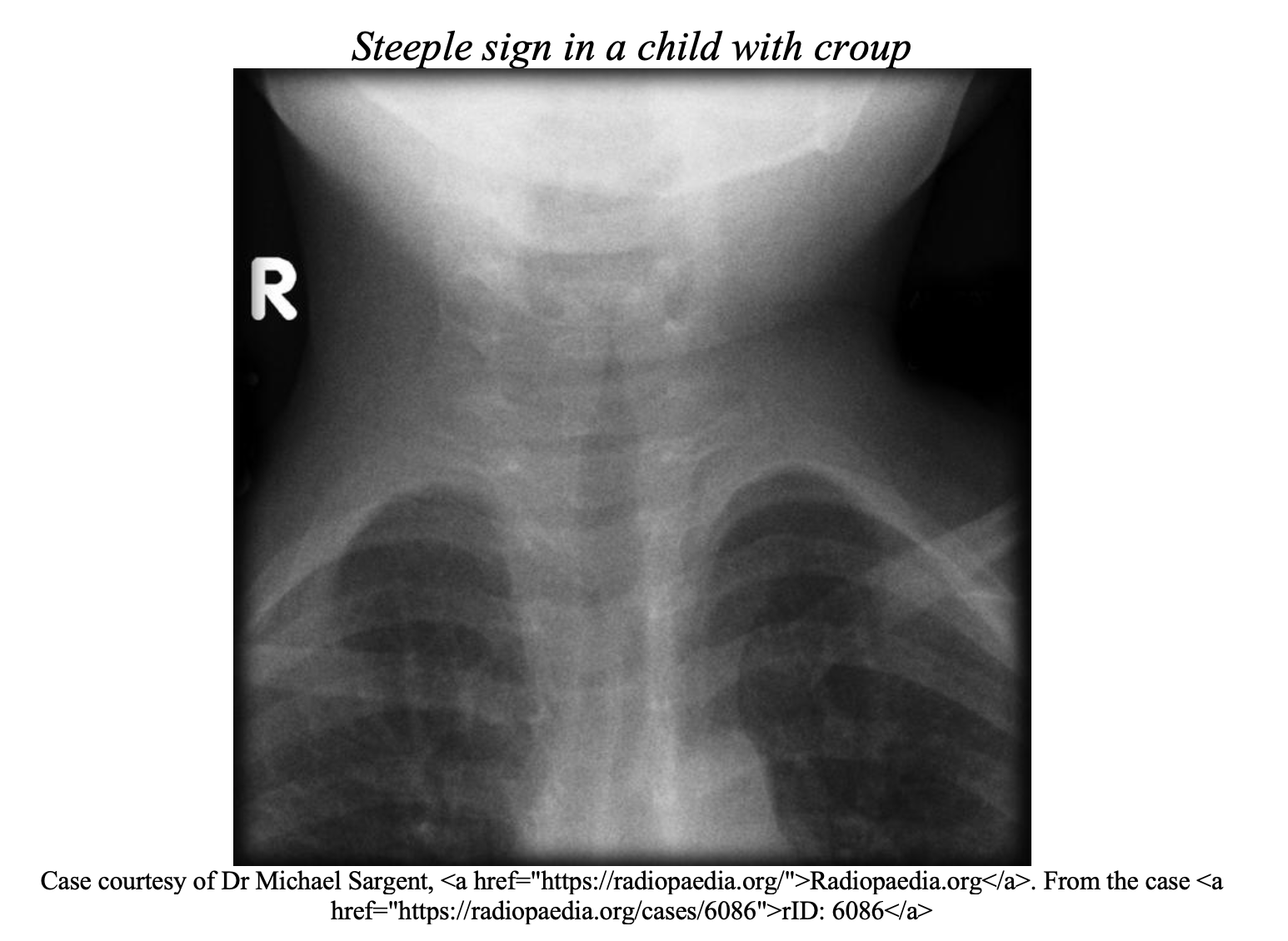
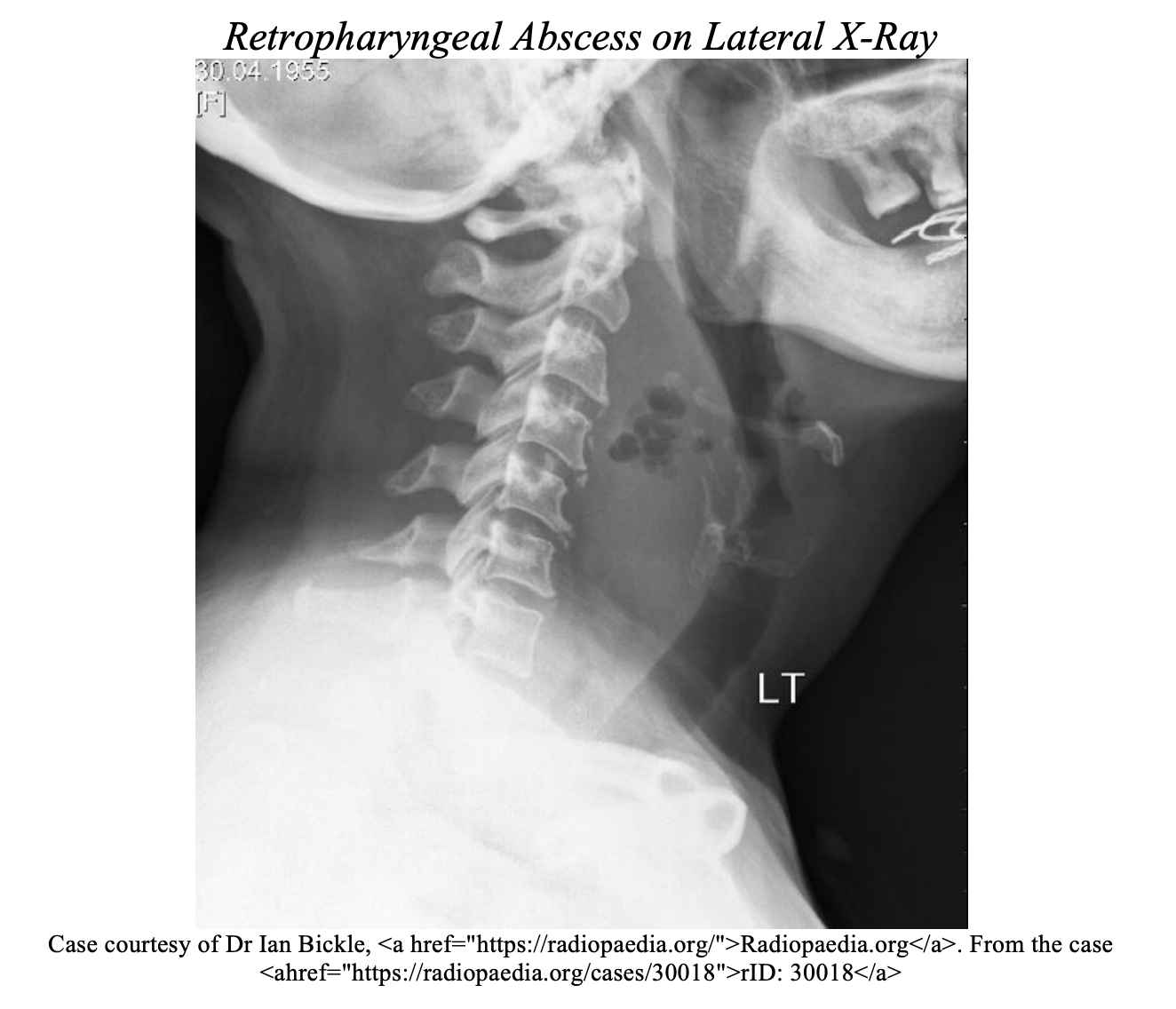
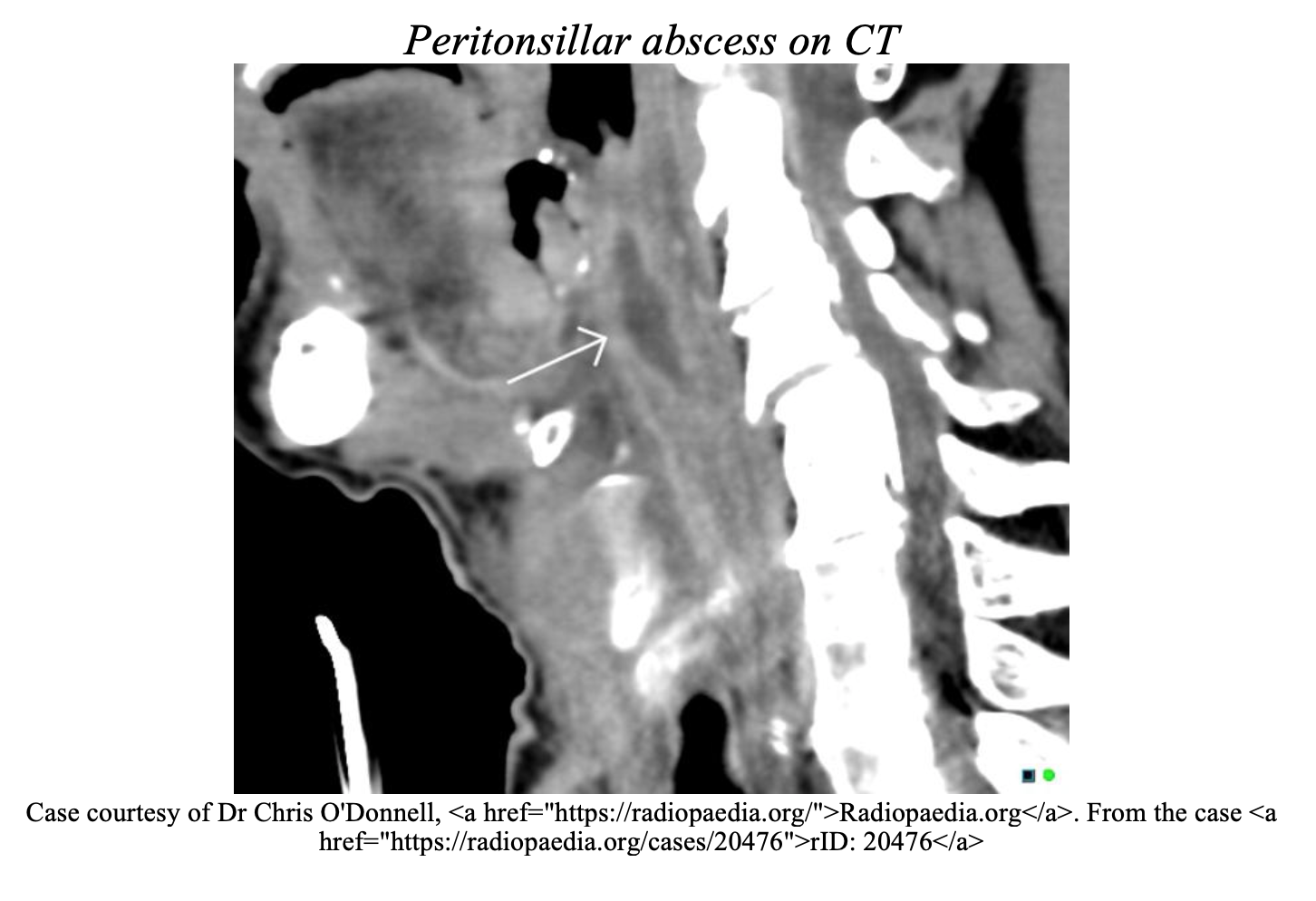
CT and MRI may be useful in chronic stridor to assess for stenosis or anatomic anomalies. Ultimately, direct visualization by a specialist will likely be the gold standard for definitive diagnosis of most pathology and especially for foreign body removal [12]. Direct laryngoscopy will provide definitive diagnosis and also assist in securing the airway if needed. Nasopharyngoscopy can be done in the ED by trained specialists in stable un-sedated patients. If radiographs are to be obtained in a stable patient with suspected acute pathology, a clinician should accompany the patient with appropriate airway equipment in case of decompensation [2]. Broad spectrum antibiotics, epinephrine, steroids, drainage and other interventions to treat the underlying pathology will be tailored to the specific etiology of stridor (see Table).

Case Conclusion
You recognize that the patient has stridor, fever, and is ill appearing with rapidly progressing symptoms and impending respiratory collapse. Bacterial tracheitis and epiglottitis are at the top of your differential, but regardless, the initial treatment is the same [11]. You discuss the patient with ENT and Anesthesia. The patient is placed on a monitor, being careful to not further agitate the patient, and immediately taking to the OR for definitive airway management.
Take home points
- Rapid intervention should proceed diagnostic work up in the ill-appearing patient.
- Intubation for ill-appearing patients should be performed by proficient healthcare clinicians, with ENT and anesthesia consultation recommended.
- A smaller ETT should be ready for a smaller than anticipated airway due to edema.
- Stridor, fever, and rapidly progressing symptoms are most likely to be epiglottitis or bacterial tracheitis.
- In afebrile patient with stridor and progressively worsening symptoms, consider foreign body, anaphylaxis, or thermal epiglottitis in the appropriate clinical setting.
- A clinician with appropriate airway equipment should accompany stable patients to radiology in case of deterioration.
- There is a wide differential for stridor, but this can be narrowed based on the timing of stridor in the respiratory cycle, age of patients, and acuity.
References/Further Reading
- Sly PD, Collins RA. Physiological basis of respiratory signs and symptoms. Pediatric Respiratory Reviews 2006; 7:84.
- Fakhoury, K MD, Quinteror, D MD. Assessment of stridor in children. Post TW, ed. UpToDate. Waltham, MA: UpToDate Inc. https://www.uptodate.com
- Benson, B. Stridor. [online] Emedicine.medscape.com.Available at: https://emedicine.medscape.com/article/995267-overview
- Doherty, G. (2015). Acute and chronic airway obstruction in children. Anaesthesia & Intensive Care Medicine, 16(12), pp.616-621.
- Loftis, L MD.Emergency evaluation of acute upper airway obstruction in children. Post TW, ed. UpToDate. Waltham, MA: UpToDate Inc. https://www.uptodate.com
- Yiannakis, C. and Hilmi, O. (2018). Evaluation and management of acute upper airway obstruction. Surgery (Oxford), 36(10), pp.560-568.
- Al-mutairi B, Kirk V. Bacterial tracheitis in children: Approach to diagnosis and treatment. Paediatr Child Health. 2004;9(1):25-30
- Pfleger, A. and Eber, E. (2013). Management of acute severe upper airway obstruction in children. Paediatric Respiratory Reviews, 14(2), pp.70-77.
- Rich, L. (2019). Intubating a Patient with Epiglottitis – Emergency Physicians Monthly. [online] Emergency Physicians Monthly. Available at: http://epmonthly.com/article/intubating-a-patient-with-epiglottitis/ [Accessed 25 Feb. 2019].
- Armstrong, E. and Bell, G. (2019). Acute and chronic airway obstruction in children. Anaesthesia & Intensive Care Medicine, 20(1), pp.35-41.
- Zoumalan R, Maddalozzo J, Holinger LD. Etiology of Stridor in Infants. Ann Otol Rhinol Laryngol. 2007;116(5):329–334
- Pfleger A, Eber E. Assessment and causes of stridor. Paediatr Respir Rev. 2016;18:64-72.
- Green SM. A is for airway: a pediatric emergency department challenge. Ann Emerg Med. 2012 Sep;60(3):261-3. doi: 10.1016/j.annemergmed.2012.03.019. Epub 2012 Apr 19. PubMed PMID: 22520991.
- Tintinalli, Judith E., et al. Tintinalli’s Emergency Medicine: A Comprehensive Study Guide. Eighth edition. New York: McGraw-Hill Education, 2016.
Here are emDocs articles that specifically cover a couple of Stridor causing etiologies:
- Facial swelling: Etiologies, Presentations, Evaluation, and Management http://www.emdocs.net/facial-swelling-etiologies-presentations-evaluation-and-management/
- More Than a Sore Throat: Evaluation and Management of Retropharyngeal Abscess in the Adult:http://www.emdocs.net/sore-throat-evaluation-management-retropharyngeal-abscess-adult/
- Croup: ED-focused Highlights: http://www.emdocs.net/croup-ed-focused-highlights/
- Management of Epiglottitis in the Community Setting: http://www.emdocs.net/management-epiglottitis-community-setting/








