Author: Anthony DeVivo, DO (@anthony_devivo, EM Resident Physician, Mount Sinai St. Luke’s-West) // Edited by: Alex Koyfman, MD (@EMHighAK); Brit Long, MD (@long_brit); and Manpreet Singh, MD (@MprizzleER)
Welcome back to Unlocking Common ED Procedures! Today, we look at knee arthrocentesis.
Check out our new downloadable procedure card with QR code link to the article. Print them out and be ready to go over it with your learners!
Case
A 56-year-old female with past history of HTN and DM presents to the ED for 4 days of progressively worsening right sided knee pain. She affirms being diagnosed with osteoarthritis of her bilateral knees several years ago but has never had such significant pain or swelling before. She has also been experiencing generalized myalgias and chills. She denies any recent trauma to her knee or wounds of any kind. On exam, she is found to have bilateral knee effusions. However, the right knee is erythematous, warm to the touch, and significantly more tender to palpation than the left.
Background
Joint pain is a particularly common presentation to the ED, and while history and physical exam can often assist in differentiating the etiologies, confirmation of several pathologies requires a diagnostic arthrocentesis.1In particular, as in the case above, an arthrocentesis is necessary for assessment if there is any concern for a septic joint. However, not every septic joint will present with systemic symptoms, or an isolated joint with obvious clinical signs concerning for infection. Patients with long standing arthritis, gout, or chronic lower extremity venous insufficiency can be particularly difficult to assess for underlying joint space infection. So how can physicians differentiate which patients need an arthrocentesis? Are there specific approaches or techniques that are more favorable over others? When do we need to call orthopedics? These questions plus many more will be addressed below with particular emphasis on the performance of a knee arthrocentesis.
An arthrocentesis is the means by which physicians gain access to the synovial fluid contained within a joint space either for therapeutic and/or diagnostic means.1 Analysis of this fluid can provide invaluable information about the etiology of a joint space effusion as well as direct further management.1,2 In addition, large joint space effusions can be cause patients significant pain as well as difficulty with joint range of motion, and thus drainage can allow for symptomatic relief.
Indications:1-4
- Diagnosis of a joint space infection
- Diagnosis of crystal-induced arthropathy
- Assessment of undifferentiated inflammatory arthropathies
- Assessment of post-traumatic joint space effusion
- Therapeutic aspiration of large joint-space effusion in order to decrease intra-articular pressure.
Contraindications:
While there is no evidence to support any absolute contraindications to performing an arthrocentesis, there are relative contraindications that predispose patients to complications to the procedure.
- Signs of cellulitis overlying the joint
- While an arthrocentesis is often performed in order to assess for joint space infection, evidence of overlying skin infection is a relative contraindication to the procedure due to concern for potential introduction of bacteria into the joint space. The signs of overlying skin infection can be difficult to differentiate from reactionary changes of the skin overlying the joint due to joint space inflammation, and so careful history and examination should be performed prior to the procedure. There is no significant data quantifying the risk of iatrogenic infection, but nevertheless it is advisable to choose a procedure point of entry without signs of cellulitis if possible.5
- Coagulopathy
- There is no evidence to support any specific degree of coagulopathy that places a patient at higher risk for developing post-procedural bleeding or the development of hemarthrosis. There is substantial literature to support the safety and lack of increased post-procedural bleeding in the setting of oral anticoagulation including direct oral anticoagulants and warfarin.6-8 However, caution should be taken with performing any invasive procedure in the setting of coagulopathy, and the risk/benefits of the procedure should be discussed.
- Prosthetic joint
- While there is no clear literature supporting the deferment of arthrocentesis in prosthetic joints, it is generally accepted that these should be performed by orthopedists. This is likely due to the distortion in anatomy from joint hardware placement and this risk of possible iatrogenic infection of that hardware. In particular, periprosthetic joint infection has a 1-3% prevalence, and so early orthopedic consultation despite arthrocentesis should be obtained.9
Knee Anatomy:
- Due to the size of the synovial joint space of the knee, an arthrocentesis can be performed from multiple entry points, including superior, inferior, medially, and laterally to the patella.1,10-11 To maximize the joint space diameter for needle entry, the procedure may be performed with the knee either fully extended or flexed at 10 to 20 degrees.10 Flexion may be facilitated by placing a pillow or towel roll under the knee. After appropriately positioning the knee, palpate around the patella in order to assess where the widest joint space for needle entry is. There are 3 possible approaches to a knee arthrocentesis, all of which can be performed from the medial or lateral aspect of the knee.12
- Superior- 1cm superior and 1cm either medial or lateral to the patella.
- Midpoint- 1cm medial or lateral to the midpoint of the patella.
- Inferior- This approach can be performed either in the position suggested above or with the knee flexed to 90 degrees. The entry site should be 0.5cm below the inferior most medial or lateral border of the patella.
- In all approaches, the needle should be directed posteriorly to the patella while remaining horizontal in relation to the joint space. In the superior and midpoint approach, the needle should be directed towards the intercondylar notch of the femur.
- There have been no studies to date that have definitively proven superiority of one particular approach to diagnostic knee arthrocentesis. There is some evidence showing that in the setting of smaller joint space effusion of the knee, fluid is more commonly distributed to the superolateral aspect of the knee.13 This may suggest, that in the case of small joint effusions, the superolateral approach may be more likely to yield fluid in a diagnostic arthrocentesis. However, additional studies are necessary to substantiate this, as well as whether or not any one approach is superior for knee arthrocentesis.
- In the setting of small joint effusions, ultrasound can be used to assess fluid distribution in order to ascertain the best approach.13 In addition to fluid pocket localization, dynamic ultrasound guidance can be used to confirm needle entry into the fluid pocket. A recent systematic review of 9 studies showed a significant difference in accuracy rate in favor of the use of ultrasound over landmark based arthrocentesis.14 In opposition, a smaller emergency department based study from 2010 showed no improvement in overall procedural success in ultrasound vs landmark based arthrocentesis of the knee.10 Thus, ultrasound has not yet become the standard of care for arthrocentesis, and further literature is needed to discern whether ultrasound guidance is superior to landmark based joint aspiration, as well as what approach is superior.
X-ray with effusion:
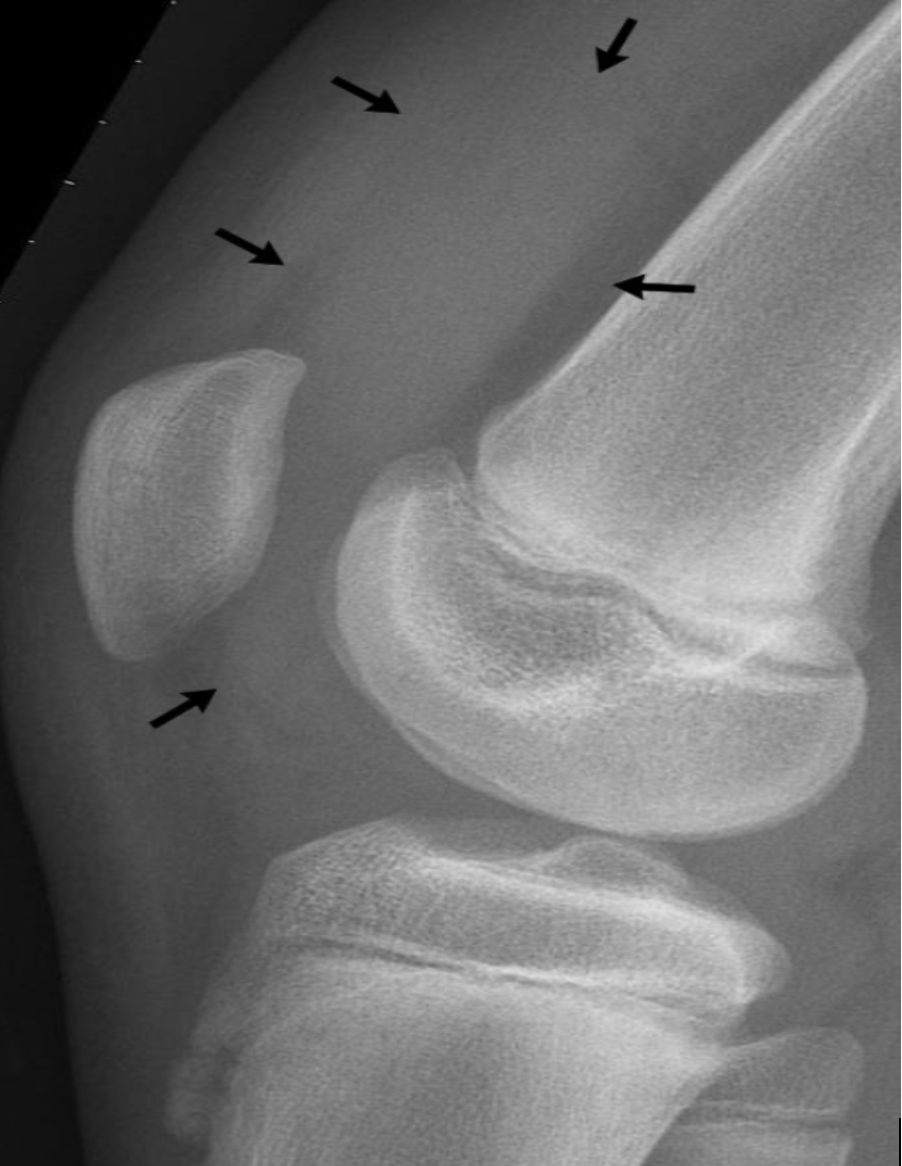
Ultrasound depicting knee effusion:

The Procedure
- Positioning
- As in all procedures, assure the patient is comfortable prior to starting. While local anesthetic should be adequate for pain control, some patient may require additional analgesia or anxiolysis. The procedure should be performed with the patient lying supine or seated in bed with the knee either fully extended or slightly flexed at 10-20 degrees.
- Assess the patient’s landmarks in order to determine which approach is best for the patient’s anatomy and effusion. As previously discussed, there is no one “best” approach, and so each scenario will be case and provider dependent. Once a site and approach has been chosen, a marking pen or gentle indentation may be made at the intended procedure point of entry.
- Preparation
- Set up a sterile area on a table or mayo stand where your supplies, cleansing materials, and sterile gloves are set aside. Do not forget a sterile container for fluid collection that can be sent to the lab for analysis. If there are no designated containers available, a sterile urine specimen cup may be used.
- Using chlorhexidine or betadine, sterilize the entire knee in the event that a different approach becomes necessary.
- Apply a sterile drape over the knee so that the chosen site of entry may be clearly visualized. It may be preferable to have a large enough drape within the field in case more than 1 attempt must be made at an alternative site.
- Procedure
- Using a small gauge needle with 1% or 2% lidocaine with epinephrine, make a superficial wheel of anesthetic at the entry site followed by insertion of the needle into the deep tissues. Be sure to draw back before introducing anesthetic.
- Using an 18-20g needle, insert the needle through the region of tissue has been anesthetized. Regardless of the approach being taken, the directionality of the needle should be posterior to the patella while horizontal to the joint space. Proceed into the joint space and maintain negative pressure on the syringe while advancing until fluid is readily returning into the syringe. For a smaller diagnostic arthrocentesis, a 10cc syringe may be utilized for aspiration, but in the setting of a large effusion, particularly if there is intention of therapeutic fluid removal, a 30-50cc syringe may be preferable. If large syringes are unavailable, multiple smaller syringes can be used with the needle left in place in the joint space or the same syringe can be repeatedly emptied into a sterile container and reattached for further aspiration.
- In order to facilitate aspiration once fluid has been obtained, the joint may be compressed or “milked”. A recent study assessed the utility of constant compression of the knee during knee arthrocentesis which showed increased aspiration volume yield. However, the is an isolated study directed at optimizing fluid aspiration volume, not necessarily accuracy of successful performance of a diagnostic arthrocentesis.16
- If fluid is unable to be aspirated, withdraw the needle to the point of entry and redirect. If fluid is still unable to be withdrawn, aspiration at a different procedure site may be considered.
- Once adequate fluid has been collected for analysis or symptomatic improvement in the setting of a therapeutic aspiration, remove the needle and apply a bandage.
- The joint should be reassessed for post-procedural bleeding or hemarthrosis formation.
- Synovial fluid laboratory analysis
- Cell count
- Gram stain
- Lactate Dehydrogenase
- Protein
- Glucose
- Culture
- Post-Procedural Complications and Care
- Post-procedural bleeding or hemarthrosis formation a complication that should be observed for after a procedure, particularly for patients who are coagulopathic. However, as previously discussed, there is no literature to show significant post-procedural bleeding is increased in the setting of coagulopathy. Hemarthrosis formation generally occurs if a blood vessel is damaged during the procedure. This is an uncommon complication and often self-limited as shown by a study which found that even in patients on therapeutic anticoagulation with warfarin, the risk of bleeding was 0.2% with no statistical difference from those not anticoagulated.8 If this complication does arise in someone who is coagulopathic, continued observation should be pursued, as blood products may be warranted. This should be done in conjunction with consultation of orthopedics and hematology.
- If the synovial fluid aspirated shows obvious pus, IV antibiotics should be promptly administered and orthopedics consulted for admission for further antibiotics and possible wash out of the joint space.
- While there is no strong literature to support this, if there is any concern that the procedure was performed through overlying cellulitis, prophylactic antibiotics may be considered.
Case Queries
There is no definitive data demonstrating which landmark-based approach to a knee arthrocentesis is most likely to yield a successful aspiration. The approach taken should be a combination of physical exam assessment as to which location appears to contain the most dependent fluid and which approach the provider feels most comfortable performing. In terms of differentiating when a joint requires a diagnostic fluid aspiration, there is also no evidence-based answer. If there is any concern for joint space infection, an arthrocentesis should be performed. While this is most commonly in the setting of isolated joint involvement, many patients have baseline polyarticular joint inflammation which does not preclude one isolated joint from becoming infected. In addition, patients with a history of diabetes and vascular disease are also at risk of septic arthritis. When in doubt, tap the joint, and make sure there is no infection.
Pearls and Pitfalls
- The optimal approach to a knee arthrocentesis is multifactorial – dependent upon patient anatomy, etiology of the effusion, extremity positioning, and provider preference. All of these aspects should be taken into account before the procedure is attempted.
- Patient comfort and flexion of the knee during the procedure may be facilitated by placing a pillow or towel roll under the extremity. As always, patient comfort and positioning are pivotal in procedural success.
- Continuous compression of the knee during the procedure may allow for localized dependence of the fluid and assist in successful aspiration.
- Once the joint space has been entered, intermittent compression or “milking” may assist in increased fluid aspiration.
- In the setting of an unsuccessful or “dry tap”, initially attempt redirecting of the needle, but if still unsuccessful, attempt a different approach.
Rapid Procedure Review- Knee Arthrocentesis
- Position patient supine with the bed with the knee fully extended or slightly flexed.
- Assess anatomical landmarks, locate a fluid pocket using either physical exam or ultrasound, and mark the procedure site.
- After initial assessment, decide which approach will likely yield a successful aspiration.
- Anesthetize the skin and down to the joint space.
- Using a 10-30cc syringe attached to an 18-20g catheter, insert the needle through the anesthetized tract into the joint space while applying negative pressure on the syringe.
- Collect synovial fluid specimen.
- Once adequate specimen has been obtained remove the needle, apply pressure and bandage the procedure site.
References/Further Reading
- Walls, Ron M., et al. Rosen’s Emergency Medicine: Concepts and Clinical Practice. Elsevier, 2018.
- Freemont, AJ, et al. “Diagnostic Value of Synovial Fluid Microscopy: a Reassessment and Rationalisation.” Annals of the Rheumatic Diseases, vol. 50, no. 2, 1991, pp. 101–107., doi:10.1136/ard.50.2.101.
- Freemont, AJ. “Microscopic Analysis of Synovial Fluid–the Perfect Diagnostic Test?” Annals of the Rheumatic Diseases, vol. 55, no. 10, 1996, pp. 695–697., doi:10.1136/ard.55.10.695
- Fine, Marcello De, et al. “The Role of Synovial Fluid Analysis in the Detection of Periprosthetic Hip and Knee Infections: a Systematic Review and Meta-Analysis.” International Orthopaedics, vol. 42, no. 5, 2018, pp. 983–994., doi:10.1007/s00264-018-3865-3.
- Dooley, David P. “Aspiration of the Possibly Septic Joint through Potential Cellulitis: Just Do It!” The Journal of Emergency Medicine, vol. 23, no. 2, 2002, p. 210., doi:10.1016/s0736-4679(02)00496-1.
- Bashir, Ma, et al. “Determination of a Safe INR for Joint Injections in Patients Taking Warfarin.” The Annals of The Royal College of Surgeons of England, vol. 97, no. 8, 2015, pp. 589–591., doi:10.1308/rcsann.2015.0044.
- Yui, Jennifer C., et al. “Arthrocentesis and Joint Injection in Patients Receiving Direct Oral Anticoagulants.” Mayo Clinic Proceedings, vol. 92, no. 8, 2017, pp. 1223–1226., doi:10.1016/j.mayocp.2017.04.007.
- Reno, Elaine. “Safety of Arthrocentesis and Joint Injection in Patients Receiving Anticoagulation at Therapeutic Levels.” The Journal of Emergency Medicine, vol. 43, no. 5, 2012, doi:10.1016/j.jemermed.2012.09.005.
- Fine, Marcello De, et al. “The Role of Synovial Fluid Analysis in the Detection of Periprosthetic Hip and Knee Infections: a Systematic Review and Meta-Analysis.” International Orthopaedics, vol. 42, no. 5, 2018, pp. 983–994., doi:10.1007/s00264-018-3865-3.
- Wiler, Jennifer L., et al. “Comparison of Ultrasound-Guided and Standard Landmark Techniques for Knee Arthrocentesis.” The Journal of Emergency Medicine, vol. 39, no. 1, 2010, pp. 76–82., doi:10.1016/j.jemermed.2008.05.012.
- Yaqub, Sabeen, et al. “Can Diagnostic and Therapeutic Arthrocentesis Be Successfully Performed in the Flexed Knee?” JCR: Journal of Clinical Rheumatology, vol. 24, no. 6, 2018, pp. 295–301., doi:10.1097/rhu.0000000000000707.
- Douglas, Robert J. “Aspiration and Injection of the Knee Joint: Approach Portal.” Knee Surgery & Related Research, vol. 26, no. 1, 2014, pp. 1–6., doi:10.5792/ksrr.2014.26.1.1.
- Ike, Robert W., et al. “Ultrasound of the Knee during Voluntary Quadriceps Contraction: A Technique for Detecting Otherwise Occult Effusions.” Arthritis Care & Research, vol. 62, no. 5, 2010, pp. 725–729., doi:10.1002/acr.20047.
- Koutsianas, Christos, and Rainer Klocke. “265. Efficacy Of Ultrasound-Guided Versus Landmark-Guided Injections In Rheumatology: A Systematic Review.” Rheumatology, vol. 56, no. suppl_2, 2017, doi:10.1093/rheumatology/kex062.267.
- Sibbitt, Wl, et al. “Does Ultrasound Guidance Improve the Outcomes of Arthrocentesis and Corticosteroid Injection of the Knee?” Scandinavian Journal of Rheumatology, vol. 41, no. 1, 2011, pp. 66–72., doi:10.3109/03009742.2011.599071.
- Bhavsar, Tej B., et al. “Improvement in Diagnostic and Therapeutic Arthrocentesis via Constant Compression.” Clinical Rheumatology, vol. 37, no. 8, 2017, pp. 2251–2259., doi:10.1007/s10067-017-3836-x.







