Authors: Brit Long, MD (@long_brit, EM Physician at SAUSHEC, USAF) and Alex Koyfman, MD (@EMHighAK, EM Attending Physician, UTSW / Parkland Memorial Hospital) // Edited by: Jennifer Robertson, MD, MSEd
A 28 year-old female presents to the emergency department (ED) complaining of a left-sided headache with associated nausea and vomiting for the last 24 hours. She went to another ED a few hours prior, where the headache resolved with medications. However, it quickly returned. The patient has no past medical history, including no history of headaches. She is one month postpartum. Her vital signs are normal, including a blood pressure (BP) of 110/62. Her neurologic exam is normal. You order an intravenous (IV) line and basic medications for headache treatment. However, you question whether you are missing something important. Besides treating the headache, are any tests necessary?
Emergency physicians evaluate many conditions that are often simple, however, we also train to recognize conditions that can be life-threatening. A patient with neurologic symptoms may have a condition that is benign, while another may be suffering a condition with high morbidity and mortality. Emergency physicians must evaluate for red flags in patients that may signify high risk disorders. Cerebral venous thrombosis (CVT) is one such disorder as it carries significant morbidity and mortality.
CVT is a rare disorder, with an annual incidence of 1.32 cases per 100,000 person-years. It accounts for approximately 1% of strokes.1-4 The disease includes thrombosis of the cerebral veins and major dural sinuses. CVT is more common in patients with history of thrombophilia, those taking oral contraceptives, and those who are pregnant or in a post-partum state.1-5 The diagnosis is often delayed and most patients are not diagnosed until 4-7 days after symptoms start6-8 Only 10% of patients are over 60 years of age. The majority of patients present under the age of 50 years (80%), with a mean age of 39 years.1-3,6
Presentation
CVT can be a difficult diagnosis to make due to a wide variety of signs and symptoms. CVT should be suspected in several situations, as shown below in Table 1. The onset may be acute, subacute, or chronic.1-3 This accounts for a high rate of misdiagnosis. ED physicians should keep in mind the risk factors for CVT and specific scenarios.
Scenarios warranting CVT investigation1-4
– Headache: in a pregnant female patient, in a young female on OCPs, or one that is atypical and persistent
– Stroke with no typical risk factors or in the setting of seizure
– Intracranial hypertension with no explanation
– Multiple hemorrhagic infarcts, or hemorrhagic infarcts not in a specific arterial distribution
– Objective neurologic symptoms in a patient with risk factors for CVT
Symptoms are not always classic, but they can be associated with the thrombus location.3,4
– Cortical vein thrombosis presents with motor and sensory deficits, as well as seizure.
– Sagittal sinus thrombosis may present with motor deficits, bilateral deficits, and seizures.
– Patients with thrombus in the lateral sinus may present with intracranial hypertension and headache alone.
– Thrombosis of the left transverse sinus can present as aphasia.
– Thrombosis of the deep venous sinus can cause behavioral symptoms due to lesions in the thalamus.
– Cavernous sinus thrombosis is associated with ocular pain, chemosis, proptosis, and oculomotor palsies.3,4
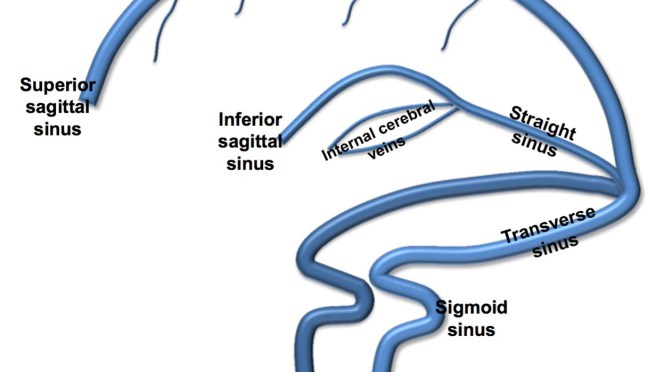
Figure 1 – Cerebral venous system components2, image from Thorell SE, Parry-Jones AR, Punter M, Hurford R, Thachil J. Cerebral venous thrombosis – A primer for the haematologist. Blood Reviews 2015;29:45–50.
Four major syndromes have been described: isolated intracranial hypertension (the most common), focal neurologic abnormality, seizure, and encephalopathy. The patient may present with one or several of these.2-4
- The most common syndrome is intracranial hypertension resulting in headache. This is often a localized, persistent headache, seen in up to 90% of patients with acute presentation. This means that 10% of patients will not have a headache during their course, which can delay diagnosis.7-9 Headache may be sudden in onset and severe, mimicking subarachnoid hemorrhage, or it may be persistent and gradually worsening. Visual symptoms may also occur with the headache. It often worsens with valsalva or coughing due to increased ICP.9,10
- Focal neurologic deficits are found in 37%-44% of patients, with motor weakness the most common focal symptom.7,9 Sensory deficits are not common.1,2
- Seizures (focal, generalized, and status epilepticus) are seen in 30-40% of patients.7,11 CVT should be considered in any patient with a focal neurologic deficit and seizure.1,2
- Encephalitis is the final syndrome, which can be found in patients with thrombosis of the straight sinus or with severe cases including extensive hemorrhage, edema, and large venous infarcts leading to herniation.1,2,4 This syndrome is more common in elderly patients, who may present with altered mental status and confusion.12
Is there a difference between cerebral venous thrombosis and cavernous venous sinus thrombosis?
CVT and CVST have common underlying etiologies including thrombosis. However, CVST includes thrombosis in the cavernous sinuses with infection. Ocular signs and symptoms predominate. Treatment requires anticoagulation and antibiotics.1,2,4,6
Risk factors
At least one risk factor is present in 85% of patients with CVT, however the disease is often multifactorial with several risk factors present.3,4,7 In fact, multiple risk factors are found in 50% of patients with CVT:1,15
– Thrombophilia is discovered or is present in 34% of patients with CVT. These disorders include factor V Leiden mutation and deficiencies of antithrombin, protein C, and/or protein S.
– CVT is commonly seen in women who are pregnant. post-partum or who are taking hormonal contraceptives
– Infections including osteitis, mastoiditis, sinusitis, and meningitis are associated with CVT
– Chronic inflammatory diseases such vasculitis, inflammatory bowel disease, malignancy, nephrotic syndrome, and hematologic disorders such as polycythemia and essential thrombocytosis also contribute to disease development.
– Other risk factors include head trauma, local injury to the cerebral sinuses, and neurosurgical procedures.1,2,4
Pathophysiology
Two major pathophysiological mechanisms are associated with CVT: (1) Thrombosis of the cerebral drainage system and (2) Decreased cerebrospinal fluid absorption. Both can lead to increased intracranial pressure, cerebral edema, and potentially hemorrhage.3,4
- Thrombosis of the cerebral drainage system causes increased venular and capillary pressure. As the local venous pressure rises, cerebral perfusion decreases, and this can cause ischemia and cytotoxic edema. Vasogenic edema can also be a result of blood-brain barrier destruction. This can lead to parenchymal hemorrhage if pressures continue to increase.13,14
- The second mechanism includes decreased CSF absorption, leading to increased pressures, cytotoxic and vasogenic edema, and parenchymal hemorrhage.13,14
Your patient denies any known blood disorders and has had no recent infections or trauma. She does have several risk factors for CVT including her age, post-partum status, and a persistent headache. As she has never had headaches before, you consider further testing.
Diagnosis
Due to the wide variety of symptoms, delays in diagnosis are common. CVT must be considered in patients under 50 years of age with headaches and atypical features. Atypical features may include focal, objective neurologic deficit(s) (often not fitting a specific anatomical region or with multiple region involvement), seizures, signs of intracranial hypertension, or hemorrhagic infarction present on initial head CT.1-4 Patients may improve with pain medication; however, if focal deficit or seizure is present, CVT must be considered.
Labs including a complete blood count (CBC), renal function, and coagulation panel should be obtained. The d-dimer is classically thought to be elevated.4,9,16,17 However, one study found a false negative rate of 24%. In addition, d dimer has been found to be normal in 40% of patients with isolated headache and no other symptoms.9 Therefore, a negative d dimer must not be relied upon to rule out CVT.16,17
A lumbar puncture (LP) should be considered to evaluate for meningitis. Results of the LP are often nonspecific in CVT including increased protein, increased RBCs, and lymphocytosis, findings similar to viral meningitis. The presence of CVT risk factors, objective neurologic deficits, and deficits in multiple arterial distributions should raise suspicion for the disease. Viral studies including polymerase chain reaction (PCR) should be ordered if LP is completed.1,2,4,9 However, CVT is still suspected after a negative or nonspecific LP, further evaluation with
Imaging is required for diagnosis. The American Heart Association/American Stroke Associations (AHA/ASA) recommend imaging of the cerebral venous system for patients with infarction across multiple arterial territories or with lobar intracerebral hemorrhage of unclear origin.4,6 Imaging should also be obtained in patients with idiopathic intracranial hypertension and headache with atypical features.4,6
- Head computed tomography (CT) is a first line test in patients with new headache, focal neurologic symptom, seizure, or altered mental status. Any patient with headache and new abnormal neurologic finding(s) (altered mental status, focal neurologic deficit, etc.) warrants emergent head CT per ACEP policy (Level B recommendation).18
- Unfortunately, this test has poor sensitivity for CVT and is normal in 30% of cases. The majority of findings on CT are nonspecific, if present.
- One third of cases demonstrate direct signs on CT. These signs include a dense triangle sign (hyperdensity with triangular shape in posterior superior sagittal sinus), an empty delta sign (triangular pattern of contrast enhancement surrounding a central area with no enhancement), or a cord sign (curvilinear density over the cerebral cortex).3,4,6,19-21
- Indirect signs of CVT are more common and include contrast enhancement over the falx and tentorium, dilated venous structures, small ventricles, and parenchymal abnormalities (seen in 80% including hemorrhagic and nonhemorrhagic lesions).19-21
- Multiple infarctions or infarctions in several arterial distributions warrant consideration of the disease.1-3
- CT combined with venography is rapid and reliable and will detect a thrombus with heterogeneous density.
- This test has an overall sensitivity of 95% and is helpful for patients with subacute or chronic presentations.1-4,6,22
- Contrast reaction, contrast nephropathy, and radiation exposure can limit its use. Due to availability of CT, this is likely the best test in the ED setting.
- Magnetic resonance (MR) imaging with T2 weighted sequence and MR venography (MRV) are the most sensitive imaging modalities. However, disadvantages include the time involved and the anatomical variation of the venous system that may be present.1,3,6,22-28
- MRI findings are dependent on the thrombus age. If the diagnosis is based on lack of blood flow only, the test may be false positive.3,4,22,29 Contrast is needed with venography.1,4,6
- This test is often unavailable in the ED, thus CT with venography is the usual go-to imaging modality.
- Cerebral intra-arterial angiography may be used if CT and MR imaging modalities do not reveal the diagnosis and the diagnosis is still under consideration,.3,6,30,31 This test is best for cortical vein thrombosis.3,4,6
A noncontrast head CT reveals hyperdensities of the left sigmoid sinus. You speak with the radiologist concerning the need for further imaging, and MRV demonstrates thrombosis of the left transverse and sigmoid sinuses. Now that you have the diagnosis, what are your next step
Management
Mortality occurs in approximately 5% of patients, most commonly with lesions leading to increased intracranial pressure (ICP) and herniation.1-3,15 First address life-threatening complications including coma, seizures, or increased ICP. This is followed by specific therapy, supportive care, and treatment of underlying causes and complications.1-4,6 Table 2 outlines treatment goals.
Table 2 – Management Goals1-4,6
– Stabilize the immediate condition
– Remove the venous occlusion and stop propagation
– Administration of thrombolytic agents in selected patients
– Use of antiepileptic agents in patients with seizures and supratentorial lesions
– Treat any underlying conditions and risk factors
– Treat long term symptoms such as headache
– Manage complications
For patients with signs of increased ICP (posturing, change in breathing, bradycardia/hypertension, decreased mental status), immediate action is needed to reduce ICP. Elevation of the head of the bed, mannitol or hypertonic saline, admission to intensive care unit, and ICP monitoring may be required.3,4,6,32 If these are ineffective, consult neurosurgery for decompressive hemicraniectomy.1,2,32-34
The patient does not show any signs of decompensation, though her pain is unchanged after the first several medications. You consider further, specific treatments for CVT.
After stabilization, the next step is consulting the neurology and hematology teams, along with admission to a stroke unit for monitoring. Specific therapy includes anticoagulation with heparin initially, followed by transition to warfarin.1-3,6,35 Over 50% of patients will experience hemorrhagic transformation, but this is not a contraindication to anticoagulation.2-4,36 The duration of treatment is 3-6 months if the CVT is provoked and 6-12 months if it is unprovoked.3,6 Thrombolysis, either systemic or catheter-directed, can be considered if anticoagulation fails.1,2,34,37,38
Supportive care includes addressing risk factors including cessation of oral contraceptive use, treating infection if present, and seizure prophylaxis. If the patient seizes with an associated supratentorial lesion such as edema, hemorrhage, or infarction on imaging, then specific seizure treatment and prophylaxis are required. If a seizure does not occur, seizure prophylaxis is not necessary.1,2,11,39 Further testing for underlying etiology is recommended, including thrombophilia.1,2,3,6 Follow up imaging at 3-6 months is required to assess for recanalization of the affected area.1-4,6
The patient undergoes testing for thrombophilia, which reveals factor V Leiden mutation. She is discharged on warfarin.
Prognosis
Mortality can reach up to 5.6% during an acute CVT, commonly due to herniation.1-3,6 Approximately 88% of patients experience complete recovery or experience only mild deficits.1-4,40 Headaches continue in up to half of patients.1,2,10,40 Recurrence is rare and occurs in only 3% of patients.40,41 Two thirds of patients achieve recanalization of the vasculature with treatment.3,6,42,43 Markers for poor long-term prognosis include malignancy or infection as the instigating event, associated intracranial hemorrhage, altered mental status on admission (particularly GCS < 9), male gender, age greater than 37 years, and deep venous system involvement.1-3,7,44
The patient undergoes repeat imaging at her six month visit, which reveals complete recanalization of the affected sinus. Her headaches are gone, and her warfarin is discontinued.
Summary
– CVT is a rare and difficult diagnosis to make due to a wide variety of signs and symptoms.
– Patients are commonly under 50 years of age.
– Scenarios warranting CVT investigation include headache that is atypical and persistent, stroke with no typical risk factors or in the setting of seizure, intracranial hypertension with no explanation, multiple hemorrhagic infarcts, hemorrhagic infarcts not in a specific arterial distribution, or objective neurologic symptoms in a patient with risk factors for CVT.
– Patients can present with four major syndromes, the most common of which is headache from intracranial hypertension.
– Do not rely on labs such as D-dimer for ruling out or ruling in. Imaging is required, including CT with venography or MRI/MRV.
– Treatment includes stabilizing immediate condition, anticoagulation, and managing underlying condition.
References/Further Reading:
- Piazza G. Cerebral venous thrombosis. Circulation 2012;125:1704-1709.
- Thorell SE, Parry-Jones AR, Punter M, Hurford R, Thachil J. Cerebral venous thrombosis – A primer for the haematologist. Blood Reviews 2015;29:45–50.
- Bousser MG, Ferro JM. Cerebral venous thrombosis: an update. Lancet Neurol 2007; 6:162-70.
- Stam J. Thrombosis of the cerebral veins and sinuses. N Engl J Med 2005;352:1791–8.
- Coutinho JM, Ferro JM, Canhao P, Barinagarrementeria F, Cantu C, Bousser MG, Stam J. Cerebral venous and sinus thrombosis in women. Stroke 2009;40:2356 –2361.
- Saposnik G, Barinagarrementeria F, Brown Jr RD, Bushnell CD, Cucchiara B, Cushman M, et al. Diagnosis and management of cerebral venous thrombosis: a statement for healthcare professionals from the American Heart Association/American Stroke Association. Stroke 2011;42:1158–92.
- Ferro JM, Canhao P, Stam J, Bousser MG, Barinagarrementeria F, Investigators I. Prognosis of cerebral vein and dural sinus thrombosis: results of the International Study on Cerebral Vein and Dural Sinus Thrombosis (ISCVT). Stroke 2004;35:664–70.
- Ferro JM, Canhao P, Stam J, Bousser MG, Barinagarrementeria F, Massaro A, et al. Delay in the diagnosis of cerebral vein and dural sinus thrombosis: influence on outcome. Stroke 2009;40:3133–8.
- Tanislav C, Siekmann R, Sieweke N, Allendorfer J, Pabst W, Kaps M, Stolz E. Cerebral vein thrombosis: clinical manifestation and diagnosis. BMC Neurol 2011;11:69.
- Agostoni E. Headache in cerebral venous thrombosis. Neurol Sci 2004;25(Suppl 3):S206 –S210.
- Ferro JM, Canhao P, Bousser MG, Stam J, Barinagarrementeria F. Early seizures in cerebral vein and dural sinus thrombosis: risk factors and role of antiepileptics. Stroke 2008;39:1152–1158.
- Ferro JM, Canhao P, Bousser MG, Stam J, Barinagarrementeria F. Cerebral vein and dural sinus thrombosis in elderly patients. Stroke 2005;36:1927–1932.
- Schaller B, Graf R. Cerebral venous infarction: the pathophysiological concept. Cerebrovasc Dis 2004;18:179.
- Gotoh M, Ohmoto T, Kuyama H. Experimental study of venous circulatory disturbance by dural sinus occlusion. Acta Neurochir (Wien) 1993;124:120.
- Canhao P, Ferro JM, Lindgren AG, Bousser MG, Stam J, Barinagarrementeria F, et al. Causes and predictors of death in cerebral venous thrombosis. Stroke 2005;36:1720–5.
- Crassard I, Soria C, Tzourio C, Woimant F, Drouet L, Ducros A, Bousser MG. A negative D-dimer assay does not rule out cerebral venous thrombosis: a series of seventy-three patients. Stroke 2005;36:1716 –1719.
- Kosinski CM, Mull M, Schwarz M, Koch B, Biniek R, Schlafer J, Milkereit E, Willmes K, Schiefer J. Do normal D-dimer levels reliably exclude cerebral sinus thrombosis? Stroke 2004;35:2820–2825.
- Edlow JA, Panagos PD, Godwin SA, Thomas TL, Decker WW. Clinical Policy: Critical Issues in the Evaluation and Management of Adult Patients Presenting to the Emergency Department With Acute Headache. Ann Emerg Med 2008 Oct;52(4):407-430.
- Virapongse C, Cazenave C, Quisling R, et al. The empty delta sign: frequency and significance in 76 cases of dural sinus thrombosis. Radiology 1987;162:779.
- Lee EJ. The empty delta sign. Radiology 2002;224:788.
- Boukobza M, Crassard I, Bousser MG. When the “dense triangle” in dural sinus thrombosis is round. Neurology 2007; 69:808.
- Khandelwal N, Agarwal A, Kochhar R, Bapuraj JR, Singh P, Prabhakar S, Suri S. Comparison of CT venography with MR venography in cerebral sinovenous thrombosis. AJR Am J Roentgenol 2006;187:1637–1643.
- Chu K, Kang DW, Yoon BW, Roh JK. Diffusion-weighted magnetic resonance in cerebral venous thrombosis. Arch Neurol 2001;58:1569–76.
- Dormont D, Anxionnat R, Evrard S, Louaille C, Chiras J, Marsault C. MRI in cerebral venous thrombosis. J Neuroradiol 1994;21:81–99.
- Lafitte F, Boukobza M, Guichard JP, Hoeffel C, Reizine D, Ille O, et al. MRI and MRA for diagnosis and follow-up of cerebral venous thrombosis (CVT). Clin Radiol 1997;52:672–9.
- Selim M, Fink J, Linfante I, Kumar S, Schlaug G, Caplan LR. Diagnosis of cerebral venous thrombosis with echo-planar T2-weighted magnetic resonance imaging. Arch Neurol 2002;59:1021–6.
- Leach JL, Fortuna RB, Jones BV, Gaskill-Shipley MF. Imaging of cerebral venous thrombosis: current techniques, spectrum of findings, and diagnostic pitfalls. Radiographics 2006;26(Suppl. 1):S19–41 [discussion S42-13].
- Meckel S, Reisinger C, Bremerich J, Damm D, Wolbers M, Engelter S, et al. Cerebral venous thrombosis: diagnostic accuracy of combined, dynamic and static, contrast-enhanced 4D MR venography. AJNR Am J Neuroradiol 2010;31:527–35.
- Linn J, Ertl-Wagner B, Seelos KC, Strupp M, Reiser M, Bruckmann H, Bruning R. Diagnostic value of multidetector-row CT angiography in the evaluation of thrombosis of the cerebral venous sinuses. AJNR Am J Neuroradiol. 2007;28:946 –952.
- Ayanzen RH, Bird CR, Keller PJ, McCully FJ, Theobald MR, Heiserman JE. Cerebral MR venography: normal anatomy and potential diagnostic pitfalls. AJNR Am J Neuroradiol 2000;21:74–8.
- Zouaoui A, Hidden G. Cerebral venous sinuses: anatomical variants or thrombosis? Acta Anat 1988;133:318–24.
- Bullock, R, Clifton G. Guidelines for the Management of Severe Brain Injury, Brain trauma foundation/American Association of Neurologic Surgeons, New York 1995.
- Stefini R, Latronico N, Cornali C, Rasulo F, Bollati A. Emergent decompressive craniectomy in patients with fixed dilated pupils due to cerebral venous and dural sinus thrombosis: report of three cases. Neurosurgery 1999;45(3):626–9.
- Ferro JM, Crassard I, Coutinho JM, Canhao P, Barinagarrementeria F, Cucchiara B, Derex L, Lichy C, Masjuan J, Massaro A, Matamala G, Poli S, Saadatnia M, Stolz E, Viana-Baptista M, Stam J, Bousser MG. Decompressive surgery in cerebrovenous thrombosis: a multicenter registry and a systematic review of individual patient data. Stroke. 2011;42:2825–2831.
- Stam J, De Bruijn SF, DeVeber G. Anticoagulation for cerebral sinus thrombosis. Cochrane Database Syst Rev. 2002: CD002005.
- Tait C, Baglin T, Watson H, Laffan M, Makris M, Perry D, et al. Guidelines on the investigation and management of venous thrombosis at unusual sites. Br J Haematol 2012;159:28–38.
- Canhao P, Falcao F, Ferro JM. Thrombolytics for cerebral sinus thrombosis: a systematic review. Cerebrovasc Dis 2003;15:159 –166.
- Dentali F, Squizzato A, Gianni M, De Lodovici ML, Venco A, Paciaroni M, Crowther M, Ageno W. Safety of thrombolysis in cerebral venous thrombosis: a systematic review of the literature. Thromb Haemost 2010;104:1055–1062.
- Masuhr F, Busch M, Amberger N, Ortwein H, Weih M, Neumann K, et al. Risk and predictors of early epileptic seizures in acute cerebral venous and sinus thrombosis. Eur J Neurol 2006;13:852–6.
- Dentali F, Gianni M, Crowther MA, Ageno W. Natural history of cerebral vein thrombosis: a systematic review. Blood 2006;108:1129 –1134.
- Martinelli I, Bucciarelli P, et al. Long-term evaluation of the risk of recurrence after cerebral ainu-venous thrombosis. Circulation 2010;121:2740.
- Baumgartner RW, et al. Recanalisation of cerebral venous thrombosis. J Neurol Neurosurg Psychiatry 2003;74:459.
- Arauz A, et al. Time to recanalisation in patients with cerebral venous thrombosis under anticoagulation therapy. J Neurol Neursurg Psychiatry 2016;87:247.
- Ferro J, et al. External validation of a prognostic model of cerebral vein and dural sinus thrombosis. Cerebrovasc Dis 2005;19(Suppl 2):154.







5 thoughts on “Cerebral Venous Thrombosis: Pearls and Pitfalls”
This is a very helpful article. I appreciate the doctors for sharing this article.
Pingback: Headache – EM Board Rounds Blog
Anyone incorporating d-dimer into their eval for CVT? I had neuro tell me I could use it for young people who may be at risk to help avoid the radiation from CTs but they couldn’t really provide me any clear evidence on this.
Pingback: emDOCs.net – Emergency Medicine EducationEM@3AM - Cerebral Venous Sinus Thrombosis - emDOCs.net - Emergency Medicine Education
Pingback: emDOCs.net – Emergency Medicine EducationSinusitis Mimics: ED-relevant pearls and pitfalls - emDOCs.net - Emergency Medicine Education