Author: Chuck Pilcher, MD, FACEP (Editor, Med Mal Insights) // Edited by: Alex Koyfman, MD (@EMHighAK, EM Attending Physician, UTSW / Parkland Memorial Hospital) and Brit Long, MD (@long_brit)
Welcome to this month’s case from Medical Malpractice Insights – Learning from Lawsuits, a monthly email newsletter for ED physicians. The goal of MMI-LFL is to improve patient safety, educate physicians, and reduce the cost and stress of medical malpractice lawsuits. To opt in to the free subscriber list, click here.
– Chuck Pilcher MD FACEP, Editor, Med Mal Insights
Anchoring bias, limited differential leads to quadriplegia
Spinal epidural abscess (SEA) too often overlooked
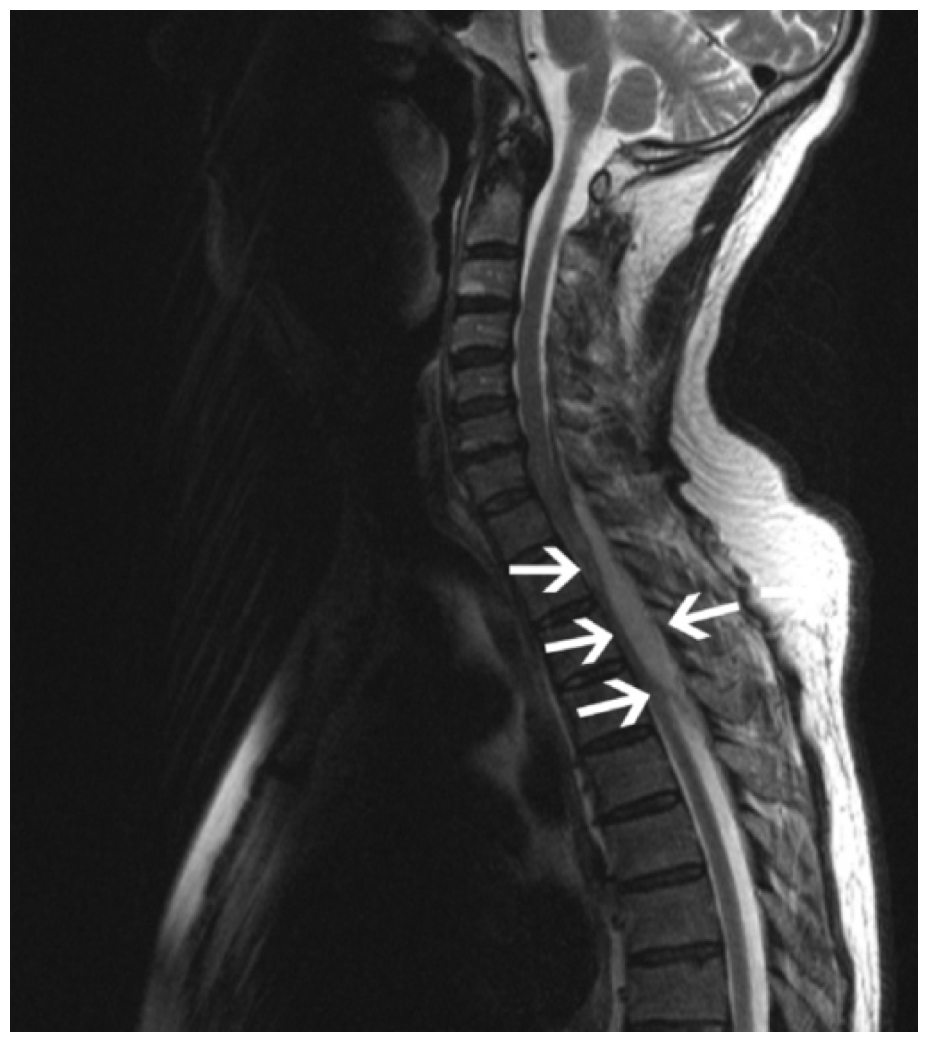 Facts: A 44-year-old male with recent interferon treatment for Hepatitis C and a prior history of neck surgery with hardware sees his PCP for new onset headache, photophobia, and URI symptoms. Hi neck is tender, and lab results reveal only abnormal liver enzymes. He is discharged with OTC analgesics. Three days later he is seen in the ED with slightly worse symptoms and again discharged. He returns to his PCP 4 days later, with worsening HA, N/V, and photophobia and is given oxycodone. When next seen (4th encounter for same problem) in the hospital’s Urgent Care Clinic, he has a temperature of 101.4, hallucinations, and neck stiffness. He is sent to the ED by ambulance. An LP shows “cloudy” CSF, 692 WBC (80% ploys), low glucose, and high protein but no organisms. He is diagnosed with viral meningitis and sent home with anti-emetics, MS-Contin, and pending blood cultures. The next morning two blood cultures show staph; the CSF culture is negative. He is called to return to the hospital and admitted with a diagnosis of Staph aureus meningitis. After 2 days in the hospital, he develops increasing lower body neurologic symptoms including urinary incontinence and retention. A cervical MRI is done and shows a spinal epidural abscess in the area of his surgical hardware. He is left quadriplegic/paretic. A lawsuit is filed.
Facts: A 44-year-old male with recent interferon treatment for Hepatitis C and a prior history of neck surgery with hardware sees his PCP for new onset headache, photophobia, and URI symptoms. Hi neck is tender, and lab results reveal only abnormal liver enzymes. He is discharged with OTC analgesics. Three days later he is seen in the ED with slightly worse symptoms and again discharged. He returns to his PCP 4 days later, with worsening HA, N/V, and photophobia and is given oxycodone. When next seen (4th encounter for same problem) in the hospital’s Urgent Care Clinic, he has a temperature of 101.4, hallucinations, and neck stiffness. He is sent to the ED by ambulance. An LP shows “cloudy” CSF, 692 WBC (80% ploys), low glucose, and high protein but no organisms. He is diagnosed with viral meningitis and sent home with anti-emetics, MS-Contin, and pending blood cultures. The next morning two blood cultures show staph; the CSF culture is negative. He is called to return to the hospital and admitted with a diagnosis of Staph aureus meningitis. After 2 days in the hospital, he develops increasing lower body neurologic symptoms including urinary incontinence and retention. A cervical MRI is done and shows a spinal epidural abscess in the area of his surgical hardware. He is left quadriplegic/paretic. A lawsuit is filed.
Plaintiff: You should have admitted me and treated me with IV antibiotics as soon as you saw the CSF results. They were grossly abnormal and indicated a bacterial infection. I had multiple risk factors for SEA, and you dismissed them. You should have done an MRI and found my abscess before it was too late. Now I’m disabled and can’t work.
Defense: You had symptoms for 2 1/2 weeks. They weren’t the classic triad for SEA. We treated you with antibiotics in the hospital.
Result: Confidential large settlement after 5+ years of litigation.
Takeaways:
- SEA is often missed, with drastic consequences for all concerned.
- The average number of visits before diagnosis ranges from 2-4.
- Staph is the most common cause of SEA and a rare cause of meningitis.
- The CSF was grossly abnormal and inconsistent with viral meningitis, and the disease course was inconsistent with staph meningitis.
- A negative CSF culture with positive blood cultures is rarely bacterial meningitis.
- After 2 weeks of symptoms, a patient with staph meningitis would be dead; a patient with viral meningitis should have recovered.
- Immunocompromised patients with spinal hardware are at high risk for SEA.
- If you’ve considered SEA in the differential and eliminated it, document why.
- In half of litigated cases, the abscess was at a level not imaged in the first MRI.
- If you can’t eliminate the diagnosis, an MRI of the entire spine is the next step.
- Cover patients with antibiotics pending blood culture results.
The “Classic Triad” (fever, pain and neurologic symptoms) occurs in only 10-15% of patients. By then it’s usually too late. The typical features include:
- Gradual onset
- Repeat ED or PCP visits over a short period
- Vague constitutional symptoms
- Fever and mildly elevated WBC
- Early neurological complaints, e.g., tingling, numbness, proprioception issues, etc. to classic cauda equina syndrome
- Elevated ESR and/or CRP; a normal ESR/CRP is a defense that SEA was considered
- Abnormal spinal fluid, which may or may not grow an organism
- Positive blood culture
- A truly worried patient (as opposed to a dramatic drug seeker)
- Risk factors, like recent surgery, spinal hardware, dental work, IV drug use, immunocompromise state, or diabetes
References:
Spinal Epidural Abscess. Huff JS. Medscape eMedicine, 22 Aug 2017.
emDocs – Spinal Epidural Abscess
“Experience enables you to recognize a mistake when you make it again.”
Franklin P. Jones (1908 – 1980), PR Executive and Columnist








