Authors: Melissa Myers, MD; Jonathan Srichandra, MD; Kristin Kann, MD; and Eric Chin, MD (Emergency Medicine, San Antonio, TX) // Edited by: Stephen Alerhand, MD (@SAlerhand Assistant Professor, Rutgers New Jersey Medical School)
Introduction
Point-of-care ultrasound (POCUS) has become increasingly available for providers in tertiary-care hospitals and the far-forward combat environment.1,2 It is widely acknowledged as a useful adjunct in the initial evaluation of the trauma patient in a hospital setting. The Focused Assessment with Sonography in Trauma (FAST) examination is commonly used to assess for hemoperitoneum (blood in the peritoneum) and hemopericardium (blood in the pericardial sac) in the setting of abdominal and thoracic trauma. The 9th edition of the Advanced Trauma Life Support (ATLS) guidelines places emphasis on the use of point-of-care ultrasound during the initial trauma evaluation, and includes a FAST examination directly following the primary survey in the trauma algorithm.3 More recently, ultrasound is noted to be extremely useful in the evaluation for pneumothorax, particularly when added to the FAST examination, then referred to as an Extended FAST (or E-FAST). This article discusses a case in which ultrasound was instrumental in the detection of a pneumothorax which was not visible on a standard chest radiograph. We will review the ultrasonographic technique, advantages and disadvantages of thoracic ultrasound for detection of pneumothorax, and its role in a resource limited environment.
Case
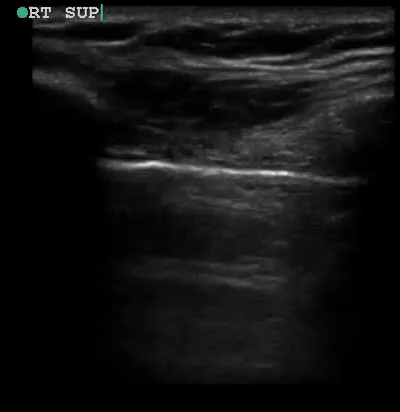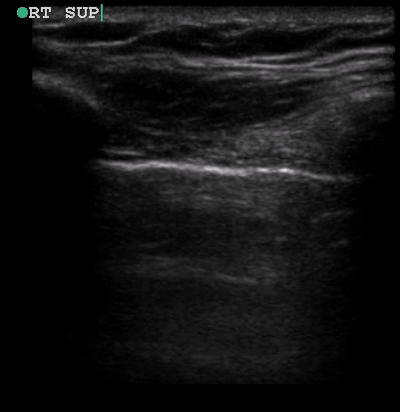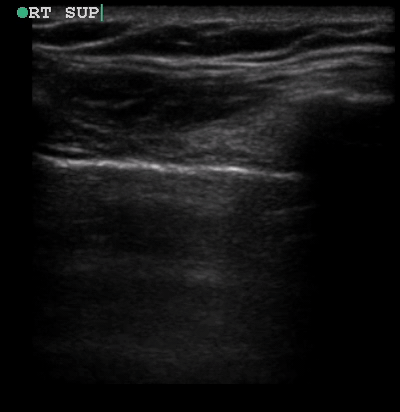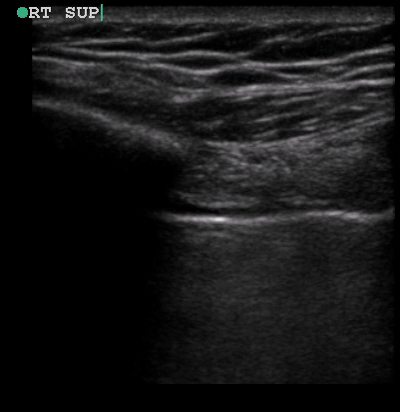
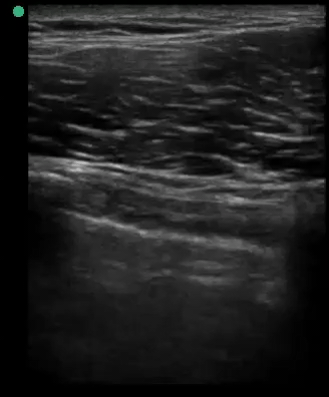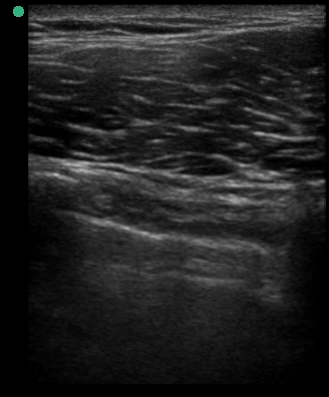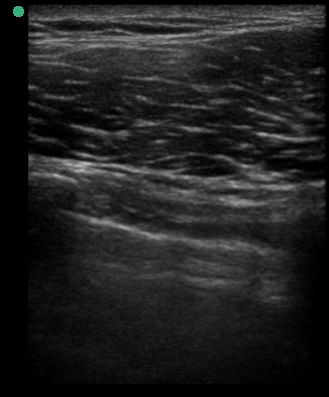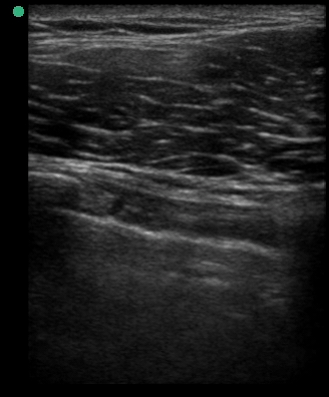
A 34-year-old male with no significant past medical history was brought to the ED by paramedics following a high-speed MVC. The patient was the restrained driver of a vehicle involved in a head-on collision with another vehicle. He was intubated in the field due to respiratory distress using intravenous midazolam, fentanyl and ketamine. On arrival, the patient was in stable condition. His vital signs were heart rate 109, respiratory rate 21, blood pressure 148/72 and oxygen saturation 95% on 100% oxygen through the endotracheal tube. His Glasgow Coma Score was 3T. Placement of the endotracheal tube was confirmed by CO2 wave form capnography and there was no difficulty with ventilation. Pulses were intact bilaterally. The patient had diminished breath sounds on the left and absent breath sounds on the right. The patient also had crepitus on palpation of the right chest wall. While the initial assessment was being performed, a supine chest radiograph was obtained. Another member of the team performed an E-FAST examination while the CXR was being uploaded for review. The E-FAST examination showed normal lung sliding on the left (Video 1), no lung sliding on the right (Video 2), and a demonstrable lung point (Video 3) on the left.
Video 1, Video 2, and Video 3

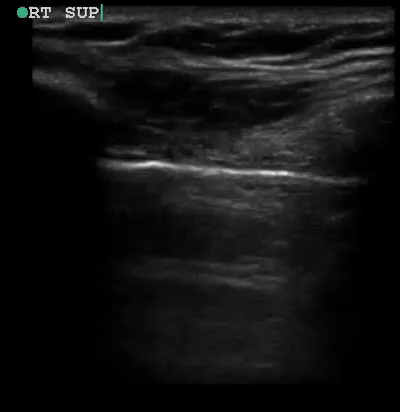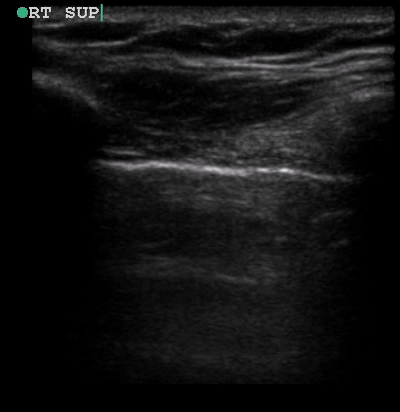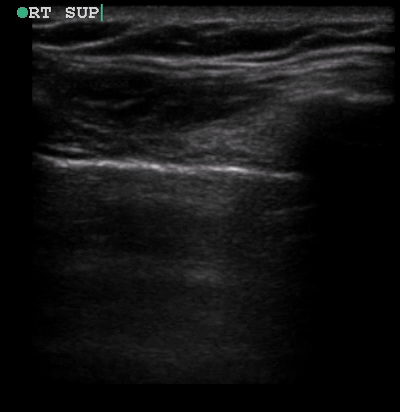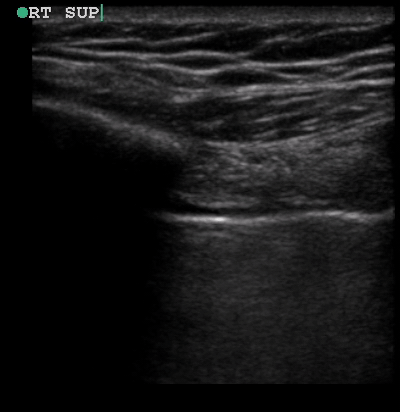
Senior members of the trauma team compared the ultrasound and CXR findings while the rest of the trauma team continued with the resuscitation. While the imaging was being reviewed, the patient began to decompensate and became hypotensive so the trauma team immediately placed bilateral chest tubes. A large rush of air was appreciated on both sides upon placement of the chest tubes with approximately 50 mL of blood return on the right. The blood pressure normalized following placement of the chest tubes. He was given two units of packed red blood cells, two units of fresh frozen plasma before further diagnostic imaging and admission to the ICU. The patient’s hospital course was complicated by severe traumatic brain injury, pericardial effusion, C1 spinal fracture, multiple rib fractures, right hemopneumothorax, left pneumothorax, pneumomediastinum, and a liver laceration. After a prolonged clinical course, the patient recovered fully and was discharged home.
Discussion
Detection of a pneumothorax is critically important in the evaluation and treatment of an unstable trauma patient. The traditional method of listening for breath sounds bilaterally is relatively insensitive for detecting pneumothoraces, and is potentially more difficult during medical evacuations in noisy environments such ambulances or helicopters. In most trauma centers, a supine chest radiograph is commonly used during the initial trauma evaluation. This modality will miss 25-70% of pneumothoraces.4-10 Furthermore, radiographs require equipment and technicians which are not available in austere or resource limited environments. If providers are unsure if a pneumothorax is present, they may feel that it is necessary to perform an empiric needle or tube thoracostomy in a patient with thoracic trauma. This procedure is not benign and may lead to increased morbidity if a pneumothorax was not actually present.
Point-of-care ultrasound offers multiple advantages. It is highly sensitive and will detect 86-98% of pneumothoraces in trauma patients.5-7 It is also highly specific, leading to a high degree of confidence in the diagnosis when found on ultrasound. One study showed a specificity of 99% for detection of pneumothorax in trauma patients.4 A 2012 meta-analysis by Alrajhi and colleagues reported a sensitivity of 90% when medical patients were included in the analysis.7 Ultrasound is excellent at detecting even small pneumothoraces. One study using a porcine model showed that 90% of pneumothoraces as small as 25mL of air were detected using ultrasound.9
Technique
Image acquisition is relatively quick and straightforward. A high-frequency linear is placed in the mid-clavicular line with the probe indicator oriented toward the head. Starting at the second rib space and moving inferiorly down the chest, three intercostal rib spaces are examined for approximately two seconds each. This is repeated on the both sides of the chest. Although the curvilinear or phased-array probe used for the abdominal portion of the FAST examination can be used to evaluate for a pneumothorax, it is not recommended because these lower frequency probes may not provide adequate visualization of the superficial pleural line.
Sonographic Findings
Pneumothorax is generally diagnosed by noting the sonographic absence of lung sliding, which will be present in 90-95% of pneumothoraces.5 Lung sliding is characterized by a shimmering to and fro appearance of the pleural line, sometimes referred to as “ants marching.” Frequently, bright hyperechoic vertical streaks, called comet tails or z-lines (see Figure 1), may be seen emanating from the pleural line and indicate the presence of lung sliding (i.e., no pneumothorax). A lung point is the visualization of the edge of a pneumothorax, where lung sliding and no lung sliding is seen in the same field of view. Sonographically, it is the point at which the visceral pleura has separated from the parietal pleura along the chest wall. This sign has a sensitivity of 60-66%, and is noted to be almost 100% specific.4,12
If it is difficult to visualize lung sliding, motion or M-mode can also be used to visualize movement of the pleura. Upon switching to M-mode, the ultrasound operator will position the M-mode line over the pleural line between two rib shadows (Video 4). M-mode is then activated, and plotted across the screen in one of two common patterns. The appearance of the “sky-ocean-beach” pattern indicates normal lung sliding and therefore no pneumothorax (see Figure 1). The appearance of a “sky-ocean-no beach” pattern, sometimes referred to as “barcode” or “stratosphere” sign, indicates the absence of lung sliding and therefore is indicative of a pneumothorax.
Video 4

Figure 1

The size of the pneumothorax can be assessed sonographically as well. In a supine patient, a small pneumothorax will only be visible anteriorly. If the absence of lung sliding is noted to extend laterally to the mid-axillary line or even posteriorly, the pneumothorax can be presumed to be larger in size. A study by Soldati and colleagues showed that in comparison with chest computed tomography (CT), ultrasound correctly identified the size of 20 out of 25 pneumothoraces.5 Similarly, a study by Blaivas and colleagues noted good correlation of the ultrasound with CT, when determining if a pneumothorax was less than or greater than 10%.4 However, the same study noted that sonographers may have difficulty differentiating between a medium (11-40%) or large (>40%) pneumothorax. In these larger pneumothoraces, the area of lung collapse increases but the area of separation from the pleural wall does not. This may limit the ability of ultrasound to correctly determine the degree of lung collapse.4
Under some conditions lung ultrasound can falsely indicate the presence of a pneumothorax. In a trauma patient, the presence of a mainstem intubation or a pleural adhesion may falsely suggest a pneumothorax due to the lack of lung sliding seen in these conditions. Thoracic dressings and extensive subcutaneous emphysema may also make the examination more difficult to perform. Although ultrasound is very sensitive, it may fail to identify a very small pneumothorax if the probe is not placed directly over the pneumothorax itself. Furthermore, the accuracy can be decreased by using a lower frequency (abdominal or cardiac) probe and is shown to be operator dependent.
In the austere environment with no nearby trauma center, point-of-care ultrasound has the potential to revolutionize care delivered at the point of injury. Commercially available units are now the size of a smartphone or handheld tablet and can deliver high quality images to help direct care, improve diagnostic accuracy over physical examination, and aid in triage and prioritization for medical evacuation. Despite their small size, these hand-held units have continued to show better sensitivity than chest radiography for detection of traumatic pneumothorax.13
Point-of-care ultrasound was critical to making a timely diagnosis of a tension pneumothorax in the case reviewed here, however, there are multiple other potential applications in the austere medical environment. In the absence of radiographs, point-of-care ultrasound can be used for the diagnosis of fracture detection and reduction, musculoskeletal injuries, and procedural guidance (e.g., abscess drainage, intravenous access, confirmation of intra-osseous needle placement).
Disclaimer: The views expressed herein are those of the authors and do not reflect the policy or position of San Antonio Military Medical Center, the Department of the Army, the Department of the Air Force and the Department of Defense or the U.S. Government.
References/Further Reading:
- Morgan AR, Vasios WN, Hubler DA, et al. Special operator level clinical ultrasound: an experience in application and training. J Spec Oper Med.2009;10(2),16-21.
- Hampton KK, Vasios 3rd WN, & Loos PE. SOLCUS: Update On Point-of-Care Ultrasound In Special Operations Medicine. J Spec Oper Med. 2015;16(1),58-61.
- International ATLS working group, Subcommittee AT. Advanced trauma life support (ATLS®): the ninth edition. J Trauma Acute Care Surg. 2013;74(5):1363-6.
- Blaivas M, Lyon M, & Duggal SA. Prospective comparison of supine chest radiography and bedside ultrasound for the diagnosis of traumatic pneumothorax. Acad Emerg Med.2005;12(9),844-849.
- Soldati G, Testa A, Sher S, et al. Occult traumatic pneumothorax: diagnostic accuracy of lung ultrasonography in the emergency department. CHEST. 2008;133(1),204-211.
- Zhang M, Liu ZH, Yang JX, et al. Rapid detection of pneumothorax by ultrasonography in patients with multiple trauma. Crit Care.2006;10(4),R112.
- Alrajhi K, Woo MY, & Vaillancourt C. Test characteristics of ultrasonography for the detection of pneumothorax: a systematic review and meta-analysis. CHEST.2012;141(3),703-708.
- Ding W, Shen Y, Yang J, et al. Diagnosis of pneumothorax by radiography and ultrasonography: a meta-analysis. CHEST. 2008;140(4),859-866.
- Chan SSW. Emergency bedside ultrasound to detect pneumothorax. Acad Emerg Med.2003;10(1),91-94.
- Alrajab S, Youssef AM, Akkus NI, etc. Pleural ultrasonography versus chest radiography for the diagnosis of pneumothorax: review of the literature and meta-analysis. Crit Care.2013;17(5),R208
- Oveland NP, Søreide E., Lossius HM, et al. The intrapleural volume threshold for ultrasound detection of pneumothoraces: An experimental study on porcine models. Scandinavian journal of trauma, resuscitation and emergency medicine. 2013;21(1),11.
- Lichtenstein D, Mezière G, Biderman P, et al. The “lung point”: an ultrasound sign specific to pneumothorax. Intensive Care Med.2000;26(10),1434-1440.
- Kirkpatrick AW, Sirois M, Laupland KB, et al. Hand-held thoracic sonography for detecting post-traumatic pneumothoraces: The Extended Focused Assessment with Sonography for Trauma (EFAST). J Trauma.2004;57(2),288-295.