Authors: Jeff Harper, MD (EM Resident Physician, LSUHSC-Baton Rouge), Raymond Beyda, MD (EM Resident Physician, SUNY Downstate-Kings County Medical Center, Brooklyn, NY), Richard Sinert, DO (EM Attending Physician, SUNY Downstate-Kings County Medical Center, Brooklyn, NY), and Emilio Volz, MD (EM Associate Program Director and Emergency Ultrasound Fellowship Director, LSUHSC-Baton Rouge) // Edited by: Manpreet Singh, MD (@MPrizzleER – Assistant Professor of Emergency Medicine / Department of Emergency Medicine – Harbor-UCLA Medical Center) and Alex Koyfman, MD (@EMHighAK – EM Attending Physician, UT Southwestern Medical Center / Parkland Memorial Hospital)
Introduction
A 12-year-old boy is brought into your Emergency Department one afternoon after being hit by a car while playing in the street. He arrives on a spine board with cervical collar in place. You see an obvious deformity to his left thigh, and scattered abrasions. As you begin to manage your first patient, the phone rings with an EMS notification: you have a 68-year-old male being brought in after being struck by a moving vehicle as he was crossing the street. As you prepare to manage both cases, you wonder to yourself, what other history should you look for? What types of injuries should you suspect and be looking for?
Pedestrian-vs-automobile accidents are a common source of severe blunt poly-trauma. Below is a discussion of the mechanism, injury patterns, and management options to consider when evaluating one of these patients in your busy department.
Background
On September 14, 1899, Henry Bliss became the first person in the United States to die as a result of a motor vehicle accident. He was a pedestrian.1 When it comes to managing trauma patients in the emergency department (ED), mechanism of injury is everything.2 The pedestrian struck by a motor vehicle represents a clinical scenario with unique injury patterns, and therefore important assessment and management considerations.2-8
Key Stats from 2015 National Highway Traffic Safety Administration3
- In 2015 there were 5,376 pedestrians killed and an estimated 70,000 injured in the United States, a 10% increase from the prior year.
- A pedestrian is killed every 1.6 hours and injured every 7.5 minutes.
- 76% fatalities occur in urban areas
- 74% fatalities occur at night.
- In 35% of cases the pedestrian had a blood alcohol content of 0.08g/dL or higher.
According to a 2017 meta-analysis, the incidence of pedestrian-vs-automobile accidents is highly variable based on location, ranging from 20 per 100,000 to 203 per 100,000.4
Pedestrian collisions occur more often in the evening and at night, likely due to the possible influence of alcohol, on either or both the driver and/or pedestrian, and impaired vision during the darker hours of the day. In rural areas, there are other factors that contribute to greater morbidity and mortality from pedestrian trauma, namely, the presence of higher speed highways, and greater distances to regional or local trauma centers.5 Pediatric patients, particularly younger than 16 years old, are at greater risk for pedestrian trauma accounting for approximately 30% of cases in the United States.5 On the opposite end of the age spectrum, geriatric patients are at higher risk for being struck due to factors associated with hearing, vision, gait, and reflex response impairment. Importantly, this is also the population of patients to suffer from chronic medical comorbidities which coupled with natural aging tend to decrease physiologic reserve and therefore have much higher rates of critical illness and overall morbidity and mortality as a result of these injuries.5,6
Pedestrian-vs-automobile accidents are usually isolated events, but on rare occasions, can be mass-casualty incidents. Recent examples are the August 12, 2017 attack on protestors in Charlottesville, Virginia7 and the intoxicated individual who lost control of his vehicle and drove into a Mardi Gras crowd in New Orleans, Louisiana on February 25, 2017.8
Mechanism
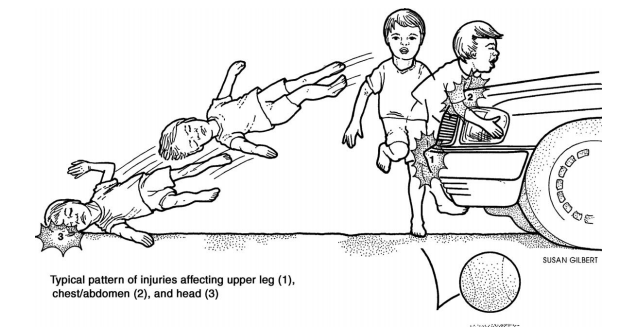
Pedestrian-vs-automobile is a serious mechanism of injury (Figure 1), even at a relatively low vehicle speed. One example is driveway/back-over injuries. In these accidents, mortality rates for children are up to ten times higher than other pediatric pedestrian accidents.9-13
Injury location and severity depends on factors such as speed, angle, and impact locations (i.e. pedestrian height vs bumper height, design/shape of vehicle).5,9,12,14 An impact to the lower legs will accelerate the legs away, rotating the upper body/head towards the hood or windshield. Alternatively, an impact at thigh-level or higher (as in a small child or in the case of a very tall vehicle) will cause the person to be thrown away from the vehicle and/or knocked down and run over.5
As vehicle speed increases, the amount of energy transferred to the patient and ultimately, mortality, increases dramatically. Mortality doubles with passenger car speeds from 30 km/h (18.6 mph) to 40 km/h (24.8 mph), and is increased six-fold by 50 km/h (31 mph). Upon exceeding 80 km/h (49.7 mph), mortality approaches 100%.14
Pedestrian related traffic accidents are also greatly affected by size of the motor vehicle involved. Bicycle and motorcycle related pedestrian accidents are approximately one-quarter and one-half as deadly as car-related accidents, respectively. A large truck is about six times deadlier than a passenger car. Trucks, in addition to their sheer mass, tend to have more rigid bumpers/frames resulting in higher energy transfer,12 and due to their dimensions, result in the pedestrian being run over nearly half the time.14

Types of Injuries
Certain regions of the body are much more likely to be injured in pedestrian-vs-automobile accidents. Analysis of a French trauma registry in 2011 classified pedestrian injuries by the Abbreviated Injury Scale (AIS).
AIS2+ injuries by body region12
- Lower extremities 49.56%,
- Head/face/neck 38.07%,
- Upper extremities 26.45%,
- Pelvis 8.79%,
- Thorax 8.54%,
- Spine 4.23%,
- Abdomen 2.98%.
However, with pediatric patients (see Figure 2) head injury becomes the most common injury followed by musculoskeletal.6,10,12 There was a higher incidence of femur fractures in the pediatric age group (15.5% in patients<14 years old), likely explained by the fact that adults sustain impact by a bumper to the lower legs whereas younger pediatric patients will sustain the majority of the impact to the thighs.10
The most life-threateningly severe (AIS4+) injuries are generally to the head and thorax. Males are more likely overall to be more severely injured and more likely to have injuries to the head or thorax. Females are more likely to have pelvic or upper extremity injuries.12
Advanced Trauma Life Support (ATLS) notes that in addition to head and pelvic/lower extremity injuries, you should also think about traumatic aortic dissection and abdominal visceral injuries.17 A 2004 study found aortic dissection to occur in 16 out of 5,838 patients (0.3%), with increasing incidence with age.10 Many other injury types also increased with age including: head, chest, spinal, and abdominal injuries. Overall, both injury severity and mortality increase significantly with age, particularly for those over 64 years old.10,12
Yanar H, et al. looked at risk factors associated with cervical spine injury (CSI).18 They found an overall incidence of CSI of 2.1%, which when stratified by age, was more likely to occur in older patients with an incidence as high as 4.4% in patients older than 65 years old.18 In this study, there was also a 40% rate of head injury with a 10.5% rate of severe TBI.18 Interestingly, patients with no associated TBI did not suffer from CSI, and in patients with more severe TBI there was a higher incidence of associated CSI, suggesting an association between severe TBI and CSI.18 There was also a higher incidence of CSI in patients with concomitant thoracic spine fracture (18.7%) pelvic fractures (11.5%), and severe chest trauma defined by AIS 3+ (11.6%).18
Reith, et al.9 found differences between pedestrians and motor vehicle occupants. Among patients admitted to the ICU, pedestrians have higher rates of mortality (22% versus 12%), head injuries (64% versus 47%), pelvic injuries (32% versus 23%), lower extremity injuries (52% versus 43%), lower presenting GCS less than 9 (36% versus 28%), and systolic blood pressure less than 90mmHg (18% versus 13%).9 These differences were despite shorter on-scene and collision-to-treatment times for pedestrians.9
Management/Workup
Management of the pedestrian-vs-automobile victim, as with any trauma patient, starts in the pre-hospital environment and continues upon arrival in the ED.2,17 Trauma assessment and resuscitation then proceeds methodically with a thorough primary survey aimed at identifying immediately life-threatening injuries which can then be potentially intervened upon.
Gathering data from pre-hospital providers with respect to mechanism of injury can guide the trauma team in predicting associated injury patterns as part of the overall assessment and resuscitation. Knowing that the patient’s mechanism of injury was a result of being a pedestrian struck by a moving motor vehicle can guide targeted evaluation, with the trauma team simultaneously resuscitating and looking for specific injuries. However, as both head injuries and intoxication are extremely common, be aware that history may be unavailable and physical exam may be unreliable.3,9-12
Decision Tools/Clinical Prediction Scores
Decision tools can be employed in appropriate patients. Criteria for head CT (PECARN, New Orleans Head-CT, Canadian Head CT)19-20 and C-spine (NEXUS, Canadian C-Spine)21 are well-known and commonly applied.
In 2009 Holmes et al.22 looked at clinical prediction rules for blunt abdominal trauma, and found that patients were low risk (100% sensitivity for ruling out therapeutic abdominal intervention) if they did not have GCS less than 14, costal margin or abdominal tenderness, femur fracture, hematuria (greater than 25 red blood cells/high powered field), hematocrit less than 30%, or an abnormal plain chest radiograph (CXR).
Consider though that decision rules in general require patients who are not altered and can provide a reliable exam; many pedestrian-vs-automobile victims may not qualify due to the high prevalence of head injuries, intoxication, and distracting injuries.
Imaging Considerations
Emergency bedside ultrasound, computed tomography scan (CT), and x-ray can be utilized to improve decision-making and aid in diagnosis. Extended Focused Assessment with Sonography in Trauma (e-FAST) in hemodynamically unstable patients with suspected thoracic or abdominal trauma can help determine need for an emergent intervention such as chest tube thoracostomy, pelvic binding, or exploratory laparotomy.23-24 Ultrasound is also a viable option for detecting pneumothorax or hemothorax, with a sensitivity of 92 to 100% in the hands of a skilled practitioner.25
Pelvic fractures are traditionally screened for with x-ray; however, this step may often be forgone in certain trauma situations. Because CT is more sensitive for pelvic fractures, x-ray may be avoided in normotensive patients in whom a CT is planned and with no pelvic instability or signs of dislocation.26
Not everything detected on CT will require intervention. In 2007, Plurad, et al.27 reviewed data from 1,873 chest computerized tomography scans (CCT) after negative CXR in trauma patients. The authors found no increased trend in diagnosis of blunt aortic injury despite a 10-fold increase in use of CCTs. They did find missed occult pneumothoraces or hemothoraces in 102 (5.4%) patients; however, only 12 (0.64%) required intervention.27
Due to the high energy transfer involved in pedestrian-vs-automobile accidents, many physicians may opt for whole body computerized tomography scans (WBCT) in this setting. The role of WBCT, however, remains controversial. In a 2006 prospective observational study of 1,000 patients, Salim et al. found that WBCT changed management in 18.9% of patients with significant mechanism of injury, no visible external injury, and either normal abdominal exam or unreliable exam due to mental status. Nearly 26% of the patients included were pedestrians hit by vehicles and thrown greater than 10 feet.28 In a 2013 retrospective study of 4,621 patients, Huber-Wagner et al.29 found a mortality benefit for WBCT vs selective-scanning for patients with polytrauma, but specific mechanisms were not compared.
In REACT-2, a prospective multicenter randomized controlled trial, immediate WBCT for trauma patients overall demonstrated decreased time to diagnosis and length of stay in the ED but no difference in mortality vs standard selective workup.30 However, pedestrian-vs-automobile victims only represented 74 out of 1,083 patients in this study. Subgroups of polytrauma and TBI tended to favor WBCT but were not statistically significant.30 A pedestrian-vs-automobile victim often belongs to multiple patient subgroups and may deserve future consideration as a separate subgroup. Furthermore, as the authors point out, 46% of patients in the standard selective group ultimately underwent the equivalent of WBCT.
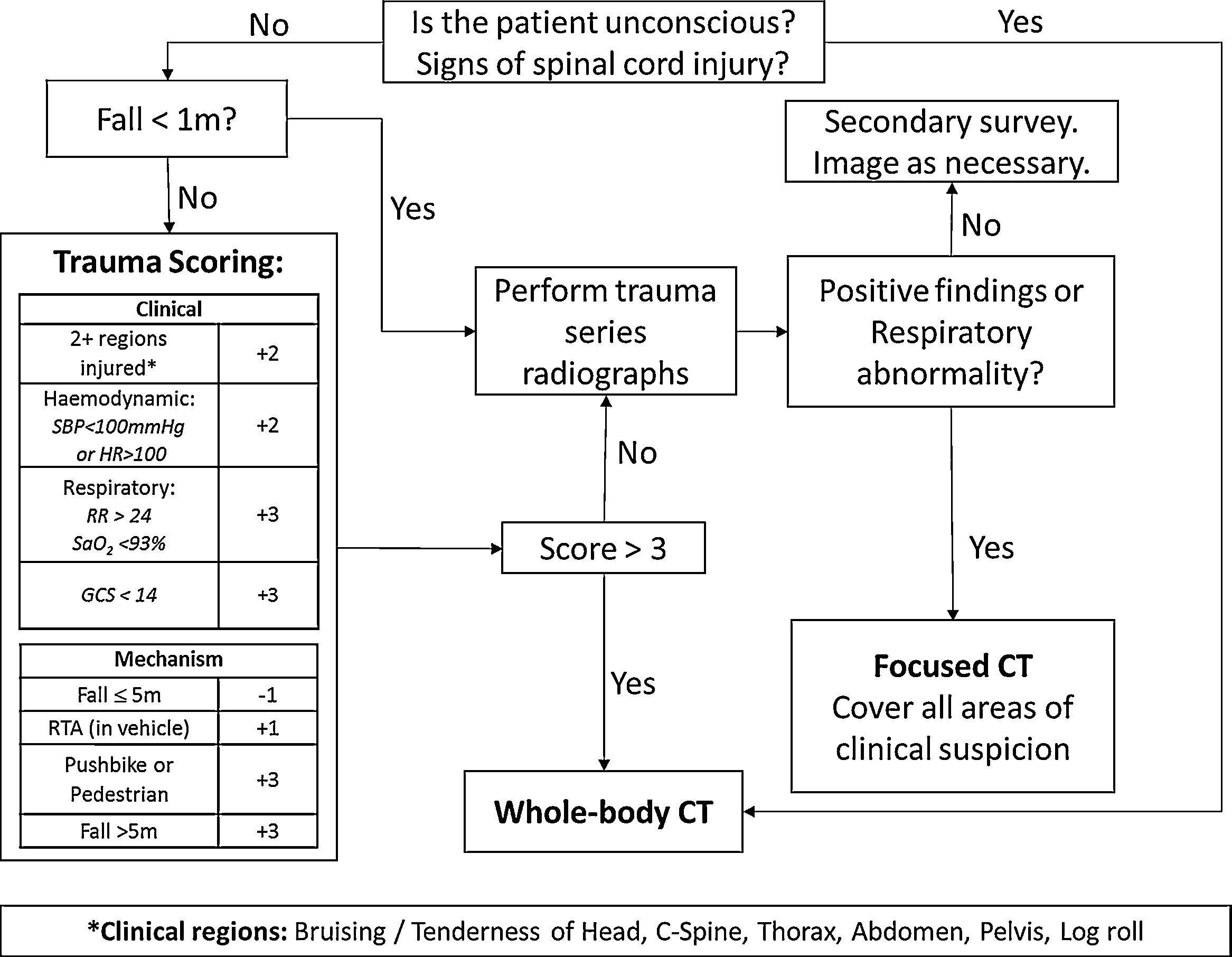
Davies, et al.31 published a cohort study in 2015 which reviewed trauma data to determine which patients might benefit from WBCT based on risk factors. Under their algorithm (Figure 3), a pedestrian-vs-automobile patient with any one of the following clinical findings will likely have a significant injury (Sensitivity – 97%, Specificity – 56%) and should be considered for WBCT: GCS is less than 14, any sign of spinal cord injury, hemodynamic instability, and multiple body regions injured.
Summary
Pedestrian-vs-automobile accidents are common, particularly in urban areas. The mechanism has the potential for high energy transfer that can result in serious polytrauma and often follows certain injury patterns. Decision tools may assist in reducing unnecessary imaging and radiation in select patients. However, the high incidence of head injuries and intoxication often limits the ability to obtain history and reliable exam findings. Maintaining a systematic approach is necessary to reduce the likelihood of missing clinically relevant injuries. Plain radiographs, ultrasound, and computed tomography can all play important roles depending on the clinical situation.
Important Injury Pattern Considerations
- Head injury: pretty much all injury patterns are fair game, and the altered patient in this setting should prompt consideration for any of the typical intracranial injuries (intra-axial and extra-axial injuries, e.g. subarachnoid hemorrhage, intraparenchymal hematoma, subdural and epidural hematoma). In older adults especially, consider use of anticoagulant and/or antiplatelet medications in assessing risk for intracerebral hemorrhage.
- Cervical Spine injury: prepare to appropriately assess and risk stratify the patient using appropriate clinical prediction scores to determine the need for imaging or cervical spine immobilization.
- Upper Extremity and Shoulder: look for joint dislocations, long bone fractures, and assess for vascular compromise and potential compartment syndrome.
- Chest wall and Ribs: assess the integrity of the chest wall, looking for rib fractures with associated blunt thoracic trauma e.g. pulmonary contusion
- Pelvis: look for the presence of an unstable pelvis and appropriately bind, image, manage associated bleeding complications, and consult the appropriate services.
- Lower Extremity: don’t forget to examine the lower extremities looking for fracture, dislocation, vascular compromise, and/or compartment syndrome. Appropriately image, splint, and consult for specific injuries to the lower extremities.
Pearls/Pitfalls
- Understanding the mechanism of injury as well as patient-related factors such as age can help to predict patterns of injury, and guide a more focused evaluation of the patient.
- Pedestrian-vs-automobile victims have suffered a severe mechanism. Expect a polytrauma patient to come through the door! In addition to the routine trauma evaluation with attention to the ABCDEs of resuscitation, focus your evaluation of the patient on commonly expected injury patterns.
- Common injuries include head trauma, lower extremity/pelvic fractures, and upper extremity fractures. Head and thoracic trauma carry the highest mortality.
- With the exception of femur fractures potentially occurring more commonly in pediatric patients, increasing age is associated with higher mortality and more severe injuries of the head, spine, chest, abdomen, pelvis and extremities.
- Don’t be distracted by dramatic injuries such as an open lower extremity fracture and miss a life-threatening thoracic/abdominal injury.
- Ultrasound, X-ray, and CT can aid in rapid diagnosis of injuries.
- Have a low threshold for the use of WBCT in pedestrian injury patients with decreased GCS, signs of neurologic injury, hemodynamic instability, polytrauma, or any patient with an unreliable history and physical exam.
References/Further Reading
- The National Committee for Injury Prevention and Control. Injury prevention: meeting the challenge. American Journal of Preventative Medicine. 1989;5(3 Suppl):115.
- Gross, Eric A. and Martel, Marc L. Multiple Trauma. In Rosen’s Emergency Medicine: Concepts and Clinical Practice. 8th ed. Philadelphia, Elsevier. 2018;33:287-300.e2.
- Traffic Safety Facts 2015: Pedestrians. National Highway Transportation Safety Administration 2017.
- Charters KE, Gabbe BJ, Mitra B. Population incidence of pedestrian traffic injury in high-income countries: A systematic review. Injury. 2017;48:1331-1338.
- Chakravarthy B, Vaca FE, Lotfipour S, Bradley D. Pediatric Pedestrian Injuries, Emergency Care Considerations. Pediatric Emergency Care. 2007;23(10):738-743.
- Peng RY, and Bongard FS. Pedestrian Versus Motor Vehicle Accidents: An Analysis of 5,000 Patients. J Am Coll Surg. 1999 Oct;189(4):343-8.
- Stolberg SG, Rosenthal BM. Man Charged after White Nationalist Rally in Charlottesville Ends in Deadly Violence. NY Times. Aug 12, 2017.
- Mele C, Robertson C. Pickup Plows Into Crowd at a Mardi Gras Parade, Injuring 28. NY Times. Feb 25, 2017.
- Reith G, Levering R, Wafaisade A, Hensel KO, Paffrath T, Bouillon B, Probst C. Injury pattern, outcome and characteristics of severely injured pedestrian. Scandinavian Journal of Trauma, Resuscitation and Emergency Medicine. 2015;23(1).
- Demetriades D, Murray J, Martin M, Velmahos G, Salim A, Alo K, Rhee P. Pedestrians injured by automobiles: relationship of age to injury type and severity. Journal of the American College of Surgeons. 2004;199(3):382-387.
- Srinivasan S, Chang T. Diagnosis and Management of Motor Vehicle Trauma in Children: An Evidence-Based Review. Pediatric Emergency Medicine Practice. 2013;10(8).
- Marin JL, Lardy A, Laumon B. Pedestrian Injury Patterns According to Car and Casualty Characteristics in France. Annals of Advances in Automotive Medicine. 2011;55:137-146.
- Patrick DA, Bensard DD, Moore EE, Partington MD, Karrer FM. Driveway crush injuries in young children: A highly lethal, devastating, and potentially preventable event. Journal of Pediatric Surgery. 1998;33(11):1712-1715.
- Martin JL, Wu D. Pedestrian fatality and impact speed squared: Cloglog modeling from French national data. Traffic Inj Prev. 2017 May 30:1-8.
- Yang J. Review of injury biomechanics in car-pedestrian collisions. International journal of vehicle safety. 2005 Jan 1;1(1-3):100-17.
- Atabaki SM. Prehospital evaluation and management of traumatic brain injury in children. Clin Ped Emerg Med. 2006; 7(2):94-104.
- Advanced trauma life support: student course manual. 9th Chicago, IL: American College of Surgeons; 2012.
- Yanar H, et al. Pedestrians Injured by Automobiles: Risk Factors for Cervical Spine Injuries. J Am Coll Surg. 2007 Dec;205(6):794-9.
- Kuppermann N, et al. Identification of children at very low risk of clinically-important brain injuries after head trauma: a prospective cohort study. Lancet. 2009;374(9696)1160-1170.
- Stiell IG, et al. Comparison of the Canadian CT Head Rule and the New Orleans Criteria in patients with minor head injury. 2005;294(12):1511-1518.
- Stiell IG, et al. The Canadian C-Spine Rule versus the NEXUS Low-Risk Criteria in patients with trauma. N Engl J Med. 2003;349:2510-2518.
- Holmes JF, Wisner DH, McGahan JP, Mower WR, Kuppermann N. Clinical prediction rules for identifying adults at very low risk for intra-abdominal injuries after blunt trauma. Ann Emerg Med. 2009;54(5):575-584.
- Montoya J, Stawicki SP, Evans DC, Bahner DP, Sparks S, Sharpe RP, Cipolla J. From FAST to E-FAST: An overview of the evolution of ultrasound-based traumatic injury assessment. European Journal of Trauma and Emergency Surgery. 2016;42(2):119-126.
- Diercks DB, Mehrotra A, Nazarian DJ, Promes SB, Decker WW, Fesmire FM. Clinical Policy: Critical Issues in the Evaluation of Adult Patients Presenting to the Emergency Department with Acute Blunt Abdominal Trauma. Annals of Emergency Medicine. 2011;57(4):387-404.
- Ball CG, Kirkpatrick AW, Feliciano DV. The occult pneumothorax: what have we learned? Can J Surg. 2009;52(5):E173-179.
- Soto JR, Zhou C, Hu D, Arazoza AC, Dunn E, Sladek P. Skip and save: utility of pelvic x-rays in the initial evaluation of blunt trauma patients. Am J Surg. 2015;210(6):1076-1079.
- Plurad D, Green D, Demetriades D, Rhee P. The increasing use of chest computed tomography for trauma: is it being overutilized? J Trauma. 2007;62(3):631-635.
- Salim A, Sangthong B, Martin M, Brown C, Plurad D, Demetriades D. Whole body imaging in blunt multisystem trauma patients without obvious signs of injury. Arch Surg. 2006;141:468-473.
- Huber-Wagner S, Lefering R, Qvick LM, et al. Effect of whole-body CT during trauma resuscitation on survival: a retrospective, multicentre study. Lancet. 2009;373:1455-1461.
- Sierink JC, Treskes K, Edwards MJR, Beuker BJA, Hartog DD, Hohmann J, Dijkgraaf MGW, Luitse JSK, Beenen LFM, Hollmann MW, Goslings JC. Immediate total-body CT scanning versus conventional imaging and selective CT scanning in patients with severe trauma (REACT-2): a randomised controlled trial. 2016;388:673-683.
- Davies RM, Scrimshire AB, Sweetman L, Anderton MJ, Holt EM. A decision tool for whole-body CT in major trauma that safely reduces unnecessary scanning and associated radiation risks: An initial exploratory analysis. Injury. 2016;47:43-49.







2 thoughts on “Pedestrian Struck by Vehicle: Pearls and Pitfalls of ED Management”
Pingback: Pedestrian Struck – Found Down
Pingback: Ped Struck – Found Down