Authors: Lilly Bellman, MD (@LillyBellman, Pediatric Emergency Medicine / Ultrasound Fellow, Harbor-UCLA Medical Center) and Manpreet Singh, MD (@MPrizzleER, EM Physician at Harbor-UCLA Medical Center, Torrance, CA) // Reviewed by Stephen Alerhand, MD (@SAlerhand); Brit Long, MD (@long_brit); and Teresa Liu, MD (@Tee1540)
Lung Ultrasound in Pandemics
Respiratory virus pandemics have shown how lung ultrasound (LUS) can shine. In 2009, when the H1N1 pandemic influenza strain caused surges in Emergency Department (ED) visits with respiratory symptoms, investigators found that LUS could help identify patterns characteristic of the influenza viral pneumonia versus suspected bacterial pneumonias versus both with good interrater reliability in both adults1 and children2. This led to presumptive diagnoses and more targeted treatment choices faster than the 1.5 hr wait for chest radiography (CXR) described at that time.2
Now with our present SARS-CoV-2 pandemic, LUS is again being recognized as a useful tool in more rapid identification of likely COVID-19 patients3,4,5, and also in their ongoing ICU management. Findings on LUS have been shown to correlate well with computed tomography (CT) findings as long as they extend to the pleural line (most do).3,4,6 We still need to find the optimal way to use LUS, especially as hospitals experiencing surges of patients may struggle with radiology resources such as CT and CXR, where “terminal cleaning” and exposure to other staff can occur. Using a bedside test such as LUS can also be beneficial through less movement of these infectious patients and exposure to fewer providers.
Here we suggest a scan protocol, review the findings of the emerging literature, and consider potential frameworks in which LUS may help us in rapid evaluation of suspected COVID patients.
How to Scan
1.) Transducer Choice:
- Linear and microconvex transducers allow the most detailed assessment of the pleura.
- Phased array or curvilinear transducers are also useful, allowing for deeper visualization of B-lines, lobar consolidations and effusions.
- Note – Depth must be decreased to appreciate subtleties of the pleural lining.
- Lung mode setting (if your machine has it) optimizes visualization of the artifacts key to interpreting lung ultrasound.
- If your machine does not have this setting, consider turning off multibeam detection.
2.) Comprehensive Scan Protocol
COVID-19 has been described to have bilateral, patchy findings, particularly in the posterior and inferior areas.4 It is best to have a comprehensive and systematic approach to image the lungs. As there are many approaches to scanning (6, 8 or 12-zone protocols), we suggest one such approach here which has been described in multiple studies in the literature6,7.
- Split the thorax into anterior, lateral (midaxillary line), and posterior zones (Figure 1).
- The posterior zone can be scanned seated or by rolling the patient.
- Scan each zone.
- Split into superior and inferior sections of each and save clips from each.
- Transverse views allow more visualization of the pleural line.
- Consider addition of your bedside cardiovascular ultrasound to look for global function, as well as your IVC/VExUS scans.
- Myocardial dysfunction described in 7% COVID patients and 22% those who are critically ill.8
- Identify alternate diagnoses.
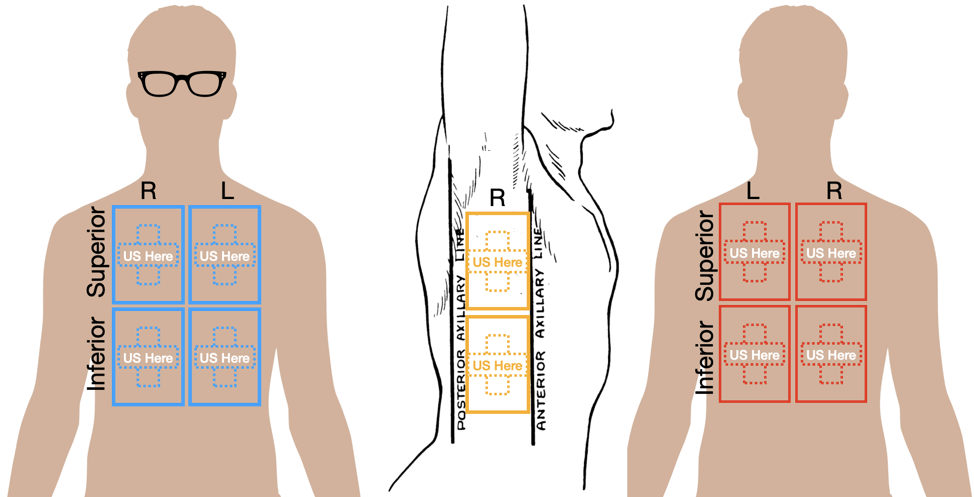
Figure 1: Comprehensive LUS scanning locations. Transverse and longitudinal scanning (cross shaped scan pattern) in each of the rectangles in the anterior (blue), lateral (yellow), and posterior (red) areas.
COVID LUS Findings3
- B-Lines and interstitial syndrome
- Early disease: Focal patches of B-lines.
- Most severe: Diffuse confluent B-lines, progress to sonographic “white lung”.

- Small subpleural consolidations (often associated with adjacent B-lines with small effusions)
- Pleural line abnormalities (irregularities, thickening)
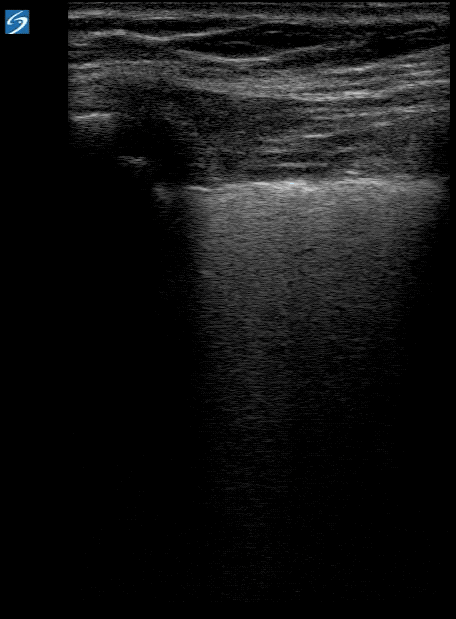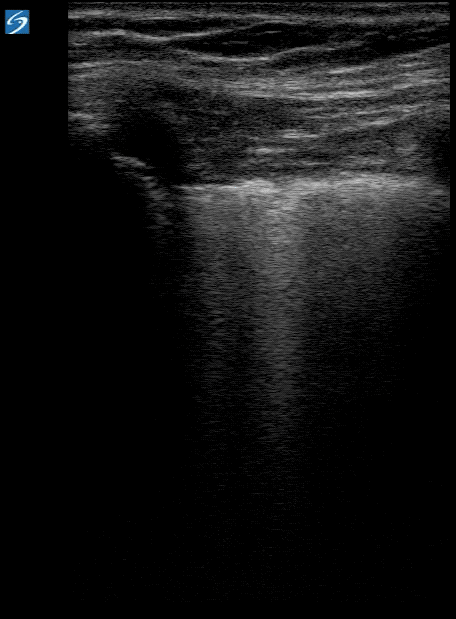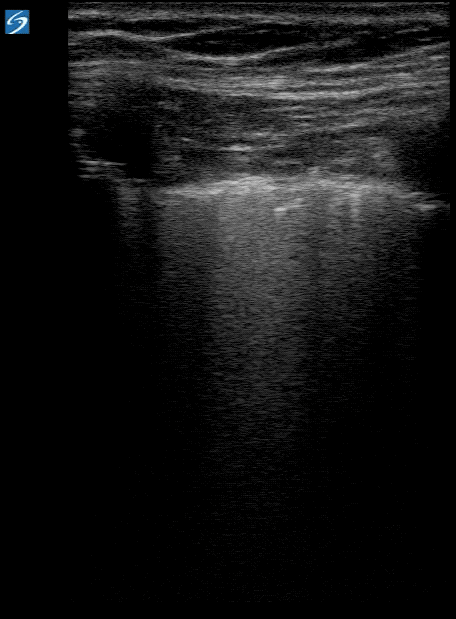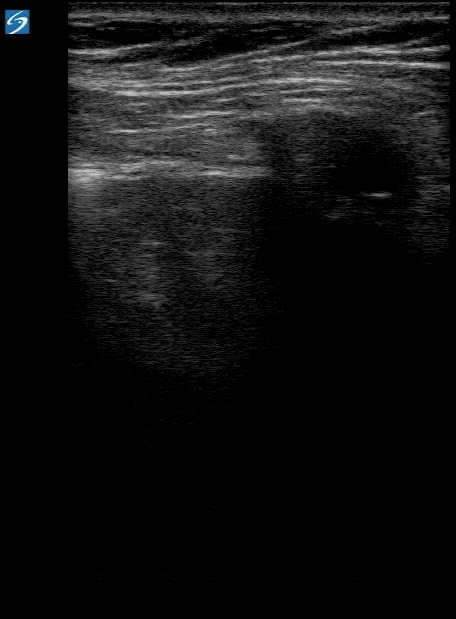
- Findings more concentrated posteriorly and inferiorly

The POCUS Atlas has assembled a collection of example findings as discussed above. The figure below summarizes the findings that occur in COVID-19.
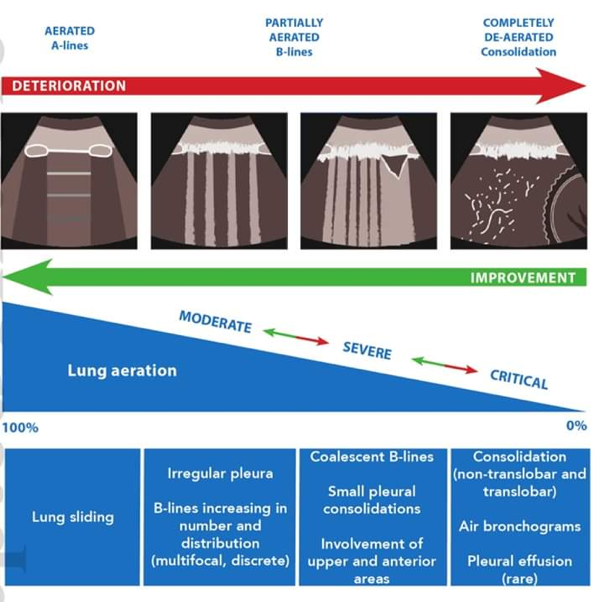
- Caveats:
- COVID vs. CHF: B-line pattern can be seen in both, but B-lines in COVID-19 are generally patchy and have accompanying pleural line abnormalities.
- Bacterial pneumonias: Larger consolidations with air bronchograms. We are still learning the frequency of superinfection. Other clinical and laboratory parameters can be helpful (i.e. CBC and procalcitonin).
Which patients to scan?
We are still figuring out how best to use LUS in this pandemic, but here are some ideas that fit into two main frameworks:
- Scan the WELL: Patients who will be discharged home and may not meet criteria to test, but we may pick up characteristic findings suggestive of COVID19 and provide them with anticipatory guidance.
- One study of cruise ship passengers showed CT findings in ~50% asymptomatic people who tested positive for SARS-CoV-2 suggesting there could be early sonographic findings to detect9.
- Could use as presumptive diagnostic modality in health systems with limited COVID-19 testing capabilities.
- CONS:
- More potential for exposure to provider(s) with closer and longer exposure with asymptomatic patient.
- Perhaps unecessary to image these patients at this stage, who could be discharged faster from the ED with return pre-cautions.
- More cleaning required of machine and additional staff exposure to patient.
- More potential for exposure to provider(s) with closer and longer exposure with asymptomatic patient.
- Scan the SICK: Patients who will likely need hospitalization due to hypoxemia, etc.
- Identify characteristic patterns, which can be tracked over time.
- Less reliance on chest x-ray and/or CT.
- Identify alternative and/or additional diagnoses (myocarditis, pneumothorax, CHF, large lobar pneumonias, pleural effusions*)
- CONS:
- More difficult to perform complete scan on sick intubated patients, where need to move patient with assistance and care.
- More time in room leads to more exposure to provider.
- Identify characteristic patterns, which can be tracked over time.
*Small pleural effusions have been noted in some COVID patients, but larger effusions more likely suggest alternative diagnoses; however this comes from limited data sets.
The Disinfection Question
This is one of the biggest questions and potential barriers to large scale LUS for COVID-19. Here are some ideas that have come up in discussions among US expert colleagues:
- Remove all non-essential items from ultrasound machine (baskets, intravenous access supplies, etc).
- Wipe whole machine from screen to wheels with vendor-approved wipes according to wipe instructions (allow effective wet time/dry time).
- Use PPE on machine (wrap in a gown to avoid contact with parts of machine).
- Use transducer covers.
- Use single-use gel packets instead of bottles of gel.
Handheld units may be particularly useful and easier to disinfect. One suggested idea is to use a wireless probe and tablet each placed in their own single use plastic covers10,11.
Take-aways
Experience from our international colleagues in China and Italy suggest that LUS is a bedside technique that can be helpful in rapid presumptive diagnoses of COVID-19 patients.
Whether you find yourself in the thick of a surge, or preparing for one, consider how you might work LUS into the workflow for caring for these patients.
References
- Testa A, Soldati G, Copetti R, Giannuzzi R, Portale G, Gentiloni-Silveri N. Early recognition of the 2009 pandemic influenza A (H1N1) pneumonia by chest ultrasound. Crit Care. 2012;16(1):1-8. doi:10.1186/cc11201
- Tsung JW, Kessler DO, Shah VP. Prospective application of clinician-performed lung ultrasonography during the 2009 H1N1 influenza A pandemic: distinguishing viral from bacterial pneumonia. Crit Ultrasound J. 2012;4. http://www.criticalultrasoundjournal.com/content/4/1/16. Accessed March 10, 2018.
- Peng QY, Wang XT, Zhang LN, Critical C, Ultrasound C, Group S. Findings of lung ultrasonography of novel corona virus pneumonia during the 2019 – 2020 epidemic. Intensive Care Med. 2020;(87):6-7. doi:10.1007/s00134-020-05996-6
- Huang Y, Liu Y, Zhang Y, et al. A preliminary study on the ultrasonic manifestations of peripulmonary lesions of non-critical novel coronavirus pneumonia (COVID-19). Soc Sci Res Netw. 2020:300. https://papers.ssrn.com/sol3/papers.cfm?abstract_id=3544750.
- Smith M, Hayward S, Innes S, Miller A. Narrative review Point-of-care lung ultrasound in patients with COVID-19 – a narrative review. Anaesthesia. 2020. doi:10.1111/anae.15082
- Lichtenstein DA, Lascols N, Mezière G, Gepner A. Ultrasound diagnosis of alveolar consolidation in the critically ill. Intensive Care Med. 2004;30(2):276-281. doi:10.1007/s00134-003-2075-6
- Copetti R, Cattarossi L. Ultrasound diagnosis of pneumonia in children. Radiol Medica. 2008;113(2):190-198. doi:10.1007/s11547-008-0247-8
- Clerkin KJ, Fried JA, Raikhelkar J, et al. Coronavirus Disease 2019 (COVID-19) and Cardiovascular Disease. Circulation. 2020;2019. doi:10.1161/CIRCULATIONAHA.120.046941
- Academico A, Paula U, Fernandes DO, Tecnico N, Lisboa TDE. Chest CT Findings in Cases from the Cruise Ship “Diamond Princess” with Coronavirus Disease 2019 (COVID-19) In. 2009;2019(0):0.
- Buonsenso D, Pata D, Chiaretti A. COVID-19 outbreak: less stethoscope, more ultrasound. Lancet Respir Med. 2020;2600(20):30120. doi:10.1016/S2213-2600(20)30120-X
- Soldati G, Smargiassi A, Inchingolo R, et al. Is there a role for lung ultrasound during the COVID-19 pandemic? J Ultrasound Med. 2020. doi:10.1002/jum.15284






3 thoughts on “Lung Ultrasound in COVID-19”
Pingback: Covid-19 Resources - General Ultrasound Resources - Zedu Ultrasound Training
Pingback: Zedu Ultrasound Training - Covid-19 POCUS Resources - General
Pingback: COVID-19 Ultrasound POCUS Resources | Zedu Ultrasound Training