Welcome back to the “52 in 52” series. This collection of posts features recently published must-know articles. This week we cover the ESETT trial which compares levetiracetam, fosphenytoin, and valproate for treatment of status epilepticus.

Author: Christiaan van Nispen, MD (Resident, Emergency Medicine Physician, San Antonio, TX); Brannon Inman, MD (Chief Resident, Emergency Medicine Physician, San Antonio, TX) // Reviewed by: Alex Koyfman, MD (@EMHighAK); Brit Long, MD (@long_brit)
Randomized Trial of Three Anticonvulsant Medications for Status Epilepticus
AKA: The “ESETT” Trial
Clinical question:
In patients with status epilepticus refractory to benzodiazepines, what is the comparative effectiveness of levetiracetam, fosphenytoin, and valproate?
Design: Multi-centered, double-blinded, randomized trial
PICO:
Population:
- Inclusion Criteria:
- Age 2 years and older
- Must have been treated with a specified minimum dose of certain benzodiazepines for generalized convulsive seizures:
- Intravenous or rectal diazepam 0.3 mg/kg or 10 mg
- Intravenous lorazepam 0.1 mg/kg or 4 mg
- Intravenous midazolam 0.2 mg/kg or 10 mg
- Intramuscular midazolam 0.3 mg/kg or 10 mg
- Seizures must persist for at least 5 minutes after administration of the prespecified benzodiazepines.
- Exclusion Criteria:
- Patients whose last dose of benzodiazepines was greater than 30 minutes prior to randomization
- Patients whose seizures were assessed to be due to hyperglycemia or hypoglycemia
- Patients whose seizures were associated with cardiac arrest
- Patients with known metabolic disorders
- Patients with liver disease
- Patients with severe renal disease
- Patients with major trauma
- Pregnant patients
- Prisoners
- Enrollment and Randomization:
- Enrollment occurred at 57 hospital emergency departments:
- 26 sites enrolled adults only
- 18 sites enrolled children only
- 13 sites enrolled both adults and children
- Both academic and community emergency departments were included amongst the sites.
- 400 enrollments (384 unique patients) occurred from November 3, 2015 to October 31, 2017; the second enrollment of those patients enrolled twice was not included in the intention-to-treat analysis but were included in the per-protocol analysis
- Baseline characteristics of enrolled population appeared similar, although perhaps not proportional to the U.S. population at large
- Enrollment was terminated at an interim analysis due to predefined futility criteria that suggested that there was a 1% chance that carrying the trial to completion would demonstrate a most effect or least effective treatment.
- Enrollment occurred at 57 hospital emergency departments:

Intervention:
- Patients were randomized to receive one of the following anti-convulsant medications:
- Intravenous levetiracetam 60 mg/kg (maximum 4500 mg) over 10 minutes
- Intravenous fosphenytoin 20 mg phenytoin equivalents/kg (maximum 1500 mg PE) over 10 minutes
- Intravenous valproate 40 mg/kg (maximum 3000 mg) over 10 minutes
Comparison:
- There was no placebo group; the three medications were compared to each other.
Outcome:
- No statistically significant difference in primary outcome, which was absence of clinically apparent seizures without the need for additional anti-convulsant medications AND improving responsiveness at 60 minutes after the start of trial-drug infusion, as determined by the treating physician.
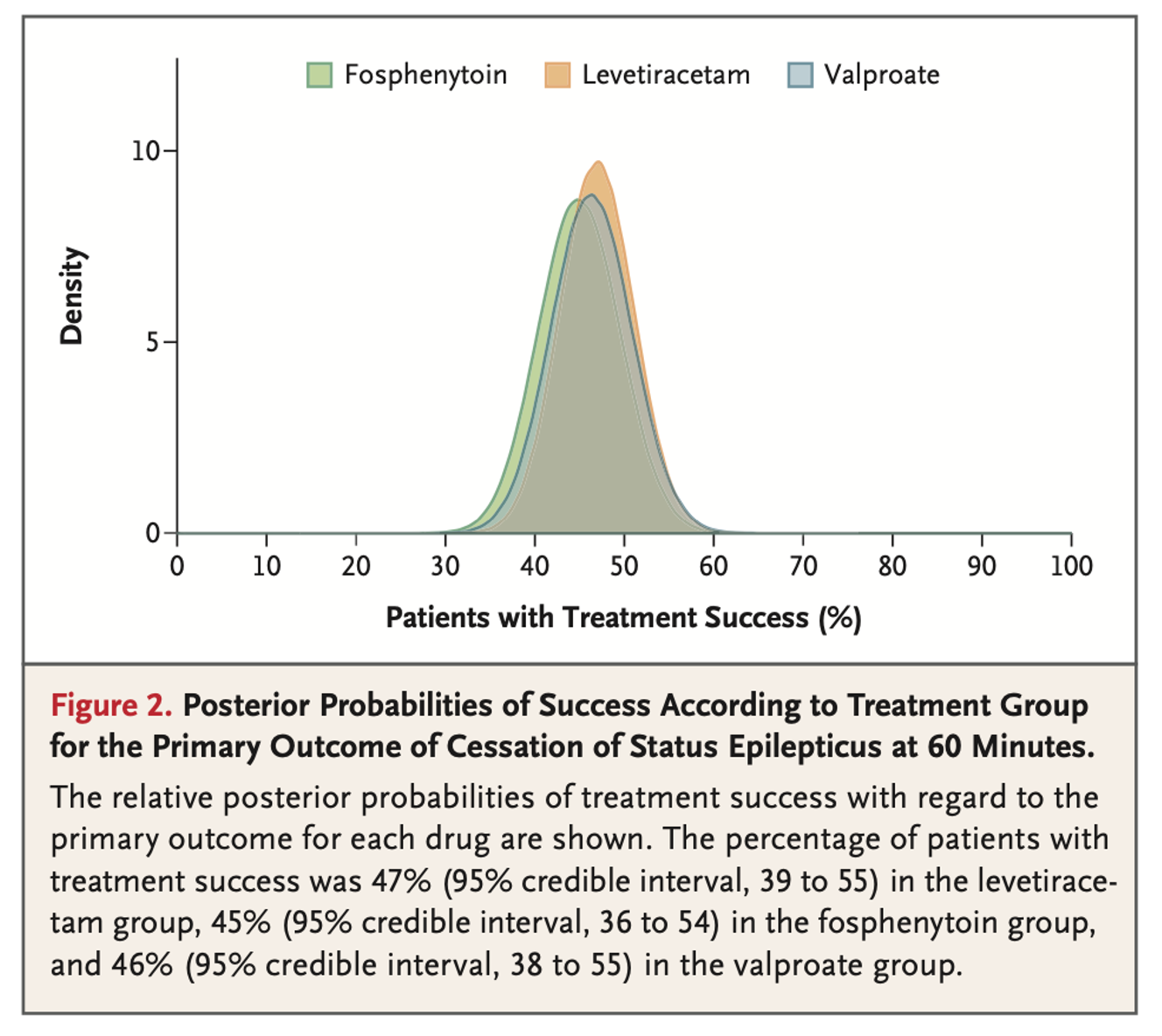
- Overall, nearly half of each group achieved the primary outcome:
- Levetiracetam 47%
- Fosphenytoin 45%
- Valproate 46%
- Amongst the patients not achieving the primary outcome:
- 144 required additional anti-convulsant medications
- 52 did not have improving responsiveness at 60 minutes
- Overall, nearly half of each group achieved the primary outcome:
- Secondary outcomes were not significantly different amongst the groups, including:
- Frequency of life-threatening hypotension
- Frequency of cardiac arrhythmia
- Need for subsequent endotracheal intubation
- Seizure recurrence 60 minutes to 12 hours after study drug infused
- Anaphylaxis
- Respiratory depression
- Purple glove syndrome
- Admission to the ICU
- Death
- 10% of the enrolled population was ultimately determined to have psychogenic non-epileptic seizures.
- There were many protocol violations that resulted in these patients being included in the intention-to-treat analysis, but excluded from the per-protocol analysis, including:
- Benzodiazepines administered too long before or two proximal to the administration of study drugs (50 patients)
- Benzodiazepine dose administered was below the specified study recommendations (26 patients)
- Enrollment of patients who were not in status epilepticus (33 patients)
- Unblinding of study drug to the clinical care team (200 patients), although most (154) were unblinded after the primary outcome had been determined at 60 minutes.

Take Aways:
- Negative trial: none of the anticonvulsants under investigation were determined to be superior or inferior to the others.
- Trial stopped early at preplanned interim analysis due to futility.
- Nearly half of all patients treated with the studied anti-convulsant medications had seizure resolution and improving mental state within 60 minutes.
- Study included children, as well as adults. This increases applicability or ED care.
- There were many protocol violations, and 10% of the studied population were not in status epilepticus. These factors in combination limit the conclusion of the study.
- About 200 of the 400 patients were ultimately unblinded.
My Take:
- Amongst patients presenting with status epilepticus refractory to benzodiazepine administration, the administration of levetiracetam (60 mg/kg, or 4500 mg), fosphenytoin (20 mg PE/kg, or 1500 mg PE/kg), and valproate (40 mg/kg, or 3000 mg) appear equally efficacious. In light of these data, I will give levetiracetam due to its less severe side effects and ease of administration.
Editor Note:
The key to status epilepticus is to stop the seizure. Give the first benzodiazepine and have the second dose ready while ordering the antiepileptic (we prefer levetiracetam at 60 mg/kg), but ready your sedative and paralytic for endotracheal intubation. If the adult patient has failed to stop seizing with two doses of benzodiazepines, rapid control of the seizure with either high dose propofol or ketamine can result in seizure cessation.
Reference:
- Kapur J, Elm J, Chamberlain JM, et al. Randomized Trial of Three Anticonvulsant Medications for Status Epilepticus. N Engl J Med. 2019; 381(22): 2103-2113. DOI: 10.1056/NEJMoa1905795






1 thought on “52 in 52 – #36: Randomized Trial of Three Anticonvulsant Medications for Status Epilepticus”
Pingback: LITFL Update 011 • LITFL • Newsletter