Authors: Brannon Inman (Resident Emergency Medicine Physician, San Antonio, TX) and Lloyd Tannenbaum (Staff Emergency Medicine Physician, San Antonio, TX) // Reviewed by: Bryant Allen, MD, FACEP, FAAEM (Associate Professor, Assistant Residency Program Director, Carolinas Medical Center, Department of Emergency Medicine); Alex Koyfman, MD (@EMHighAK); Brit Long, MD (@long_brit)
Case:
A 35-year-old man with a history of depression who was recently started on trazadone presents to the local emergency department with a persistent, painful erection. He is uncertain when the erection started, as he awoke in this state this morning but states the condition has been present for at least 4 hours. He has no history of sickle cell disease, HIV, recent medication changes, use of nitrates, or use of erectile dysfunction medications. He denies history of malignancy and is not under treatment for any other chronic conditions. He denies any trauma to the perineum or saddle-type injury and endorses a significant amount of pain and distress.
The diagnosis:
Priapism, likely ischemic given the medication history (trazadone) and the presence of pain. To confirm, you could obtain a blood gas from the corpus cavernosum. The following chart helps to differentiate ischemic and high-flow priapism:1,2
Table 1: Blood gas comparison for Ischemic/Low-flow and Non-Ischemic/ High- Flow priapism, Adapted from AUA guideline statement

Ischemic priapism is tantamount to compartment syndrome of the penis and requires treatment with the same degree of urgency.3 Treatment, according to the American Urological Association Priapism Guidelines, should occur in a stepwise fashion until detumescence is achieved.3
Treatment involves first aspirating blood from the corpus cavernosum.
Typically, the procedure is performed in the following fashion
- Perform nerve block
- Use 18 g needle to aspirate blood from the corpus cavernosum
- Change syringes with an unstable needle in the corpus cavernosum and irrigate
- Repeat process a required number of times
- Remove the needle and repeat on the other side
- If unsuccessful stab the penis again to inject phenylephrine
This results in a significant number of needle insertions. Also, leaving the sharp tip 18 g needle in the corpus cavernosum can be anxiety-provoking.
There is an adapted method using an angio-catheter, some IV tubing, a 3-way stop cock, and two syringes to irrigate blood more effectively from the corpus cavernosum. This is known as the “Stop-Cock” method.
What you will need:
- An 18g IV angio-catheter needle
- A section of short IV tubing with a connecter
- A 3-way stopcock
- Two 10 cc syringes
- Sterile saline
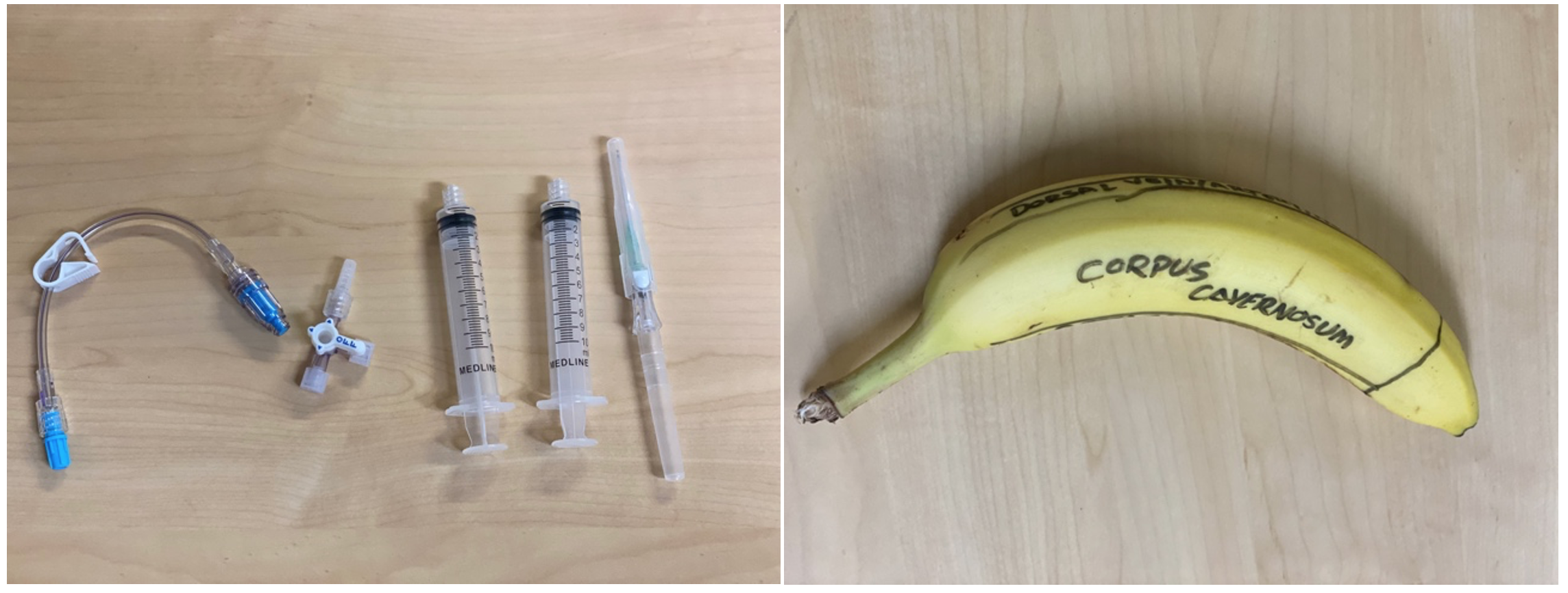
Figure 1: Necessary materials for the described technique
First, disconnect the luer lock from the IV tubing and connect the 3-way stopcock
Figure 2: Disconnection of luer lock and IV tubing cap
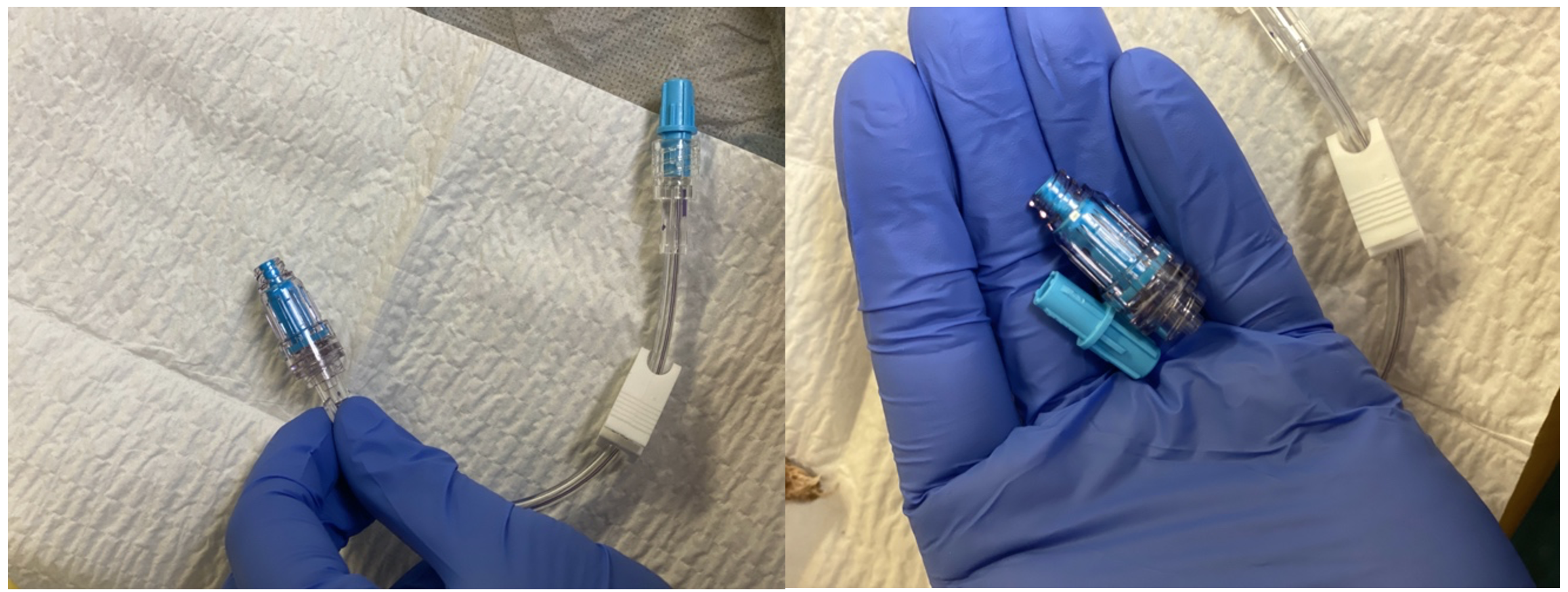
Figure 3: Connection of 3-way stopcock

Second, position the patient (after nerve block and analgesia) and insert the 18g IV needle at the 10 o’clock position into the corpus cavernosum, then remove the needle leaving the angiocath.
Figure 4: Insertion of 18g IV needle, avoiding dorsally located vein artery and nerve and inferiorly located urethra
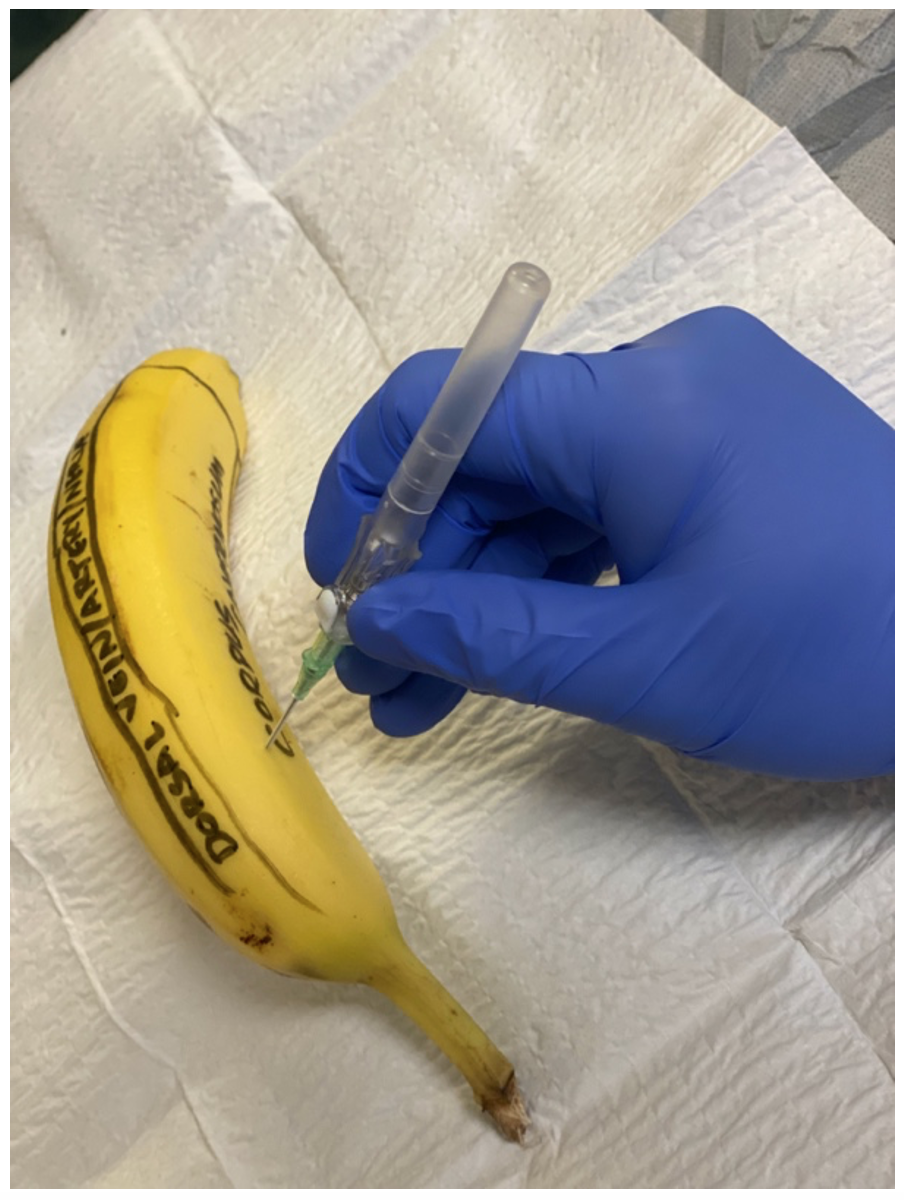
Next, connect the IV tubbing to the angiocath, and connect a saline-filled syringe and an empty syringe.
Figure 5: Connection of IV tubing
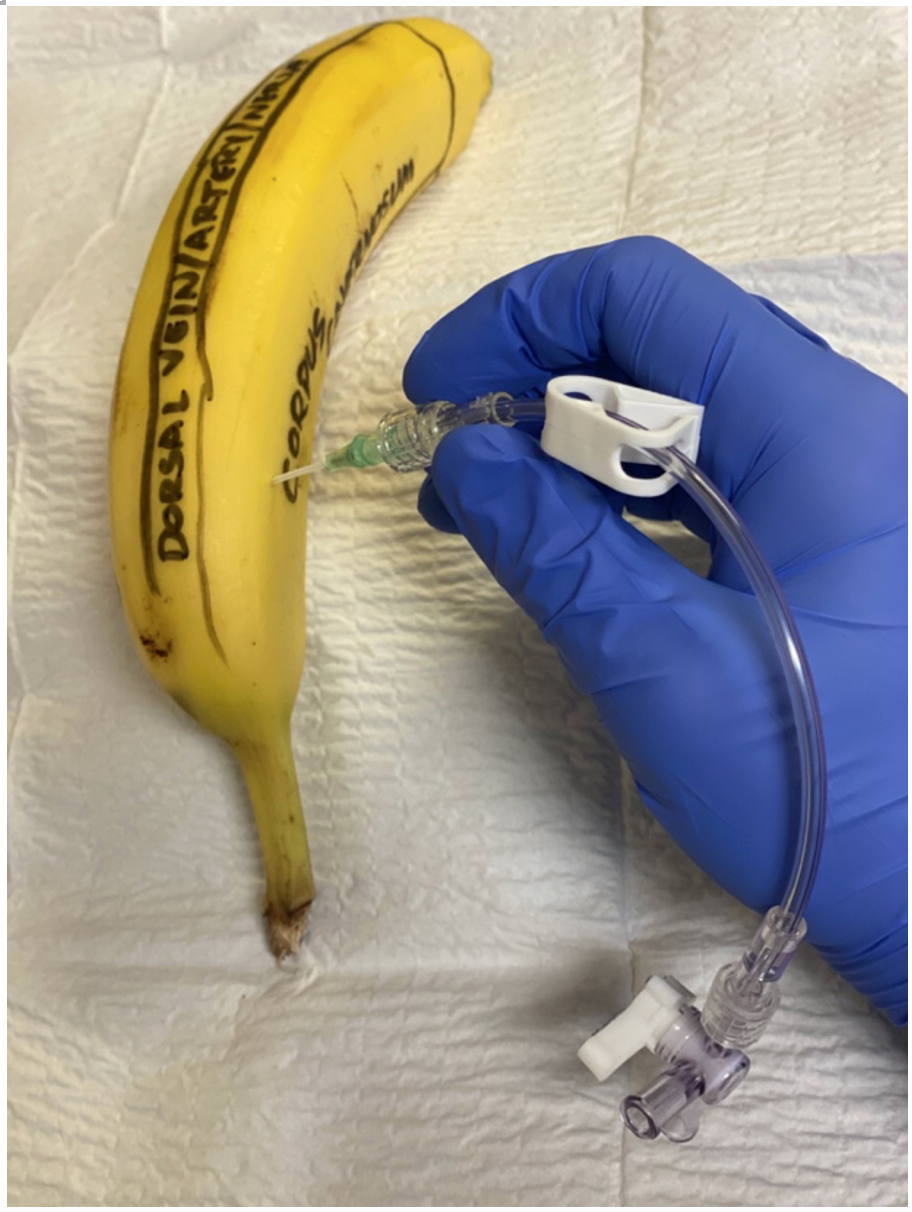
Figure 6: Image showing saline-filled syringe and empty syringe with 3-way stopcock flange off to saline-filled syringe
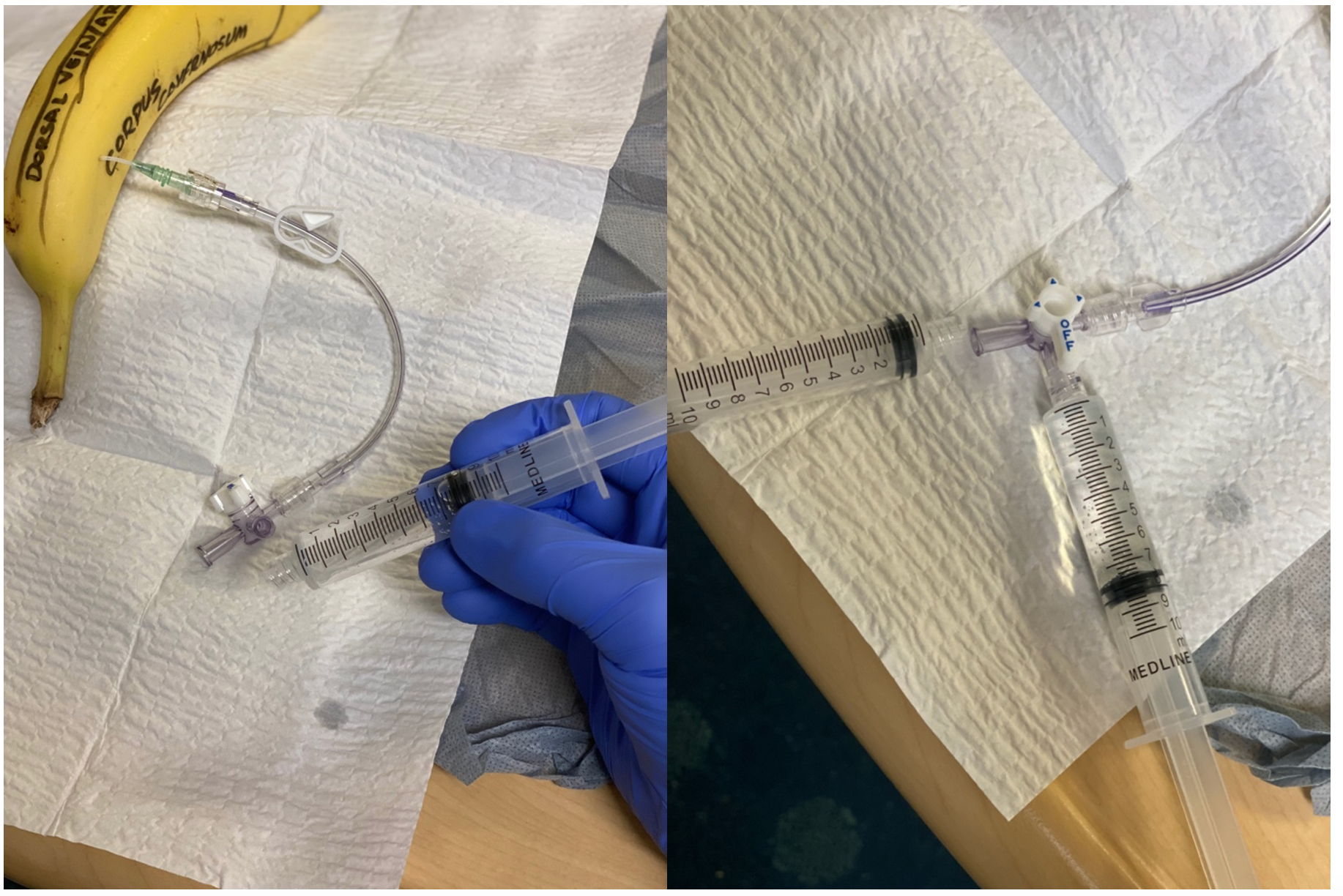
After you have connected the IV tubing to a saline-filled syringe and an empty syringe, turn the flange on the 3-way stopcock off to the saline-filled syringe. Then, pull back on the plunger on the empty syringe to aspirate blood from the corpus cavernosum.
Figure 7: Aspiration of blood (represented in this model by Mountain Dew) from the corpus cavernosum
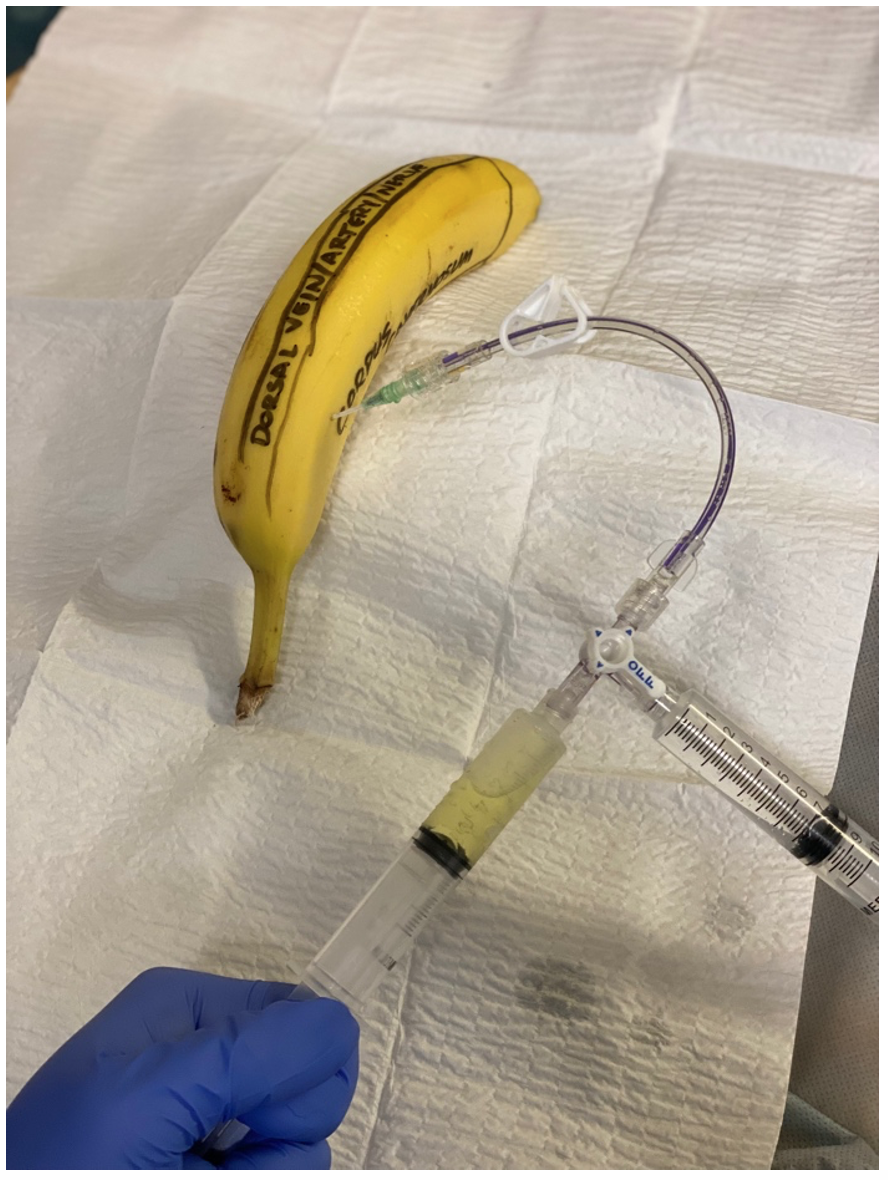
After aspiration you will likely reach a point where blood is no longer easily aspirated. This is likely due to coagulated blood in the compartment. This is where irrigation becomes helpful. Turn the flange to be in the off direction to the blood-filled syringe and press down on the plunger of the saline-filled syringe.
Figure 8: Irrigation of the corpus cavernosum
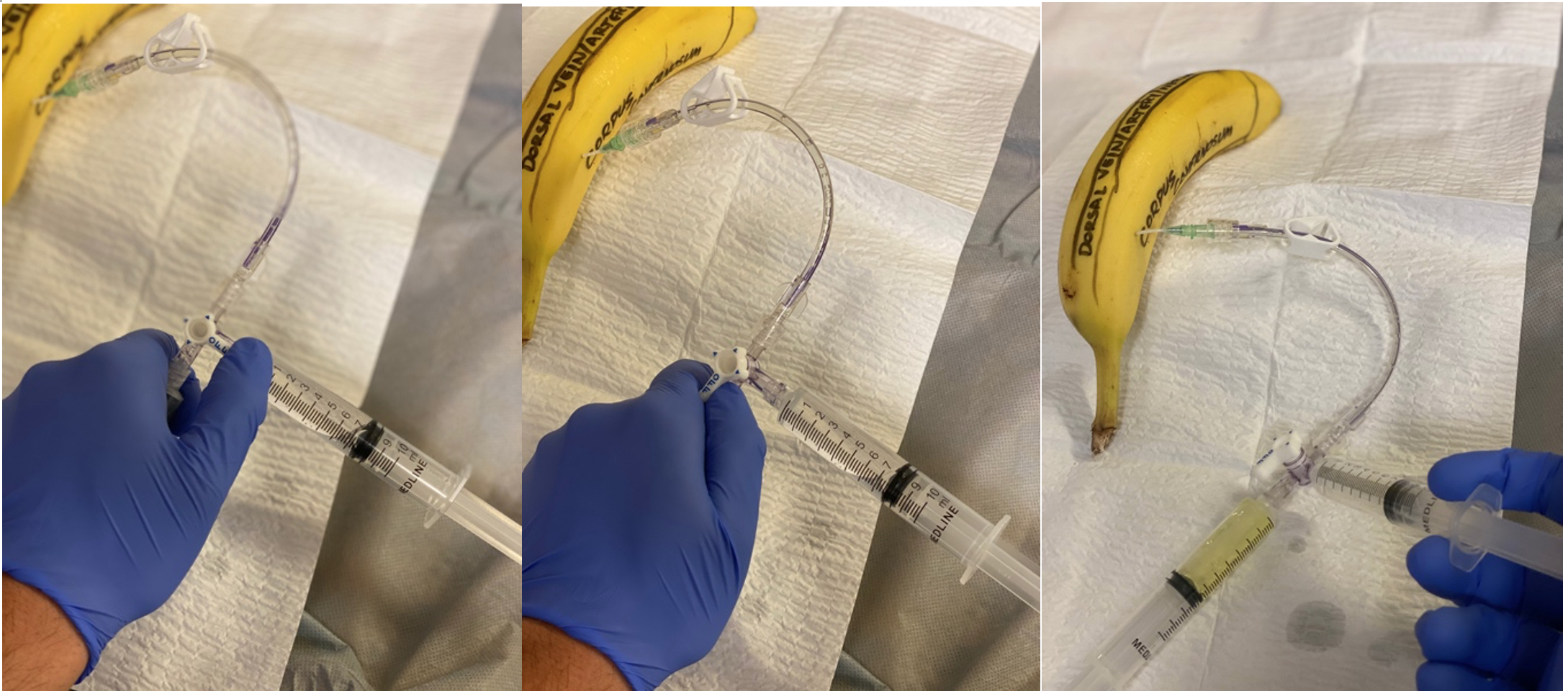
If after irrigation and aspiration detumescence is not achieved the next recommended step is the injection of a vasoactive agent. In theory, repeat aspiration and irrigation on the contralateral side should not be necessary as the two sides are connected. However, if the patient has remained erect for a prolonged time coagulated blood may inhibit the communication between the two sides. If repeat aspiration is performed on the contralateral side, leave the angiocath in the corpus cavernosum, disconnect the tubing, and repeat the process on the contralateral side.
With an angiocath in either side, you could apply a slight degree of compression to further aid in the reduction of cavernosal blood.
AUA guidelines strongly recommend the use of a vasoactive agent.3 Therefore following aspiration the next step is the intracavernosal injection of a vasoactive agent. By leaving the angiocath in the corpus cavernosum, you can easily deliver phenylephrine without the need for additional needles.
The recommended vasoactive agent is phenylephrine, as it is a pure alpha agonist and less prone to other systemic sympathomimetic effects.1,3 Phenylephrine typically comes in a 10 mg/mL concentration. There are a few ways to dilute phenylephrine to the desired concentration of 100 micrograms/mL. One way is to take the entire 10mg and inject it into a 100 mL bag of normal saline, shake well, and withdrawal 10 mL of the now 100 micrograms/mL solution (Figure 9). Serial dilution may also be performed. To serially dilute take a 10 mL saline flush and waste 1 mL and draw up the 10 mg of phenylephrine resulting in 1 mg/mL phenylephrine. Repeat this process once more and the result is 100 micrograms/mL phenylephrine (Figure 10).
Figure 9: Making 100 mcg/mL phenylephrine using 100 mL bag normal saline
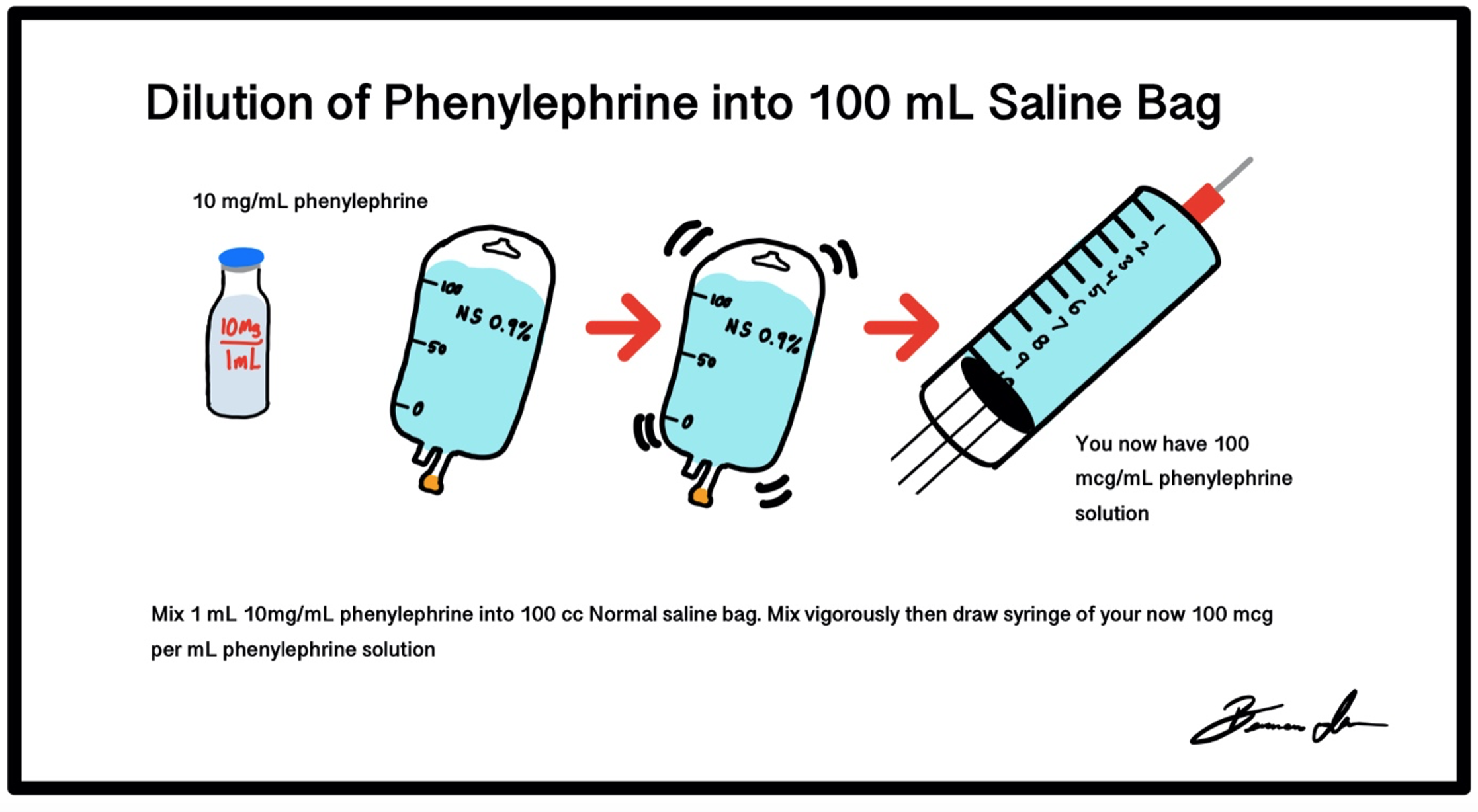
Figure 10: Serial Dilution technique for phenylephrine
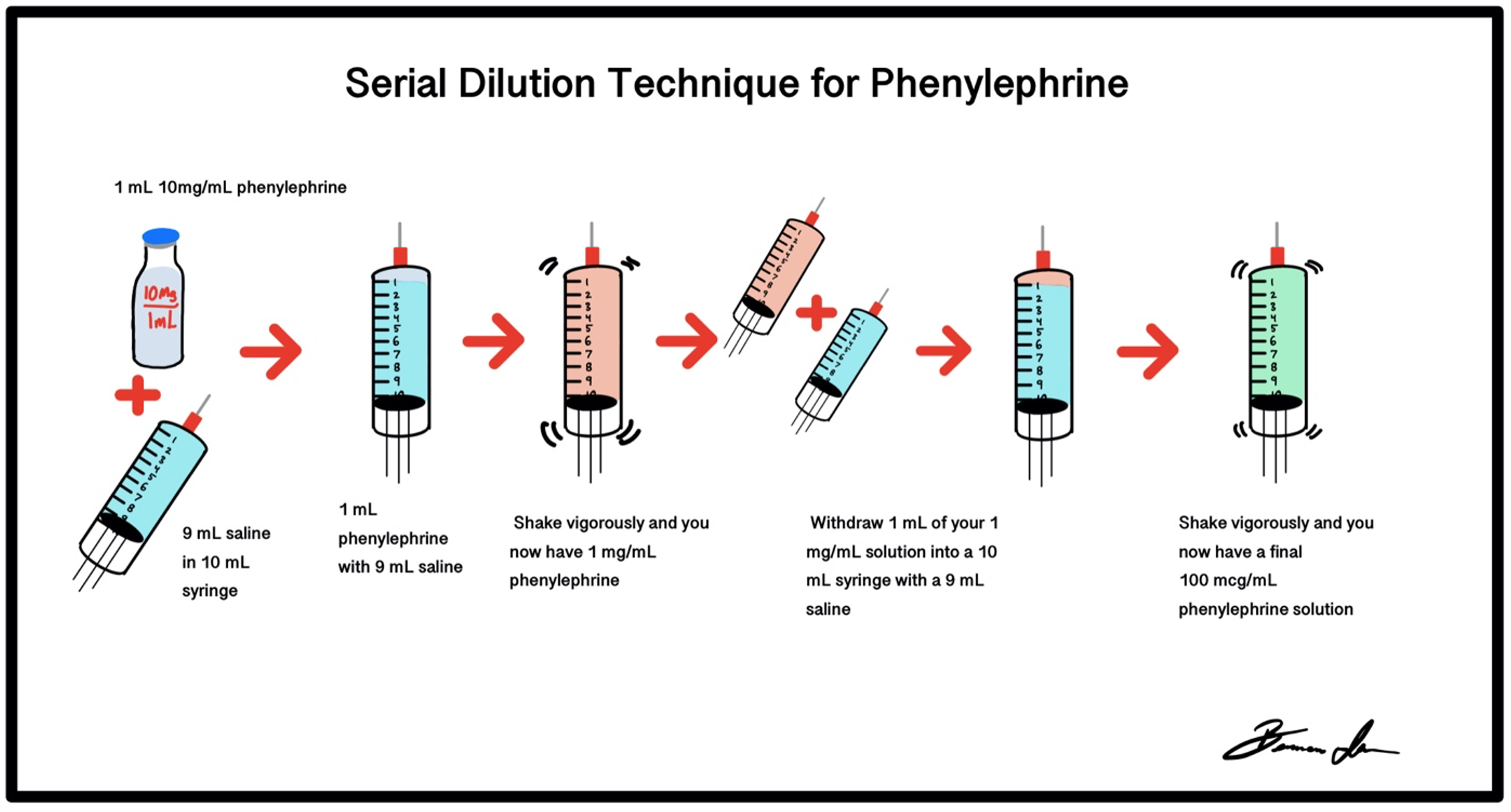
Figure 11: Disconnection of IV tubing and injection of phenylephrine
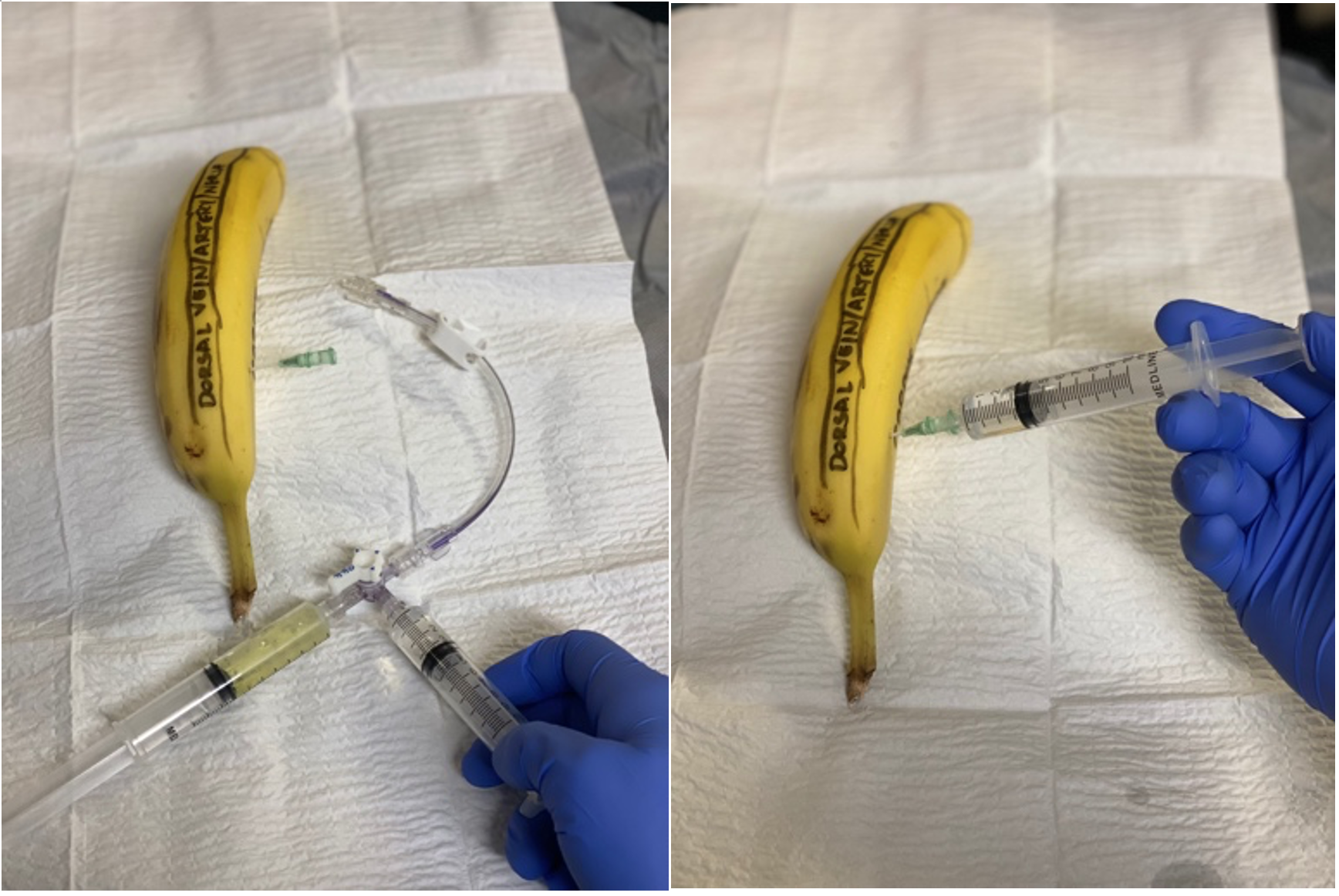
Per AUA guidelines 1 mL of 100 micrograms/mL phenylephrine should be injected every 3-5 minutes for one hour before declaring treatment failure. This sounds aggressive. However, the next line of therapy is a surgical fistula/shunt between the corpus cavernosum and the corpus spongiosum, glans, or a penile vein. This procedure rarely results in the preservation of erectile function. In fact, in one study preservation of normal erectile function following treatment of priapism was 66% for those that underwent aspiration, and 18 – 20% for those who underwent surgical shunting.4 The degree of erectile dysfunction is so high some experts actually recommend a penile implant be performed at the same time for this reason.1–3
Case resolution:
After aspiration and irrigation of the corpus cavernosum, you fail to achieve adequate detumescence. You repeat the process of irrigation and aspiration on the contralateral side, followed by infusion of 100 mcg/mL phenylephrine via a retained angio-catheter. After an injection of approximately 800 mcg of phenylephrine over 45 minutes the patient achieves detumescence and is discharged to urology follow up.
Key takeaways:
- Priapism is most commonly low-flow/ischemic in origin.
- Ischemic priapism is a compartment syndrome of the penis and is a urologic emergency
- Treatment of priapism should follow a step wise approach
- You can use standard ED supplies to easily aspirate and irrigate the corpus cavernosum
- Don’t be afraid to be aggressive with non-surgical treatment in the ED, because the surgical options are quite morbid
References:
- Priapism – UpToDate. Accessed September 3, 2021. https://www.uptodate.com/contents/priapism?search=priapism%20blood%20gas&source=search_result&selectedTitle=1~150&usage_type=default&display_rank=1#H9
- emDOCs.net – Emergency Medicine Education Priapism in the ED: Pearls & Pitfalls – emDOCs.net – Emergency Medicine Education. Accessed September 3, 2021. http://www.emdocs.net/priapism-ed-pearls-pitfalls/
- Priapism Guideline – 2010 American Urological Association. Accessed September 3, 2021. https://www.auanet.org/guidelines/guidelines/priapism-guideline
- Pal DK, Biswal DK, Ghosh B. Outcome and erectile function following treatment of priapism: An institutional experience. Urology Annals. 2016;8(1):46. doi:10.4103/0974-7796.165717






