Author: Wells Weymouth, MD (Resident Physician, SAUSHEC, USA) and Erica Simon, DO, MHA (@E_M_Simon, EMS Fellow, SAUSHEC, USAF) // Edited by: Alex Koyfman, MD (@EMHighAK, EM Attending Physician, UTSW / Parkland Memorial Hospital) and Brit Long, MD (@long_brit, EM Attending Physician, SAUSHEC, USAF)
Welcome to EM@3AM, an emdocs series designed to foster your working knowledge by providing an expedited review of clinical basics. We’ll keep it short, while you keep that EM brain sharp.
A 22-year-old male, seen in the ED 5 days prior (diagnosis: corneal abrasion), presents for a second visit due to persistent left eye pain and redness. The young man, a soft contact lens wearer, reports non-compliance with the discharge instructions to remove and replace his contact lenses. Since resuming contact lens wear, the patient notes severe left eye pain, increased redness, and profound light sensitivity. The man denies fever, known ocular trauma, and sick contacts.
Triage VS: BP 128/81, HR 122, T 99.6 F oral, RR 12, SpO2 99% on room air.
OD: 20/20
OS: 20/70
OU: 20/40
Pertinent physical examination findings:
HEENT: PERRLA, 3 mm bilaterally; EOMI, visual fields intact. OS: Severe conjunctival injection and hyperemia, diffuse corneal haze, small hypopion. No FB on lid eversion.
Examination with Fluorescein:
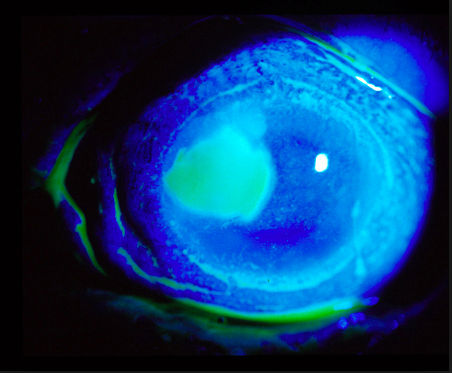
What’s the next step in your evaluation and treatment?
Answer: Corneal Ulcer1-7
- Epidemiology: Commonly the result of contact lens wear or traumatic lesions that become secondarily infected.1,2
- Pathogens: Pseudomonas aeruginosa, Staphylococcus species, Streptococcocus species, and Mycobacterium are frequently associated with contact lens wear. Infection caused by viral pathogens (Herpes simplex/Herpes zoster) often results in ulceration. Fungal infection/ulceration (Aspergillus, etc.) may occur in the immunosuppressed, those utilizing corticosteroid drops, or in agricultural workers (ocular contamination with vegetative material). Acanthamoeba infection/ulceration frequently occurs in the developing world.2,3 Suspect Neisseria gonorrhoeae in patients with new sexual partners and rapidly developing symptoms (< 24 hours).1
- Clinical Manifestations: Patients may report eye pain and redness, light sensitivity, blurred or hazy vision +/- discharge and foreign body sensation.3
- Evaluation, Treatment, and Disposition:2-5
- Assess the ABCs and obtain VS.
- Perform a thorough H&P:
- Question specifically regarding duration of symptoms, new sexual contacts, contact lens use, and previous Herpes simplex/zoster infection.
- Perform a thorough ocular examination:
- HEENT: Herpes zoster: dermatomal rash (CNV1) of the upper forehead/eyelid +/- the nose (nasociliary nerve; Hutchinson’s sign), +/- local Horner’s syndrome.5
- Slit lamp exam with fluorescein staining:5
- “Heaped up edges” with stromal edema and infiltrate.
- Herpes simplex: dendritic lesions, punctate epithelial erosions, stromal whitening, thinning of the cornea.
- Herpes zoster: pseudodentritic lesions more commonly associated with iritis, uveitis, and choroiditis.
- Treatment:5-7
- Consult ophthalmology => ocular emergency.
- Suspected bacterial etiology:
- Discuss initiation of topical vs. systemic antibiotic therapy.
- Floroquinolones = good ocular penetration.
- Discuss initiation of steroids (decrease inflammation).
- Discuss cycloplegic agents (i.e. homatropine or cyclopentolate => minimize ciliary spasm and produce mydriasis = reduce pain and prevent synechiae formation).1
- Discuss initiation of topical vs. systemic antibiotic therapy.
- Suspected viral etiology:
- Herpes simplex: Discuss initiation of topical vs. systemic antivirals.
- Topical trifluridine vs. oral acyclovir or valacyclovir.
- Herpes zoster: systemic antiviral therapy is the standard of care.5
- Prophylactic erythromycin ointment is recommended in the setting of presumed viral etiology.
- A cycloplegic may be considered if signs of iritis.
- Herpes simplex: Discuss initiation of topical vs. systemic antivirals.
- Disposition:
- Discuss with specialist: If discharge, recommend close ophthalmology follow-up (repeat evaluation within 24 hours).5
- Pearls:
- Unexplained corneal ulcers in pediatric patients => suspect vitamin deficiency (Cystic Fibrosis), metabolic disorder (tyrosinemia), or sensory disorder (neurotrophic keratitis).1
References:
- Olitsky, S., Hug D., Plummer, E., Stahl, E., Ariss M., and Lindquist, T. (2016). Abnormalities of the Cornea. Nelson Textbook of Pediatrics. 627, 3041-3044.e1.
- Garg, P., Rao, B. (1999). Corneal Ulcer: Diagnosis and Management. Community Eye Health, 12(30), 21-23.
- Gangopadhyay, N., Daniell, M., Weih, L., & Taylor, H. R. (2000). Fluoroquinolone and fortified antibiotics for treating bacterial corneal ulcers. British journal of ophthalmology, 84(4), 378-384.
- Stern, G. A., & Zam, Z. S. (1986). The Pathogenesis of Contact Lens-Associated Pseudomonas aeruginosa Corneal Ulceration I. The Effect of Contact Lens Coatings on Adherence of Pseudomonas aeruginosa to Soft Contact Lenses. Cornea, 5(1), 41-46.
- Guluma, K., and Lee, J. Ophthalmology. (2018). Rosen’s Emergency Medicine: Concepts and Clinical Practice, 61, 790-819.e3.
- McLeod, S. D., LaBree, L. D., Tayyanipour, R., Flowers, C. W., Lee, P. P., & McDonnell, P. J. (1995). The importance of initial management in the treatment of severe infectious corneal ulcers. Ophthalmology, 102(12), 1943-1948.
- Hoddenbach, J. G., Boekhoorn, S. S., Wubbels, R., Vreugdenhil, W., Van Rooij, J., & Geerards, A. J. (2014). Clinical presentation and morbidity of contact lens–associated microbial keratitis: a retrospective study. Graefe’s Archive for Clinical and Experimental Ophthalmology, 252(2), 299-306.
For Additional Reading:
Acute Visual Loss in the Emergency Department: Pearls and Pitfalls:
Acute Visual Loss in the Emergency Department: Pearls and Pitfalls