Author: Brit Long, MD (@long_brit, EM Attending Physician, San Antonio, TX) // Reviewed by: Alex Koyfman, MD (@EMHighAK, EM Attending Physician, UTSW / Parkland Memorial Hospital)
Welcome to EM@3AM, an emDocs series designed to foster your working knowledge by providing an expedited review of clinical basics. We’ll keep it short, while you keep that EM brain sharp.
A 42-year-old male presents with headache, fever, chills, nausea, and myalgias. He denies cough, shortness of breath, vomiting, diarrhea, and neck stiffness, but states he returned from a month-long trip to Africa several weeks ago.
On examination, he is tachycardic and febrile. You do not find a rash or meningismus, but you palpate an enlarged spleen and liver.
What is your next step in evaluation and management?
Answer: Malaria
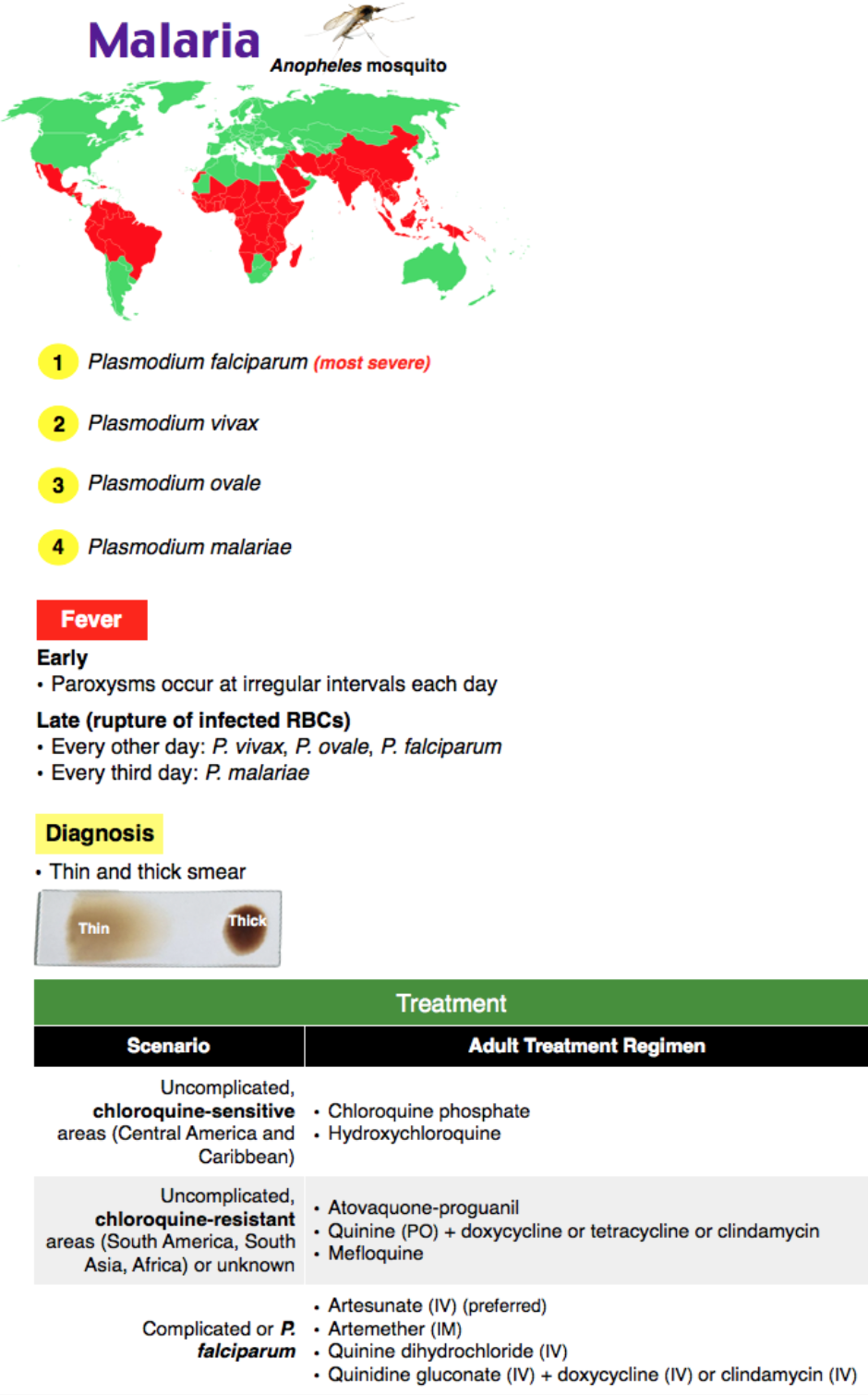
Background: Malaria is an infection due to Plasmodium species (P. ovale, P. vivax, P. malariae, P. knowlesi, P. falciparum), a parasitic protozoa spread by the Anopheles mosquito which bites at night.
- P. falciparum is the most deadly form and is often resistant to chloroquine.
- P. falciparum has higher levels of parasitemia (this species infects RBCs of all ages) compared to other species and has a banana-shaped gametocyte.
- P. vivax and ovale can persist in the liver for months in their hypnozoite form.
- P. knowlesi should be suspected in patients from Southeast Asia.
- Many endemic areas, including Africa, Southeast Asia, Middle East, and South America. See CDC for more.
- Sub-Saharan Africa has highest rates of P. falciparum for U.S. travelers.
- 300-500 million cases annually, with 1-3 million deaths per year (most deaths occur in those < 5 years in rural sub-Saharan Africa).
- 10,000-30,000 new cases each year among U.S. and European travelers.
- In the U.S., most likely will occur in travelers, even for short time periods.
- Chemoprophylaxis does not prevent infection for all patients.
- 5-7% of patients are infected with multiple species.
- Pregnant women are 10X more likely to contract malaria.
- Outcome of infection depends on host immunity. Those with immunity can spontaneously clear malaria, but in those without, the parasites reproduce.
Precautions for Travelers:
- Use chemoprophylaxis: doxycycline, atovaquone/proguanil, and others (depends on location).
- Use insecticide-treated bed nets, DEET insect repellants, long-sleeve shirts and pants.
- Limit dawn and dusk exposure.
- A vaccine is available, which can reduce malaria episodes by 40%.
History:
- Assess current symptoms: fevers, headache, malaise, chills, myalgias, GI complaints, neck stiffness, PO intake, rash, urine changes (dark urine, amount), cough, dyspnea.
- Past medical history, prior infections, immunosuppression (diabetes, HIV, etc.), pregnancy, allergies.
- Travel: locations, dates, season, reason, transportation.
- Exposure: local water, street food, meat, animal/insect exposures and bites, freshwater activities, sick contacts, body fluid or blood exposures, sexual encounters.
- Prophylaxis: Malaria and otherwise.
Examination:
- Vital signs, HEENT, neurologic exam, mental status, meningismus, skin (rash, petechiae, jaundice), abdomen (hepatosplenomegaly), lymphadenopathy, CV, respiratory.
Malaria Presentation:
- Incubation period for malaria typically ranges from 8-25 days, but it may be up to 1 year.
- Classic Triad: Fever, splenomegaly, thrombocytopenia. However, this is not specific or sensitive.
- Headache, cough, chills, fatigue, nausea/vomiting, diarrhea, myalgias, joint pain common.
- Fever present in 90% of patients, may occur every 2-3 days or continuously.
- Patients may have paroxysms of fever, sweats, chills every 48-72 hours, but this depends on the species. Do not use the absence of these paroxysms to exclude the diagnosis of malaria.
- Hemoglobinuria (blackwater fever) with dark urine suggests impending renal failure.
- Splenomegaly +LR 6.5, fever +LR 5.1, jaundice/icterus +LR 4.5, pallor +LR 2.8, hepatomegaly +LR 2.4, vomiting +LR 2.0 for malaria.
Differential Diagnosis: Sepsis, encephalitis, meningitis, pneumonia, endocarditis, dengue, typhoid fever, typhus, chikungunya, yellow fever, viral hemorrhagic fever, typhus, Q fever, amebiasis, zika virus, acute HIV, rheumatologic disease.
Laboratory testing:
- CBC with differential, glucose, renal function, electrolytes, liver function with bilirubin, thick and thin smears, LP for CSF if concern for cerebral malaria/meningitis present, dengue serology, LDH and haptoglobin (assess hemolysis) blood cultures X2, lactate, coagulation panel + fibrinogen (evaluate for DIC).
- Thrombocytopenia, atypical lymphocytes, and elevated LDH suggest malaria.
- Leukocytosis in malaria is uncommon (< 5%).
- HIV testing in select cases (those with high risk of HIV).
- Chest radiograph if respiratory symptoms present.
- CT head if the patient is altered or displays signs of meningitis.
- Hyperbilirubinemia associated with +LR of 7.3, thrombocytopenia +LR of 5.6 for malaria.
Diagnosis:
- Consult infectious disease specialist if suspecting malaria.
- Malaria Hotline for Healthcare Providers
- Via telephone: 1-770-488-7788 or 1-855-856-4713 (toll free)
- Via telephone (after hours): 1-770-488-7100
- Diagnosis classically includes thick (sensitive and determines whether malaria is present) and thin smears (identifies species). Need 3 negative smears at least 12 hours apart to rule out malaria.
- The first smear is negative in over 10% of patients. Do not rely on a single smear to rule out malaria.
- Assess parasite load (> 5% = severe).
- PCR assay is specific and sensitive for determining the presence of Plasmodium but may not be available in all settings.
- Nucleic acid sequence-based amplification (NASBA) is also available and is more sensitive than thick smears.
- Rapid diagnostic tests (RDT) include immunochromatographic testing. These can perform better than microscopy, but they are less effective for parasite levels < 100 parasites/mL of blood. If positive, this test should be confirmed with a second type of test.
Treatment:
- Discuss with infectious disease specialist.
- All cases require reporting, as malaria is a notifiable disease.
- Provide symptomatic therapy, including acetaminophen and/or NSAIDs.
- For P. falciparum or severe malaria, parenteral artesunate or quinidine (or quinine) therapy is recommended:
- Artesunate (while not available in all ED’s, this is more effective). Literature suggests improved survival using this medication.
OR
- Quinidine + doxycycline, clindamycin, or pyrimethamine-sulfadoxine.
- Quinidine can be cardiotoxic, resulting in ventricular dysrhythmia, QT prolongation, hypotension.
- For uncomplicated malaria, may use artemether + lumefantrine, artesunate + amodiaquine or mefloquine, dihydroartemisinin + piperaquine, or artesunate + sulfadoxine-pyrimethamine.
- Avoid sulfadoxine-pyrimethamine in HIV/AIDs patients on cotrimoxazole, and avoid amodiaquine in those on efavirenz or zidovudine.
- Chloroquine can be utilized for those with chloroquine sensitive species.
- P. vivax and ovale infections can be treated with chloroquine plus primaquine. Chloroquine alone can treat P. malariae.
- A new medication is tafenoquine, primarily used for vivax.
- Treat P. knowlesi the same as P. falciparum.
- Many of these antimalarials are safe for pregnant women (first line include mefloquine, artemether-lumefantrine, or quinine + clindamycin).
- Provide antibiotics covering meningitis if clinical picture is suggestive.
- Treat complications. Administer dextrose for hypoglycemia.
- Exchange transfusion should be considered for those with parasite load > 10% or life-threatening complications.
Severe Malaria: Medical emergency!
- Patients may have end organ damage and dysfunction, anemia, electrolyte abnormalities, hemoglobinuria, hypoglycemia, cerebral edema (AMS, seizure coma.).
- Complications include seizures, shock, renal failure, ARDS, DIC/spontaneous bleeding.
- Infection with P. falciparum or knowlesi is typically severe.
- Initiate antimalarial therapy for these patients while waiting results (ie, IV artesunate).
Disposition:
- Most patients with suspected malaria, especially P. falciparum, should be admitted.
- Admit patients with severe malaria, cerebral malaria, pregnant or pediatric patients; these populations typically require higher level care (ICU).
- Patients with non-P. falciparum may be appropriate for outpatient therapy if otherwise non-toxic and well-appearing, diagnosis is confirmed, PO tolerant, and no other significant comorbidities.
Key Points:
- Malaria is caused by Plasmodium species spread by the Anopheles mosquito. P. falciparum is the most severe species.
- Obtain a full travel history and ask about prophylaxis.
- Do not use absence of paroxysms or fever to exclude malaria. Most patients will have fever.
- The classic triad includes fever, splenomegaly, and thrombocytopenia, but do not use its absence to exclude the diagnosis.
- Obtain 3 separate thick and thin smears separated by at least 12 hours. If available, use PCR or RDT testing. Do not use a single negative smear to exclude malaria.
- Consult infectious disease specialist if considering malaria.
- Malaria Hotline for Healthcare Providers
- Via telephone: 1-770-488-7788 or 1-855-856-4713 (toll free)
- Via telephone (after hours): 1-770-488-7100
For more on malaria, see these great pieces from Dr. Katy Hanson at www.hansonsanatomy.com




A 40-year-old man presents to the emergency department with a fever two weeks after traveling from Nigeria. On initial evaluation, he has a generalized tonic-clonic seizure. Vital signs are BP 90/60, HR 110, RR 22, oxygen saturation 92% on room air, and T 102°F. Which of the following organisms is most likely to be found on peripheral blood smear?
A) Plasmodium falciparum
B) Plasmodium malariae
C) Plasmodium ovale
D) Plasmodium vivax
Answer: A
Malaria is a mosquito-borne parasitic infection caused by Plasmodium vivax, Plasmodium ovale, Plasmodium malariae, Plasmodium knowlesi, and Plasmodium falciparum. The most virulent Plasmodium species is Plasmodium falciparum. Malaria should be suspected in any patient with a fever who has traveled to endemic areas such as South America, Asia, and Africa. Transmission occurs through a bite from an Anopheles mosquito followed by an incubation period of 12 to 35 days before the onset of symptoms. At the end of the incubation period, infected red blood cells rupture, leading to the clinical signs and symptoms. Symptoms of malaria are often nonspecific and include fever, myalgias, cough, nausea, vomiting, abdominal pain, and diarrhea. The clinical manifestations of severe malaria are the result of infected red blood cells adhering to small blood vessels, causing small infarcts, capillary leakage, and organ dysfunction. The signs and symptoms of severe malaria include altered mental status, seizures, acute respiratory distress syndrome, hypotension, metabolic acidosis, renal failure, hepatic failure, coagulopathy, severe anemia, and hypoglycemia. The most severe and complicated forms of malaria are usually due to Plasmodium falciparum. The diagnosis of malaria is made using a thick and thin blood smear. Treatment of severe malaria involves antimalarial therapy with artesunate, quinine, or quinidine.
Plasmodium malariae (B), Plasmodium ovale (C), and Plasmodium vivax (D) are much less virulent species and are unlikely to lead to severe malaria. Initially, all species may present with similar clinical features, but patients with central nervous system signs and symptoms are more likely to be infected with Plasmodium falciparum.
Further Reading:
FOAMed
Emergency Medicine Cases – Fever in the Returning Traveler
Emergency Medicine Cases – Malaria Video
LIFTL – CCC Malaria
LIFTL – Cases Extravaganza
LIFTL – Malaria Vaccine
WikEM – Malaria
References
1. WHO – Guidelines for the treatment of malaria
2. WHO – Management of Severe Malaria
3. CDC – malaria
4. Taylor SM, Molyneux ME, Simel DL, Meshnick SR, Juliano JJ. Does this patient have malaria? JAMA. 2010 Nov 10;304(18):2048-56. Epub 2010 Nov 5. Review.
5. Rapid diagnostic tests for malaria —Haiti, 2010. MMWR Morb Mortal Wkly Rep. 2010 Oct 29. 59(42):1372-3.
6. Wongsrichanalai C, Barcus MJ, Muth S, Sutamihardja A, Wernsdorfer WH. A review of malaria diagnostic tools: microscopy and rapid diagnostic test (RDT). Am J Trop Med Hyg. 2007 Dec. 77(6 Suppl):119-27.
7. Centers for Disease Control and Prevention. Notice to Readers: Malaria Rapid Diagnostic Test. Centers for Disease Control and Prevention. Available at http://www.cdc.gov/mmwr/preview/mmwrhtml/mm5627a4.htm.
8. de Oliveira AM, Skarbinski J, Ouma PO, et al. Performance of malaria rapid diagnostic tests as part of routine malaria case management in Kenya. Am J Trop Med Hyg. 2009 Mar. 80(3):470-4.
9. Polley SD, Gonzalez IJ, Mohamed D, et al. Clinical evaluation of a loop-mediated amplification kit for diagnosis of imported malaria. J Infect Dis. 2013 Aug. 208(4):637-44.
10. Sinclair D, Donegan S, Isba R, Lalloo DG. Artesunate versus quinine for treating severe malaria. Cochrane Database Syst Rev. 2012;6:CD005967.
11. Dondorp A, et al; South East Asian Quinine Artesunate Malaria Trial (SEAQUAMAT) group. Artesunate versus quinine for treatment of severe falciparum malaria: a randomised trial. Lancet. 2005 Aug 27-Sep 2;366(9487):717-25.
12. Dondorp AM, et al; AQUAMAT group. Artesunate versus quinine in the treatment of severe falciparum malaria in African children (AQUAMAT): an open-label, randomised trial. Lancet. 2010 Nov 13;376(9753):1647-57. doi: 10.1016/S0140-6736(10)61924-1. Epub 2010 Nov 7. Erratum in: Lancet. 2011 Jan 8;377(9760):126.







2 thoughts on “EM@3AM: Malaria”
From Dr. David Talan:
Hi Brit,
I read your malaria post and had a couple things I teach that I think are critical to EM.
1) fever + return from malaria area = malaria regardless of other seeming explanation for fever
2) you must get a smear or rapid Ag test asap; if it’s the weekend or you work in a small hospital where no one can, some places have a pathologist on call and otherwise you may need to transfer the patient
3) if stable and this first test is negative, you can d/c but with explicit f/u for care next day and repeat smears q 8 x 3 (Ag test only good for P fal. and it’s not ‘in-fal-able’)
4) if P. fal is dx’d, then you can’t just click an order for IV artesunate – you have to get it thru CDC emergency number and then they arrange stat shipment via depots at big airports, like LAX
Malaria Hotline for Healthcare Providers
Via telephone: 1-770-488-7788 or 1-855-856-4713 (toll free)
Via telephone (after hours): 1-770-488-7100
Also, you may be interested in the travel clinical network Geosentinel, which was funded by CDC when our EMERGEncy ID NET was, and their awesome paper showing DDx by chief complaint in travelers from various areas (attached). Here is an example:
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4629801/
Leder K, Torresi J, Libman MD, et al. GeoSentinel surveillance of illness in returned travelers, 2007-2011. Ann Intern Med. 2013;158(6):456–468. doi:10.7326/0003-4819-158-6-201303190-00005
Pingback: Round 18 (Fatigue) – EM Clerkship, LLC