Authors: Haley Sinatro, MD (EM Resident Physician, UT Southwestern); Vietvuong Vo, MD (Assistant Professor of Emergency Medicine, UT Southwestern); Cassandra Mackey, MD (Assistant Professor of Emergency Medicine, UMass Chan Medical School); Alex Koyfman, MD (@EMHighAK); Brit Long, MD (@long_brit)
Welcome to EM@3AM, an emDOCs series designed to foster your working knowledge by providing an expedited review of clinical basics. We’ll keep it short, while you keep that EM brain sharp.
A 32-year-old male with HIV presents to the ED for loss of taste. He noticed white plaques on his tongue, worsening over the last few days. Although painless, the plaque is associated with a cotton sensation and a dull sense of taste. The patient reports being compliant with his medications and denies other symptoms. On exam, the tongue (image 1) is covered in white curd-like plaques that are easily removed with scraping, leaving behind an erythematous base. The posterior oropharynx is without abnormality.
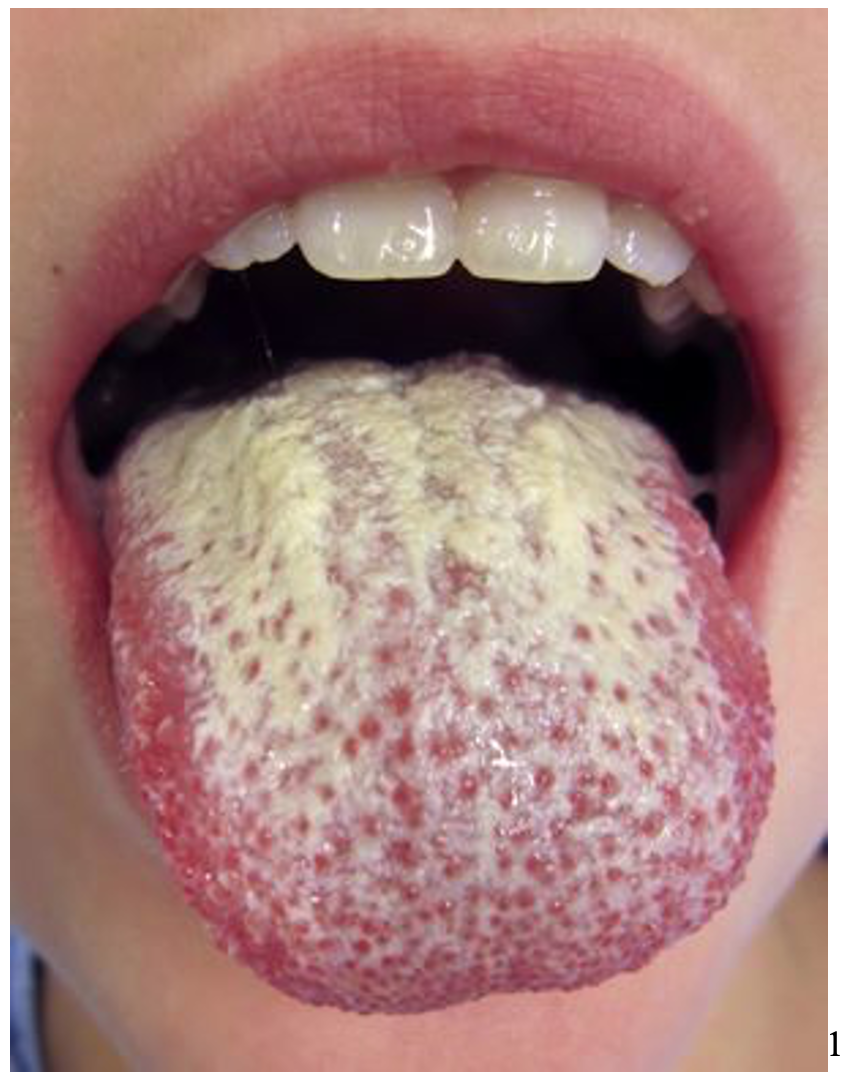
What is the diagnosis?
Answer: Oropharyngeal candidiasis (OPC), also known as thrush
Epidemiology
- Typically, an overgrowth of the fungus Candida Albicans
- 3 primary susceptible populations
- Immunocompromised (i.e. HIV or AIDs, diabetes, on an immunosuppressant, steroid, or antibiotic medications)
- Infants
- More susceptible due to underdeveloped immune systems
- Premature infants or those with low birthweight more susceptible to systemic candidiasis
- Elderly (more common with denture use)
- More commonly presents as an erythematous, atrophic form under upper dentures, with a prevalence of 15% in denture wearers4
Clinical Presentation
- Frequently asymptomatic
- May experience a dry, cotton-mouthed feeling, loss of taste
- Disease severity:
- Mild disease – usually asymptomatic
- Moderate disease – may have pain and greater surface area involvement (>50% of oral mucosa)
- Severe disease – can be painful, can impair the ability to eat
- Esophageal involvement – can occur with OPC or separately; suspect with pain on swallowing. Diagnosed as esophageal candidiasis
- Typically occurs in patients with CD4+ count of <100 cells/microL5

- Risk Factors
- Immunocompromised
- Denture use
- Inhaled/oral steroid use
- Infant with low birth weight or prematurity
- Diagnosis in absence of risk factors may warrant HIV testing
Treatment

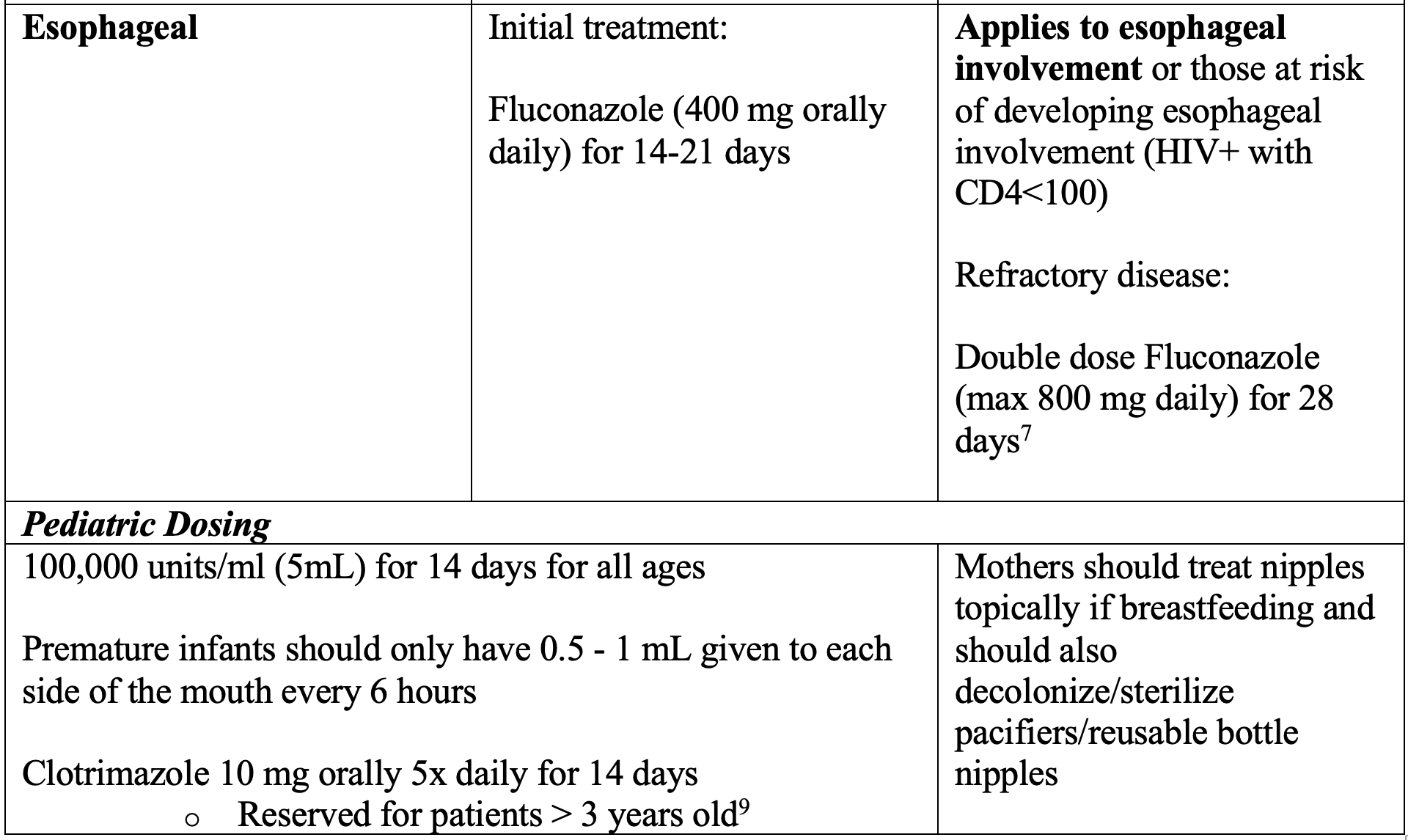
Disposition
- Discharge is warranted in most patients, as the infection is typically self-limited
- Admit if concurrent symptoms merit further investigation
Pearls
- In the absence of risk factors, diagnosis of thrush should warrant HIV testing
- Evaluate for esophageal involvement as these patients are prone to esophagitis
- Counsel denture wearers/pediatric patients’ caregivers on the importance of sterilizing/decolonization to prevent recurrence

A 40-year-old man with HIV presents to the emergency department with a sore throat, difficulty swallowing, and retrosternal pain for several days that is worsened with eating. Examination of the oropharynx reveals white raised plaques in the posterior oropharynx. Given his dysphagia, the clinician wants to provide coverage for candidal esophagitis in addition to oropharyngeal candidiasis. Which of the following therapies is most appropriate to provide this coverage?
A) Clotrimazole troches
B) Intravenous amphotericin B
C) Nystatin oral suspension
D) Oral fluconazole
Answer: D
This patient should be started on oral fluconazole daily for 2 weeks empirically due to the concern for candidal esophagitis. Esophageal candidiasis most often presents with odynophagia and retrosternal pain. It is most commonly seen in patients who are immunosuppressed. It is an AIDS-defining illness in those with HIV. However, it is rarely seen with CD4 cell counts > 200/µL. Definitive diagnosis requires endoscopy, showing classic linear white plaques similar to other candida infections. However, patients with classic symptoms and immunosuppression should begin empiric treatment to prevent further progression of the disease. Patients that do not improve with antifungal therapy should also have an endoscopy performed to rule out other less common causes of infective esophagitis. Many cases will be seen concurrently with oropharyngeal esophagitis that has spread locally to the esophagus. Systemic therapy is preferred for candidal esophagitis to provide adequate coverage.

Clotrimazole troches (A) and nystatin oral suspension (C) may be used for oropharyngeal candidiasis in healthy patients but do not provide adequate coverage for esophageal infection. Intravenous amphotericin B (B) is used in disseminated fungal infections.
- https://wikem.org/wiki/Oropharyngeal_candidiasis#References
- https://coreem.net/podcast/episode-136-0/
References
- “Human tongue infected with oral candidiasis” by James Heilman, MD – Own work. Licensed under CC BY-SA 3.0 via Wikimedia Commons – https://commons.wikimedia.org/wiki/File:Human_tongue_infected_with_oral_candidiasis.jpg#mediaviewer/File:Human_tongue_infected_with_oral_candidiasis.jpg
- Gani F, Caminati M, Bellavia F, Baroso A, Faccioni P, Pancera P, Batani V, Senna G. Oral health in asthmatic patients: a review : Asthma and its therapy may impact on oral health. Clin Mol Allergy. 2020 Nov 7;18(1):22. doi: 10.1186/s12948-020-00137-2. PMID: 33292326; PMCID: PMC7648282.
- Vazquez, J. A. (2000). Therapeutic options for the management of oropharyngeal and esophageal candidiasis in HIV/AIDS Patients. HIV Clin. Trials1, 47–59. doi: 10.1310/T7A7-1E63-2KA0-JKWD
- Budtz-Jørgensen E. Oral mucosal lesions associated with the wearing of removable dentures. J Oral Pathol. 1981 Apr;10(2):65-80. doi: 10.1111/j.1600-0714.1981.tb01251.x. PMID: 6792333.
- Bonacini M, Young T, Laine L. The causes of esophageal symptoms in human immunodeficiency virus infection. A prospective study of 110 patients. Arch Intern Med. 1991 Aug;151(8):1567-72. PMID: 1651690.
- Venugopal S, Gopalan K, Devi A, Kavitha A. Epidemiology and clinico-investigative study of organisms causing vaginal discharge. Indian J Sex Transm Dis AIDS. 2017 Jan-Jun;38(1):69-75. doi: 10.4103/0253-7184.203433. PMID: 28442807; PMCID: PMC5389219.
- Peter G. Pappas, Carol A. Kauffman, David R. Andes, Cornelius J. Clancy, Kieren A. Marr, Luis Ostrosky-Zeichner, Annette C. Reboli, Mindy G. Schuster, Jose A. Vazquez, Thomas J. Walsh, Theoklis E. Zaoutis, Jack D. Sobel, Clinical Practice Guideline for the Management of Candidiasis: 2016 Update by the Infectious Diseases Society of America, Clinical Infectious Diseases, Volume 62, Issue 4, 15 February 2016, Pages e1–e50, https://doi.org/10.1093/cid/civ933
- Iacopino AM, Wathen WF. Oral candidal infection and denture stomatitis: a comprehensive review. J Am Dent Assoc. 1992 Jan;123(1):46-51. doi: 10.14219/jada.archive.1992.0023. Erratum in: J Am Dent Assoc 1992 Mar;123(3):preceding 24. PMID: 1740572.
- Fisher BT, Smith PB, Zaoutis TE. Candidiasis. In: Feigin and Cherry’s Textbook of Pediatric Infectious Diseases, 8th ed, Cherry JD, Harrison G, Kaplan SL, et al (Eds), Elsevier 2018, Philadelphia 2018. p.2030.






