Author: Dalbir Bahga, MD (EM Resident Physician, UTSW/Parkland Memorial Hospital) // Reviewed by: Alex Koyfman, MD (@EMHighAK, EM Attending Physician, UTSW/ Parkland Memorial Hospital) and Brit Long, MD (@long_brit, EM Attending Physician, San Antonio, TX)
Welcome to EM@3AM, an emDOCs series designed to foster your working knowledge by providing an expedited review of clinical basics. We’ll keep it short, while you keep that EM brain sharp.
A 31-year-old G3P2 female at 32 weeks gestation is brought in by EMS after a fall with complaint of lower abdominal pain. She slipped on water, fell on her side, and is now having lower abdominal cramping. There was no LOC/seizures observed, and serum glucose was 102. She denies any leakage of fluids or vaginal bleeding.
In the ED, her vitals are BP 126/78, HR 90, RR 16, SpO2 99% on RA, Temp 37 C. Exam reveals gravid abdomen with lower abdominal tenderness and no signs of bruising. Her underwear reveals fresh spotting of vaginal blood. External pelvic exam shows no signs of external trauma, but there is scant blood at the introitus. Fetal heart rate is measured at 110 bpm with bedside ultrasound.
What is the patient’s diagnosis? What is the next step in your evaluation and treatment?
Answer: Placental Abruption
Background:
- Placental abruption is defined as the premature separation of the placenta from the uterine wall usually after 20 weeks and prior to delivery.1,2
- The different classifications of placental abruption include:
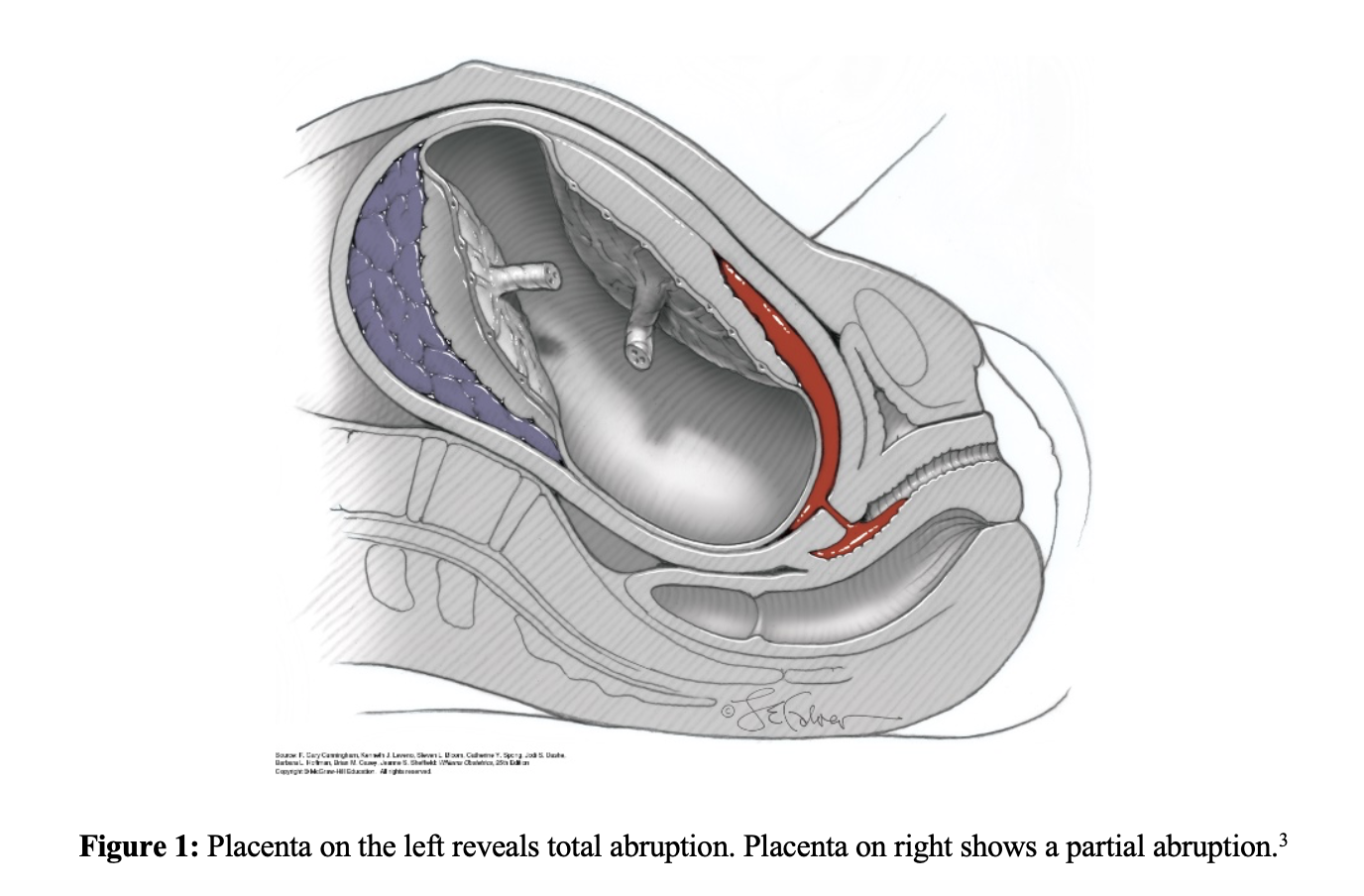
- Total or partial abruption, which evaluates the extent of the placental detachment from the uterine wall.3 (Figure 1)
- Revealed or concealed abruption, which will dictate if vaginal bleeding is present or not.3 (Figure 2)
- There are significant maternal and fetal morbidity and mortality associated with placental abruption. Thus catching this diagnosis is critical.
- Maternal complications/risks: coagulopathy including disseminated intravascular coagulation (DIC), need for blood transfusions, hemorrhagic shock, uterine rupture, hysterectomy, and multiple organ failure.2,4,5
- Fetal complications/risks: preterm deliver, growth restriction, low birth weight, cerebral palsy, fetal hypoxia, and stillbirth.2,4,5

Epidemiology:
- Incidence: placental abruption has been seen in about 0.6-1% of births in the U.S.2,4-6
- Increased incidence found to be highest at 24-26 weeks gestation and drops with advancing gestation.6
Risk Factors:
- Prior abruption, hypertension, advance maternal age, multiparous, cigarette smoking, cocaine use, trauma (MVC, physical assault, falls), preeclampsia, chorioamionitis, preterm ruptured membranes, multifetal gestation, single umbilical artery, uterine leiomyoma.3,4, 6-8
Pathophysiology:
- Likely from a ruptured decidual spiral artery causing an expanding retroplacental hematoma.3 This bleeding can cause a total or partial separation.
- Often times the blood from the detachment will escape through to the cervix causing vaginal bleeding. However the blood can be retained between the detached placenta and uterus, concealing the hemorrhage and resulting in no bleed.4
- Abnormal trophoblastic invasion of uterine vessels can be a predisposing factor to abruption.4 Other contributing factors include shearing forces from trauma, long-standing processes such as HTN, and vasoconstriction with cocaine use.6
- As tissue is separated in placental abruption, clot formation and the repeated release of thromboplastic material into circulation increases the risk of DIC.4
- Blood accumulation in the uterine wall can stimulate the myometrium to contract causing uterine contractions.4
- With placental separation, the oxygen and nutrient supply to the fetus is compromised, causing growth restrictions and even risk for fetal death.5-6
Clinical Presentation:
- Painful third trimester vaginal bleeding.
- Classic presentation: sudden abdominal pain, vaginal bleeding, and uterine tenderness.3,6
- Other common symptoms include back pain, fetal compromise (non-reassuring fetal heart tracings), hypertonic uterus.3,4
- In cases of concealed abruptions, patients often present without vaginal bleeding.4,6
- The degree of placental abruption can cause different presentations:
- Mild abruption can present as mild uterine with mild or no vaginal bleeding. This patient can have normal vital signs, no coagulopathy or fetal distress.1,3
- Severe abruption can present with severe uterine pain, continuous or repetitive uterine contractions, heavy or no vaginal bleeding, fetal distress, coagulopathy, hypotension or shock.1,3
- Uterine contractions can be seen on initial presentation, with placental abruption being the causing factor, but can be missed diagnosis if abruption is not considered.6
- Fetus clinical presentation:
- Changes in fetal heart rate pattern can indicate fetal distress from uteroplacental insufficiency.6
Differential Diagnoses:
- Consider causes for abdominal pain and vaginal bleeding including placenta previa, uterine rupture, appendicitis, urinary tract infections, preterm labor, fibroid degeneration, ovarian pathology, and muscular pain.6
Evaluation and Diagnosis:
- Placental abruption is a clinical diagnosis and often confirmed after delivery by evaluating the placenta.4
- History:
- Important factors to consider: trauma, hypertension, history of abruption, vaginal bleeding, cocaine use, signs of infection, cigarette smoking, how many previous pregnancies, and the age of the patient, as these all serve as risk factors for abruption.
- Ask if the patient has been receiving regular prenatal care, any concerning ultrasounds, previous complications.
- Vital signs! Detection of hypotension and tachycardia can signal hypovolemic shock from blood loss. However, women with hypertension can easily mask hypovolemia with normal blood pressure values, so do not rely on blood pressure alone.
- Physical Exam: All trauma patients should be evaluated completely to look for other injuries. The abdomen should be evaluated for external signs of trauma. External pelvic exam should be done to check for vaginal bleeding, however, do not perform speculum or bimanual without confirming location of placenta with ultrasound first.
- Signs of fetal distress such as non-reassuring fetal heart tones is often seen with placental abruption. Therefore it is very important to initiate fetal monitoring to monitor activity.
- Lab studies: CBC, blood type and screen, and coagulation studies including fibrinogen, prothrombin time, and activated partial thromboplastin time.
- Fibrinogen level has been used as a good tool to detect severity of bleeding, presence of DIC, and the need for transfusion of blood products.9
- Initial fibrinogen levels <200mg/dL: 100% positive predictive value for severe postpartum hemorrhage.9
- Kleihauer-Betke test is frequently done, but has been shown to have poor usefulness to confirm diagnosis of abruption. It does however relay information that helps guide dosing of Rh-immune globulin in Rh-negative women.6,10
- Fibrinogen level has been used as a good tool to detect severity of bleeding, presence of DIC, and the need for transfusion of blood products.9
- Imaging:
- Ultrasound is recommended with any vaginal bleeding to rule out placenta previa prior to pelvic exam and to evaluate for placental abruption. However, ultrasound use for detecting placental abruption holds a low sensitivity and is not the best tool, as placenta and fresh blood clots can have similar sonographic characteristics. One study by Glantz and Purnell found a 24% sensitivity with ultrasound.11
- A negative ultrasound does not rule out placental abruption!4,6
- MRI can be a useful diagnostic test but is of limited value in an unstable patient.
- The key in managing placental abruption is maternal stabilization, cardiotocographic fetal monitoring, and emergent OB consultation.
- Continuous maternal/fetal monitoring.
- Secure IV access with 2 large bore IVs, as these patients may be at risk for hemorrhagic shock, so they may need blood transfusions.
- RhoGAM administration should be considered if mother is Rh negative.
- Repletion of coagulation factors should be initiated if labs indicate DIC.
- Severe abruption should be managed by immediate delivery.

Disposition:
- Consult OBGYN
- Observation with fetal monitoring in L&D vs Delivery.
- In cases of blunt/minor trauma and unclear diagnostics, observation is recommended with electronic fetal monitoring.
- Optimal duration is unclear, but recommendations include:
- Women with viable pregnancies after trauma without contractions: 6 hours with cardiotocography after trauma.
- Women with viable pregnancies after trauma with contractions: 24 hours with cardiotocography.
- Optimal duration is unclear, but recommendations include:
Pearls:
- Placental abruption classically presents with painful, often sudden third trimester bleeding, but you may not always see vaginal bleeding if the abruption is concealed.
- Common risk factors: abdominal trauma, cocaine use, advanced maternal age, HTN, multiparous.
- Never perform a pelvic exam until an ultrasound is done to confirm the location of the placenta. Manipulation can cause worsening dislocation of the placenta and increased risk of further bleeding.
- Do no rely on ultrasound to rule out the condition.
- Keys in management include maternal stabilization, cardiotocographic fetal monitoring, and emergent OB consultation.

A 32-year-old woman presents with acute onset abdominal pain and dark vaginal bleeding that started this morning. She is 34 weeks pregnant. The uterus is appropriate size for gestational age and is firm and tender on palpation. Cardiotocographic monitoring shows uterine irritability and intermittent late decelerations. Which of the following correlates best with the severity of bleeding in placental abruption?
A) Amount of bleeding reported and visualized on pelvic examination
B) Fibrinogen level
C) Hemoglobin level
D) Kleihauer-Betke result
Answer: B
This patient’s presentation is concerning for placental abruption, a condition in which the placenta separates from the uterine wall. Vaginal bleeding is present in 70% of patients and is often dark in color. The amount of bleeding can vary and does not correlate with the degree of separation. Bleeding may be concealed behind the placenta so the absence of vaginal bleeding does not rule out the diagnosis. Fibrinogen levels correlate best with the severity of bleeding, with initial levels of ≤ 200 mg/dL having a 100% positive predictive value for severe hemorrhage. Lower abdominal and back pain are common, as are uterine contractions and irritability. Depending of the degree of separation, fetal distress may be noted on cardiotocographic monitoring in the form a category III fetal heart rate pattern (e.g., absent variability with recurrent late decelerations, bradycardia). Risk factors for placental abruption include hypertension, previous placental abruption, preeclampsia, multiparity, cocaine use, and smoking. The combination of hypertension and smoking has a synergistic effect on the risk of abruption.

As noted above, the amount of bleeding reported and visualized on pelvic examination (A) does not correlate with the severity of hemorrhage as blood may be concealed behind the placenta. The initial hemoglobin (C) level will not necessarily be reflective of the degree of hemorrhage in acute placental abruption. The Kleihauer-Betke test (D) is used to measure for the presence of fetal hemoglobin in the maternal bloodstream. This test is only positive in a small number of abruptions and, therefore, can not be used to diagnosis the condition or as a marker of bleeding severity.
Further Reading:
- EMin5 Video on vaginal bleeding in third trimester: https://emin5.com/2018/06/05/third-trimester-vaginal-bleeding/
- EM:RAP Placental Abruption https://www.emrap.org/episode/emrap20186/placental
- EmDocs: The Bleeding Pregnant Patient in the Third Trimester http://www.emdocs.net/9117-2/
- WikiEM on Placental Abruption: https://www.wikem.org/wiki/Placental_abruption
References:
- Ananth CV, Lavery JA, Vintzileos AM, et al. Severe placental abruption: clinical definition and associations with maternal complications. Am J Obstet Gynecol. 2016;214(2):272.e1-272.e9.
- Tikkanen M. Placental abruption: epidemiology, risk factors and consequences. Acta Obstet Gynecol Scand. 2011;90(2):140-9.
- Obstetrical Hemorrhage. Cunningham F, Leveno KJ, Bloom SL, Dashe JS, Hoffman BL, Casey BM, Spong CY, eds. Williams Obstetrics, 25e New York, NY: McGraw-Hill
- Hladky K, Yankowitz J, Hansen WF. Placental Abruption. Obstet Gynecol Surv. 2002; 57: 299-305
- Downes KL, Grantz KL, Shenassa ED. Maternal, Labor, Delivery, and Perinatal Outcomes Associated with Placental Abruption: A Systematic Review. Am J Perinatol. 2017;34(10):935-957.
- Oyelese Y, Ananth CV. Placental abruption. Obstet Gynecol. 2006; 108 (4): 1005-16.
- Young J. Maternal Emergencies After 20 Weeks of Pregnancy and in the Postpartum Period. Tintinalli JE, Stapczynski J, Ma O, Yealy DM, Meckler GD, Cline DM. eds. Tintinalli’s Emergency Medicine: A Comprehensive Study Guide, 8e New York, NY: McGraw-Hill; 2016.
- Vaught A, Deering S, Harris C. Trauma and Pregnancy. Foley MR, Strong, JR TH, Garite TJ eds. Obstetric Intensive Care Manual, 5e New York, NY: McGraw-Hill
- De Lloyd L, Bovington R, Kaye A, et al. Standard hemostatic tests following major obstetric hemorrhage. Int J Obstet Anesth 2011; 20:135.
- Atkinson AL, Santolaya-Forgas J, Matta P, et al. The sensitivity of the Kleihauer-Betke test for placental abruption. J Obstet Gynaecol 2015; 35:139.
- Glantz C, Purnell L. Clinical Utility of sonography in the diagnosis and treatment of placental abruption. J Ultrasound Med. 2002; 21: 837-40.





