Authors: Richard Schwamb, DO (North Shore / Long Island Jewish, Manhasset, New York) and Victor Huang, MD (North Shore / Long Island Jewish, Manhasset, New York) // Reviewed by: Sophia Görgens, MD (EM Resident Physician, Zucker-Northwell NS/LIJ, NY) and Cassandra Mackey, MD (Assistant Professor of Emergency Medicine, UMass Chan Medical School)
Welcome to EM@3AM, an emDOCs series designed to foster your working knowledge by providing an expedited review of clinical basics. We’ll keep it short, while you keep that EM brain sharp.
A 75-year-old male with a history of hypertension, osteoarthritis, and diabetes mellitus presents to the ED with a chief complaint of lower back pain. He states that he fell a few days ago and the pain is getting worse, particularly when he is sitting down. His vitals include blood pressure 150/95, heart rate 95, SPO2 99%, temperature 36.6C, and a glucose of 143. On examination, the pelvis is stable, but he endorses tenderness midline along his sacrum. He has normal motor and sensation function in all extremities.
What’s the diagnosis?
Answer: Sacral fracture
Epidemiology
- 67 per 100,000 people suffer from sacral fractures1
- Has a bi-modal distribution of injury:2-6
- Young patients (age 18-35) from high energy trauma such as motor vehicle collisions
- Elderly patients (age > 65) from low energy trauma such as ground level falls2
- Risk factors: osteoporosis, chronic steroid use, radiation, malignancy and hyperparathyroidism 3-7
Anatomy
- The bony pelvis is composed of five main elements: ilium, ischium, pubis, sacrum, coccyx
- The sacrum has four pairs of foramina
- Located between the left and right iliac bones
- Anterior muscles comprise the piriformis, coccyges, and iliac; posterior aspect has the gluteus maximus attachment, multifidus lumborum, and erector spinae
- Ventral foramen are the openings of the sacrum
- Represent S1-S4
- S1 ventral foramen is up to 80% filled by the ventral root
- In comparison to the S4, 15% is filled in by the foot
- Lower sacral nerve roots (S2-S5) are responsible for anal sphincter, perianal sensation and bulbocavernosus reflex2


Clinical presentation
- Typically presents with pelvic pain, pain with sitting down, tenderness along lower back
- Patients may or may not have difficulty with ambulation secondary to pain
- Younger patients present after high velocity mechanism of injury while elderly patients can present after a fall from standing height
Evaluation
- A detailed physical exam including soft tissue and neurological exam
- In the setting of a traumatic event:
- Perform primary and secondary survey before focusing on the sacrum, including assessment for thoracic and intraabdominal injuries 7
- Concentrate on pelvic bone stability, neurovascular status, and soft tissue injury
- Assess externally for soft tissue injury: Rectal / vaginal exam
- Puncture injuries may be considered open fractures
- A fracture extending into the rectum or vagina is considered an open fracture
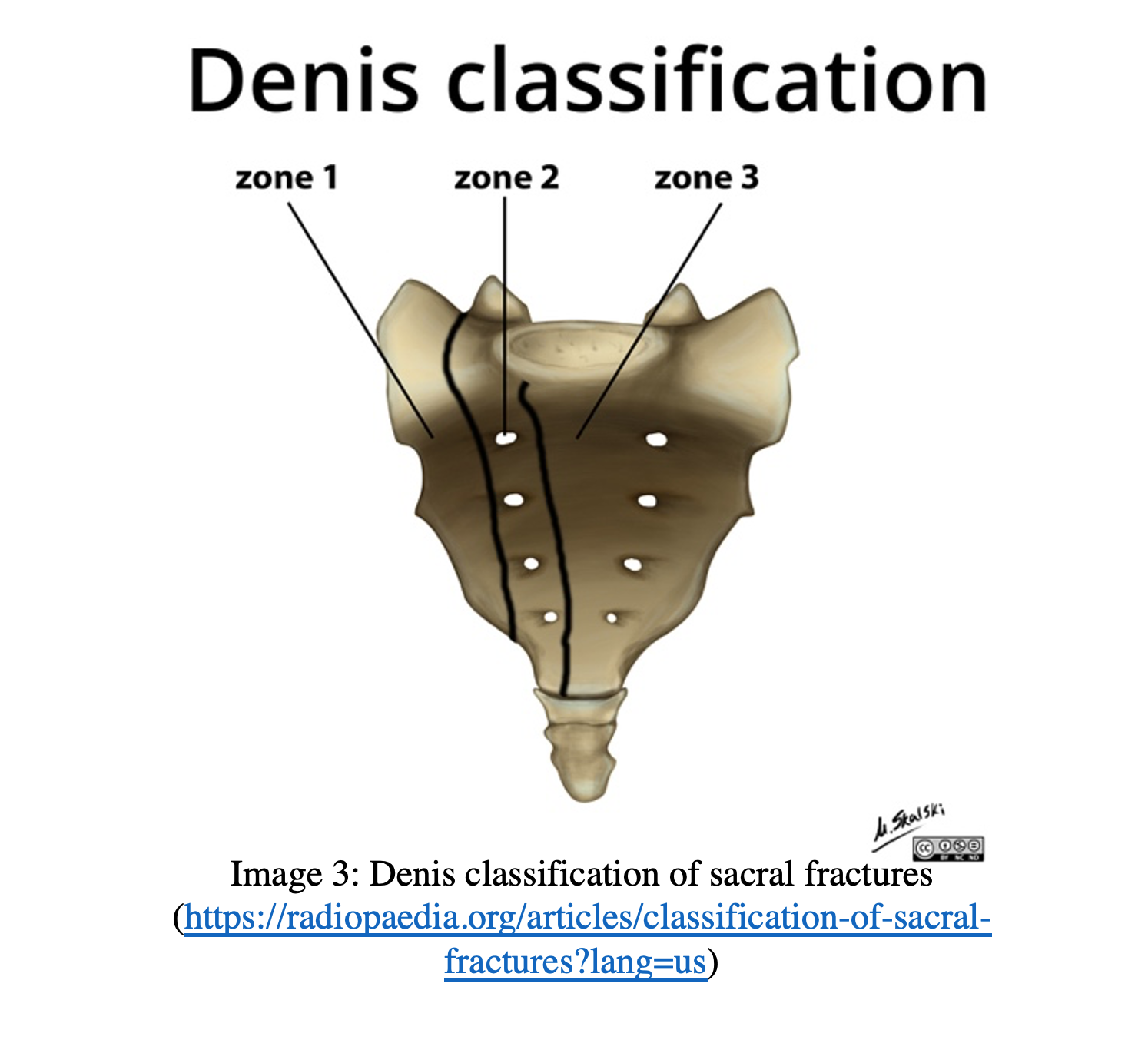
- Denis Classification of sacral fractures:
- Zone 1: Injury lateral to the sacral foramina
- Sacral alar fracture
- Can present with foot drop (L5 nerve root)
- Neurological involvement is present in less than 5% of patients
- Zone 2: Injury involving sacral foramina (No spinal canal involvement)
- Foraminal Zone
- 30% of patients have a neurological involvement
- Zone 3: Injury involving the spinal canal
- Can induce cauda equina,
- Loss of bladder, bowel and sexual function
- Longitudinal and transverse variants for zone III
- CT scan with axial imaging best for visualization
- Can induce cauda equina,
- Transverse Fractures
- Axial load can cause a transverse fracture at the weakest aspects, usually S2 and S3
- CT is the best imaging to visualize3
- Zone 1: Injury lateral to the sacral foramina
- If mechanism is atraumatic, consider a sacral pathologic fracture secondary to malignancy or sacral insufficiency fracture, which can be secondary to osteoporosis5
- Radiographic evaluation
- AP pelvis, inlet, and outlet views
- Commonly inconclusive and demonstrates poor sensitivity
- CT in conjunction with inlet and outlet views are most often necessary when there is suspicion for fracture5
- Proceed with admitting and obtaining an MRI if there is neurological damage / deficits
- Emergent MRI warranted if signs or symptoms of cauda equina syndrome
- AP pelvis, inlet, and outlet views
Treatment
- If stable
- Assess for other signs of injury / pelvic fracture
- Patient stabilization
- Pain control as needed
- If presenting with an open pelvic fracture, apply a pelvic binder and obtain a CT with contrast
- Pelvic binders should be placed over the greater trochanters of the femur
- Orthopedic consultation
- Non-operative management is indicated for stable sacral fractures with no displacement, no soft tissue involvement, and no neurological deficit7
- These patients benefit from activity modification, weight bearing as tolerated
- Some patients may require hip spica casts, bracing, or traction, varying upon orthopedic consult service7
- Surgical management is indicated for sacral fractures with instability, displaced fracture fragment, soft tissue injury, or neurological involvement6
Disposition
- Home with orthopedic follow up if stable
- Disposition pending orthopedic recommendation
Pearls
- A full neurologic exam, specifically aimed at the lower nerve roots (L5-S5), is needed to find any deficits
- CT may be needed to discover if there is a fracture; x-rays have poor sensitivity
- Most patients are appropriate for discharge with orthopedic follow up with weight bearing ambulation as tolerated

A 28-year-old man presents after a motor vehicle collision. He is conscious and reports severe pain shooting down the back of his legs. On exam, you note bilateral leg weakness and decreased lower extremity reflexes, decreased rectal tone, decreased sensation over the inner thighs, and pain on gentle compression of the pelvis. You obtain an X-ray, which shows a sacral fracture. What is the most critical next step in the management of this patient’s condition, along with appropriate further imaging?
A) Catheterization of the bladder
B) Methylprednisolone administration
C) Neurosurgical consultation
D) Physical therapy consultation for sacral fracture
Answer: C
Traumatic cauda equina syndrome is not a spinal cord injury since the cauda equina (Latin for “horse’s tail”) is a bundle of nerve roots distal to the conus medullaris. Since injury to or compression of any of these nerve roots is possible, there is no single finding that is 100% predictive of the diagnosis, and the presentation may be variable. Symptoms and signs may include a sensory deficit over the buttocks, perineal area, and inner thighs (saddle anesthesia), decreased rectal tone, severe sciatica, variable sensory and motor loss in one or both lower extremities, and decreased lower extremity reflexes. Variable bladder or bowel dysfunction, including overflow incontinence, is possible but often not present when presenting acutely. Likewise, rectal tone may be spared. In contrast, lesions that affect only the conus medullaris present with early bladder and bowel dysfunction. When trauma is the cause of cauda equina syndrome, trauma protocols should be adhered to, and pelvic X-rays may reveal a sacral fracture. Magnetic resonance imaging is the study of choice to assist in the diagnosis, although computed tomography or myelography may help delineate the injury. Neurosurgical consultation is critical since acute traumatic cauda equina syndrome presents as a surgical emergency with decompression, preferably within 6 hours, traditionally regarded as the treatment of choice.
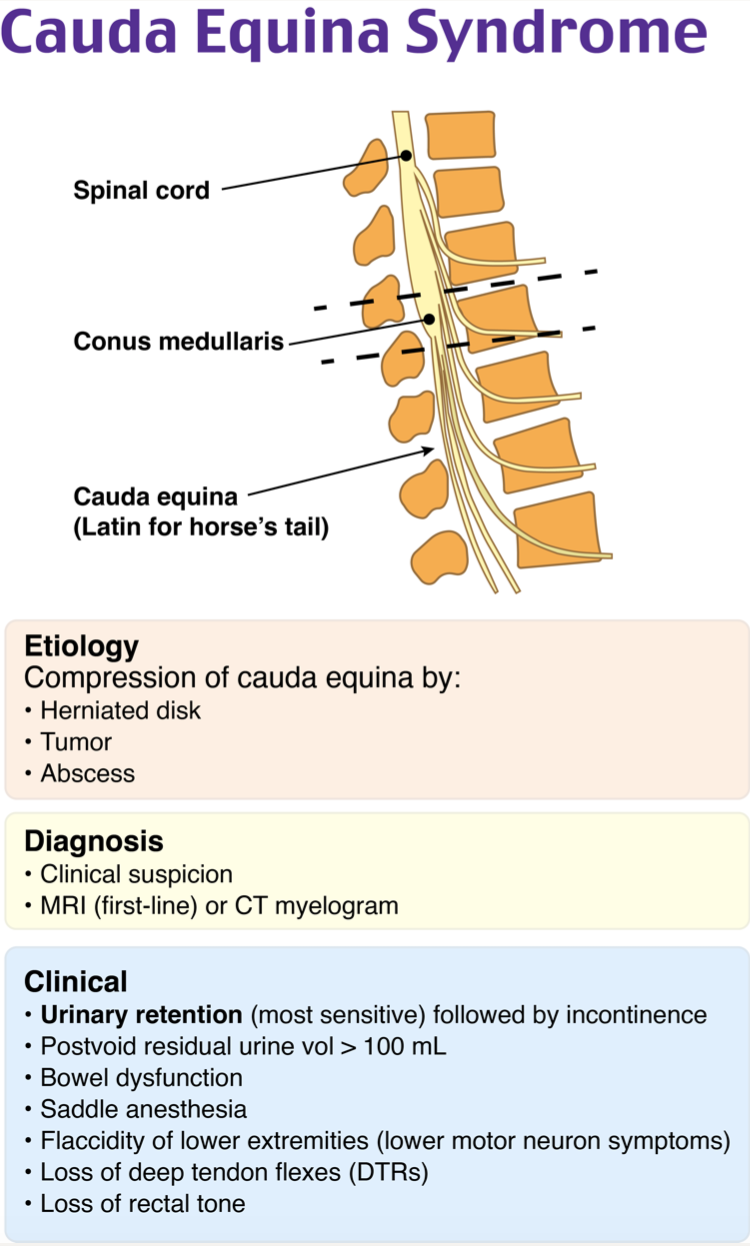
Catheterization of the bladder (A) may become necessary in this patient, as bladder dysfunction is a common part of the presentation. However, classic signs such as overflow incontinence tend to present late, and this would not be the most critical next step in management. Methylprednisolone administration (B) is recommended within eight hours of presentation in cases where cauda equina syndrome was caused by an inflammatory condition, but it has not been shown to be of any benefit in cases caused by acute trauma. Physical therapy consultation for sacral fracture (D) is not the most critical next step. The main concerns with a fracture of the sacrum are neurological injuries and a keen awareness of the amount of force necessary to cause this fracture. Unstable and displaced fractures may need surgery even in the absence of nerve injury. It is prudent to carefully look for associated injuries. Physical therapy may be needed later in the patient’s hospital or outpatient course.
FOAMed Sources:
References:
- Bydon M, De la Garza-Ramos R, Macki M, Desai A, Gokaslan AK, Bydon A. Incidence of sacral fractures and in-hospital postoperative complications in the United States: an analysis of 2002-2011 data. Spine (Phila Pa 1976). 2014;39(18):E1103-E1109. doi:10.1097/BRS.0000000000000448
- Bydon M, Fredrickson V, De la Garza-Ramos R, et al. Sacral fractures. Neurosurg Focus. 2014;37(1):E12. doi:10.3171/2014.5.FOCUS1474
- Beckmann NM, Chinapuvvula NR. Sacral fractures: classification and management. Emerg Radiol. 2017;24(6):605-617. doi:10.1007/s10140-017-1533-3
- Urits I, Orhurhu V, Callan J, et al. Sacral Insufficiency Fractures: A Review of Risk Factors, Clinical Presentation, and Management. Curr Pain Headache Rep. 2020;24(3):10. Published 2020 Feb 17. doi:10.1007/s11916-020-0848-z
- Galbraith JG, Butler JS, Blake SP, Kelleher G. Sacral insufficiency fractures: an easily overlooked cause of back pain in the ED. Am J Emerg Med. 2011;29(3):. doi:10.1016/j.ajem.2010.04.015
- Lykomitros VA, Papavasiliou KA, Alzeer ZM, Sayegh FE, Kirkos JM, Kapetanos GA. Management of traumatic sacral fractures: a retrospective case-series study and review of the literature. Injury. 2010;41(3):266-272. doi:10.1016/j.injury.2009.09.008
- Gutierrez-Gomez S, Wahl L, Blecher R, Olewnik L, Iwanaga J, Maulucci CM, et al. Sacral fractures: an updated and comprehensive review. Injury. 2021; 52(3): 366-375. Doi:10.1016/j.injury.2020.11.015






1 thought on “EM@3AM: Sacral fractures”
Pingback: April 2023 Asynchronous – MSK/Ortho | Harbor-UCLA DEM Education