Prevent and Identify – the ED’s equivalent of Search & Rescue when managing elevated Intracranial Pressures (ICP). The causes of elevated ICP are typically described in the context of Traumatic Brain Injury (TBI), however many other pathologies can benefit from standardized ICP management. Such problems exist either intracranially (edema, hematoma, seizure, etc) and/or extracranially (coughing, fever, hypoxia, hypercarbia, pain, airway obstruction, etc).(1) Tintinalli describes the primary goals in managing TBI: prevent further secondary brain injury, identify treatable mass lesions, and other life-threatening injuries.(2)
An estimated 10 million TBI cases lead to hospitalization and death annually.(1) Mortality in severe injuries, defined as a Glasgow Coma Scale (GCS) score of less than 8, approaches up to 60%.(3) In the information-scarce, time-limited environment emergency physicians work in, having a high index of suspicion for elevated ICP while implementing interventions early goes a long way between patient presentation and definitive management.
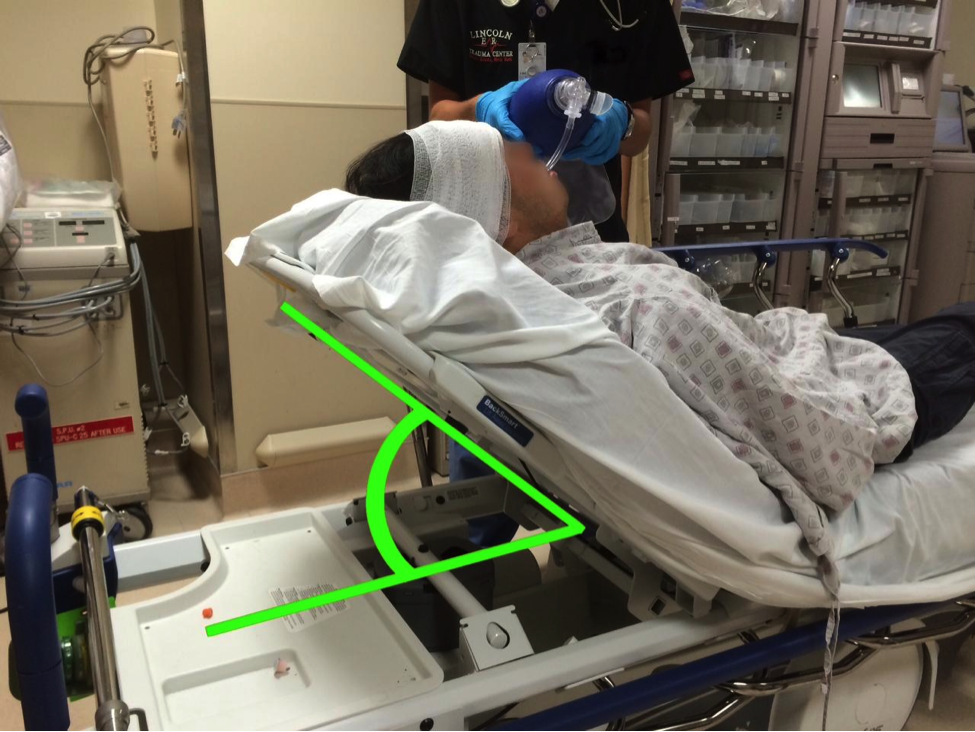
How can we minimize further elevations? There are several stepwise approaches described in the literature. In May 2014, the New England Journal of Medicine released a TBI review, where within Stochetti et al discuss a traditional “staircase approach to the treatment of increased intracranial pressure.” Dr. Scott Weingart confers his “tiered” management in EMCrit Podcast 78; all of these are either linked or referenced below. Historically, there is a wide scope of traditional management, ranging from head of bed elevation (see picture above) to the potential use of steroids, barbiturates, etc. – these won’t be discussed in this update. Here we discuss the most current analyses of therapies in the elevated ICP patient, via the trusted ABC’s… and D (and a conceptually interesting E).
Airway
There are two rapid sequence intubation (RSI) premedications frequently discussed.
Lidocaine originally gained favor as an RSI pretreatment after several small trials had demonstrated “less of an increase” in ICP during neurosurgical procedures.(4,5) Despite this initial data, recent meta-analyses have shown that there is no clinically significant reduction in ICP with the administration of lidocaine before direct laryngoscopy.(6) Some sources argue there is little downside to pretreatment, with a potential/theoretical benefit in ICP reduction in patients at risk for secondary brain injury.(7)
Fentanyl has been known to be effective at blunting the sympathetic response during direct laryngoscopy. As per Up To Date, “No data exist regarding the effects of fentanyl on the ICP of patients with acute head injuries undergoing RSI.” They also warn to be weary of tenuous blood pressures; either reduce the dose or avoid altogether.(7) There is some promising recent data, as a study from the Journal of Trauma Acute Care Surgery found that in the treatment of intracranial hypertension, fentanyl infusions achieved “smaller but significant ICP reductions” when compared to osmotic agents.(8)
For a more in depth discussion, be sure to check out this previous emDocs update: http://www.emdocs.net/intubating-critically-ill-patient/
Breathing
Traditionally, hyperventilation has been known to decrease ICP by up to 25%.(3) A Cochrane Review states “while hyperventilation therapy can reduce ICP after traumatic brain injury, the review of trials found there is no strong evidence about whether this improves outcomes. More trials are needed.”(9)
Circulation
Another debated topic is the choice of fluids/osmotic agents, namely mannitol and hypertonic saline (HTS). A Cochrane Review states that “mannitol may have a detrimental effect on mortality when compared to hypertonic saline.”(10) HTS has been shown to be safe and effective for the reduction of ICP while also improving the patient’s hemodynamic status; however, this has not been shown to significantly affect outcomes.(11) Ultimately, neither agent has been shown to be superior.(1) A search of the Cochrane database shows a study in the protocol stage titled, “Hypertonic saline versus other intracranial pressure-lowering agents for people with acute traumatic brain injury;” so stay tuned.(12,13)
emDocs also further discusses BP management in the ICP patient in this prior article: http://www.emdocs.net/aggressive-bp-management-patients-ich/
Diameter
A relatively new adjunct to consider in traumatic head injury is the ocular ultrasound (US). It is rapid, minimally invasive, and may have reliable diagnostic capability. It may not obviate the need for further testing, but has the potential for earlier recognition prompting earlier therapeutic action. Several studies have examined optic nerve sheath diameter (ONSD) as measured by US compared to CT scan, as wells as invasive pressure measurements.(14,15) The pooled sensitivity from these studies was shown to be 90% in a meta-analysis from the journal of Intensive Care Medicine.(16) Another meta-analysis from the Journal of Neurosurgery in 2014 found there may be diagnostic utility with ONSD ultrasound, but due to concerns regarding the heterogeneity of the included studies, is not recommended as a standard of care.(17)
Ex-Lap
Although completely outside the realm of ED management, Joseph et al expands the conceptualization of trauma management by introducing decompressive laparotomy to treat intractable ICP.(18) The hypothesis in short: the body is a circuit of compartments arranged in series. Each compartment has the capacity to become pathologic in the trauma patient, i.e.:
- abdominal compartment syndrome
- thoracic compartment syndrome (pneumothorax, tamponade)
- intracranial compartment syndrome (discussed above)
Decompressing one compartment decompresses another.
… ok, so it’s not really Exploratory, as much as it is Therapeutic laparotomy. But let’s be honest, you probably won’t remember the mnemonic “ABCDT” when your brain is under pressure.
Bottom Line
- Have a high index of suspicion; not just in the trauma patient.
- Airway: Use discretion with fentanyl and lidocaine as RSI pretreatments, time-permitting.
- Breathing: Hyperventilation – not as useful as previously thought.
- Circulation: Mannitol vs. HTS – still controversial; HTS favored.
- Diameter: ONSD ultrasound can’t hurt (unless there’s a globe rupture).
- Ex-lap: food for thought.
Further Reading/Listening
- Dr. Scott Weingart on ICP/Herniation Management and Neurocritical Care Intubations
- Ocular Ultrasound:
- Dr. Tom Scalea on Cutting Edge ICP Management
- http://www.ncbi.nlm.nih.gov/pubmed/20580516
- http://www.ncbi.nlm.nih.gov/pubmed/23811861
References
- Stochetti et. al. Traumatic Intracranial Hypertension. N Engl J Med May 2014 370;22.
- Ma, O. J., Cline, D., Cydulka, R., & Meckler, G. (2011). Tintinalli’s emergency medicine: a comprehensive study guide. New York: McGraw-Hill.
- Marx, J., Hockberger, R., & Walls, R. (2013). Rosen’s Emergency Medicine-Concepts and Clinical Practice. Elsevier Health Sciences.
- Bedford RF, Winn HR, Tyson G, et al. Lidocaine prevents increased ICP after endotracheal intubation. In: Shulman K, Mamorou A, Miller JD, et al., eds. Intracranial Pressure IV. Berlin, Germany: Springer-Verlag; 1980:595-598.
- Grover VK, Reddy GM, Kak VK, et al. Intracranial pressure changes with different doses of lignocaine under general anesthesia. Neurol India 1999; 47:118-121.
- Robinson, N., and M. Clancy. “In patients with head injury undergoing rapid sequence intubation, does pretreatment with intravenous lignocaine/lidocaine lead to an improved neurological outcome? A review of the literature.”Emergency Medicine Journal 18.6 (2001): 453-457. PMID: 11696494
- Caro, D. (2014). Pretreatment agents for rapid sequence intubation in adults. In R.M. Walls (Ed.), UpToDate. Retrieved from: http://www.uptodate.com/contents/pretreatment-agents-for-rapid-sequence-intubation-in-adults
- Colton, K., Yang, S., Hu, P.F., Chen, H.H., Bonds, B., Scalea, T.M., & Stein, D.M. Intracranial pressure response after pharmacologic treatment of intracranial hypertension. Journal of Trauma Acute Care Surgery. 2014 Jul;77(1):47-53. PMID: 24977754.
- Roberts I, Schierhout G. Hyperventilation therapy for acute traumatic brain injury. Cochrane Database of Systematic Reviews 1997, Issue 4. Art. No.: CD000566.
- Wakai A, McCabe A, Roberts I, Schierhout G. Mannitol for acute traumatic brain injury. Cochrane Database of Systematic Reviews 2013, Issue 8. Art. No.: CD001049.
- Holmes, J.A. (2013). Therapeutic Uses Of Hypertonic Saline In The Critically Ill Emergency Department Patient. EM Critical Care, Volume 3, Number 1.
- Chen H, Song Z. Hypertonic saline versus other intracranial pressure–lowering agents for people with acute traumatic brain injury. Cochrane Database of Systematic Reviews 2014, Issue 2. Art. No.: CD010904.
- Ropper, A. H. (2012). Hyperosmolar therapy for raised intracranial pressure. New England Journal of Medicine, 367(8), 746-752.
- Tayal VS, Neulander M, Norton HJ, Foster T, Saunders T, Blaivas M. Emergency department sonographic measurement of optic nerve sheath diameter to detect findings of increased intracranial pressure in adult head injury patients. Ann Emerg Med. 2007 Apr;49(4):508-14. Epub 2006 Sep 25. PMID: 16997419
- Major R, al-Salim W. Towards evidence based emergency medicine: best BETs from the Manchester Royal Infirmary. BET 3. Ultrasound of optic nerve sheath to evaluate intracranial pressure. Emerg Med J. 2008 Nov;25(11):766-7. PMID:18955621.
- Dubourg, J., Javouhey, E., Geeraerts, T., Messerer, M., & Kassai, B. (2011). Ultrasonography of optic nerve sheath diameter for detection of raised intracranial pressure: a systematic review and meta-analysis. Intensive care medicine, 37(7), 1059-1068. PMID: 21505900
- Yavin, D., Luu, J., James, M. T., Roberts, D. J., Sutherland, G. R., Jette, N., & Wiebe, S. (2014). Diagnostic accuracy of intraocular pressure measurement for the detection of raised intracranial pressure: meta-analysis: A systematic review. Journal of neurosurgery, 1-8.
- D’Andrea, K. J., Dutton, R. P., Aarabi, B., & Scalea, T. M. (2004). Decompressive laparotomy to treat intractable intracranial hypertension after traumatic brain injury. Journal of Trauma-Injury, Infection, and Critical Care,57(4), 687-695. PMID: 15514520.






2 thoughts on “ICP Management Update”
Pingback: Best Case Ever 55 Pediatric Cerebral Herniation - Emergency Medicine Cases
Pingback: emDOCs.net – Emergency Medicine EducationThe Crashing Trauma Patient - emDOCs.net - Emergency Medicine Education