Here’s another case from Medical Malpractice Insights – Learning from Lawsuits, a monthly email newsletter for ED physicians. The goal of MMI-LFL is to improve patient safety, educate physicians, and reduce the cost and stress of medical malpractice lawsuits. To opt in to the free subscriber list, click here.
Chuck Pilcher, MD, FACEP
Editor, Med Mal Insights
Transverse myelitis (TM) leaves patient quadriplegic
A melodramatic attorney and a wheelchair-bound patient in the courtroom leads to $8 million settlement.
Facts: A 34-year-old previously healthy and athletic security guard collapses suddenly in his driveway at home and is taken to the ED. He is briefly evaluated, diagnosed with stress and muscle aches and discharged 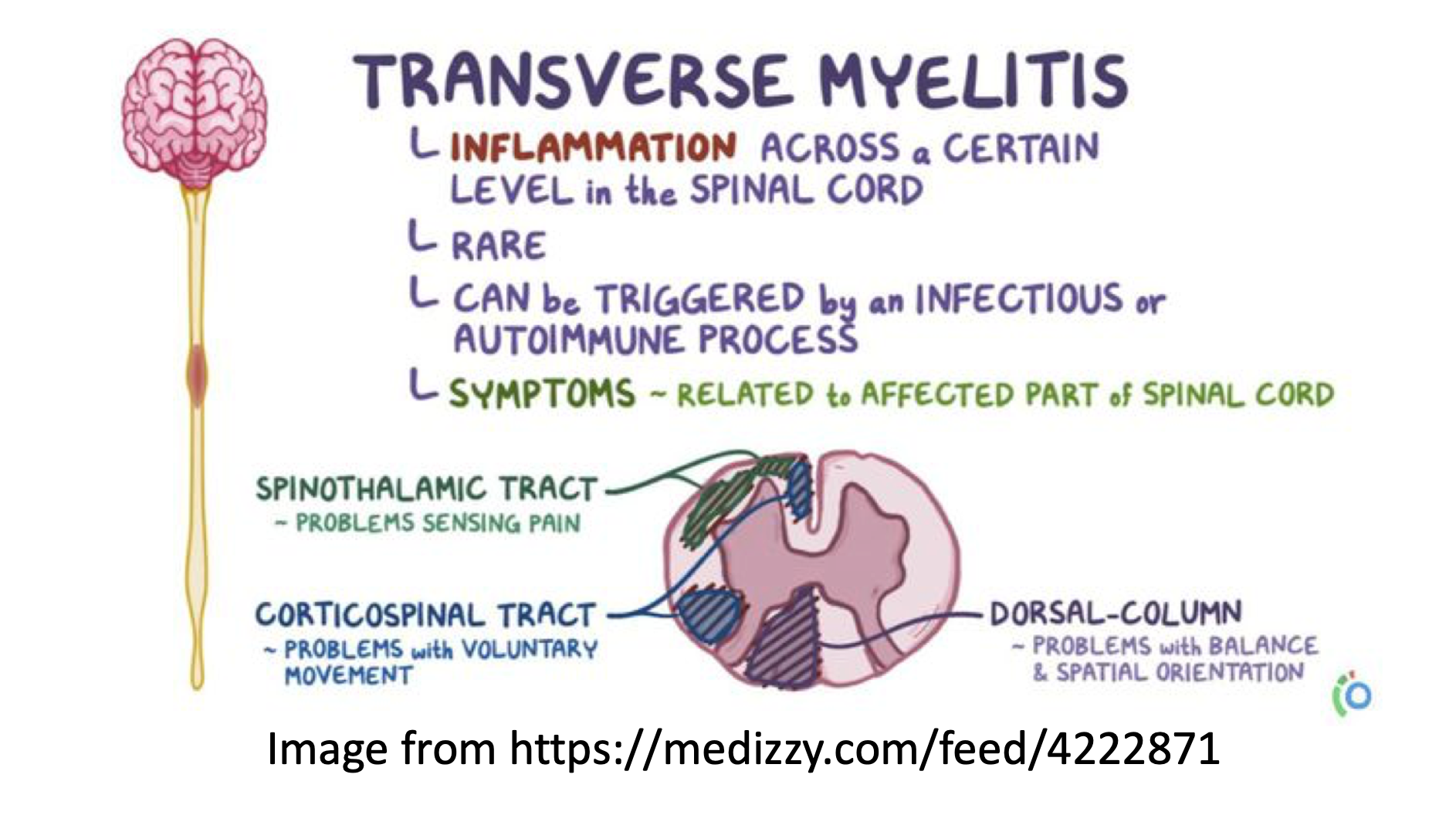 with instructions to follow up with his PCP if not improving. Over the next month, he becomes increasingly weak, but does not seek follow-up. He falls again and is returned to the hospital where he is diagnosed with transverse myelitis (TM). Despite treatment, he is left quadriplegic. He seeks legal advice, and a lawsuit is filed against the EP and the hospital. The case goes to trial.
with instructions to follow up with his PCP if not improving. Over the next month, he becomes increasingly weak, but does not seek follow-up. He falls again and is returned to the hospital where he is diagnosed with transverse myelitis (TM). Despite treatment, he is left quadriplegic. He seeks legal advice, and a lawsuit is filed against the EP and the hospital. The case goes to trial.
Plaintiff: You should have diagnosed my client’s TM on his first visit. TM is a horrible disease. My client’s “immune system rebelled… and attacked his spinal cord like a foreign invader, and 100 million forest fires started at the same time.” [Yes, the attorney said that.] Just look at this video of him having to have his mother give him a bath! [Yes, a bath video was shown to the jury.] You should have made the diagnosis when he came to the ER the first time. If you’d have done an MRI, the TM would have been found. If you’d have found it, you should have treated him with steroids, and he’d be fine today. Now you owe him $20 million for missing this life-changing diagnosis.
Defense: TM is an extremely rare condition. It occurs in about 5 people out of a million each year. The EP’s care was reasonable. You spent a month getting worse and did nothing about it. Yes, maybe an MRI would have helped, but it’s normal in in up to 40% of TM cases, especially in the first hours of the disease. Yes, high-dose steroids and other options could have been tried, but no treatment has been proven to make a major difference. Your case was in its early stages on the first visit and evidence for any treatment is only Class 2C. Grade C evidence has no good randomized controlled studies to support it, i.e., a “very weak” recommendation that’s little more than a “suggestion.” Tx doesn’t work for every patient. Benefits and risks must be balanced and are uncertain. And even if treated, only 1/3 of individuals recover with few or only minor symptoms. Another 1/3 have some permanent disability and 1/3 are left severely disabled. The outcome is worst in patients with rapid onset of symptom like your client. So, you can’t say beyond a reasonable doubt that your client’s outcome would have been good. Our care was not negligent. Even if it were, you cannot say the delayed diagnosis changed the outcome.
Result: After 4 1/2 years of litigation and several days of trial, the treating EP, an independent contractor, was removed from the suit. The matter was then settled during jury deliberations by the hospital for $8 million.
Takeaways:
- Because of its rarity, transverse myelitis will always be missed if one fails to consider it.
- Neuro symptoms associated with back pain should make one think of spinal epidural abscess. Neuro symptoms with little or no back pain should put TM on the differential.
- The defense in this case was very strong and the outcome rather surprising.
- At best, this seems to be a “loss of chance” case, i.e., the plaintiff had lost the opportunity for a better outcome.
- There is no clear protocol that assures a good recovery in patients with TM and little evidence that an earlier MRI and/or treatment would have helped.
- The mere presence of a quadriplegic who is represented by a melodramatic attorney in the courtroom can indeed sway a jury.
References:
- Misdiagnoses leaves ex-security guard a quadriplegic. Michaud S. MyLANews.com. January 30, 2017. https://mynewsla.com/crime/2017/01/30/misdiagnoses-leaves-ex-security-guard-a-quadriplegic-victim-just-wants-to-walk/
- Diagnosis and Treatment of Transverse Myelitis-A New Guideline. Wilner A. Wilner on Neurology. Feb 29, 2012. http://boards.medscape.com/forums/?128@@.2a2fc19e!comment=1
- Transverse Myelitis. Siegel Rare Neuroimmune Association (SRNA). https://wearesrna.org/living-with-myelitis/disease-information/transverse-myelitis/prognosis-management/
- Transverse Myelitis Information Sheet. The Transverse Myelitis Association. www.myelitis.org http://files.wearesrna.org/resources/Information_Sheets/About_TM.pdf






