Author: Cliffe Kwon, MD (Resident Physician, UT Southwestern University/Parkland Memorial Hospital); Steven Field, MD (@EMFieldDoc, Assistant Professor of EM, UT Southwestern University/Parkland Memorial Hospital) // Edited by: Stephen Alerhand, MD (@SAlerhand Assistant Professor, Rutgers New Jersey Medical School)
Introduction
A 20-year-old healthy male presents to your emergency department complaining of right shoulder pain that occurred during a pick-up basketball game 20 minutes prior to arrival. He was blocking a shot when he suddenly felt a sharp pain in his right shoulder. He has an obvious shoulder deformity and is holding his arm in internal rotation close to his body.
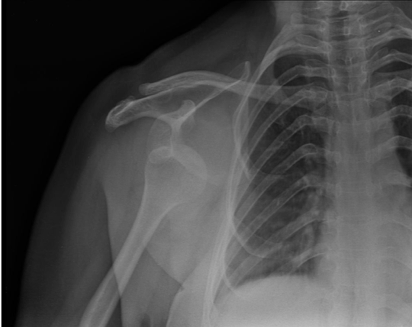
Case courtesy of Dr Maulik S. Patel, httpL//radiopaedia.org/cases/13397
You think: “What are my alternatives to procedural sedation for providing adequate muscle relaxation and analgesia to maximize my chances of successfully reducing this shoulder?”
(See this post for using US to diagnose and confirm reduction of shoulder dislocations.)
The Ultrasound-Guided Interscalene Block
The interscalene block of the brachial plexus has been used since the 1970’s for rotator cuff and other shoulder surgeries. Underhill et al performed 30 interscalene blocks for dislocations in the Emergency Department. Out of 30 cases, 26 were successfully reduced without additional analgesia or sedation, or complications as well. Blaivas et al performed 42 interscalene blocks and shoulder reductions. They found that using a nerve block significantly reduced the length of stay (average 177 mins. vs 100 mins).
Block Setup
- 20-22 gauge spinal needle
- 25 gauge needle
- 3 cc syringe, 10 cc syringe
- Lidocaine with epinephrine
Positioning
- Have the patient’s head turned to the contralateral side about 30 – 45 degrees.
- Place machine on opposite side of patient. Skin, transducer, and screen should all be within the same line of sight.
- Start in the supraclavicular fossa with your transducer placed transversely. Find the subclavian artery and brachial plexus next to it.

- Follow the postero-lateral border of the SCM until the anterior and middle scalene muscles form.
- Scan cephalad until you identify the C5, C6, C7 nerve roots (“stoplight sign”).
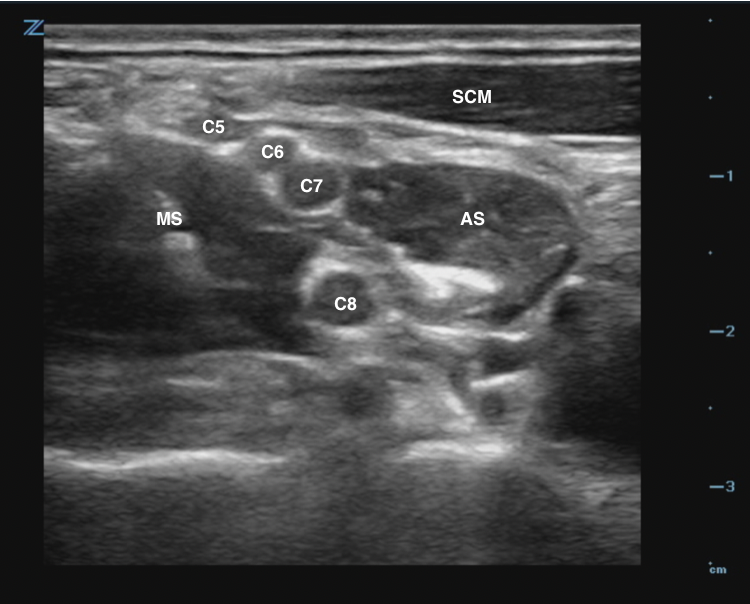
- Use color Doppler to find and avoid the transverse cervical artery.
- Approach in-plane view (ie. visualizing the entire needle length) lateral to medial in the interscalene groove.
- Inject ~ 20 cc of anesthetic near C5-7 with the anesthestic appearing as hypoechoic fluid extent of spread of anesthetic.

- Wait 10-15 minutes and reduce using your desired technique.
Potential Pitfalls
- Vascular puncture
- Use color Doppler to identify vessels.
- Nerve injury
- Use non-cutting or spinal needle.
- Phrenic nerve block causing diaphragmatic paralysis
References
- Blaivas, Michael. “A Prospective Comparison of Procedural Sedation and Ultrasound-Guided Interscalene Nerve Block for Shoulder Reduction in the Emergency Department.” Academy of Emergency Medicine, 18, no. 9, Sept. 2011, pp. 922-927.
- Blaivas, Michael. “Ultrasound-Guided interscalene block for shoulder dislocation reduction in the ED.” American Journal of Emergency Medicine, vol. 24, 2006, pp. 293-296.
- “Interscalene.” Highland EM Ultrasound Fueled pain management, highlandultrasound.com/interscalene-block/. Accessed 16 Sept. 2017.
- USRA – Interscalene Block, usra.ca/regional-anesthesia/specific-blocks/upper-limb/interscaleneblock.php. Accessed 16 Sept. 2017
- Underhill TJ, Wan A, Morrice M. “Interscalene brachial plexus blocks in the management of shoulder dislocations.” Arch Emerg Med. 6, no 3, 1989, pp. 199-204.





