Author: Taylor Guinn, MD (EM Resident Physician, UT Southwestern, Dallas, TX) // Reviewed by: Alex Koyfman, MD (@EMHighAK); Brit Long, MD (@long_brit); Cynthia Santos, MD
Welcome to EM@3AM, an emDOCs series designed to foster your working knowledge by providing an expedited review of clinical basics. We’ll keep it short, while you keep that EM brain sharp.
A 42-year-old female with a past medical history of iron deficiency anemia presents to the ED with an uncomplicated peritonsillar abscess. You give 2 benzocaine sprays and successfully aspirate the abscess. As she is waiting for her discharge paperwork, the nurse alerts you that her oxygen saturation is now in the mid-80s. Repeat vitals in the room are as follows: BP 102/78, HR 102, O2 85%, RR 24.
On physical exam, she is in moderate respiratory distress with tachypnea and subcostal retractions. She has perioral cyanosis that was not seen on your initial exam. What is the diagnosis and best next step?
Answer: Methemoglobinemia; obtain methemoglobin level and give methylene blue1,2
Background:
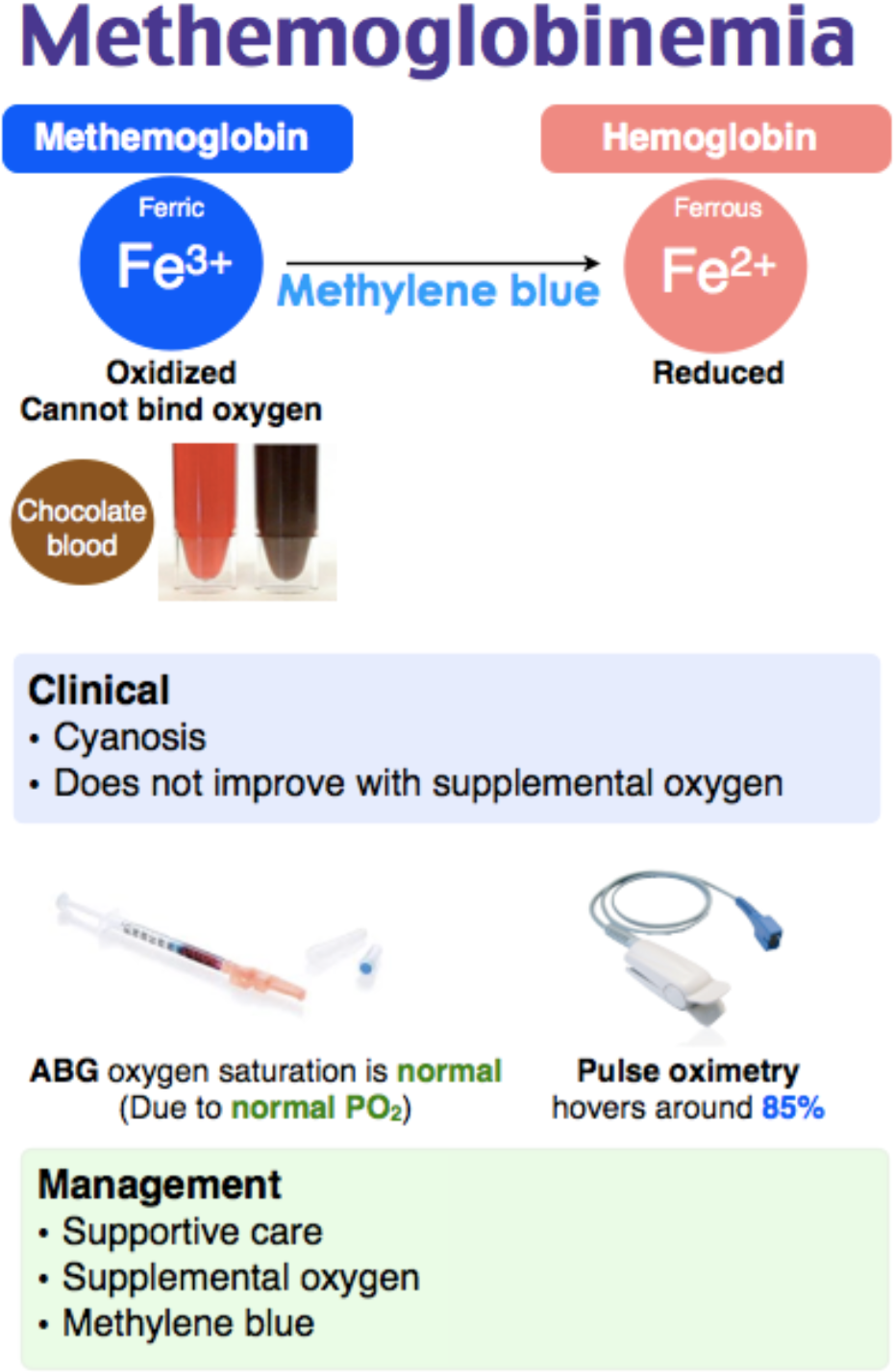
- Oxygen is able to bind normal hemoglobin while it is in the ferrous state (2+).
- Methemoglobin is an oxidized form of hemoglobin in which the heme iron configuration has been converted from ferrous (2+) to ferric (3+) thus it cannot bind to oxygen.
- The ferric heme causes the remaining normal ferrous hemes to have an increased affinity for O2, pushing the oxygen dissociation curve to the left and making it more challenging for oxygen to be delivered to tissues.3
- A functional anemia results from the inability to bind oxygen and the resulting left shift of the oxygen dissociation curve.
- Normally we have ~1-3% methemoglobin in our blood and physiologic mechanisms to convert methemoglobin back to hemoglobin. When these mechanisms are overwhelmed, clinically apparent methemoglobin develops and can lead to death if untreated.

- Methemoglobinemia is either congenital or acquired. There are compensation mechanisms for congenital methemoglobinemia, thus other than an undesirable cosmesis it is unlikely to be fatal unless there is an additional predisposing event.1 Therefore, this discussion will focus on recognizing and treating acquired methemoglobinemia.
- How rare is methemoglobinemia?
- Very rare—around 100 cases requiring methylene blue each year.2
- <0.1% incidence when using benzocaine.5,6
- A study with 28478 patients receiving benzocaine prior to TEE found 19 patients developed methemoglobinemia.5 Another retrospective study involving 94694 procedures using benzocaine reported 33 cases of methemoglobinemia.6 Those who developed methemoglobinemia were more likely to be anemic and have sepsis at the time of TEE.
Clinical presentation:
- Classically, a pulse oximeter will read ~85% in a patient with clear lungs that doesn’t improve with supplemental O2 after use of a substance that is associated with development of methemoglobinemia. 2
- The severity of symptoms ranges from mild dyspnea, cyanosis and/or headache to overt shock. Symptom severity is roughly correlated with percentage of methemoglobin.
- Cyanosis typically becomes apparent when total methemoglobin (total hemoglobin x % methemoglobin) is >1.5 g/dL. 1,7
- For example, a patient with a hemoglobin of 10 g/dL will likely become cyanotic when methemoglobin percentage is roughly 15%, and a patient with a hemoglobin of 5 g/dL will likely become cyanotic around 30% methemoglobin.
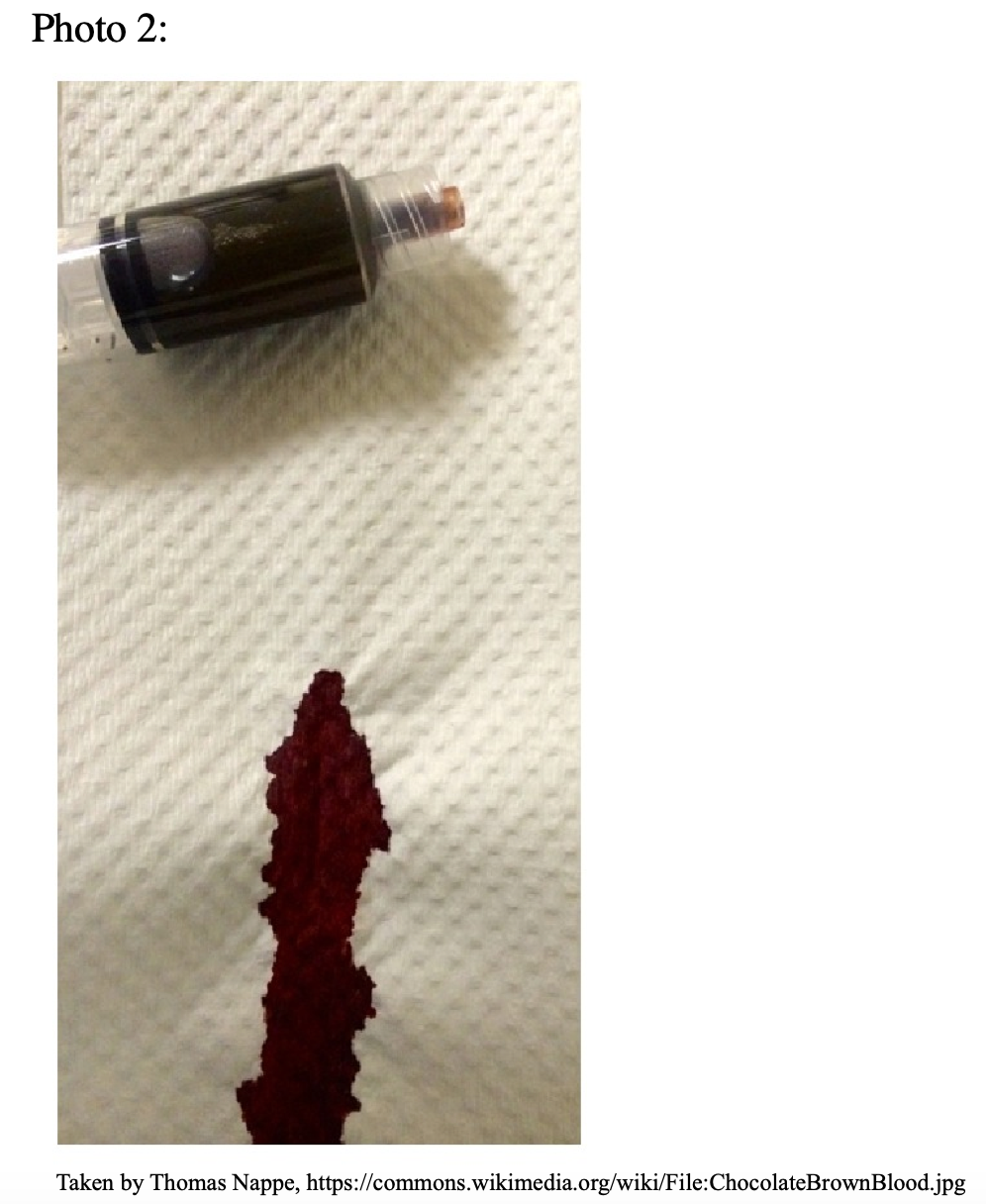
- Patients with methemoglobinemia will typically have brown blood.
Evaluation:
- Once you suspect methemoglobinemia you can measure the methemoglobin level.
- How to detect methemoglobin:
- VBG or ABG (both give same result for methemoglobin level) in a fresh sample of blood. Methemoglobin levels increase with prolonged storage. With some POC ABGs you will need to specifically order a methemoglobin level; this is laboratory dependent.1,2
- Co-oximetry will detect absorption of methemoglobin at 630 nm.8
- Rad-57 co-oximeter9,10 and a direct assay (Evelyn-Malloy method)1, although these may be less available depending on institution.
- Caution on estimating oxygen level:
- Routine pulse oximetry is misleading because methemoglobin absorbs light at the pulse oximeter’s two wavelengths which results in an erroneous estimation of true % deoxy- and oxy- hemoglobin, thus causing the pulse oximeter to falsely read around 85%.11
- PaO2 readings on blood gases may be falsely elevated despite serious methemoglobinemia. This is because the PaO2 reflects the amount of oxygen available in blood, although methemoglobin cannot bind and transport it.1
- This discrepancy in the PaO2 and pulse oximetry may result in a large PaO2-saturation gap that points to a hemoglobinopathy.
Management:
- Remove exposures if possible.
- Supportive care (IV access, hydration or ventilation if necessary).
- Treat anyone who is symptomatic (vital sign abnormality, acidosis or signs of end organ damage) or anyone who has a methemoglobin level >25%.1,2
- Give methylene blue which allows reduction of methemoglobin back to hemoglobin.
- Dose of methylene blue: 1-2 mg/kg (0.1-0.2 mL/kg of 1% solution) as a slow push over 5 minutes to decrease pain of infusion.2,12
- Start with 1 mg/kg for mild symptoms and 2 mg/kg for more severe symptoms
- Symptoms should resolve in minutes. If there is no response in 1 hour, can give a repeat dose. If they do not respond or get worse with ~2 mg/kg, consider G6PD deficiency (below) or an alternative diagnosis.
- Methylene blue treatments at >7 mg/kg can cause side effects like nausea, vomiting, shortness of breath. At much higher levels, methylene blue can paradoxically worsen methemoglobinemia.1,13
- Caution on use of methylene blue in patients on SSRIs as methylene blue is a MAOI. There have been case reports of death in patients on serotonergic antidepressants.14
- Differences for those with G6PD deficiency15:
- Methylene blue may be ineffective or even cause hemolysis. If a patient has G6PD deficiency, you will need to consider alternative treatments including:
- Administration of an alternative reducing agent like vitamin C. There are case reports of patients treated with high doses of vitamin C (~1-5 g q 6 hour). When using vitamin C, the methemoglobinemia usually takes >24 hours to fully correct.2,16,17
- Exchange transfusion18 and hyperbaric oxygen.19 Persistent methemoglobinemia can be treated with blood transfusion; this is most likely helpful if the patient is also anemic.1
A note on kids:
- Infants <3 months old are more susceptible to methemoglobinemia due to fetal hemoglobin being more easily oxidized and children having ~60% activity of cytochrome b5 reductase.20
- Well-water with high levels of nitrates poses a high risk of methemoglobinemia in kids, called “blue baby syndrome.”1
- Enteritis-associated methemoglobinemia can be present in over 60% of infants with severe diarrhea.21,22
Disposition:
- Depends on the severity and rate of improvement. Depending on the substance and degree of ingestion, may see rebound methemoglobinemia within 12 hours.1
- Can discuss with a toxicologist or poison control.
- If a patient is improving there is not a need to recheck the methemoglobin level.2
- If you give methylene blue and reorder a co-oximetry test, you will get a false value because the dye interferes with proper methemoglobin analysis.1
Pearls:
- While rare, it is important to be aware of causative factors for methemoglobinemia, with topical anesthetics being the most common precipitant in the ED.
- Treat with methylene blue if a patient is symptomatic or has a methemoglobin level >25%.
- Methylene blue dose is 1-2 mg/kg given over a 5 minute slow push.
- Improvement and disposition should be dictated by clinical examination, not repeat methemoglobin testing.

A previously healthy 7-month-old boy presents to the ED with new onset of cyanosis and fatigue first noticed this morning. The child was recently treated for thrush and his parents have been using over the counter benzocaine for teething. The child is sleepy but easily awakens and cries. He is not in respiratory distress. The only vital sign abnormalities include a heart rate of 190 beats per minute at rest and oxygen saturation of 82% on room air. Placement of a non-rebreather facemask does not improve the patient’s oxygenation. After confirming the diagnosis, which of the following treatments is indicated?
A) Congenital heart surgery
B) Heparin
C) Methylene blue
D) Sodium thiosulfate
Answer: C
Methemoglobinemia occurs when the iron associated with hemoglobin is changed through oxidation from a ferrous (Fe2+) to a ferric (Fe3+) state thus preventing the hemoglobin from binding oxygen. Patients with congenital methemoglobinemia generally have lifelong cyanosis but are otherwise asymptomatic. Substances known to cause acquired methemoglobinemia include dapsone and topical anesthetics, especially mucous membrane use of benzocaine, although it has been reported with lidocaine, tetracaine, or prilocaine use. Most reported cases are thought to be due to high doses or a break in the mucosal barrier such as by mucositis or thrush. Treatment for methemoglobinemia includes removing the offending agent, and if symptomatic, administering methylene blue which activates a non-physiologic NADPH pathway for faster reduction of the iron molecule.
Congenital heart surgery (A) would be indicated for a congenital heart defect such as Tetralogy of Fallot which can cause hypoxia in this age group, but is generally associated with fussiness or agitation during a “tet spell.” Heparin (B) would be indicated for a pulmonary embolism, however this typically does not present in this age group and is also generally associated with a family history, trauma, infection, or a central line. Sodium thiosulfate (D) is used for cyanide poisoning, not for methemoglobinemia.
Further Reading:
FOAM Resources
https://wikem.org/wiki/Methemoglobinemia
https://www.emrap.org/corependium/chapter/recMQJ3w4jFN4Y3rR/Methemoglobinemia
References
- Prchal J. Methemoglobinemia. UpToDate. https://www.uptodate.com/contents/methemoglobinemia. Published 2020.
- Katz K, Amaducci A. Methemoglobinemia. EM:RAP. https://www.emrap.org/corependium/chapter/recMQJ3w4jFN4Y3rR/Methemoglobinemia. Published 2020. Mack E. Focus on diagnosis: co-oximetry. Pediatr Rev. 2007;28(2):73-74. doi:10.1542/pir.28-2-73
- Darling RC, Laboratory FF, Roughton FJW, Baines AD. The Effect of Methemoglobin on the Equilibrium Between Oxygen and Hemoglobin. American Journal of Physiology-Legacy Content. https://journals.physiology.org/doi/abs/10.1152/ajplegacy.1942.137.1.56. Published August 1, 1942.
- Elahian F. Human cytochrome b5 reductase: structure, function, and potential applications. Critical reviews in biotechnology. https://pubmed.ncbi.nlm.nih.gov/23113554/.
- Kane GC. Benzocaine-induced methemoglobinemia based on the Mayo Clinic experience from 28 478 transesophageal echocardiograms: incidence, outcomes, and predisposing factors. Archives of internal medicine. https://pubmed.ncbi.nlm.nih.gov/17923598/.
- Chowdhary S, Bukoye B, Bhansali AM, et al. Risk of topical anesthetic-induced methemoglobinemia: a 10-year retrospective case-control study. JAMA Intern Med. 2013;173(9):771-776. doi:10.1001/jamainternmed.2013.75
- Price DP. Methemoglobin Inducers. In: Nelson LS, Howland M, Lewin NA, Smith SW, Goldfrank LR, Hoffman RS. eds. Goldfrank’s Toxicologic Emergencies, 11e. McGraw-Hill
- Mack E. Focus on diagnosis: co-oximetry. Pediatr Rev. 2007;28(2):73-74. doi:10.1542/pir.28-2-73
- Feiner JR, Bickler PE, Mannheimer PD. Accuracy of methemoglobin detection by pulse CO-oximetry during hypoxia. Anesth Analg. 2010;111(1):143-148. doi:10.1213/ANE.0b013e3181c91bb6
- Annabi EH, Barker SJ. Severe methemoglobinemia detected by pulse oximetry. Anesth Analg. 2009;108(3):898-899. doi:10.1213/ane.0b013e318172af73
- Barker SJ, Tremper KK, Hyatt J. Effects of methemoglobinemia on pulse oximetry and mixed venous oximetry. Anesthesiology. 1989;70(1):112-117. doi:10.1097/00000542-198901000-00021
- Kearney TE, Manoguerra AS, Dunford JV Jr. Chemically induced methemoglobinemia from aniline poisoning. West J Med. 1984;140(2):282-286.
- Goluboff N, Wheaton R. Methylene blue induced cyanosis and acute hemolytic anemia complicating the treatment of methemoglobinemia. J Pediatr. 1961;58:86-89. doi:10.1016/s0022-3476(61)80064-4
- Zuschlag ZD, Warren MW, K Schultz S. Serotonin Toxicity and Urinary Analgesics: A Case Report and Systematic Literature Review of Methylene Blue-Induced Serotonin Syndrome. Psychosomatics. 2018;59(6):539-546. doi:10.1016/j.psym.2018.06.012
- Rosen PJ, Johnson C, McGehee WG, Beutler E. Failure of methylene blue treatment in toxic methemoglobinemia. Association with glucose-6-phosphate dehydrogenase deficiency. Ann Intern Med. 1971;75(1):83-86. doi:10.7326/0003-4819-75-1-83
- Reeves DJ, Saum LM, Birhiray R. I.V. ascorbic acid for treatment of apparent rasburicase-induced methemoglobinemia in a patient with acute kidney injury and assumed glucose-6-phosphate dehydrogenase deficiency. Am J Health Syst Pharm. 2016;73(9):e238-e242. doi:10.2146/ajhp150591
- Rehman A, Shehadeh M, Khirfan D, Jones A. Severe acute haemolytic anaemia associated with severe methaemoglobinaemia in a G6PD-deficient man. BMJ Case Rep. 2018;2018:bcr2017223369. Published 2018 Mar 28. doi:10.1136/bcr-2017-223369
- Patnaik S, Natarajan MM, James EJ, Ebenezer K. Methylene blue unresponsive methemoglobinemia. Indian J Crit Care Med. 2014;18(4):253-255. doi:10.4103/0972-5229.130582
- Goldstein GM, Doull J. Treatment of nitrite-induced methemoglobinemia with hyperbaric oxygen. Proc Soc Exp Biol Med. 1971;138(1):137-139. doi:10.3181/00379727-138-35846
- Eng LI, Loo M, Fah FK. Diaphroase activity and variants in normal adults and newborns. Br J Haematol. 1972;23(4):419-425. doi:10.1111/j.1365-2141.1972.tb07076.x
- Methemoglobinemia: Select 5-Minute Pediatrics Topics. Methemoglobinemia | Select 5-Minute Pediatrics Topics. https://www.unboundmedicine.com/5minute/view/Select-5-Minute-Pediatric-Consult/14050/all/Methemoglobinemia.
- Babbitt, CJ et al. Diarrhea and methemoglobinemia in an infant : Pediatric Emergency Care. LWW. https://journals.lww.com/pec-online/Citation/2000/12000/Diarrhea_and_methemoglobinemia_in_an_infant.10.aspx.









1 thought on “EM@3AM: Methemoglobinemia”
Pingback: Quiz 92, November 27th, 2020 – The FOAMed Quiz