Authors: Zachary Sletten, MD (EM Attending, Brooke Army Medical Center) and Simon Sarkisian, DO (EM Attending, Cooper University Hospital/US Army, Camden, NJ) // Reviewed by: Alexander Y. Sheng, MD, MHPE (@theshenger); Alex Koyfman, MD (@EMHighAK); Brit Long, MD (@long_brit)
You are a busy emergency medicine (EM) attending physician, and you hear about a facial laceration that just checked in. The intern asks you for help repairing the laceration, and you eagerly accompany them into the room excited to endow them with your wisdom on laceration repair. After stepping into the room, you realize you might be in over your head (no pun intended). This is not your run of the mill facial laceration.
The series will review the repair of head, eyes, ears, nose, and throat (HEENT) lacerations, with a focus on the areas where emergency physicians tend to struggle. Today we look at nasal lacerations.
Case
A 31-year-old male presents after an ATV accident in which he was ejected resulting in facial contusions and a nasal laceration transecting his ala. You inspect for signs of a septal hematoma and begin to consider methods for closure and wonder if you are in over your head.
Nasal Lacerations
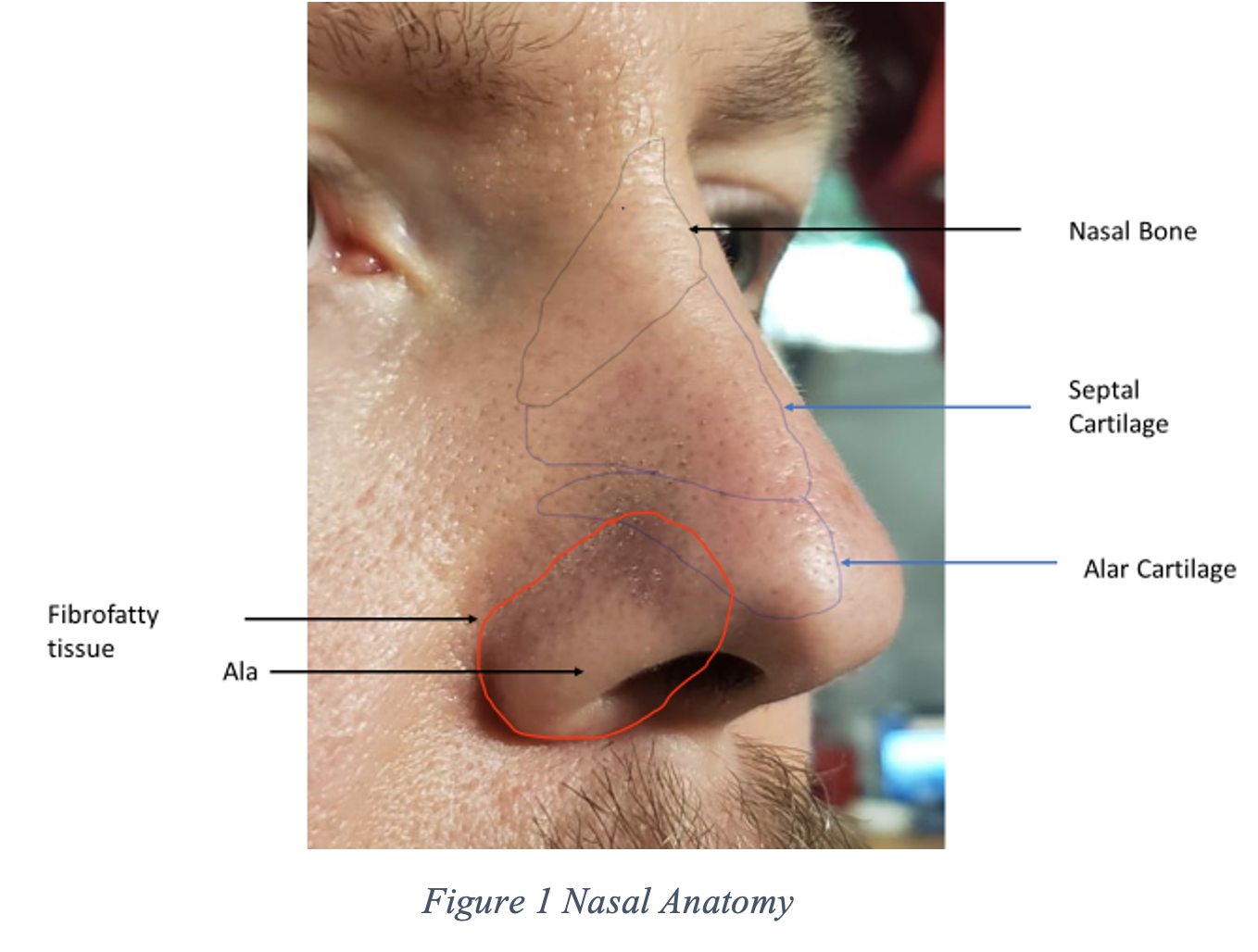
As mentioned in the case presentation, be sure to evaluate for septal hematoma after nasal trauma. Simple lacerations can be closed with 6-0 non-absorbable sutures. For incisions that extend through the alar margin (see Figure 1), begin by aligning the margin with a 5-0 non-absorbable suture leaving the sutures untied until the end, applying gentle traction as you continue to repair the mucosal and skin surfaces to ensure alignment1. Proceed to repair the mucosal surface with 5-0 absorbable sutures. Generally, the cartilage does not need to be repaired if involved. Finish the repair by suturing the remainder of the skin with 6-0 absorbable sutures. Be sure to irrigate between layers. Infraorbital nerve blocks are an excellent method of achieving anesthesia6 as are lidocaine-soaked cotton swabs in the nasal mucosa7. Typically, the infraorbital foramen is in line with the pupil when the patient has a forward gaze, and although the foramen may not be palpable, it is present immediately under the easily palpated infraorbital ridge. The 25- or 27-gauge needle is inserted parallel to and at the level of the second maxillary premolar and advanced approximately 2.5 cm; injection is adjacent to the foramen4,5. and is depicted in Figures 2, 3, and 4 below. For lacerations overlying a suspected palpable fracture or bony deformity, or for considerable tissue injury, consider involving a surgeon6.



Stay tuned for our next piece in the series on repair of eyelid lacerations.
References/Further Reading
1. Tintinalli JE, Ma OJ, Yealy DM, et al. Tintinalli’s emergency medicine: a comprehensive study guide. 2020.
2. Hollander JE, Richman PB, Werblud M, Miller T, Huggler J, Singer AJ. Irrigation in facial and scalp lacerations: does it alter outcome? Ann Emerg Med 1998;31:73-7.
3. Singer AJ, Gulla J, Hein M, Marchini S, Chale S, Arora BP. Single-layer versus double-layer closure of facial lacerations: a randomized controlled trial. Plast Reconstr Surg 2005;116:363-8; discussion 9-70.
4. Farion KJ, Russell KF, Osmond MH, et al. Tissue adhesives for traumatic lacerations in children and adults. Cochrane Database of Systematic Reviews 2002.
5. Holger JS, Wandersee SC, Hale DB. Cosmetic outcomes of facial lacerations repaired with tissue-adhesive, absorbable, and nonabsorbable sutures. Am J Emerg Med 2004;22:254-7.
6. Walls RM, Hockberger RS, Gausche-Hill M. Rosen’s emergency medicine: concepts and clinical practice2018.
7. Sabatino F, Moskovitz JB. Facial wound management. Emerg Med Clin North Am 2013;31:529-38.





