Author: Dustin Taliaferro, DO (EM Resident Physician, UT Southwestern, Dallas, TX) // Reviewed by: Cynthia Santos, MD (@Cynthia Santos, MD); Alex Koyfman, MD (@EMHighAK); Brit Long, MD (@long_brit)
Welcome to EM@3AM, an emDOCs series designed to foster your working knowledge by providing an expedited review of clinical basics. We’ll keep it short, while you keep that EM brain sharp.
A 30-year-old male presents to the emergency department with intense left forearm pain after cleaning an aquarium at his job 20 minutes prior to arrival. He is unsure what kind of fish were in the aquarium. The pain has been constant since onset. He does not endorse any nausea, vomiting, headache or weakness to his left arm. He denies any medical problems.
Initial vital signs: BP 122/82, HR 102, T 98.2 Oral, RR 16, SpO2 98% on RA. Physical exam reveals a patient who appears uncomfortable holding his left arm. He is A&OX3. His lungs and heart are normal. There is a 5 cm area of erythema to his anterior forearm that is warm to the touch. Radial pulses are 2+.
What is the diagnosis and the best next step in management?
Answer: Marine animal injury; treatment – hot water immersion
Background: Human contact with species of venomous marine life are relatively common especially in tropical and coastal regions of the world. Common organisms include spiny fish, cone snails, jelly fish, sea snakes, octopi and stingrays. There is an estimated 10 million envenomations worldwide, most being caused by jellyfish. Most of these animals do not inhabit US waters. It is important to know what the common organisms are based on region to determine if an envenomation can be potentially fatal. While most of these envenomations are relatively mild, there are fatal organisms that are most commonly in Australian and Pacific waters.
- Envenomations can be broken down into three classes based on mechanism of delivery: stingers, nematocysts and bites
Stingers
Rays: Rays are a member of the class Chondrichthyes. Families in this class include sting rays, whip rays, skates, round rays, eagle rays, butterfly rays and freshwater rays. There are 11 different species of sting rays in US coastal waters. It is estimated that 1500 to 2000 ray injuries occur in the US every year. A majority of these injuries occur when the ray is stepped on. Deaths from these envenomations typically occur from hemorrhagic abdominal trauma, organ puncture or tetanus.

- Envenomation:
- Rays possess a tail that is covered with retroverted spines. There is a ventrolateral groove that contains venom and saturates the spines. The venom is made up of heat labile polypeptides. The ray venom causes local vasoconstriction that can cause necrotic tissue. Typically, a single puncture wound is found on the top or side of the foot. Stepping on a ray causes the ray’s tail to whip and contact the person. Intense pain out of proportion to the wound is usually observed. Peak onset of symptoms is 30 to 90 minutes after initial injury and may last for 48 hours. Wounds may progress to a hemorrhagic necrosis and possibly necrotizing fasciitis.
- Symptoms from the venom cause weakness, nausea, vomiting, diarrhea, headache, syncope, seizures, muscle cramps, hypotension and dysrhythmias.
- Management:
- Radiographs for retained spine
- Wound irrigation, tetanus prophylaxis
- Consider antibiotics covering skin flora and aquatic organisms
- Hot water immersion (43C-45C) relieves pain and inactivates venom
- Observe for 3-4 hours for systemic symptoms
- Disposition:
- Discharge if no systemic symptoms after 2 hours of observation
- Admit for compartment syndrome, skin necrosis or NSTI
Bony Fish: Bony fish are classified under the family Scorpaenidae have several venomous species. Some of the more common species include lionfish, stonefish, scorpionfish, weevers and catfish. People at high risk for these envenomations include fishermen, waders and aquarium handlers. There are very few deaths associated with Scorpaenidae with only five reported. Scorpaenidae have 12-13 dorsal, 2 pelvic and 3 anal spines covered by an integumentary sheath. Stings occur from direct contact with spines on the fish. Venom from these spines can remain toxic for 24-48 hours even after death.
- Lionfish and Scorpionfish: These stings are common in aquarium enthusiasts. They are the most common poison center call for bony fish stings in the US. Due to their popularity in the US, Lionfish have become an invasive species in US Caribbean waters. They have no known natural predators which allows them to thrive and disrupt coral ecosystems. Immediately following a sting, the victim experiences intense pain and if left untreated can last up to 48 hours. The area becomes warm, erythematous, and edematous with vesicles.

- Stonefish: Stonefish are commonly found in coastal Australia. They are disguised to accommodate living on the rocky sea bottom. Stings from stonefish are the most severe in this category. The area of the sting becomes immediately painful and erythema can progress up the effected extremity. Although pain typically subsides in 6-12 hours, it can last for several days. Signs of systemic toxicity include headache, vomiting, abdominal pain, delirium, seizures, limb paralysis, arrhythmia, congestive heart failure and hypotension.
- Weevers: Weever stings are common in Italian coastal towns. They inhabit shallow temperate waters in the eastern Atlantic and Mediterranean.
- Catfish: Most species of catfish live in freshwater but marine catfish that can inflict injury inhabit tropical Indo-Pacific waters.
- Management:
- Management for all bony fish is centered around hot water immersion to inactive venom, removal of retained spines and pain control
- Copious wound irrigation and inspection/radiographs for retained spines
- Oral analgesia and local injection of lidocaine for pain
- Consider antibiotic prophylaxis with coverage for vibrio parahaemolyticus such as doxycycline, trimethoprim-sulfamethoxazole, third-generation cephalosporins (cefotaxime and ceftazidime), aminoglycosides (gentamicin and amikacin) and fluoroquinolones
- Address tetanus immunization status
- There is an antivenom for stonefish stings that is used for systemic symptoms or pain refractory to first aid
- Observe for anaphylactic reaction to antivenom
- Disposition:
- Discharge after 2 hours observation if no systemic symptoms
- Stonefish envenomations will need ICU level care if systemic symptoms
Echinodermata, Annelida, and Porifera: The Echinodermata phylum include sea stars, sea urchins, sand dollars and sea cucumbers. The Annelida phylum include segmented worms such as the bristle worm. The Porifera phylum include sponges. These are slow moving or sessile creatures that live on the ocean floor where envenomation happens passively by people stepping on the animals or mistakenly handling them.
- Echinodermata
- Sea urchins are covered in spines and pedicellariae (pincer-like appendages used for feeding, cleaning and defense). Wounds with more pedicellariae are generally more severe due to the pedicellariae containing more venom and being harder to remove. The venom found in sea urchins consist of steroid glycosides, serotonin, hemolysin, protease and acetylcholine-like substances.
- Most injuries from sea urchins are mild. Burning with local irritation and erythema occur at the site of envenomation. A Pacific Ocean urchin, Tripneustes, has a neurotoxin that can affect cranial nerves.
- Sea urchins are covered in spines and pedicellariae (pincer-like appendages used for feeding, cleaning and defense). Wounds with more pedicellariae are generally more severe due to the pedicellariae containing more venom and being harder to remove. The venom found in sea urchins consist of steroid glycosides, serotonin, hemolysin, protease and acetylcholine-like substances.

-
- Sea star envenomations are usually less severe than urchins due to sea stars having short and blunt spines. The Crown-of-Thorns sea star has longer spines that contain a toxic saponin venom with hemolytic and anticoagulant properties.
- Small cuts on the foot or hands from sea stars can lead to contact dermatitis. The Crown-of-Thorns species may cause nausea, vomiting and muscle paralysis.
- Sea cucumbers excrete holothurin from their anus as a defense mechanism. This toxin inhibits neural conduction in fish. Sea cucumbers can also eat jellyfish and subsequently excrete their toxin.
- Contact with sea cucumbers cause a mild dermatitis. Scleral or corneal contact can cause several corneal inflammation and blindness.
- Sea star envenomations are usually less severe than urchins due to sea stars having short and blunt spines. The Crown-of-Thorns sea star has longer spines that contain a toxic saponin venom with hemolytic and anticoagulant properties.
- Annelida
- Bristle worms have stingers that project from pseudo legs. They excrete an unknown venom.
- Contact with the bristles of bristle worms cause a mild urticarial rash.
- Bristle worms have stingers that project from pseudo legs. They excrete an unknown venom.
- Porifera
- Sponges attach to the sea floor or other coral and have elastic skeletons with projecting spicules. These spicules contain a halitoxin, okadaic acid and subcritine. Dried sponges are nontoxic but can produce toxin upon rewetting, even after years.
- Contact with certain species of sponges can cause a rash with vesicles and bullae. These symptoms usually subside within a week with skin desquamation occurring from 10 days to 2 months. Skin changes can last from months to several years. Sponges colonized with Cnidaria spp. can lead to skin necrosis (sponge diver’s disease).
- Sponges attach to the sea floor or other coral and have elastic skeletons with projecting spicules. These spicules contain a halitoxin, okadaic acid and subcritine. Dried sponges are nontoxic but can produce toxin upon rewetting, even after years.
- Management:
- Particularly for urchins and sea stars, the primary objective is venom inactivation by hot water immersion
- Irrigate sponge envenomations with cold water
- Pain control
- Radiographs to evaluate for foreign bodies
- Some urchin species have spines that contain dyes that may resemble a foreign body
- Spicule removal from sponges by adhesive tape or edge of a credit card
- Antihistamine and steroid creams may provide some relief for itching
- Consider antibiotics for severe wounds that cover skin and aquatic flora
- Disposition:
- Discharge after 2-hour observation period if no systemic symptoms
Cone Snails: Cone snails are cone-shaped with a broad conical spire at the apex. They belong to the genus Conus with about 400 species totaling in the genus. 18 of these are known to be venomous to humans. There are a reported 15 human deaths associated with cone snail stings. The fish hunting cone is the species that is most implicated in human envenomations. Envenomations typically occur when they are handled.

- Envenomation: Cone snails have a long hollow tube (proboscis) that contains a single tooth bathed in venom. When the snail detects nearby prey, the tooth is fired from the proboscis into the victim. Some specie’s venom contains a vasopressin-like peptide that is used in medical pain control for its antinociceptive properties. Cone snail stings can be very severe. The venom causes local inflammation, intense pain, tissue cyanosis and numbness. Systemic symptoms include weakness, blurred vision, aphonia, dysphagia, muscle paralysis, muscle paralysis, respiratory failure and cardiovascular collapse. Death is rapid and occurs within two hours.
- Management:
- Cone snails are widespread throughout the world, including off the Atlantic Coast of Florida. Consider these injuries in divers handling wildlife
- Airway management
- Supportive care
- Hot water immersion for pain control
- Pressure immobilization is controversial
- Tetanus prophylaxis
- Disposition: Patients without systemic signs of toxicity at 4-6 hours can be discharged. Symptoms typically take 3 days to fully recover.
Nematocysts
Nematocysts (Cnidarians): The Cnidaria phylum consist of true jellyfish, cubozoans (box jellyfish) and Physalia (Portuguese Man-of-War), sea anemones and coral. Organisms from this phylum are invertebrates that are the leading cause of lethal envenomations from marine animals worldwide. While most envenomations are nonlethal, injuries from the box jellyfish can be fatal.
- Cubozoans (box jellyfish)
- Chironex fleckeri: C. fleckeri are a species of box jellyfish that can cause cardiac arrest within minutes. They have a unique sting pattern known as the “frosted ladder” pattern that appears in a cross-hatch pattern. C. fleckeri are found in Australia and Indo-Pacific waters. Death is usually immediate within 5-20 minutes. Antivenom is needed immediately but there is controversy over efficacy.

-
- Carukia barnesi (Irukandji jellyfish): C. barnesi are characteristic in causing Irukandji Syndrome. This syndrome is characterized by muscle cramps, severe back pain, burning sensation to skin and face, headaches, nausea, restlessness, sweating, nausea, hypertension and tachycardia. Irukandji Syndrome is mediated by a catecholamine release from exposure to the toxin. C. barnesi have small bells with small tentacles. They do not leave typical serpiginous wounds on contact. This species is typically limited to Australia and the Indo-Pacific, although cases have been reported off the coast of Florida.
- Physaliidae: Members of the Physaliidae family are of the Hydrozoa class and, like the Cubozoans, are not true jellyfish. These organisms exist as floating colonies meaning the bells and tentacles are actually different organisms. They are recognized by a blue sail that floats on the surface of the water.
- Physalia physalis is known as the Portuguese man-of-war and are found on Atlantic coastlines, especially in Florida. These envenomations are common among beachgoers on the Atlantic Florida beaches. Their tentacles can reach lengths of 30 meters and contain over 750,000 nematocysts on each tentacle (up to 40 tentacles).
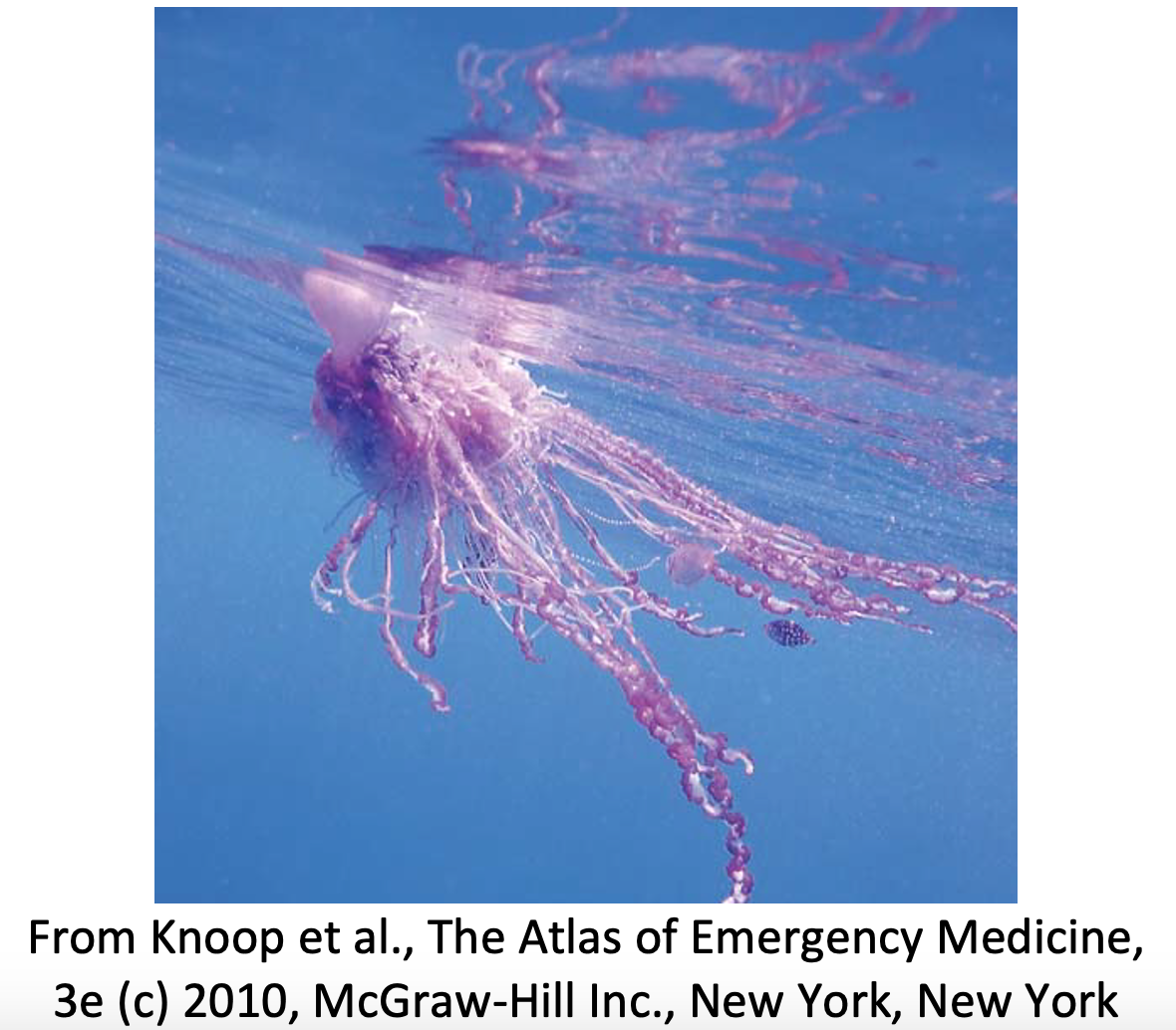
- Physalia utriculus is known as the blue bottle and are found in Indo-Pacific waters. They contain only one tentacle that can reach 15 meters in length.
- The most common reactions from these toxins include intense pain with burning and redness at the site. There have been reports of wounds severe enough requiring skin grafts. Systemic signs include anaphylaxis, headache, vomiting, abdominal pain and diarrhea. Death is extremely rare.
- Scyphozoa are the class of true jellyfish. Jellyfish species are diverse in shape, color and size. Common jellyfish that are known to envenomate are the hair jelly, sea nettle and mauve stinger. The mauve stinger is well known as it is pink during the day and phosphorescent at night.
- Envenomation: Envenomation from Cnidaria occur from persons coming into contact with tentacles. The tentacles are lined with nematocysts (cnidae). Envenomation is typically inadvertent from swimmers coming into contact with them. Mechanical stimulation of the tentacles causes cnidae to discharge venom. The venom is consisted of various neurotoxins, myocardial toxins, vasodilatory toxins (histamine and serotonin), proteolytic and lipolytic enzymes and membranotoxic pore-forming complexes. It is estimated that less than 1% of cnidae discharge venom on initial contact. Subsequent discharge of cnidae is caused by pouring freshwater on or trying to take off the tentacles. Most of these injuries are non-life threatening. Stinging and burning occur immediately. Skin changes range from urticaria to bullae and skin necrosis. Whip-like lesions may not appear for several minutes to hours.
- Management:
- Address ABCs
- It is critical in reducing venom load and reducing venom exposure by removing tentacles
- It is important to know which species inhabit the region the victim is in. Box jellyfish only inhabit Australian waters so for an envenomation in the US, antivenom does not need to be considered. Stings regionally in the US are likely to be from less lethal species such as Portuguese man-of-war
- Antivenom for box jellyfish should be administered immediately if possible
- IV magnesium can be given if no response to antivenom
- Irukandji Syndrome can be fatal. Use benzodiazepines for hypertension, agitation and tachycardia. Consider nitroglycerine or phentolamine drips for refractory symptoms.
- 100% vinegar for 30 seconds should be applied first to irreversibly inhibit nematocyst discharge
- Tentacles should be picked off, not scraped. Scraping can lead to increased nematocyst discharge
- Methods that increase nematocyst discharge and should be avoided are rinsing with freshwater, urine, ethanol and ammonia
- Saltwater rinses are not recommended as it can discharge nematocysts by mechanical force
- Topical lidocaine is not recommended as it can increase nematocyst discharge
- Hot water has been shown to significantly reduce pain
- Disposition:
- If systemic or severe symptoms, patient will need admission
- Discharge if no systemic symptoms
- Fire Coral
- The fire coral (Millepora alcicornis) is different than other members of the Cnidaria class as it is sessile and exists as a fixed colony of hydroids. It appears like normal coral and has a white to yellow or green exoskeleton. Small tentacles (dactylozooids) protrude through small gastropores in the exoskeleton. The venom contains in the nematocysts have hemolytic, dermonecrotic and cytotoxic toxins. Fire corals are widespread and exist in throughout the world with most victims being snorkelers and scuba divers.

-
- Lacerations are associated with fire coral injuries due to their rigid structure. Envenomation occurs immediately and results in intense pain, pruritis and urticaria. Blistering occurs up to 6 hours after exposure. Pain and sensitivity can last for months after exposure. Systemic symptoms are extremely rare.
- Management:
- Fire coral are found throughout the world. Consider these injuries in swimmers and divers.
- Oral analgesics, topical lidocaine and steroids may help symptoms
- Hot and cold water equally efficacious for pain with irrigation
- Lacerations should be copiously irrigated and loose closure
- Antibiotics covering skin and aquatic flora
- Tetanus prophylaxis
- Disposition:
- Symptoms are usually localized to the skin. Patient can be discharged if no systemic symptoms.
- Sea anemones
- Sea anemones are in the class Anthozoa and are considered venomous carnivores. Anemones have tentacles that are coated in toxins that inactive voltage gated sodium channels causing paralysis to victims. Anemones have modified nematocysts called sporocysts. These envenomations are typical in persons swimming around coral reef without protective suits.
- Management:
- Due to the neurotoxic nature of the venom, manage ABCs extremely closely
- Deactivate sporocysts with vinegar
- Hot water immersion of injured extremity for up to 90 minutes
- Oral or IV analgesia
- General wound care and consider antibiotics that cover aquatic species and skin flora if wound appears infected
- There is no antivenom available
- Disposition:
- Symptoms are usually mild and localized to skin lesions. Patient can be discharged if no systemic symptoms.
Bites
Octopus
- Background: Octopuses are of the phylum Mollusca and the Cephalopoda class. The cephalopod of greatest toxicologic concern is the blue-ringed octopus. Blue-ringed octopuses are typically found in Australia. Most bites from these animals come from being handled out of water. When agitated, their bodies darken, and their blue circles become iridescent blue.
- Envenomation: The beak of the octopus creates small puncture wounds in which the venom is introduced. Bites may be painless and symptom onset is within 10 minutes. One of the toxins found in blue-ringed octopus’ venom is identical to tetrodotoxin. Tetrodotoxin blocks fast sodium channel conduction ranging from a tingling sensation around the mouth to flaccid muscle paralysis. Death results from respiratory failure and hypotension. Patients may need ventilatory support from 6 hours to several days.

- Management:
- Fatal octopus bites are only found in Australia
- ABCs; intubate if respiratory failure
- No antivenom available
- Consider pressure bandage immobilization
- Wound care, tetanus prophylaxis
- Disposition:
- ICU care for ventilatory support
- Prognosis is good even with artificial respiratory support
- If no paralysis, patient can be discharge after an observation period of 4-6 hours
- Delayed hypersensitivity can occur
- Joint pain can persist for weeks
Sea snakes
- Background: Sea snakes are front fanged venomous reptiles that are closely related to the cobra and krait. Their bodies are flattened and brightly colored. They are distinguished from eels by the presence of scales and the lack of gills and fins. All 52 species of sea snakes are venomous with the most common being the baked sea snake and the yellow-bellied sea snake. Sea snakes are common in Australia, Pacific Ocean, Indian Ocean and the Persian Gulf. Hawaii is the only US state where sea snakes inhabit. They are usually docile except when threatened or during mating season. Fishermen and waders are people at most risk.
- Envenomation: Bites range from painless to mild discomfort. 1-4 fang marks are common but over 20 can be found with multiple bites. Sea snake venom contains neurotoxic and myotoxic proteins. Some venoms contain nephrotoxins associated with acute renal tubular degeneration, proliferative glomerulonephritis and liver failure. Venom from sea snakes is generally more lethally potent than terrestrial snakes. Myotoxic venom results in rhabdomyolysis, painful muscular rigidity, myoglobinuria and skeletal muscle paralysis. These are hallmarks of sea snake envenomations. The neurotoxic component results in an ascending muscle paralysis, dysarthria, dysphagia, ptosis and airway compromise.
- Management:
- Bite marks may not be apparent. History and presenting symptoms are vital
- Symptom onset is within 4 hours
- ABCs
- If respiratory failure and/or rhabdomyolysis, give antivenom
- CSL sea snake antivenom is first line starting with 1-3 vials, max 10, if severe symptoms
- CSL tiger snake antivenom can be used if sea snake antivenom unavailable
- 1 vial sea snake antivenom=2-4 vials of tiger snake antivenom
- Neostigmine and atropine can be considered if no antivenom available although there is no evidence to evaluate efficacy
- Electrolytes, creatinine, CK, urinalysis to assess for the presence of renal failure, rhabdomyolysis, myoglobinuria and hyperkalemia
- EKG
- Do not wash wound
- Apply PBI if no antivenom available
- IV fluids for rhabdomyolysis
- Disposition
- Patient can be discharged if no symptoms within 2-4 hours (“dry bite”)
- Consider ICU level care for symptomatic patients
- If given antivenom, education on serum sickness 4-14 days after therapy needs to be given

A 26-year-old man presents to the emergency department with severe finger pain after accidentally touching a lionfish in his saltwater tank while cleaning the glass. He is afebrile, and the remainder of his vital signs include a heart rate of 101 beats per minute, blood pressure of 128/91 mm Hg, respiratory rate of 19 per minute, and a room air pulse oximetry reading of 100%. Examination is remarkable only for mild erythroderma at the site of his pain, where he reports touching the fish. Which of the following therapies is most appropriate?
A) Acetic acid application
B) Cold-water immersion
C) Hot-water immersion
D) Salt water immersion
E) Topical calcium gluconate
Answer: C
Human contact with venomous marine creatures, both in nature and captivity, is common. Serious harm can result from biologic toxins or mechanical trauma inflicted by the stinging apparatus. Common venomous aquatic organisms include the phylum Cnidaria (anemones and jellyfish), Mollusca (octopods and snails), Echinodermata (sea urchins and sea stars), Hydrophiidae (sea snakes), and various spined fish. The lionfish (Pterois spp) is a spiny fish of the family Scorpaenidae and is often kept in home saltwater tanks. Lionfish possess dorsal, anal, and pelvic spines that are linked to venom glands, so the pressure applied topically to the spine is proportional to the amount of venom released. The venom contains a variety of compounds that cause immediate–onset pain, erythroderma, and swelling. Local symptoms are effectively treated with hot-water immersion. This is performed by immersing the envenomated site at 45°C for 20 minutes. Additional cycles of hot-water immersion can be performed if necessary secondary to persistent discomfort. Patients occasionally require a single dose of oral or parenteral analgesia, however, these are infrequently required upon discharge. The organism’s spine often breaks off in the wound, therefore, radiography and ultrasound should be performed to investigate the possibility of retained foreign bodies. Tetanus immune status should be addressed, and prophylactic antibiotics (including cefazolin and a quinolone) have been shown to decrease the rate of wound infection.

Topical acetic acid application (A) is a common first-line treatment for jellyfish stings. Jellyfish possess microscopic cnidae (“nettles”), which are specialized organelles consisting of a barbed thread bathed in venom. Release of this whiplike structure is controlled by a cnidocil. Cnidae are organized into nematocysts and distributed along the jellyfish’s tentacles. These discharge and release venom in response to changes in physical pressure (from contact with a victim’s skin) or osmolarity. The osmolarity of acetic acid, particularly in vinegar, is similar to that of seawater and, therefore, causes a decrease in venom release. Cold-water immersion (B) is not nearly as effective as hot-water immersion in treating lionfish envenomation. Many marine venoms are heat labile and denature or otherwise neutralize at supraphysiologic temperatures. Saltwater immersion (D) of the affected digit would be useful in jellyfish envenomation for the same reasons as acetic acid. Topical calcium gluconate (E) has been reported to be effective in treating dermal hydrofluoric acid exposures, but it plays no role in the management of marine envenomations.
Further Reading:
FOAMed
References:
Nelson, L., & Goldfrank, L. R. (2019). Marine Envenomations. In Goldfrank’s toxicologic emergencies / Lewis R. Goldfrank, Lewis S. Nelson. New York: McGraw-Hill Education.
RAP CorePendium. (n.d.). Retrieved July 24, 2020, from https://www.emrap.org/corependium/chapter/recVD0p2YSerBeICI/Marine-Envenomations?MainSearch=%22Marine+Envenomations%22





