EM@3AM: Purpura
- Mar 27th, 2021
- Katherine M. Buckley
- categories:
Author: Katherine M. Buckley, MD (EM Resident Physician, UT Southwestern, Dallas, TX) // Reviewed by: Alex Koyfman, MD (@EMHighAK) and Brit Long, MD (@long_brit)
Welcome to EM@3AM, an emDOCs series designed to foster your working knowledge by providing an expedited review of clinical basics. We’ll keep it short, while you keep that EM brain sharp.
A 4-year-old vaccinated male is brought to the ED by his parents for 3 days of hematuria and abdominal pain. They present now because he refuses to ambulate. He has a rash on his legs that family attributes to playing outside in the grass. His vital signs include HR 135, RR 20, and temperature of 37.9 C. His abdomen is diffusely tender, and he has red, raised papules on the buttocks and lower legs.
What is the diagnosis, and what is the most common gastrointestinal complication?
Answer: Henoch-Schonlein purpura; intussusception
Background:
- Purpura is a non-blanching rash caused by extravasation of blood into the dermis from the capillaries
- Color ranges from bright to deep red and changes to purple, green, and yellow as heme pigments are broken down over time1
- Definition varies by size:1
- Petechiae: < 4 mm
- Purpura: 4-9 mm
- Ecchymosis: ³ 1 cm

Evaluation:
- History is important: ask about foreign travel, new medications, sexual history, vaccination status, sick contacts, family history of bleeding or thrombotic disorders, and recent illness
- Assess overall appearance and vital signs: fever, hypotension, and toxic appearance are red flags for a life-threatening illness such as meningitis, TTP, or DIC
- Fully undress the patient to examine the entire body, including the palms and soles, as well as mucosal membranes
- Determine if lesions are raised (palpable) versus flat or blanching versus non-blanching by touching the rash with a gloved hand
- Palpable petechiae/purpura: meningitis, HSP, endocarditis
- Non-palpable petechiae/purpura: ITP, TTP, HUS
- Blanching: scalded skin syndrome, scarlet fever, measles, anaphylaxis
- Non-blanching: petechiae, purpura
- If the skin sloughs with gentle pressure, this is Nikolsky’s sign, suggestive of pemphigus vulgaris, TEN, or SJS
Categorized by cause:
- Intravascular (platelet changes/coagulopathy)
- Idiopathic thrombocytopenic purpura (ITP): anti-body mediated destruction of the platelets leading to isolated thrombocytopenia
- Primary ITP if no inciting event
- Secondary ITP is due to preceding viral syndrome or in the setting of known autoimmune disorder
- Risk of ICH is low, about 1%, and risk of severe non-ICH bleeding is over 9%2
- Clinical presentation: non-palpable petechiae/purpura in the dependent areas of the body and oral mucosal bleeding
- Labs: normal LDH, haptoglobin, PT, PTT, fibrinogen
- Treatment: steroids (methylprednisolone 1g IV daily for 3 days or dexamethasone 40mg PO/IV daily for 4 days), platelet transfusions and IVIG if significant bleeding or platelet count < 30,0003
- Idiopathic thrombocytopenic purpura (ITP): anti-body mediated destruction of the platelets leading to isolated thrombocytopenia

-
- Thrombotic Thrombocytopenic Purpura (TTP):
- Congenital deficiency of von Willebrand factor cleaving protease that results in abnormal platelet aggregation and micro thrombi
- Clinical presentation: non-palpable purpura, pentad of fever, microangiopathic hemolytic anemia, renal failure, thrombocytopenia, and neurologic abnormalities4
- Pentad is rare (only < 5%) so microangiopathic hemolytic anemia and thrombocytopenia is enough to suspect TTP and start treatment5
- Labs: elevated LDH, decreased haptoglobin, normal PT/PTT/fibrinogen
- Treatment: plasma exchange/steroids, +/- FFP- do not delay as mortality is up to 90%4
- Hemolytic uremic syndrome (HUS):
- Typically occurs in children and 90% of cases are due to Shiga toxin-producing E. coli w/ prodrome of abdominal pain, vomiting, and bloody diarrhea6
- Atypical causes include Streptococcus pneumoniae, immunosuppression, and complement mutations
- Clinical presentation: non-palpable purpura, microangiopathic hemolytic anemia, thrombocytopenia, renal injury
- Labs: elevated LDH, decreased haptoglobin, normal PT/PTT/fibrinogen
- Treatment: supportive (platelet transfusion only if life-threatening bleeding)
- Disseminated intravascular coagulation (DIC):
- Activation of both the coagulation and fibrinolysis cascades leading to the production of thrombi and the consumption of coagulation factors, causing bleeding, end-organ damage, and clot formation
- Occurs in the setting of underlying processes, including sepsis, trauma, malignancy, and obstetric complications7
- Clinical presentation: toxic-appearing, non-palpable purpura, renal failure, ARDS, AMS, bleeding from IV sites or mucus membranes
- Labs: elevated d-dimer, thrombocytopenia, elevated PT/PTT, decreased fibrinogen
- Treatment: treat the underlying cause and replacement therapy with pRBCs, platelets, FFP, and cryoprecipitate
- Mortality ranges from 40-80% and risk of death increases with age and severity of organ dysfunction8
- Thrombotic Thrombocytopenic Purpura (TTP):

-
- Purpura Fulminans:
- Rare syndrome of rapidly evolving extensive microvascular thrombosis and hemorrhagic skin necrosis9
- Three types:1
- Neonatal: hereditary deficiency of protein C, protein S, or antithrombin III
- Idiopathic: autoantibodies deplete protein S after an infection
- Acute infectious: commonly a complication of DIC
- Clinical presentation: initially lesions with thin, irregular borders on the extremities that extend proximally to form necrotic lesions and hemorrhagic bullae
- Treatment: often requires surgical decompression as compartment syndrome develops
- Purpura Fulminans:

- Vasculitis
- Henoch-Schonlein purpura (IgA vasculitis):
- The most common vasculitis in pediatrics caused by deposition of IgA immune complexes in the walls of small vessels typically after preceding URI
- Classic tetrad of palpable purpura (predominantly on buttocks and lower limbs), arthritis/arthralgias, abdominal pain, and renal disease (most commonly isolated hematuria)
- Most common GI complication is intussusception, occurring in 3-4% of patients
- Scrotal pain and swelling most common GU symptoms, occurring in about 13% of boys, although testicular torsion is rare11
- Treatment: supportive care by maintaining adequate hydration and analgesia with NSAIDs
- Disposition: home with supportive care or admit for renal failure, GI complications, bleeding, or intussusception
- Henoch-Schonlein purpura (IgA vasculitis):

- Infectious
- Sepsis
- Meningococcal meningitis:
- Neisseria meningitidis, an encapsulated gram-negative diplococcus, is the leading cause of bacterial meningitis in children and young adults with a mortality rate of up to 13%12
- Clinical presentation: palpable purpura, fever, AMS, neck stiffness, photophobia, headache, myalgias, N/V
- Rash can be present in up to 64% of patients and in one study up to 91% had petechiae13
- Erythematous, macular and petechial rash starts on the extremities and extends proximally (similar to Rocky Mountain spotted fever), becoming purpuric and leading to purpura fulminans14
- Treatment: do not delay if suspect à ceftriaxone/cefotaxime 2g IV (if PCN allergy, meropenem 2g IV) plus vancomycin 30mg/kg IV
- Consider HSV coverage with acyclovir 10mg/kg IV
- Ampicillin for Listeria coverage if > 50 yo (2g IV) or neonate to 1 month (50 mg/kg IV)
- Infective endocarditis:
- Risk factors include rheumatic heart disease, degenerative valve disease, IVDU, and diabetes
- 80-90% of cases due to gram-positive cocci (staph, strep, and enterococcus), with aureus the cause of up to 30% of cases15
- Clinical presentation: fever, new cardiac murmur, petechiae, splinter hemorrhages
- Osler nodes (painful nodes on fingers/toes), Janeway lesions (painless macules), and Roth spots (retinal hemorrhages) are rare15
- Consider with sepsis of unknown origin or unexplained bacteremia

-
- Rocky Mountain spotted fever:
- Tick-borne disease caused by Rickettsia rickettsia that is most in the southeastern and south-central states during the spring and summer months
- Clinical presentation: non-specific symptoms (fever, headache, myalgias) and hallmark rash that occurs in 88-90% of patients16
- Rash starts on the hands and feet as blanching erythematous macules that progress to petechiae and extends spreads proximally to the trunk
- Mortality can range from 20-30% without antibiotic treatment, so have a high suspicion given season and geographic location16
- Treatment: doxycycline 100mg PO/IV BID
- Rocky Mountain spotted fever:
Pearls:
- A thorough history is important. Ask about travel, recent illness, new medications, family history of bleeding/clotting disorders, immunosuppression, and fevers.
- Evaluate vital signs, mucosal regions, and fully undress the patient to examine the distribution and characteristics of the rash.
- In patients with fever and palpable petechial rash, think meningitis until proven otherwise.
- Thrombocytopenia + hemolytic anemia = TTP
- Isolated thrombocytopenia + petechiae = ITP
- If suspect TTP, meningitis, or RMSF, do not delay treatment given high mortality.

A 45-year-old woman presents with fatigue and shortness of breath for the past three days. Physical exam reveals pale conjunctiva, scleral icterus and scattered purpura on her legs. Laboratory evaluation shows WBC 6,000/mcL, hemoglobin 9 g/dL, and platelets 15,000/mcL. Peripheral blood smear reveals schistocytes. On further questioning, she notes a couple recent episodes of headache with transient blurry vision. Which of the following is the most effective treatment for this condition?
A) Corticosteroids
B) Plasmapheresis
C) Transfusion of packed red blood cells
D) Transfusion of platelets
Answer: B
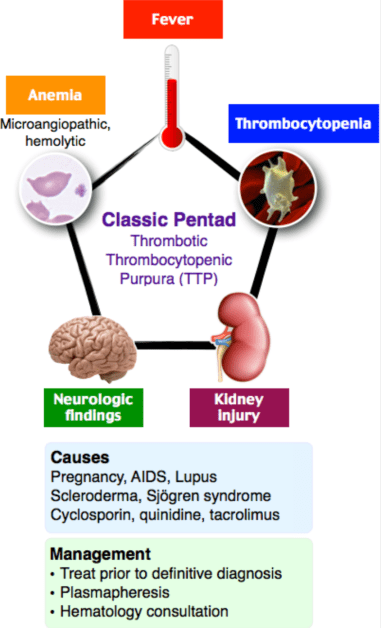
This patient has thrombotic thrombocytopenic purpura (TTP), a rare but deadly disease with an untreated mortality approaching 100%. TTP involves microangiopathic hemolytic anemia and thrombocytopenia via platelet aggregation in the microvascular circulation. A congenital or acquired deficiency of the ADAMTS13 protein prevents the normal cleavage of von Willebrand factor, leading to intravascular microthrombi. Red blood cells are fragmented as they travel through these partially occluded arterioles and capillaries. Microangiopathic hemolytic anemia can be identified by the findings of schistocytes on peripheral blood smear, as well as anemia with decreased haptoglobin, and elevated LDH and unconjugated bilirubin. Microthrombi in TTP can cause local tissue necrosis leading to transient neurologic deficits and, less commonly, fever and renal failure. The classic pentad of TTP (low-grade fever, anemia, thrombocytopenia, renal failure, and neurologic problems) is rarely seen except in late presentations. The diagnosis of TTP should be considered in any patient with hemolytic anemia and thrombocytopenia. The treatment of TTP involves immediate hematology consult to arrange for plasmapheresis, which can lower mortality by greater than 80%. Steroids may play a role in treatment and are often given along with plasmapheresis, but their treatment efficacy is not as clear. Fresh frozen plasma can be given if there will be a delay in starting plasmapheresis.
Corticosteroids (A) are often given as part of the treatment for TTP. However, the primary treatment proven to be effective in TTP is plasmapheresis. Corticosteroids are the mainstay of treatment for primary immune thrombocytopenia. Immune thrombocytopenia does not cause hemolytic anemia or neurologic symptoms. Platelet transfusion (C) should be avoided in TTP unless there is life-threatening bleeding or intracranial hemorrhage. There is limited data to suggest increased risk of thrombosis from platelet transfusion during TTP and it does not have the same proven benefit as plasmapheresis. Red blood cell transfusion (D) is not necessary in this patient, but it should be considered if there is life-threatening bleeding, active coronary ischemia, or severe anemia with hemoglobin less than 7 g/dL.
Further Reading:
#FOAMed
emDOCs – Approach to Rash
emDOCs – Pediatric Rash
SAEM – Pediatric Derm Approach
References:
- Reyes MA, Eichenfield LF. Purpura. Principles and Practice of Pediatric Infectious Diseases (Fifth Edition). https://www.sciencedirect.com/science/article/pii/B9780323401814000712. Published July 18, 2017.
- Neunert C, Noroozi N, Norman G, et al. Severe bleeding events in adults and children with primary immune thrombocytopenia: a systematic review. Journal of Thrombosis and Haemostasis. 2015;13(3):457-464. doi:10.1111/jth.12813.
- Arnold DM. Immune thrombocytopenia (ITP) in adults: Initial treatment and prognosis. UpToDate.com.
- James WD, Berger TG, Elston DM. Cutaneous Vascular Diseases. In: Andrews’ Diseases of the Skin: Clinical Dermatology. Philadelphia, PA: Elsevier; 2016:813-861.
- George JN, Cuker A. Acquired TTP: Clinical Manifestations and Diagnosis. UpToDate.com. Published December 4, 2020.
- Ardissino G. Epidemiology of haemolytic uremic syndrome in children. Data from the North Italian HUS network. European Journal of Pediatrics. 2015;175(4):465-473. doi:10.1007/s00431-015-2642-1.
- Farkas J. Acute Disseminated Intravascular Coagulation (DIC). EMCrit Project. https://emcrit.org/ibcc/dic/. Published January 19, 2021. Accessed March 13, 2021.
- Leung L. Disseminated Intravascular Coagulopathy (DIC) in Adults: Evaluation and Management. UpToDate. Published January 4, 2021.
- Perera TB. Purpura Fulminans. StatPearls. https://www.ncbi.nlm.nih.gov/books/NBK532865/. Published January 11, 2021.
- Farkas J. Purpura Fulminans. EMCrit Project. https://emcrit.org/ibcc/pf/. Published February 19, 2021.
- Søreide K. Surgical management of nonrenal genitourinary manifestations in children with Henoch-Schönlein purpura. Journal of Pediatric Surgery. 2005;40(8):1243-1247. doi:10.1016/j.jpedsurg.2005.05.005.
- Apicella M. Clinical Manifestations of Meningococcal Infection. UpToDate. Published November 21, 2019.
- Heckenberg SG, de Gans J, Brouwer MC, et al. Clinical Features, Outcome, and Meningococcal Genotype in 258 Adults with Meningococcal Meningitis. Medicine. 2008;87(4):185-192. doi:10.1097/md.0b013e318180a6b4.
- Santistevan J. What’s that Rash? An approach to dangerous rashes based on morphology. emDOCs.net – Emergency Medicine Education. http://www.emdocs.net/9009-2/. Published May 5, 2017.
- Cahill TJ. Infective endocarditis. The Lancet. 2016;387(10021). doi:https://doi.org/10.1016/S0140-6736(15)00067-7.
- Sexton DJ, McClain MT. Clinical manifestations and diagnosis of Rocky Mountain spotted fever. UpToDate.com. Published June 24, 2020.
