Authors: Alena Hoover, MD (EM Resident Physician, ACMC/Oak Lawn, IL); Thaer Ahmad, MD (EM Attending Physician, Oak Lawn, IL) // Reviewed by: Sophia Görgens, MD (EM Physician, Northwell, NY); Cassandra Mackey, MD (Assistant Professor of Emergency Medicine, UMass Chan Medical School); Brit Long, MD (@long_brit)
Welcome to EM@3AM, an emDOCs series designed to foster your working knowledge by providing an expedited review of clinical basics. We’ll keep it short, while you keep that EM brain sharp.
A 70-year-old female with past medical history diabetes mellitus, hypertension, hyperlipidemia, dementia presents from nursing home with acute unilateral swelling along the left side of her face. She is breathing comfortably but seems to experience significant pain at the associated site of swelling. Vitals include T38.5, HR 102, BP 150/90, SpO2 98% on room air. On examination, she has erythema and tenderness overlying her left parotid gland. Massaging the gland causes expression of purulent material.
What is the diagnosis?
Answer: Sialadenitis
Definitions:
- Sialadenitis refers to inflammation of salivary glands1
- Sialolithiasis refers to obstruction of salivary glands via calculi1
- Sialadenosis refers to painless swelling of salivary glands (usually this process is bilateral and symmetric)1,2
- Associated with chronic diseases such as alcohol use disorder, diabetes mellitus, bulimia2
Epidemiology:
- Sialolithiasis affects men more than women whereas sialadenitis affects men and women equally3,4
- Of the salivary glands, submandibular glands are most frequently affected by sialolithiasis1
- Parotid glands are most frequently affected by sialadenitis4,5
- Patients with sialadenitis are often in their sixth or seventh decade5
- Elderly individuals who are prone to experiencing dehydration, those who were recently hospitalized or those who recently underwent surgical operations5,6
- Only 0.001% to 0.002% of hospital admissions are due to sialadenitis5

Anatomy:
- Salivary glands consist of the paired major salivary glands as well as multiple minor salivary glands1
- Paired major salivary glands include the following: the parotid, submandibular, sublingual glands7
- Parotid glands are the largest of the salivary glands1
- Important structures within the parotid glands include the facial nerve, auriculotemporal branches of the mandibular division of trigeminal nerve CN V3, external carotid artery, retromandibular vein, intra-parotid lymph nodes1
- Parotid glands are drained via Stenson’s ducts which pierce through buccinator muscles opposite 2nd maxillary molars1
- Submandibular glands are drained via Wharton’s ducts which course up through sublingual space and ultimately drain along the side of the frenulum1
- The vertical course Wharton’s ducts must take to drain the glands may be why the submandibular glands are the most frequently implicated in sialolithiasis3
- Sublingual glands are the smallest of the major glands and are drained via Bartholin’s ducts which feed into Wharton’s ducts1
Etiology of Sialadenitis:
- Sialadenitis can be acute vs. chronic
- Various causes of sialadenitis1,6,8
- Suppurative (bacterial)
- Suppurative infection of the parotid gland is also known as suppurative parotitis
- Viral
- Autoimmune diseases
- Granulomatous diseases
- Obstructive
- Obstructive causes include sialolithiasis, which refers to obstruction of salivary gland duct drainage secondary to presence of stones
- Neoplasm
- Suppurative (bacterial)
Pathophysiology and Risk Factors for Sialadenitis:
- Pathophysiology depends on the cause of sialadenitis
- Stasis of salivary flow followed by retrograde migration of bacteria is thought to play a role in the development of acute suppurative sialadenitis6
- Major risk factors for acute suppurative sialadenitis include1
- Dehydration
- Medications
- Commonly implicated medications include anticholinergics, diuretics and more
- Anticholinergics, for example, reduce salivary flow which contributes to increased risk of calculus formation
- Elderly age
- Sialolithiasis (obstruction)
- Radiation history
- Smoking
- Trauma to the area
- Viral causes of sialadenitis include1,8
- Mumps (most common)
- Parainfluenza
- HIV
- EBV
- Autoimmune conditions commonly associated with sialadenitis include1
- Sjogren’s disease
- Sarcoidosis
Clinical Presentation and Diagnosis of Sialolithiasis and Sialadenitis:
- Sialolithiasis presents with recurring episodes of pain and swelling in a salivary gland precipitated by eating8
- Viral or bacterial sialadenitis will typically present with physical exam findings such as erythema of the salivary gland and associated tenderness8
- Majority of viral sialadenitis cases present as bilateral swelling9
- Viral sialadenitis is more common in children9
- Peak incidence of viral sialadenitis is 4-6 years old whereas elderly, debilitated patients are more at risk of developing acute suppurative sialadenitis8,9
- As always, ABC’s come first
- Pay particular attention to airway
- Consider other life-threatening head and neck emergencies
- Complications of suppurative sialadenitis include extension of the infection to deeper spaces such as Ludwig’s angina, abscess development and even a fistula formation between the salivary gland duct and the skin8
- Thorough head and neck examination should be performed to assess for possible complications of sialadenitis and determine if there is concern for extension of the infection to deeper spaces
- Diagnosis can be made via clinical examination alone
- Imaging options within the ED for diagnosis include radiograph, CT imaging and POCUS (operator dependent)
- Imaging is not always necessary
- Consider imaging in cases where there is uncertainty about extent of the infection and there is concern for complications, when diagnosis is unclear, or if the patient is not improving with typical treatment10
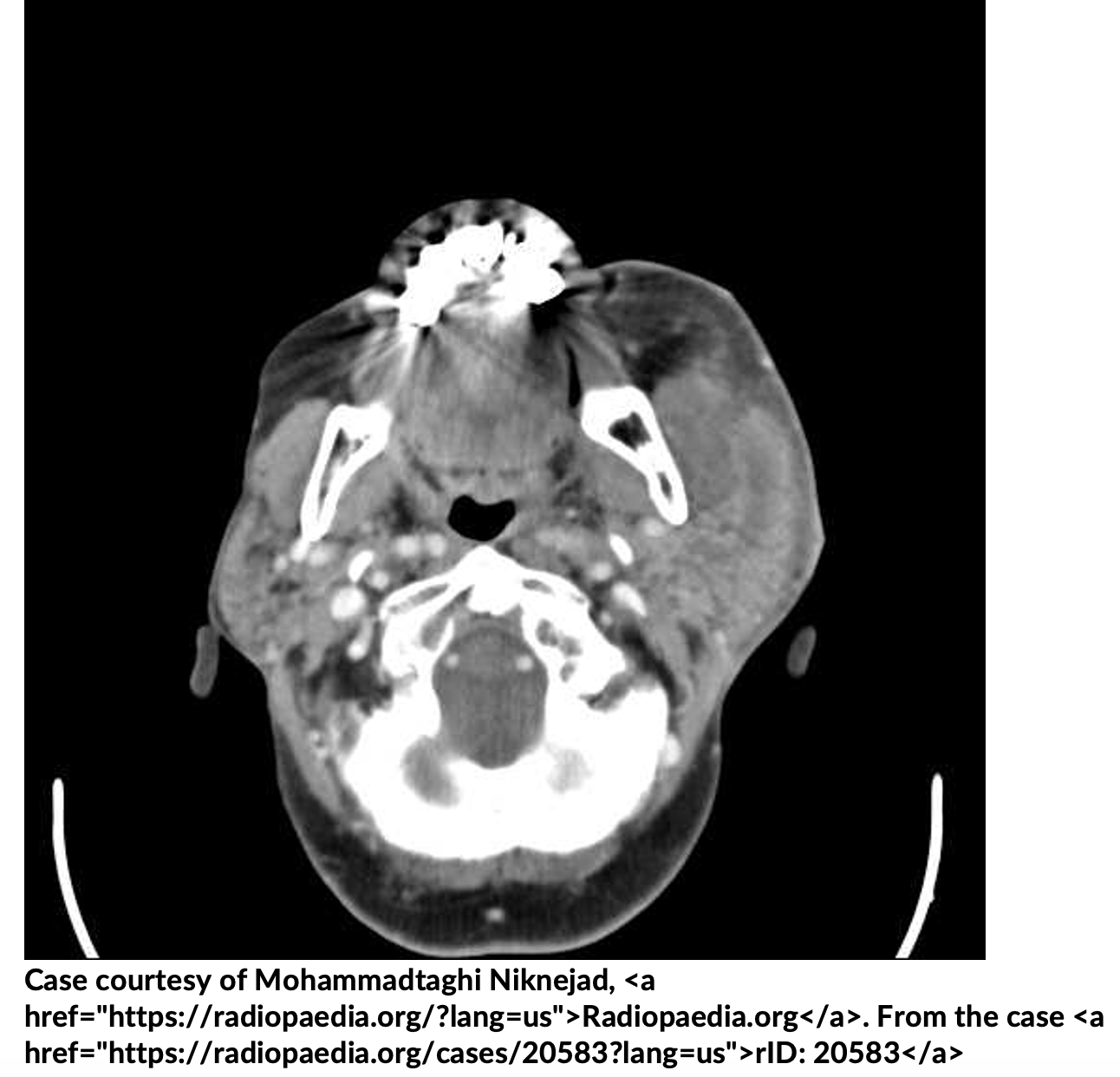
Treatment of sialadenitis:
- Depends on the etiology
- Suppurative sialadenitis
- Antibiotics should cover Staphylococcal aureus and other oral flora6
- PO antibiotics unless infection is severe4
- Augmentin 500-875 mg twice daily x 10 days, clindamycin, or cephalosporin + metronidazole3
- For severe infections or immunocompromised patients, use ampicillin-sulbactam, cephalosporin + metronidazole; add vancomycin for patients who are critically ill or have risk factors for MRSA
- Supportive treatment with sialogogues8
- Sour candy
- Encourage oral hygiene and rehydration
- Warm compresses8
- Antibiotics should cover Staphylococcal aureus and other oral flora6
- Viral sialadenitis
- Treatment is similar to suppurative with the exception of no antibiotic therapy8
- Referral to ENT should be considered in patients who are presenting with recurrent sialolithiasis or in patients who present with painless swelling of the glands and neoplasm is a concern
- Consider emergent consult ENT when there is concern about extension of infection into deeper spaces
Pearls:
- Patient populations most frequently affected by sialadenitis include elderly, recently hospitalized or post-operative patients
- Sialadenitis can be diagnosed clinically, but when unclear, imaging can be used
- Consider imaging patients in whom you are concerned about spread of infection or other infectious head and neck processes
- Suppurative sialadenitis should be treated with antibiotic therapy and supportive care

A 45-year-old man with a history of tobacco use, HIV infection, diabetes mellitus, and chronic kidney disease on intermittent hemodialysis presents to the ED with concerns for swelling and warmth just below the left ear. Vital signs include an HR of 90 bpm, a BP of 125/85 mm Hg, an SpO2 of 99% on room air, and a T of 38.4°C. Physical exam shows erythema, warmth, and tenderness to palpation of the left parotid gland. Visualization and palpation of the Stensen duct leads to the expression of purulent drainage. Moderate trismus limits the remainder of the exam. What is the most appropriate initial antimicrobial therapy for this patient?
A) Amoxicillin-clavulanate
B) Ampicillin-sulbactam
C) Ceftriaxone and metronidazole
D) Ceftriaxone, metronidazole, and vancomycin
Answer: D
Suppurative parotitis describes the acute bacterial infection of the parotid gland, often secondary to impairment of salivary flow and migration of oral bacterial flora into the salivary duct and glandular tissue. Most cases can be attributed to Staphylococcus aureus infection, though less frequent causes include Streptococcus pneumoniae, Streptococcus pyogenes, Haemophilus influenzae, and anaerobes (e.g., Bacteroides species, Peptostreptococcus species, and Fusobacterium species). Patients who are immunocompromised may experience infection related to gram-negative organisms (e.g., Pseudomonas aeruginosa, Escherichia coli). Risk factors include oral neoplasms, sialolithiasis, advanced age, dehydration, ductal foreign bodies, concomitant tracheostomy, and recent receipt of an anesthetic agent. Patients with a history of other comorbidities that predispose them to infection should also be considered high risk (i.e., those with HIV infection, diabetes mellitus, kidney failure, hepatic failure, malnutrition). Presenting features include erythema and tenderness of the skin overlying the parotid gland, tenderness of the gland itself, expression of purulent exudate from the Stensen duct, fever, and trismus.
The diagnosis is clinical, defined by purulent drainage from the Stensen duct. Imaging (e.g., ultrasonography or computed tomography with contrast) may aid in the diagnosis or evaluation for associated complications (e.g., abscess, osteomyelitis). Treatment focuses on appropriate antimicrobial therapy and promotion of salivary flow (e.g., lemon drops). Oral agents may be appropriate unless patients appear systemically ill, are immunocompromised, or cannot tolerate an oral regimen due to pain or trismus. Antimicrobial therapy should cover both Staphylococcus and Streptococcus species. Parenteral regimens in immunocompetent patients may include ampicillin-sulbactam, cefuroxime or ceftriaxone with metronidazole, or levofloxacin with metronidazole. If patients have risk factors for methicillin-resistant Staphylococcus aureus infection(e.g., recent hospitalization, residence in a long-term care facility, HIV infection, previous antibiotic use, hemodialysis), then vancomycin, linezolid,or daptomycin should be added. Broadening of antimicrobial therapy, imaging, and surgical drainage may be required if there is no improvement within 48 hours of antimicrobial and salivary-stimulating therapies.

Amoxicillin-clavulanate (A) is only available in an oral form and does not provide adequate breadth of coverage in a patient with several comorbidities for severe disease (e.g., HIV infection, chronic kidney disease, hemodialysis use, and diabetes mellitus).
Ampicillin-sulbactam (B) and ceftriaxone and metronidazole (C) are appropriate parenteral regimens for immunocompetent patients who otherwise lack risk factors for methicillin-resistant Staphylococcus aureus infection.
Further Reading:
Further #foamed:
References:
- Kessler AT, Bhatt AA. Review of the Major and Minor Salivary Glands, Part 1: Anatomy, Infectious, and Inflammatory Processes. J Clin Imaging Sci. 2018;8:47. Published 2018 Nov 15. doi:10.4103/jcis.JCIS_45_18.
- Ogle OE. Salivary Gland Diseases. The Dental clinics of North America. 2020;64:87-104.
- Hammett JT, Walker C. Sialolithiasis. In: StatPearls. Treasure Island (FL): StatPearls Publishing; September 26, 2022.
- Insalaco LF. Ferri’s clinical advisor 2023. Sialadenitis. 01/01/2023:1391-1392.e1. doi: 10.1016/B978-0-323-75573-3.00837-4.
- Adhikari R, Soni A. Submandibular Sialadenitis and Sialadenosis. [Updated 2022 Aug 8]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK562211/.
- Wilson KF, Meier JD, Ward PD. Salivary gland disorders. Am Fam Physician. 2014;89(11):882-888.
- Jauch EC, Hall G, Knoop KJ. Sialadenitis. In: Knoop KJ, Stack LB, Storrow AB, Thurman R. eds. The Atlas of Emergency Medicine, 5e. McGraw Hill; 2021. Accessed June 22, 2023. https://accessmedicine-mhmedical-com.aah.proxy.liblynxgateway.com/content.aspx?bookid=2969§ionid=250456248.
- Haidar H, Menon A, Al Duhirat E. Diseases of the salivary glands. In: Textbook of Clinical Otolaryngology. Cham: Springer International Publishing; 2020:387-395.
- Abdel Razek AAK, Mukherji S. Imaging of sialadenitis. Neuroradiol J. 2017;30(3):205-215. doi:10.1177/1971400916682752
- Medina J, MS III, Corey N, BS, Hahn B, MD. Acute Wharton’s Duct Sialadenitis and Submandibular Infection. The Journal of emergency medicine. 2013;44:e125-e127.






