Authors: Travis Mok, MD (@tkcm01 on Threads, Emergency Medicine Resident, Rutgers New Jersey Medical School); Cynthia Santos, MD (Emergency Medicine Attending, Medical Toxicologist, Rutgers New Jersey Medical School) // Reviewed by: Anthony Spadaro, MD (@TSpadaro91, Medical Toxicology Fellow, Rutgers New Jersey Medical School, Newark, NJ); James Dazhe Cao, MD (@JamesCaoMD, Associate Professor of EM, Medical Toxicology, UT Southwestern Medical Center, Dallas, TX); Alex Koyfman, MD (@EMHighAK); Brit Long, MD (@long_brit)

Case:
A resident sees a patient with a chief complaint of witnessed unknown ingestion. Bystanders state that this 60-year-old had been drinking at a bar when he supposedly started consuming an unknown amount of liquid from an unlabeled canister located in a nearby garage. On presentation, he is clinically intoxicated and is unable to provide additional history. Ethanol concentration is measured at 385 mg/dL. He calculates the patient’s osmol gap using their lab values for sodium, glucose, BUN, and the measured serum osmolality and gets a gap of 100.
Questions:
- What is the difference between osmolality and osmolarity?
- How do you calculate the osmol gap?
- What are common confounders that reduce the utility of calculating the osmol gap?
Discussion:
Osmolality and osmolarity are commonly incorrectly interchanged terms that both refer to the number of osmoles (number of moles of an osmotically active material, abbreviated osm) fully dissolved in a given amount of solvent within a solution. When used in the context of biology, the concentrations are usually so small that milliosms (mOsm) are often used. The difference lies in what unit the solvent is expressed in, either in kilograms or liters.
To put it more succinctly:1

Temperature-dependent: volume generally increases with temperature.
Used in calculations: laboratory measurement of ion concentration in serum is calculated as a function of mOsms per volume of solution (serum).
Technically bigger than osmolality: the volume of the solution includes the volume of the dissolved solute, however in a dilute solution the difference is insignificant.2

Temperature-independent: the mass of the solution is independent of its temperature.
More useful in biological contexts: its independence off the temperature of the solution allows it more generalizability in the context of human physiology.3
Measured in analytical testing: Laboratories measure plasma concentration using osmometers which measures values as a function of kilograms of solvent.1
Technically smaller than osmolarity: the mass of the solution does not include the mass of the dissolved solute.
What is the osmol gap equation, and what does it measure?
The osmol gap equation is as follows:3,4

Where: Measured serum osmolality is determined by laboratory osmometers, is the “true” osmolality of the patient’s serum.
Calculated serum osmolarity can be defined as follows:3,4

A normal osmol gap is <10 mOsm/kg. Normal values for the serum osmolality are 275 – 295 mOsm/kg.3,4
This mathematically calculates what the expected serum osmolality of the blood should be based off the values of sodium, glucose, and BUN. This is subtracted by the true serum osmolality. Any significant difference can be due to a variety of factors, most important of which are toxic alcohols3. This is discussed in further detail later.
The inclusion of sodium, glucose, and BUN in this calculation take in account that solutes are osmotically active and are the largest contributors of serum osmolarity (in addition to Cl– and HCO3–).5–7 As such, a relatively accurate approximation of the true serum osmolarity can be extrapolated from these values.
If these are the largest contributors to serum osmolarity, why are we performing additional calculations on each value? Let’s go through each one:
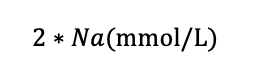
Sodium (Na+) is a major ionic osmotic solute in the serum along with Cl– and HCO3–. As part of homeostasis, it can be stated with relative accuracy that all sodium cations are counterbalanced by an anion. Thus, multiplying its osmolarity by 2 will account for its associated anions and gives a reasonable approximation of the total osmolarity of sodium, chloride, and bicarbonate.4,8
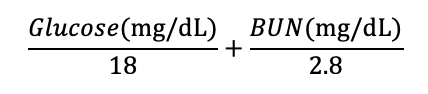
Glucose and BUN are analytically measured in mg/dL, which must be converted into a molar value. This can be accomplished by converting mg/dL into mmol/L, which involves dividing the mg/dL value by the 1/10th of the molecular weight of that substance.4,7 Both solutes are non-ionic and do not disassociate in solution.5
While there are a plentiful number of other osmotically active solutes present in serum, the additional of more and more solutes into the calculation can lead to further errors due to complex interactions in serum9.
Ethanol
Ethanol can be a major osmotically active solute in serum on par with sodium, BUN, and glucose.7,10 If ethanol is present in the patient’s serum but not accounted for in the calculated serum osmolarity, this can lead to an abnormally large osmol gap. Calculations exist for adding on ethanol into the calculated serum osmolarity equation (where 4.6 is the molecular weight of ethanol converted into milligrams and divided by 10):7,8

However, empiric observations have concluded that ethanol does not behave ideally when interacting with water in a solution. A more accurate calculation would involve adjustment of the denominator with increasing ethanol concentration, a complex calculation that will introduce errors.8
Case Follow-up:
Due to the large osmol gap and the concerning clinical history, the resident contacts Poison Control due to the unknown ingestion. When discussing the osmol gap, the resident realizes that they had forgotten to include the patient’s ethanol concentration as part of their calculations. When correcting for ethanol, the osmol gap is 16.
Clinical Pearls:
- An osmol gap appears when an osmotically active solute is abnormally present in the patient’s blood and large gaps (>50-70 mOsm/L) are indicative of a toxic alcohol ingestion.
- Serum ethanol must be accounted for when calculating serum osmolarity by adding (ethanol in mg/dL/4.6) to the calculated osmolarity.
- Be careful of your units! Glucose, BUN, and ethanol must be in mg/dL.
- To calculate an accurate osmol gap, the sodium, BUN, glucose, ethanol, and serum osmolality must be measured at the same time.
References:
- Erstad BL. Osmolality and Osmolarity: Narrowing the Terminology Gap. Pharmacotherapy. 2003;23(9):1085-1086. doi:10.1592/phco.23.10.1085.32751
- Koeppen BM, Stanton BA. Renal Physiology. 5th ed. Elsevier Mosby; 2013.
- Nelson LS, Goldfrank LR. Goldfrank’s Toxicologic Emergencies. New York Mcgraw-Hill Education; 2019.
- Rasouli M. Basic concepts and practical equations on osmolality: Biochemical approach. Clin Biochem. 2016;49(12):936-941. doi:10.1016/j.clinbiochem.2016.06.001
- Martín-Calderón JL, Bustos F, Tuesta-Reina LR, Varona JM, Caballero L, Solano F. Choice of the best equation for plasma osmolality calculation: Comparison of fourteen formulae. Clin Biochem. 2015;48(7-8):529-533. doi:10.1016/j.clinbiochem.2015.03.005
- Edelman IS, Leibman J, O’meara MP, Birkenfeld LW. Interrelations Between Serum Sodium Concentration, Serum Osmolarity and Total Exchangeable Sodium, Total Exchangeable Potassium and Total Body Water. J Clin Invest. 1958;37(9):1236-1256. doi:10.1172/jci103712
- Marts LT, Hsu DJ, Clardy PF. Mind the Gap. Ann Am Thorac Soc. 2014;11(4):671-674. doi:10.1513/annalsats.201401-033cc
- Hoffman RS, Smilkstein MJ, Rowland MA, Goldfrank LR. Osmol gaps revisited: Normal values and limitations. J Toxicol Clin Toxicol. 1993;31(1):81-93. doi:10.3109/15563659309000375
- Heavens KR, Kenefick RW, Caruso EM, Spitz MG, Cheuvront SN. Validation of equations used to predict plasma osmolality in a healthy adult cohort. Am J Clin Nutr. 2014;100(5):1252-1256. doi:10.3945/ajcn.114.091009
- Inaba H, Hirasawa H, Mizuguchi T. SERUM OSMOLALITY GAP IN POSTOPERATIVE PATIENTS IN INTENSIVE CARE. The Lancet. 1987;329(8546):1331-1335. doi:10.1016/s0140-6736(87)90646-5





