Today on the emDOCs cast with Brit Long, MD (@long_brit), we cover severe asthma and asthma mimics.
Severe Asthma and Asthma Mimics
Background
Asthma is common, affecting 1 in 11 children and 1 in 12 adults in the U.S. Asthma lacks a clear definition, despite it being a common disease. The Global Initiative for Asthma defines it as “a heterogeneous disease, usually characterized by chronic airway inflammation. It is defined by the history of respiratory symptoms such as wheeze, shortness of breath, chest tightness, and cough that vary over time and in intensity, together with variable expiratory airflow limitation.”
An asthma exacerbation often presents with wheezing and prolonged expiration. Patients with severe respiratory distress may present in a tripod position, leaning forward. The most dangerous lung sound is the absences of air movement, which is due to severe bronchoconstriction or patient exhaustion.
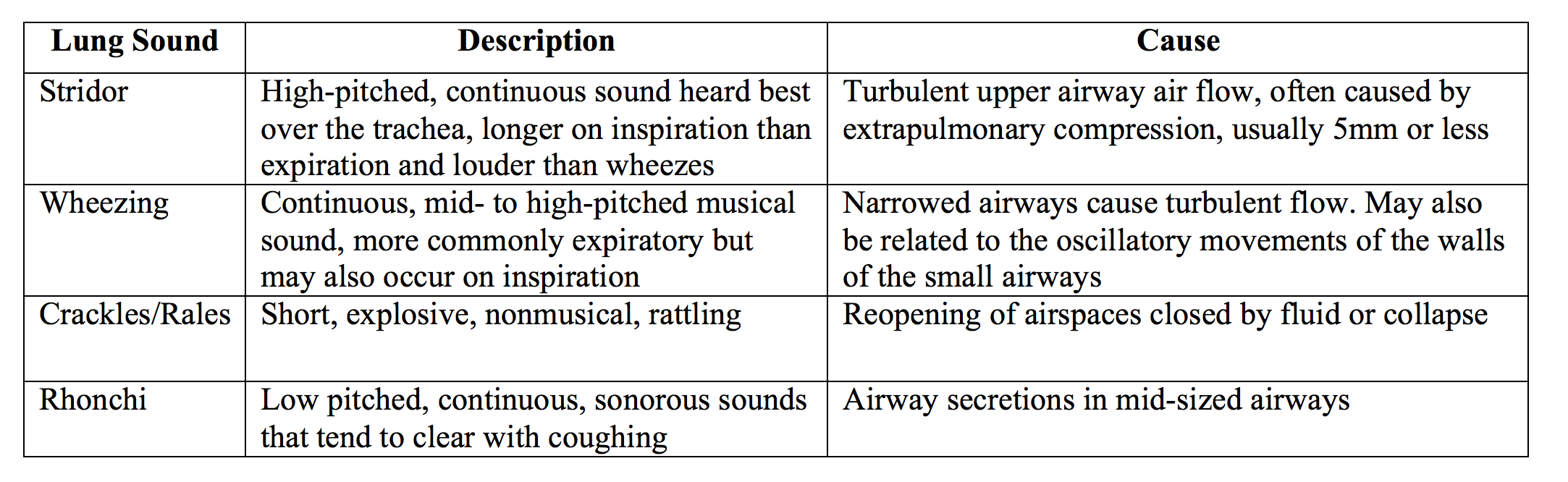
There are many mimics of asthma, especially conditions that present with wheezing. Some patients may present with no wheezing, but most report obstructive type symptoms. Over 75% of COPD patients and nearly 30% of patients with cardiac pathology experience similar symptoms. Airways narrow through swelling, compression, and intrinsic compression, and this narrowing with turbulent air flow can result in wheezing. Emergency physicians should be aware of conditions that can result in similar symptoms. Lung findings on exam are explained below.
Asthma Mimics
Anaphylaxis: Anaphylaxis involves two organ systems or a known allergic exposure with low blood pressure. Exam usually reveals urticaria (10-20% will not have rash), and nausea, vomiting, or diarrhea may also be observed. Treatment requires immediate resuscitation with epinephrine, steroids, intravenous (IV) fluids, and histamine antagonists. Any concern for anaphylaxis warrants intramuscular epinephrine.4
COPD: Like asthma, COPD is an obstructive airway disease. Patients may have asthma/COPD overlap. Official diagnosis is often completed by pulmonologist, though asthma is usually diagnosed in young adulthood and COPD usually after age 40 with history of bronchodilator responsiveness, Initial treatment of COPD is similar to asthma, though long term medication management differs (such as Long Acting Beta Agonists (LABA) in COPD improving mortality). In asthma, LABA use may increase mortality if used without inhaled steroids.
Heart Failure: Heart failure may result in wheezing with lung fluid accumulation. Some patients may not be diagnosed with heart failure upon initial presentation, and patients may present acutely with respiratory distress or with chronic worsening orthopnea and dyspnea (the most common presentation). Flash pulmonary edema (the acute version) can be due to ischemia, acute valvular pathology, cardiomyopathy, and other conditions. Exam may reveal rales, S3 heart sound, elevated JVP, and edema. Patients may have a history of dyspnea with exertion or with lying flat. Acute exacerbation with pulmonary edema requires venodilators and positive pressure ventilation (CPAP or BPAP). Diuretics can be used after venodilation.
PE: PE is not always an easy diagnosis, though emergency physicians evaluate patients with potential PE on a regular basis. Close to 1 in 10 patients with PE may have wheezing on exam.This may be due to vasoactive mediators released in response to the embolus.The key is to evaluate for PE risk factors in the history. If patients do not improve with standard asthma medications, PE should also be considered. Evaluation includes risk stratification such as Wells criteria, with D-dimer and CT pulmonary as needed. Significant PE requires anticoagulation.
Foreign body aspiration: A small object in the bronchioles from aspiration can result in focal lung finds, and worse, respiratory distress. Patients with greatest risk for this include children, older adults, and those mentally disabled. Patients may present with acute cough or wheezing. The classic history is lack of preceding upper respiratory symptoms or prior wheezing. Choking followed by cough is present in 75% of pediatric patients with foreign body aspiration. Chest x-ray can help, erect and lateral, which may show hyperinflation. Bronchoscopy is required if concern for aspiration, even with negative chest x-ray.
Angioedema: “Angioedema” refers to localized swelling in locations with loose connective tissue, including the face, oropharynx, bowel wall, extremities, and genitalia. There are many causes. Primary pathology includes mast cell-mediated and bradykinin-mediated. Mast-cell mediated angioedema can have other signs of allergic reaction such as urticaria. Bradykinin-induced angioedema is not associated with urticaria and pruritis, as it is not allergic. This form is the cause in ACE-inhibitor-induced angioedema and hereditary angioedema. Angioedema associated with systemic findings such as upper airway swelling, wheezing, abdominal pain, nausea, and vomiting should be managed as anaphylaxis until proven otherwise and treated with epinephrine, antihistamines, and corticosteroids. Rapid airway protection with intubation may be required, and a difficult airway should be assumed with adjuncts available.
Drug Related Wheezing: This is most commonly associated with aspirin. Aspirin Exacerbated Respiratory Disease, or Samter’s Triad, consists of asthma, nasal polyps, and sensitivity to aspirin or other NSAIDs. Non-selective beta-blockers can precipitate wheezing in patients with underlying disease (such as asthma). ACE-inhibitors, while commonly causing dry cough, may result in bronchospasm and wheezing. Many drugs can cause asthma symptoms, or worsen asthma in patients with known disease. The risks and benefits of continuing aspirin or an NSAID must be strongly considered, or an alternative can be used.
Central Airway Obstruction: Obstruction in the trachea and main stem bronchi include bronchogenic carcinomas, tracheal strictures, sarcoidosis, and goiter. Though these usually do not present acutely, patients may notice other symptoms including weight loss. If the obstruction is fixed, wheezing will likely be constant and fixed. Asthmatic wheezing usually occurs after exposure to allergen or upper respiratory infection. Wheezing due to fixed obstruction may be localized on exam. Further evaluation and testing relies on the history and exam. Risk factors for cancer, symptoms consistent with hyperthyroidism, or a history of intubation should be obtained. Chest CT will most likely identify the obstruction, though the patient must be able to lie supine. Further consultation is required if diagnosed, with bronchoscopy as well.
Vocal Cord Dysfunction: Paradoxical, involuntary closure of the vocal cords during inspiration, (or edema of the vocal cords) may result in wheezing and acute respiratory distress. Wheezing in this condition is usually inspiratory or inspiratory and expiratory (asthmatic wheezing is mostly expiratory). This is due to forced expiration stenting open the cords and decreasing the obstruction. Patients often present soon after exposure to a stressor, inhaled irritants, or exercise. Risk factors include prior intubation or neck surgery (leading to possible damage to the recurrent laryngeal nerve). Diagnosis is often confirmed through laryngoscopy. Treatment of vocal cord dysfunction includes several maneuvers. Panting, which can abduct the vocal cords through activation of the posterior cricoarytenoids, breathing through a straw, patient jaw thrust while breathing, nose to mouth breathing, administration of a helium-oxygen mixture such as heliox, or continuous positive airway pressure (CPAP) can be used. The condition is often self-limited and usually does not require other invasive interventions.
Approach
The approach for asthma and asthma mimics is to first assess for life threats, provide emergent interventions, and then obtain history and focused exam. Rapid treatment with bronchodilator and corticosteroids is required. Non-Invasive Positive Pressure Ventilation (NIPPV) should be considered.
Once treatment and initial stabilization have been completed, focused history and exam should be conducted to evaluate for mimics. As discussed, there are many causes of wheezing, and these conditions must be considered to prevent anchoring bias. Red flags for other conditions include absence of asthma history, prior history of mild asthma, or poor response to therapy.
Treatment:
– Assess the ABCs.
– Administer oxygen to relieve hypoxemia. If severe exacerbation present, provide IV fluids (address secondary losses).
-Deliver a short acting beta-agonist (SABA) with ipratropium (anticholinergic).
-Give systemic corticosteroids to decrease airway inflammation. Options include prednisone, methylprednisolone, and dexamethasone.
-If patients fail to respond to inhaled therapies and steroids, next steps include parenteral beta agonist, magnesium, heliox, ketamine, and/or NIPPV.
-Epinephrine is a non-selective beta agonist that causes bronchodilation, vasoconstriction, increased cardiac contractility and increased heart rate. Dose for IM is 300-500 mcg, while IV is recommended in hypotensive patients or those who fail to respond to IM dosing. Dose is 5mcg IV and titrate to effect.
-Magnesium is effective in those with severe exacerbation by relaxing bronchial smooth muscle. In adults, start with 2g, which can be repeated twice.
-Ketamine may have bronchodilator properties. It can also assist with delayed sequence intubation.
-Heliox is an option; it can improve laminar flow of inhaled has which may allow better airflow through the constricted airways; allows better gas exchange and transport of medications to flow down to distal airways and alveoli. Evidence suggests limited utility, and if hypoxic, an adequate amount of FiO2 may not be reached.
-Non-invasive positive pressure ventilation should be considered for all patients who display: moderate to severe dyspnea or respiratory distress, hypercapnic acidosis, a respiratory rate > 25/min, accessory muscle use, or paradoxical breathing. Bilevel settings are recommended to improve ventilation.
-Intubation is an inherently dangerous intervention in asthma because it does not fix the underlying problem (bronchoconstriction) and can cause dynamic hyperinflation, and rapid acidosis if respiration is not matched during RSI or post-intubation. The decision to intubate is based on a number of factors including the patients overall appearance, work of breathing, perceived ability to maintain their effort of breathing, mental status etc. Before intuition, preoxygenate and rehydrate with IV fluids. Ketamine 1-2 mg/kg IV can be used for induction. A paralytic such as rocuronium offers the advantage of longer paralysis which avoids vent asynchrony early in management.
-Mechanical ventilation: Must ensure that the patient has an adequate time to fully expire the delivered breath and avoid hyperinflation. Permissive hypercapnia involves decreasing the RR and allowing PaCO2 to rise to supranormal levels, which avoids breath stacking. Ensure post-intubation analgesia and sedation, which will assist with vent synchrony.
- Initial Ventilator Settings
- RR: 6-10 breaths/min
- VT: 6-8 ml/kg (ideal body weight
- PEEP: 0-5 cm H2O
- FiO2: Minimum necessary to maintain O2 sat > 93%
- Inspiratory Flow Rate: (suggest 100-120 L/min)
- Check Plateau Pressures and maintain at < 30 mm Hg
- Plateau pressure reflects the pressure experienced by alveoli
- Maintaining Pplat < 30 mm Hg helps to avoid alveolar damage
- If plateau pressure is > 30 mm Hg, consider lowering the RR and VT.
Mechanical ventilation does not fix the underlying bronchoconstriction. Be sure to continue maximal medical management.
Trouble Shooting the Ventilator:
- Hemodynamic instability and hypoxia after intubation/mechanical ventilation are common and life-threatening. Rapid recognition of the underlying problem and treatment are critical.
- DOPES Mnemonic
- Displacement of the endotracheal tube (ETT)
- Direct visualization with laryngoscope preferred (US confirmation another option)
- Obstruction of the endotracheal tube
- Pass ETT suction catheter
- Pneumothorax (tension)
- Lung POCUS for lung sliding
- Empiric needle decompression or finger thoracostomy
- Equipment failure
- Disconnect the vent and deliver manual BVM breaths
- Stacked Breaths
- Forcibly exhale patient (gently push down on anterior chest wall with two hands until no further exhalation detected.
- Displacement of the endotracheal tube (ETT)
-ECMO and anesthetic gases are final options for patients who continue to decline.






