Authors: Shannon M. Burke, MD (Education Scholarship Fellow, University of Wisconsin BerbeeWalsh Department of Emergency Medicine) and Benjamin H. Schnapp, MD, MEd (EM Associate Program Director, Associate Professor, University of Wisconsin BerbeeWalsh Department of Emergency Medicine) // Reviewed by: Michael J. Yoo, MD (EM Assistant Professor, San Antonio, TX), Alex Koyfman, MD (@EMHighAK), and Brit Long, MD (@long_brit)
Case:
A 55-year-old male with history of hypertension on hydrochlorothiazide presents to the emergency department (ED) with a chief complaint of a red, swollen, and painful left big toe. The patient states his toe felt uncomfortable when he went to bed last night, but he woke up this morning with severe pain, including when wearing his socks and shoes. He denies injury, fevers, chills, or recent infection. The patient does not smoke, but he consumes one or two glasses of wine with dinner each night. In the ED, his vital signs are: T 98.9°F, HR 88 BPM, BP 154/88, RR 16, and saturating 99% on room air. You suspect an acute gout flare. What are your next steps in confirming the diagnosis and treating the patient’s acute symptoms?
What are gout flares?
Gout is a common inflammatory arthritis that affects almost 4% of adults in the United States.1 Patients with or without an established history of gout arthritis typically present to the ED with an acute flare. Acute flares are caused by deposition of intra-articular monosodium urate (MSU) crystals that initiate an inflammatory response within the joint, leading to pain, erythema, and swelling.1 There are many risk factors for the development of gout, to include genetics and active medication profile (Table 1). These risk factors make patients susceptible to acute flares, which are often triggered by medical or surgical illness, dehydration, or dietary factors.1

How will patients present?
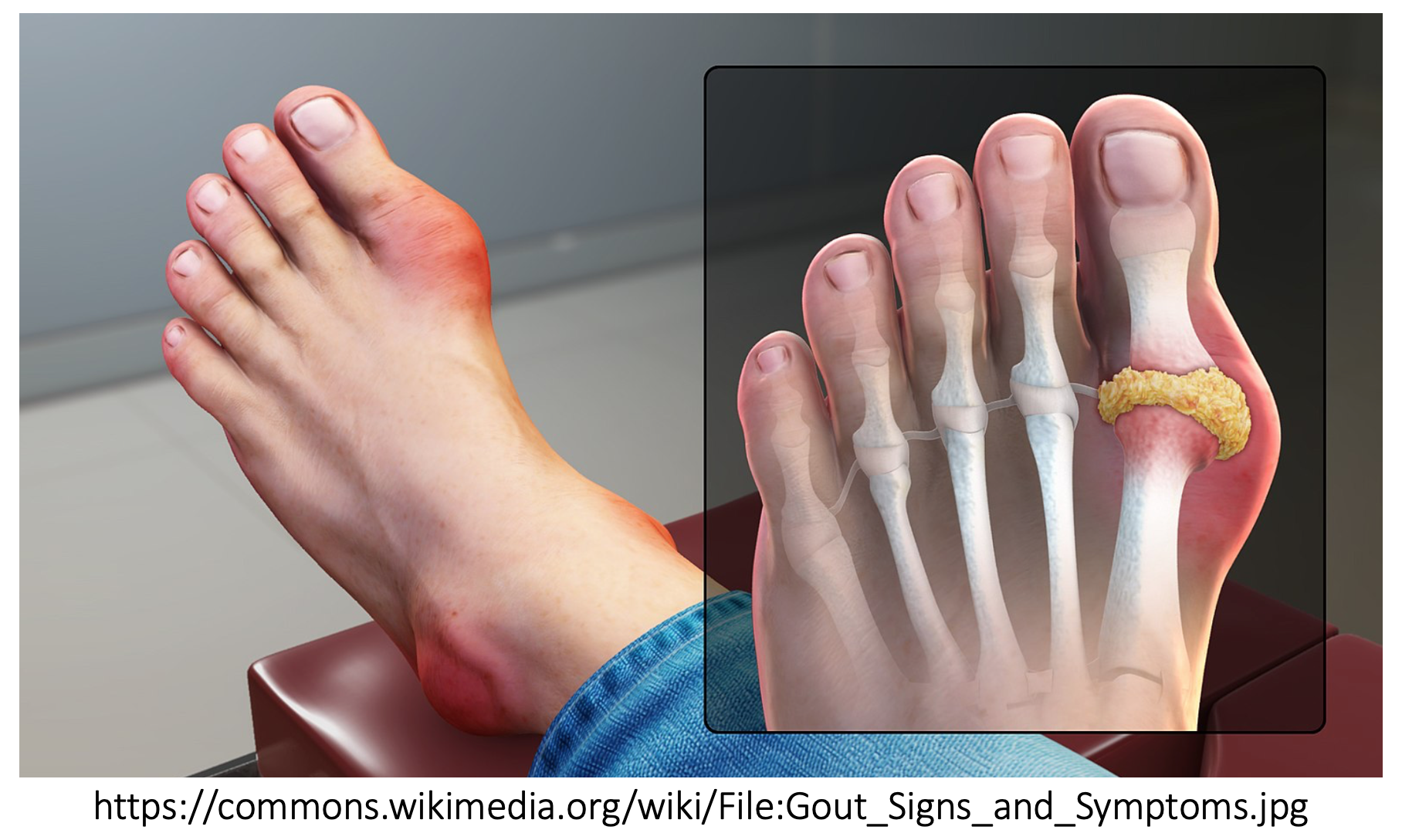
Many patients who present to the ED with an acute flare will have experienced a gout flare previously—ask your patients about their typical locations, quality of pain, etc. Inflammatory changes lead to pain, erythema, and swelling of the involved joint. Gout flares often start at night, start with mild joint discomfort, and usually peak within 24 hours of the onset of symptoms. The most commonly involved joint is the first metatarsophalangeal joint (MTP) followed by the lower extremity joints overall, such as the ankles and knees. Patients may also have tophi on exam, which are nodules that represent the chronic inflammatory granulomatous response to the monosodium urate crystals, often occurring over the first MTP, Achilles’ tendon, peroneal tendon, helix of the ear, olecranon bursa, and finger pads. Although rare, patients with polyarticular flares can also develop systemic symptoms such as fever.1
How do we diagnose gout?
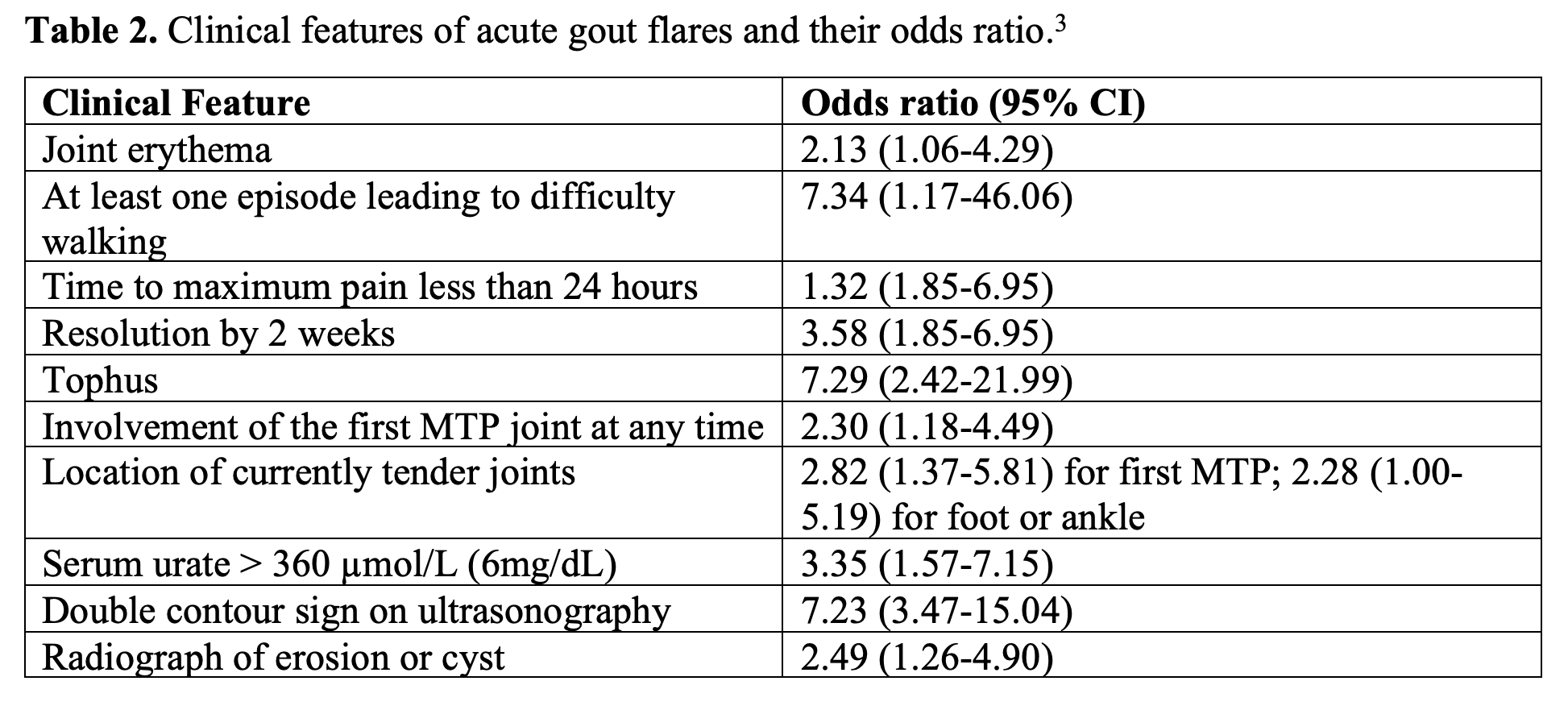
The gold standard in diagnosing gout is visual confirmation of negatively birefringent, needle shaped MSU crystals obtained from either synovial fluid or tophaceous material. In patients with an established history of gouty arthritis who present with typical gout flare symptoms, a diagnosis of an acute flare can be inferred by clinical symptoms.2 These features include: a sudden and exquisitely painful joint, especially the first MTP or lower extremity joints (ankles or knees), history of renal disease or medications that can cause hyperuricemia, and a favorable response to NSAIDs or topical ice.2 A rheumatologic study identified clinical features of gout and their respective odds ratios highlighted in Table 2. Of note, serum urate can be normal during an acute gout attack due to acute uricosuria, induced by IL-1 and IL-6 cytokine activation during the acute gout attack.2 It is also possible to have crystals present on a joint aspiration if patients have hyperuricemia without an acute gout flare, especially if they have previously had a gout flare in that joint.1
So, what should we do? Do we need to perform an arthrocentesis? Generally, an arthrocentesis should be performed whenever there is concern for a septic joint or if the clinical picture is not consistent with an acute gout flare (e.g., first flare, atypical features).2 Specifically, patients with systemic symptoms, vital sign abnormalities, and risk factors for either direct or hematogenous seeding of a joint should undergo joint aspiration with subsequent synovial fluid analysis. Of note, there have been no studies that compare the cost and outcome of crystal-proven diagnosis versus clinical diagnosis.2
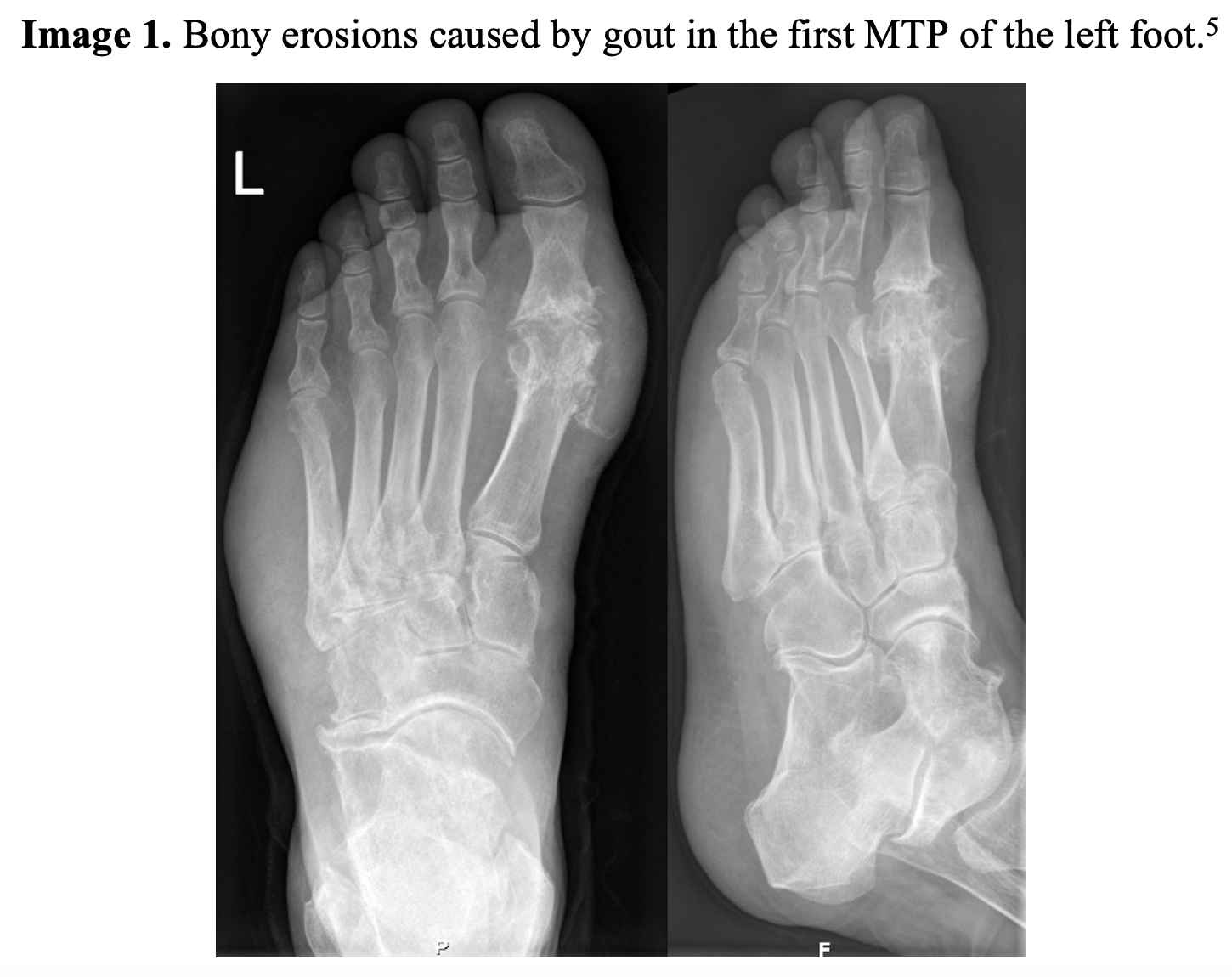
A septic joint is often the most important alternative consideration on the differential diagnosis of a painful joint, and gout and a septic joint can co-exist. Furthermore, the pain and swelling in gout is caused by an inflammatory response, so the synovial fluid can also appear cloudy, yellow, and have a significant number of WBCS (usually mostly neutrophils), similar to the synovial studies of a septic joint.1 A retrospective study of patients with a joint that was both infected and gouty stressed the importance of obtaining a culture even if there is a low number of leukocytes and no bacteria on gram stain of the synovial fluid.4 The authors further noted that the septic process within the joint can lead to crystal shedding, so the presence of crystals does not rule out a septic joint.4 A deeper discussion of septic arthritis can be found here and here. Imaging can be used to help diagnose gout. X-rays often only show non-specific soft tissue swelling unless the patient has advanced gout, which can manifest as a bony erosion (Image 1).1 In a retrospective chart review of 542 patients clinically diagnosed with gout, 85% of the X rays were read as “normal.” However, X-rays can help rule out alternative diagnoses for joint pain and swelling such as fracture.2
How do we treat gout flares?
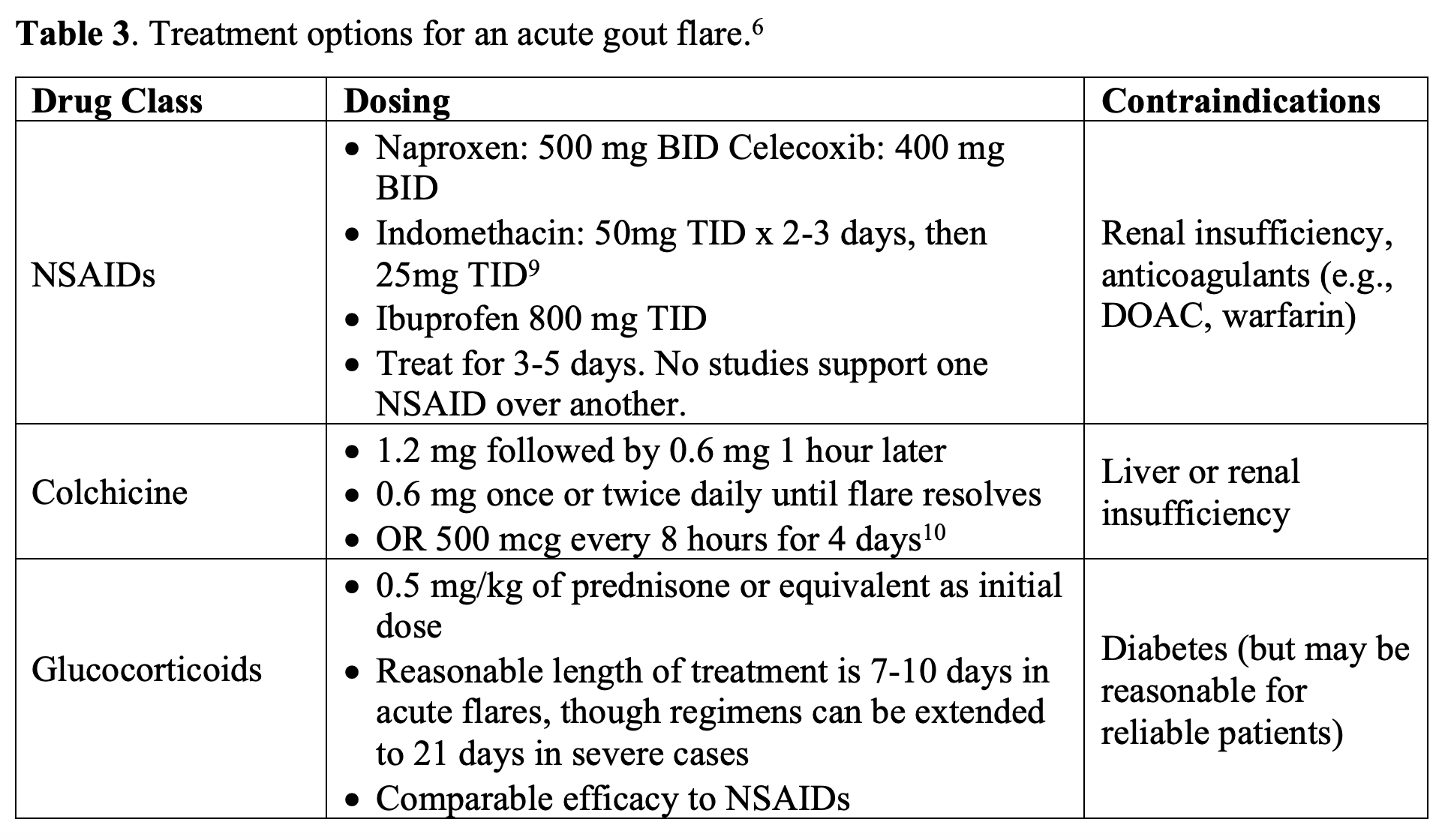
Gout flares are often self-limited and will self-resolve in 1-2 weeks. However, flares are quite painful, and treatment can significantly improve the patient’s pain and decrease the length of the flare.1 The most important determinant of therapeutic success is how soon treatment is started and that adequate dosing and duration of treatment is given.2 Guidelines recommend NSAIDs, colchicine, or steroids as the three main options.1 These drugs can be used alone or in combination.1 Notably, treatment with NSAIDs and corticosteroids in combination is generally not advised due to additive gastrointestinal (GI) toxicity.6-7 Treatment regimens should last until the flare has subsided. Acetaminophen does not treat the underlying pathology of inflammation and may not be beneficial in patients with acute gout flares.7 Additionally, aspirin should not be given as it can raise uric acid levels.8 Applying ice to the joint is often helpful for pain control.2 Finally, patients should be counseled on modifiable risk factors such as obesity and dietary choices.
How Can We Do Better?
First, the 2020 update on gout guidelines from the American College of Rheumatology now recommends initiating urate-lowering therapy (ULT) during gout flares.7 Generally, this is recommended for patients with tophi, radiographic damage attributable to gout, or frequent flares (2 or more per year). Allopurinol is preferred over febuxostat, which is preferred over probenecid. Doses are started low and titrated to affect.7 It is important to also prescribe anti-inflammatory prophylaxis (such as colchicine, NSAIDs, and/or steroids) to prevent acute gout flares during the first 3-6 months of ULT. Doses of allopurinol can start at 50-100 mg per day and increase by the same amount every 2-4 weeks to a maximum dose of 800 mg per day.11 As the patient will continue these medications for a prolonged period of time with a need for titration, patients should be encouraged to follow up closely with primary care.7
In a retrospective chart review from a single university hospital in the United States, an anti-inflammatory drug was given in 44% of visits and prescribed in 75% of visits.2 40% were given anti-inflammatories both in the ED and as a prescription. However, there were 20% who were NOT given an anti-inflammatory in the ED or as a prescription. Beyond this, 32% were given an opioid in the ED, and 52% were given a prescription for opioid.2 Furthermore, a 2021 recent retrospective study investigated 214 patients with acute gout flares.7 30% of these patients did not receive an anti-inflammatory at discharge, and 23.8% of patients seen in the ED or hospital with gout were prescribed opioids, with 82.3% of these patients not previously being on opioids. These prescribing patterns were noted in patients without specific contraindications, though opioids were seen more in patients with a history of gastroesophageal reflux.7 We reiterate that anti-inflammatory medications should be administered early in acute gout flares, unless there are specific contraindications, and that opioid analgesics should be reserved for patients with refractory pain or contraindications to other first line medications.
Key Points:
- It’s possible to diagnose acute gout flares clinically, but the gold standard is arthrocentesis. Use this whenever there is concern for a septic joint or if the clinical picture is not entirely consistent with an acute gout flare.
- Treatment of gout is anti-inflammatory medications, and this mostly means NSAIDs, corticosteroids, and colchicine.
- Avoid the combination of NSAIDs and corticosteroids due to additive GI toxicity.
- Remember there are contraindications to these medications. Pay attention to a patient’s kidney function, liver function, and history of diabetes.
- Certain patients may also be eligible for initiation of urate-lowering therapy even in an acute gout flare.
- Opioids are not a first-line treatment for gout, although they may be used if there are significant contraindicationsto anti-inflammatory medications.
References:
- Dalbeth N, Merriman TR, Stamp LK. Lancet. 2016; 388: 2039-2052.
- Schlesinger N, Radvanski DC, Young TC, McCoy JV, Eisenstein R, Moore RF. Diagnosis and treatment of acute gout at a university hospital emergency department. Open Rheumatol. J. 2015; 9: 21-26.
- Taylor WJ, Fransen J, Jansen TL, et al. Study for updated gout classification criteria (SUGAR): identification of features to classify gout. Arthritis Care Res 2015; 67: 1304–15.
- Yu KH, Luo SF, Liou LB, et. al. Concomitant septic and gouty arthritis – an analysis of 30 cases. Rheumatology. 2003;42: 1062-1066.
- Gichtfuss im Roentgenbild 002. Wikimedia commons.https://commons.wikimedia.org/wiki/File:Gichtfuss_im_Roentgenbild_002.png. Published November 17, 2010. Accessed November 17, 2021.
- Pillinger MH, Mandell BF. Therapeutic approaches in the treatment of gout. Arthritis Rheum. 2020; 50: S24-S30.
- Brunetti L, Vekaria J, Lipsky PE, Schlesinger N. Treatment of acute gout flares in the emergency department: Prescribing patterns and revisit rates. Ann Pharmacother. 2021:1-8.
- Roberts JR. InFocus: Treatment for gout. Emergency Medicine News. 2010; 32(5): 6-9.
- Burton JH, Fortuna TJ. Chapter 284: Joints and bursae. In: Judith E. Tintinalli, J. Stapczynski, O. John Ma, et al, editors. Tintinalli’s Emergency Medicine: A Comprehensive Study Guide (8th ed). New York: McGraw-Hill; 2015.
- Roddy E, Clarkson K, Blagojevic-Bucknall M, Mehta R, et. al. Open-label randomized pragmatic trial (CONTACT) comparing naproxen and low-dose colchicine for the treatment of gout flares in primary care. Annal Rheum Dis. 2020; 79: 276-284.
- Eggebeen AT. Gout: an update. Am Fam Physician. 2007; 76(6):801-808.





