Here’s another case from Medical Malpractice Insights – Learning from Lawsuits, a monthly email newsletter for ED physicians. The goal of MMI-LFL is to improve patient safety, educate physicians and reduce the cost and stress of medical malpractice lawsuits. To opt in to the free subscriber list, click here.
Chuck Pilcher, MD, FACEP
Editor, Med Mal Insights
Undiagnosed Hemorrhage while on Warfarin
Patients on warfarin at risk for bleeding deserve an INR
Facts: A 75-year-old female is admitted to the hospital from the ED with a DVT and presumed pulmonary embolus. She is treated for 5 days and discharged home on warfarin. At her follow-up visit with her PCP, her INR is low so her dosage is increased. A few days later she develops 10/10 hip and groin pain, calls 911 shortly after midnight, and returns to the ED via EMS. She is “moaning” in pain when seen by the PA-C with “spasms” in her thigh and inability to walk. No gait assessment is done, no imaging is ordered, and no INR is 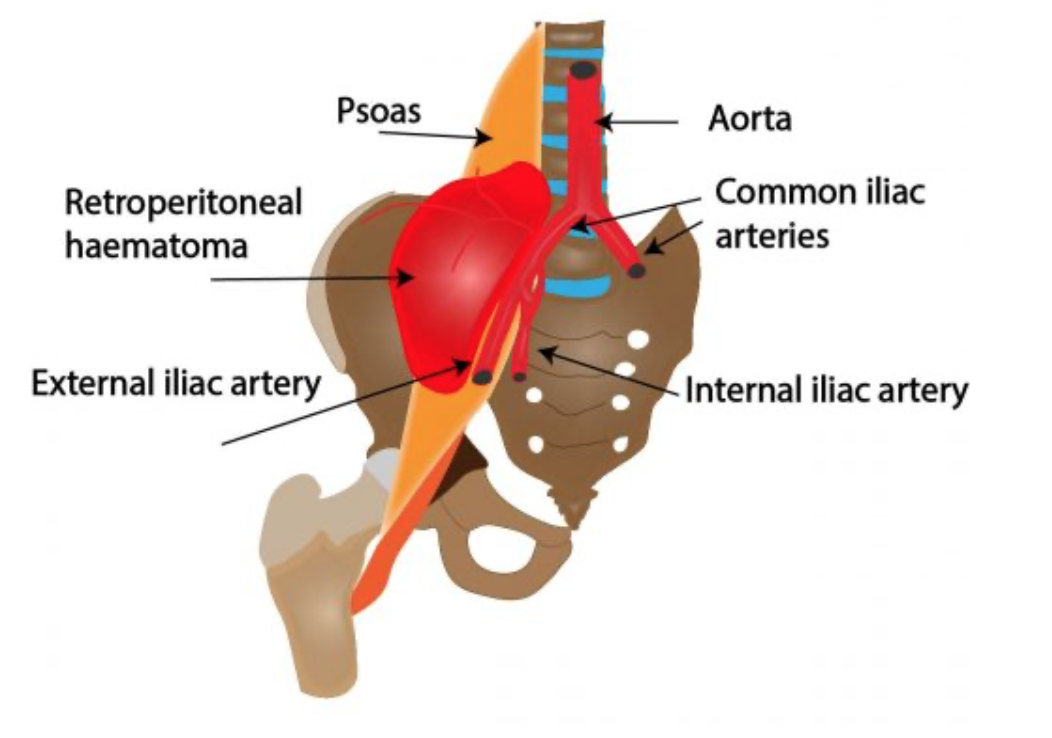 performed. After 10 hours in the ED and limited relief from 3 doses of narcotic analgesic, she is diagnosed with musculoskeletal pain and transferred to a nursing home. Eighteen hours after discharge, her flank pain increases, she develops SOB, and is transported back to the ED a third time. On arrival she is hypotensive with a hematocrit of 20 and an INR of 9.9. A massive retroperitoneal hemorrhage near her hip is found. She receives 11 units of PRBC but eventually expires. A lawsuit is filed against the PA-C, the supervising ED physician, and the hospital.
performed. After 10 hours in the ED and limited relief from 3 doses of narcotic analgesic, she is diagnosed with musculoskeletal pain and transferred to a nursing home. Eighteen hours after discharge, her flank pain increases, she develops SOB, and is transported back to the ED a third time. On arrival she is hypotensive with a hematocrit of 20 and an INR of 9.9. A massive retroperitoneal hemorrhage near her hip is found. She receives 11 units of PRBC but eventually expires. A lawsuit is filed against the PA-C, the supervising ED physician, and the hospital.
Plaintiff: Because I had been recently discharged on warfarin, my sudden hip pain should have alerted you to a possible hemorrhage in my hip or pelvis. You should have checked my INR. If you had, then an ultrasound, CT, or MRI of my hip would have shown the problem. You didn’t even get an x-ray to see if I might have had a fracture. In fact, you never even asked me to stand up and walk. Because of your negligence, I continued to bleed, developed complications, and died. I could still be alive if you had been more careful.
Defense: If your INR had been too high, we would have stopped your warfarin and you would have had another blood clot and PE. If it had been too low, we would have increased your warfarin and you would have had the same problem. You can’t have it both ways. Even if we had done tests and treated you appropriately, the same result would have occurred. [This is a “causation” defense. cp]
Result: After a 6 day trial and 9 hours of deliberation, the jury awarded $570,000 to the surviving spouse and children.
Takeaways:
- Take a decent history from patients on anticoagulants.
- Patients on warfarin, especially those who have just started the drug or had their dose changed, need to have their INR’s carefully monitored.
- Sudden onset of pain is a symptom of hemorrhage/hematoma and should be in the differential of anticoagulated patients.
- Do a “road test” before discharge. Patients who can’t walk are high risk, especially if you haven’t addressed why they can’t walk.
- Fortunately, we may assume that the average ED physician OR PA-C would have managed this case better. A jury apparently believed so.
Reference: Nontraumatic Retroperitoneal Hematoma After Warfarin Administration: Fatal Case Report and Review of the Literature.Hosseini M et al. Am J Forensic Med Pathol. 2015 Dec;36(4):245-8.
In case you missed it:
COVID-19 ALERT
EvergreenHealth in Kirkland, WA, is the first US hospital impacted by the COVID-19 outbreak that began at a SNF < 2 miles from the ED. Rob Orman interviewed Emergency Physician Pat Reinfried on a HippoED podcast about how the patient surge is being managed. The link to the conversation has been posted on emDocs and is packed with front-line experience and information that will save lives – perhaps even yours. Check out “COVID: Lessons Learned and First Hand Account From Kirkland, WA.”






