Author: Seth Lotterman, MD (Assistant Professor of EM, Univ of Connecticut School of Medicine) // Edited by: Alex Koyfman, MD & Justin Bright, MD
It’s a typical busy afternoon ED shift for you. The rack seems to be overflowing, and 3 new patients have just checked in. All have abdominal pain. You have a systematic approach to your abdominal pain patients. But, does your approach keep one critical diagnosis in mind?
The first patient is a 75 year-old female with atrial fibrillation, and she is complaining of acute diffuse abdominal pain which she rates 8/10. She also states she feels very nauseated, but has not yet vomited. Her vital signs are within normal range, and she is afebrile. On exam she has an irregularly irregular rhythm, has clear lungs bilaterally, and displays diffuse mild tenderness on abdominal exam without guarding or rebound.
The second patient is a 68 year-old male with several hours of constant diffuse abdominal pain that began after eating dinner. He has had similar pain after eating in the past, but it has never lasted this long. He has a history of coronary artery disease, hypertension, and hypercholesterolemia. His vital signs are also within normal range, and he is afebrile. On exam he has a regular cardiopulmonary exam, and diffuse mild tenderness on abdominal exam without guarding or rebound.
The third patient is a 30 year-old female with constant upper abdominal pain which started 2 days ago, but is now worsening. She reports a history of DVT several years ago but is no longer on anticoagulation therapy. On further history she does mention that her mom also had a blood clot when she was younger. On exam she has a normal cardiopulmonary exam, and diffuse mild tenderness on abdominal exam without guarding or rebound.
Question: Is there a single clinical entity that could be the cause of pain in all three of these patients?
Answer:
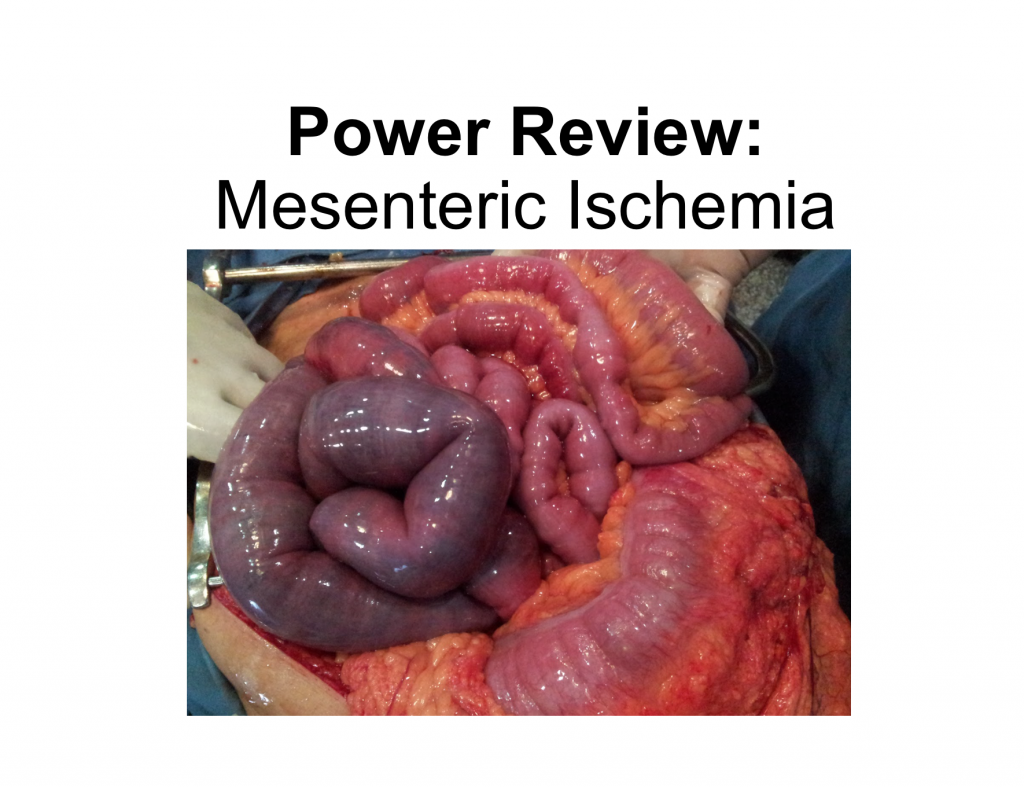
All three patients have mesenteric ischemia. While it is a rare cause of abdominal pain, it carries a high morbidity and mortality. Mesenteric ischemia has an annual incidence of 0.09% to 0.2% per patient year, although this may be underreported.1 Approximately 1% of acute abdomen hospitalizations are the result of mesenteric ischemia and it occurs in one in 1,000 patients presenting to emergency departments.2
Mesenteric ischemia can be the result of several different pathologies. Acute arterial embolus accounts for approximately 40-50% of cases. Emboli lodge in the superior mesenteric artery (SMA) resulting in acute onset of pain. There are multiple predisposing factors, including atrial fibrillation, cardiomyopathy, recent angiography, and valvular disorder such as rheumatic valve disease. Mortality rate have remained greater than 50% after surgical embolectomy over the past 4 decades.3,4
Acute arterial thrombosis usually presents as intermittent pain that becomes constant (intestinal angina). Patients may develop food fear because the pain becomes intense after eating. Acute thrombosis most often occurs as a result of atherosclerosis – either acute plaque rupture or gradual build up until critical stenosis. Other risk factors include hypercoagulability, estrogen therapy, and prolonged hypotension. In some cases, the occlusion is amenable to embolectomy by interventional radiology. More commonly, the patient will require open laparotomy and bowel resection if there is infarcted bowel. Mesenteric ischemia that requires surgery carries a particularly high mortality rate of greater than 70%.3,4
Although mesenteric ischemia is commonly thought to be an arterial pathology, venous thrombosis causes about 10-15% of cases. These patients may present with diarrhea, and a longer history of pain. The treatment is usually anticoagulation, although surgery may be indicated depending on how severe the ischemia is on presentation. Risk factors for mesenteric venous thrombosis include oral contraceptives or estrogen therapy, malignancy, hypercoagulability, portal hypertension, portal vein thrombosis or other deep vein thrombosis, sickle cell disease, hepatosplenomegaly, hepatitis, pancreatitis, coagulopathic states, sepsis, cigarette smoking, prior abdominal surgery, and alcohol use.3,4
Non-occlusive mesenteric ischemia is the etiology of about 20% of cases and is the result of low-flow states due to hypotension, hypovolemia, heart failure, or sepsis. A vicious cycle then occurs as the ischemia results in more hypotension which results in more ischemia and then more hypotension. Some medications such as cocaine, digitalis, ergot alkaloids and vasopressors (alpha-constricting agents) can be associated with this condition as well.3,4
Overall mortality is up to 60-80%, especially in patients with greater than a 24-hour delay in diagnosis or presentation.3 Twenty-four hour delay decreases survival by 20%2. Surgical intervention that can be initiated in less than 6 hours from symptom onset adds significant increase in survival.5
Unfortunately there are no presenting characteristics, historical features, or findings on physical examination that definitively establish the diagnosis.1 Patients often present with non-specific symptoms of vomiting and/or diarrhea and abdominal pain due to initial gut emptying4, making early diagnosis challenging. The classic exam finding of pain out of proportion to exam is due to ischemic visceral pain. It is intense and constant, does not increase with palpation and initially does not result in abdominal wall rigidity or other peritoneal signs.4 It is not until later stages that peritoneal inflammation and localization of pain in the abdomen occur.4
Early diagnosis is challenging because of the wide variability in clinical presentation of mesenteric ischemia.2 While multi-detector CT angiography is fairly sensitive (64-93%) and specific (92-100%) for this disease1,7, lab testing is less helpful. Both lactate and d-dimer are sensitive, 86% and 96% respectively, but only 44% and 40% specific.1 One review article found that there is no single serum marker that is specific and elevated early enough in the serum to diagnose acute mesenteric ischemia.1,6 White blood cell count over 20,000 ml/cc3 can be seen, but is not specific to mesenteric ischemia.2 Lactate is not elevated until late in the disease process as the liver will clear the lactate initially.4 Neither D-dimer nor lactate is sensitive enough to rule out disease if negative.1
In the end, it will take a high degree of suspicion on the part of the physician, taking into account the constellation of history, physical, labs, and CT angiography to arrive at the diagnosis. While there are some identifiable risk factors and laboratory test results may be suggestive of mesenteric ischemia, this will continue to be difficult for emergency physicians to diagnose due to the wide variety of presentations, the lack of a single blood test that rules in or out the diagnosis, and the rareness of the condition. However, if you do not keep it on your differential of abdominal pain, you will never be able to make the diagnosis. The take-home is to keep this diagnosis in your differential when evaluating patients with abdominal pain. Lab tests such as WBC, d-dimer, and lactate can be helpful in diagnosing this disease, although none are good enough to rule out the disease. If you suspect the diagnosis, multi-detector CT-angiography is the test of choice. Early surgical involvement is also important.
References / Further Reading:
1. Cudnik, M et al. The Diagnosis of Acute Mesenteric Ischemia: A Systematic Review and Meta-analysis. Academic Emergency Medicine, November 2013, Vol. 20, No. 11
2. van den Heijkant TC et al. “Diagnosis of mesenteric ischemia.” World J Gastroenterol 2013 March 7; 19(9): 1338-1341
3. Lewiss RE, Egan DJ, Shreves A. “Vascular Abdominal Emergencies” Emerg Med Clin N Am 29 (2011) 253–272
4. Sise M. “Acute Mesenteric Ischemia” Surg Clin N Am 94 (2014) 165–181
5. Wadman M, Syk I, Elmsta° hl S. Survival after operations for ischaemic bowel disease. Eur J Surg 2000;166(11):872–7.
6. Demir IE, Ceyhan GO, Friess H. “Beyond Lactate: Is There a Role for Serum Lactate Measurement in Diagnosing Acute Mesenteric Ischemia?” Dig Surg 2012;29:226–235
7. Moschetta M, Telegrafo M, Rella L, Stabile Ianora AA, Angelelli G. Multi-detector CT features of acute intestinal ischemia and their prognostic correlations. World J Radiol 2014; 6(5): 130-138
8. http://www.ncbi.nlm.nih.gov/pubmed/24051008
9. http://www.ncbi.nlm.nih.gov/pubmed/18180128
10. http://www.mdguidelines.com/mesenteric-thrombosis
11. http://www.vascularweb.org/vascularhealth/Pages/mesenteric-ischemia.aspx








3 thoughts on “Mesenteric Ischemia: A Power Review”
This is a good reminder- thank you for very well researched summary. Have you looked at bedside ultrasound for identification of thickened bowel wall?..sometimes one can map it to a vascular distribution- or alternatively look at the SMA branch for flow or excess calcification. I have tried power doppler to check for vascularity of the thickened bowel segment, but have not enough experience yet to know what constitutes abnormal. This would be useful research if anyone is interested.
Pingback: emDOCs.net – Emergency Medicine EducationRenal colic mimics: Differential diagnosis and approach to management - emDOCs.net - Emergency Medicine Education
Pingback: REBEL Core Cast 45.0 - Mesenteric Ischemia - REBEL EM - Emergency Medicine Blog