Authors: Nathan LeDeaux, MD (EM Resident Physician, University of Wisconsin) and Benjamin Schnapp, MD (EM Assistant Program Director, University of Wisconsin) // Reviewed by: Courtney Cassella, MD; Alex Koyfman, MD (@EMHighAK); Brit Long, MD (@long_brit)
A 28-year-old male who is currently incarcerated at a local prison is brought to the emergency department (ED) secondary to a spreading skin rash. On arrival, you note a well-appearing male with numerous tattoos of various styles. His right shoulder has a large area of erythema that appears to be spreading from a quarter-sized tattoo. There are multiple papules, pustules, and ulcerations in the tattooed area overlying the erythema. He states that this tattoo was done by a friend in prison one week ago with the cut end of a plastic pen and pen ink diluted with water. The redness has been spreading from the area of the tattoo over the course of a week and has been increasingly painful. He has noticed no drainage from the wound.
Questions
What antibiotics should be used to cover this patient’s suspected infection?
Are there any complications that need to be urgently assessed for due to the method of tattoo application?
Background
Tattooing, pigmentation of the skin by the introduction of various substances into the dermis is far more varied and complex than many believe. Presenting to a tattoo parlor that uses sterilized instruments, standard precautions, and commercial inks is not a universal practice. Commercial tattoo parlors have varying levels of regulation based on their geographic area and a wide variety of compliance with health standards given the lack of standardized training and licensure in many states [1,2].
Tattoos are extremely common; 24% of the US population from late childhood to the age of 60 is estimated to have a tattoo [1]. While complications are relatively rare, the significant prevalence of tattooing means that complications are common. The most common short-term complications are localized infection and allergic dermatitis. While these complications are easily managed by conservative measures and/or by outpatient providers, they may also present to the ED for assessment. Long-term complications such as skin cancer, localized activation of autoimmune conditions, and chronic skin changes may also result and be first noticed by emergency providers [1].
There are two main methods of cosmetic tattooing: the use of an electric “tattoo gun” that has multiple needles and reciprocates with an electric motor or electromagnet and “hand poke” which is performed with a handheld needle or needles. The incidence and severity of complications vary most greatly based on the experience of the artist, the use of properly sterilized instruments, and materials as opposed to the method of application [1,3].
Common complications
The two acute complications of tattooing are immunologic reactions and infections. The occurrence of immunologic complications is primarily related to the type of pigment used while infectious complications are related to the sterility of the instruments in question.
Infections
Infection is always a risk with tattooing. Professional tattoo artists reduce this risk by sterilizing instruments, preparing the skin, using standard precautions, and providing after care instructions to clients to minimize this risk. Amateur tattoos including those done with home-made instruments such as needles, razors, or pens have a significant risk of infection. This risk is increased by the use of non-sterile inks, lack of skin preparation, and lack of appropriate after care [1,3].
Folliculitis, Cellulitis, and Impetigo
Staphylococcus aureus and Streptococcus pyogenes are the most common microbes that are implicated in tattoo-related skin infections [4]. These microbes are all implicated in the development of folliculitis, cellulitis, and impetigo, any of which can occur in the setting of a tattoo. Folliculitis is defined by the presence of small papules and pustules centered around follicles, cellulitis by spreading redness and edema from a central source, and impetigo by erosion and serous crusting.
In the setting of a tattoo related infection note that the “central source” of spreading cellulitis may be the entire tattoo, one color of the tattoo, or one small area of the tattoo. Cellulitis typically presents as ongoing spreading redness two or more days after tattooing. Impetigo generally develops later than cellulitis, with redness and crusting developing two or more days after tattooing. Folliculitis tends to form one to three days after tattooing in the area that was shaved prior to the tattoo or an area that was wrapped with cling wrap to protect the new tattoo.
Treatment of these conditions in the setting of a tattoo does not differ from their usual emergency department treatment [4,5].
- Folliculitis: Topical mupirocin 2% TID for 5 days
- Cellulitis: Cephalexin 500 mg QID for 7 days
- Impetigo: Either of the above treatments
For more information on the presentation of cellulitis see our article on cellulitis and its mimics in the ED.
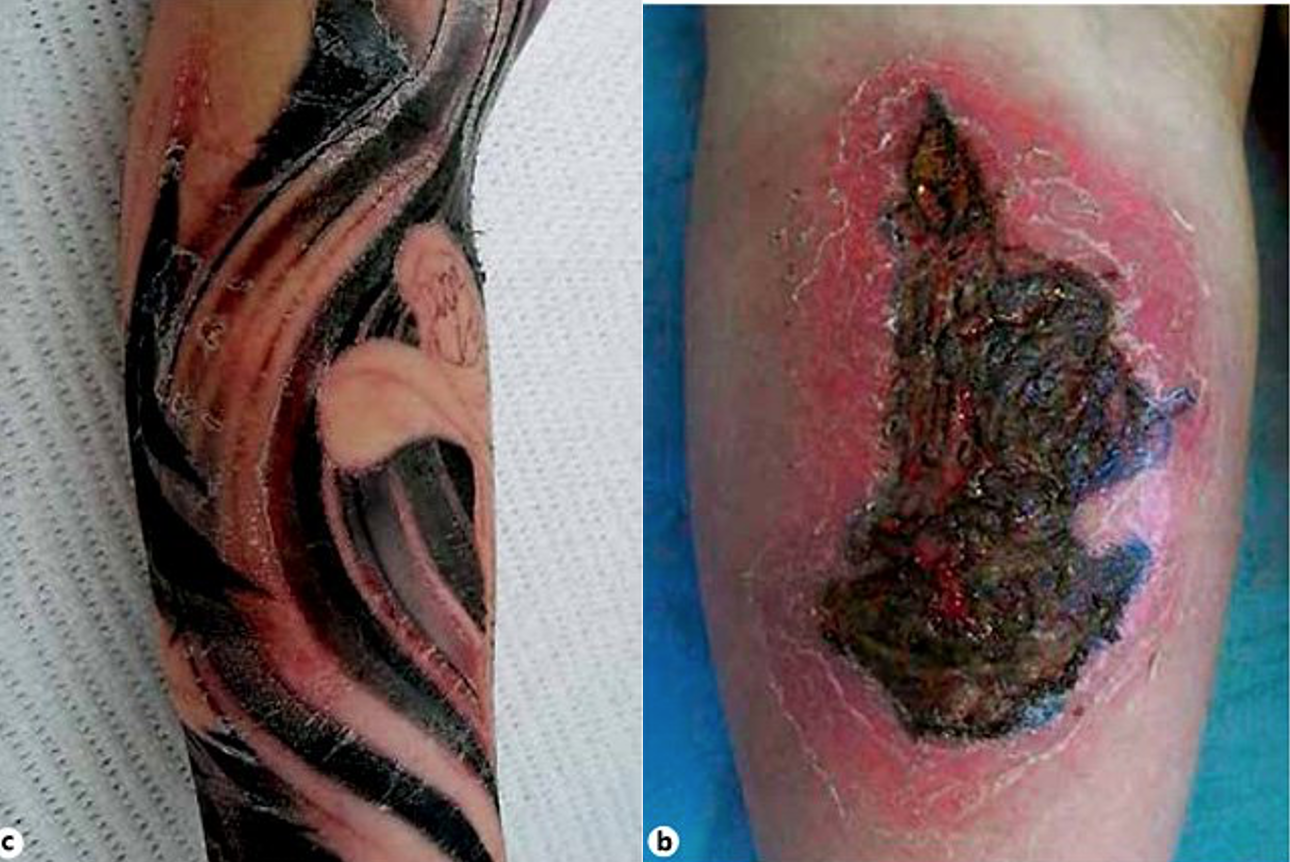
Cellulitis in the setting of a tattoo. Left image with multifocal spreading redness from multiple areas of the tattoo. Right image with large central ulcerated area with cellulitis surrounding.

Classic cellulitis not associated with a tattoo. Note the roughly oval-shaped spread.

Classic folliculitis with pustules surrounding hair follicles.

Serous crusting over lesions typical of impetigo. Lesions over tattoos may be difficult to diagnose.
Mycobacterial
Mycobacterium chelonae and other nontuberculous mycobacterial are seen in certain tattoos. These pathogens are commonly present within grey areas of the tattoo. Grey coloration is obtained by diluting black in with water. If non-sterile water is used, these normally non-pathogenic waterborne organisms can enter the skin and cause disease [7].
These infections generally present with “erythematous papules, nodules, pustules, ulcers, abscesses, or plaques [6].” Lesions with multiple morphologies are often present in various stages of healing [1,7]. They can develop any time after tattooing but are commonly seen months to weeks after placement of the tattoo due to the slow growth rate of mycobacteria.
These lesions should be cultured if drainage is seen and referred for biopsy if there are no active areas of drainage. Treatment should be begun in the ED and the patient should be referred to a dermatologist for follow up and potential biopsy. Treatment often requires months of dual antibiotics.
- Antibiotic choice is guided by culture and susceptibility results; empiric treatment should not be started without dermatology consultation [4].

Mycobacterial infection in recent tattoo, note areas of erythema and ulceration with no clear pattern of spread.

Mycobacterial infection in a chest tattoo. Note the multiple morphologies of lesions with uninvolved skin between.

Mycobacterial infection in an arm tattoo.
Abscess
Abscess is rare in the setting of a tattoo given that the skin is generally only punctured to the level of the dermis. If fluctuance, purulent drainage, or mass is seen, consider incision and drainage along with antibiotic coverage for soft tissue infection (SMX-TMP 320mg/1600mg BID for 7 days) [5].
- If the patient is toxic appearing, hypotensive, or immunocompromised, inpatient admission with broad-spectrum empirical coverage is recommended (cefepime or piperacillin/tazobactam plus vancomycin) [5,9].
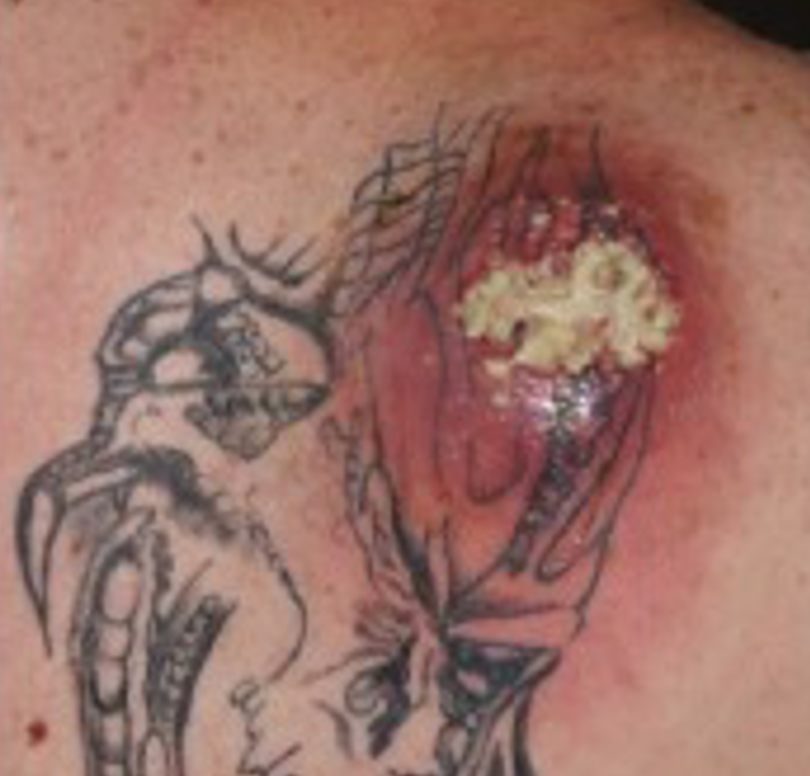
Abscess formation in a recent chest tattoo.
Necrotizing infections
More severe infections such as necrotizing fasciitis, gangrene, ecthyma, and erysipelas can occur as a result of tattooing. These complications are associated with traditional “hand poked” tattoos where instruments penetrate more deeply into the skin [3,4]. Fortunately, these infections are rare, and their treatment does not differ in the presence of tattoos.
- Pain out of proportion to exam, rapidly expanding erythema, and crepitus to palpation may occur and should trigger evaluation with imaging (i.e., ultrasound, CT).
- Immediate surgical consultation is recommended in all cases of suspected necrotizing infection.
- Broad spectrum antibiotics should be administered [9].
- Piperacillin-Tazobactam 4.5 g Q 8 hours
- Vancomycin 15 mg/kg up to 2000mg Q 8 hours
- Clindamycin 900 mg Q 8 hours
Hepatitis and HIV
Systemic viral infections such as hepatitis C, hepatitis B, and HIV can all be transmitted through tattooing. This risk is only associated with poor sterilization of instruments between clients and with amateur tattoos performed in groups with homemade equipment [1,4].
Immunologic reactions
The pigments used for tattoo application are not regulated by the US Food and Drug Administration [1]. Many colored inks utilize metal salts, carbon compounds, and organic colorants. Any of these can cause the following immunologic reactions.
Allergic Contact Dermatitis
Many tattoo pigments can cause contact dermatitis. This is more common in individuals with previous episodes of contact dermatitis in response to metals such as nickel, gold, and cobalt. This reaction is defined by the presence of pruritic papules and vesicles on an erythematous base. Given the large amount of antigen, bullae and crusts may form on the surface of the skin [1,6]. This reaction can spread outside of the tattooed area and may be the result of an allergen to ointments used for after-care as opposed to the tattoo itself [4]. These reactions can occur at nearly any time but are almost always progressive. They begin with mild symptoms in one area that do not resolve and spread to other similar areas of the tattoo.
- Treat with steroid ointments such as clobetasol 0.05% or triamcinolone 0.1% twice daily until follow up with PCP [7].
- For large tattoos of 20% or more total body surface area consider prednisone 0.5 – 1mg/kg daily for 7 days and dermatology referral [6].

Plaque-like presentation of contact dermatitis in the red area of the tattoo.

Papular/nodular presentation of contact dermatitis in the red area of the tattoo.
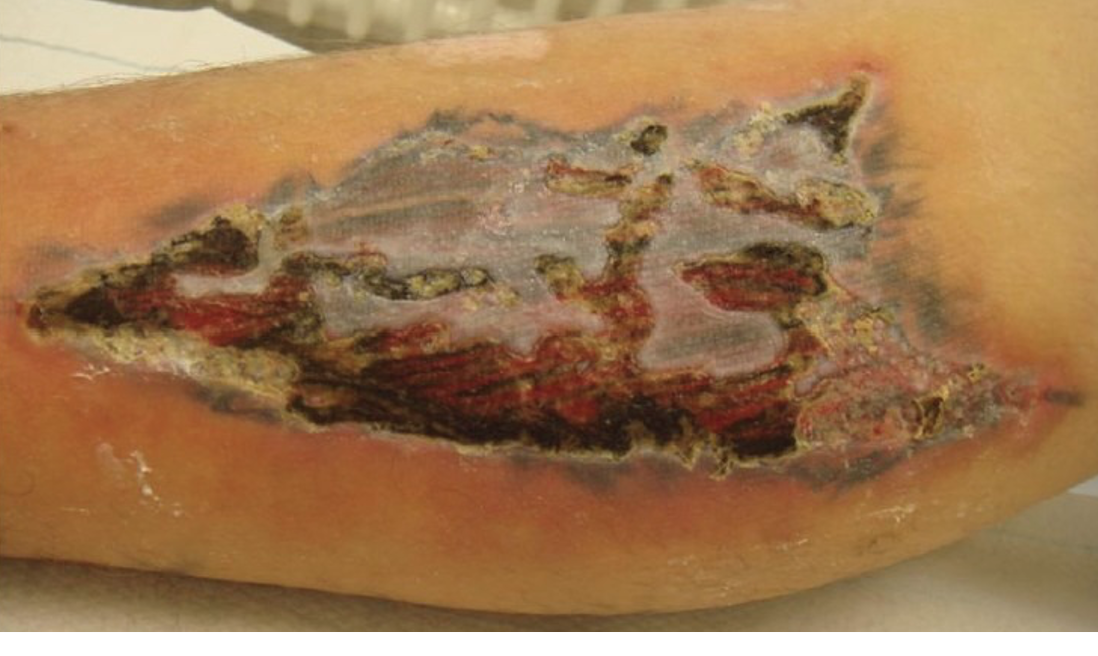
Desquamating presentation of contact dermatitis throughout an entire tattoo. Note the disconnect between the severity of desquamation over the tattoo and the relative minor ring of reactive erythema surrounding the tattoo arguing against infection. Lab work, a detailed history of the lesion’s appearance, and follow up with dermatology is likely to be required to fully rule out cellulitis.
Photosensitivity
Some patients report a burning sensation, pruritus, and localized edema in the area of a tattoo following significant sun exposure. This is thought to be related to breakdown of pigment molecules and does not lead to long-term harm. This reaction can occur in a tattoo of any age but is generally more severe in newer tattoos. The use of a strong sunscreen may prevent recurrent symptoms [8]. This is one of the most common complications of tattooing and can lead to pervasive symptoms in individuals who live in areas of significant sun exposure [3].
- Diphenhydramine 25 to 50mg PO BID may be used for acute pruritus and pain.

Photodermatitis, note the edematous and raised appearance of the entire tattoo without surrounding skin changes.
Lichenification
The most common type of sustained skin reaction to a tattoo [1]. Presents as flat-topped papules or plaques both on the tattoo and in nearby normal skin. These lesions are only mildly pruritic and are not associated with underlying erythema or edema. Like other allergic reactions these lesions may arise at any time. Unlike other allergic reactions symptoms may resolve and recur in various areas of the tattoo.
- Referral to a dermatologist is required; topical, systemic, and injectable treatments are all used and vary based on biopsy results.

Red areas of lichenoid reactions on and around a tattoo. Note that the areas of lichenification randomly appear in and around the tattooed area.

Red and scale covered areas of lichenoid reaction on and around a tattoo.
Case conclusion
This patient’s amateur tattoo performed with non-sterile instruments, pigments, and water is suspicious for a localized infection. The spreading redness and edema from the site likely represents cellulitis and the polymorphic lesions overlying the area of cellulitis are concerning for codominant infection with a non-tuberculous mycobacterial infection. The patient’s cellulitis is treated with cephalexin and dermatological consultation is obtained for biopsy and culture of the suspected mycobacterial lesions. Serology for HIV, hepatitis C, and hepatitis B should be sent given the method of application of this patient’s tattoo. Follow up will be required with the prison health system for ongoing HIV and hepatitis testing given the recency of this patient’s exposure.
Pearls and Pitfalls
- Multiple complications of tattooing can be present in a single area. Consider dermatology consultation for any patient who has lesions of multiple morphologies.
- Normal skin flora is the most common organism implicated in tattoo-related infections.
- Life-threatening conditions that result from tattoos do not change in presentation as a result of a tattoo. Necrotizing infections and sepsis as a result of severe infection should always be considered.
References
- Islam, P.S., Chang, C., Selmi, C. et al. Medical Complications of Tattoos: A Comprehensive Review. Clinic Rev Allerg Immunol 50, 273–286 (2016). https://doi.org/10.1007/s12016-016-8532-0
- Ncsl.org. 2021. Tattooing and Body Piercing | State Laws, Statutes and Regulations. [online] Available at: <https://www.ncsl.org/research/health/tattooing-and-body-piercing.aspx> [Accessed 2 August 2021].
- Serup J, Carlsen KH, Sepehri M. Tattoo complaints and complications: diagnosis and clinical spectrum. Curr Probl Dermatol. 2015;48:48-60. doi:10.1159/000369645
- Kluger N. Acute complications of tattooing presenting in the ED. The American Journal of Emergency Medicine. 2012;30(9):2055-2063. doi:10.1016/j.ajem.2012.06.014
- Ramakrishnan K, Salinas RC, Agudelo Higuita NI. Skin and Soft Tissue Infections. Am Fam Physician. 2015;92(6):474-483.
- Ryan R. Falsey, Michael H. Kinzer, Stanley Hurst, Andrea Kalus, Paul S. Pottinger, Jeffrey S. Duchin, Jiong Zhang, Judith Noble-Wang, Michi M. Shinohara, Cutaneous Inoculation of Nontuberculous Mycobacteria During Professional Tattooing: A Case Series and Epidemiologic Study, Clinical Infectious Diseases, Volume 57, Issue 6, 15 September 2013, Pages e143–e147, https://doi.org/10.1093/cid/cit347
- Usatine RP, Riojas M. Diagnosis and management of contact dermatitis. Am Fam Physician. 2010;82(3):249-255.
- Hutton Carlsen K, Serup J. Photosensitivity and photodynamic events in black, red and blue tattoos are common: A ‘Beach Study’. J Eur Acad Dermatol Venereol. 2014;28(2):231-237. doi:10.1111/jdv.12093.
- Stevens DL, Bisno AL, Chambers HF, Dellinger EP, Goldstein EJ, Gorbach SL, Hirschmann JV, Kaplan SL, Montoya JG, Wade JC. Practice guidelines for the diagnosis and management of skin and soft tissue infections: 2014 update by the infectious diseases society Clin Infect Dis. 2014 Jul 15;59(2):147-59. doi: 10.1093/cid/ciu296.
Images
All images contained within this article are licensed under the international Creative Commons Standard for non-commercial reuse. When utilizing these images please refer to the Creative Commons standards and attribute all original sources. Below are the individual sources for each of the above images.
i. Serup J, Carlsen KH, Sepehri M. Tattoo complaints and complications: diagnosis and clinical spectrum. Curr Probl Dermatol. 2015;48:48-60. doi: 10.1159/000369645. Epub 2015 Mar 26. PMID: 25833625.
ii. Cellulitis | DermNet NZ. https://dermnetnz.org/topics/cellulitis/.Accessed August 14, 2021.
iii. Folliculitis | DermNet NZ. https://dermnetnz.org/topics/folliculitis/.Accessed August 14, 2021.
iv. Impetigo | DermNet NZ. https://dermnetnz.org/topics/impetigo/. Accessed August 14, 2021.
v. Kay MK, Perti TR, Duchin JS. Tattoo-associated Mycobacterium haemophilum skin infection in immunocompetent adult, 2009.Emerg Infect Dis. 2011;17(9):1734-1736. doi:10.3201/eid1709.102011
vi. Whitaker J, Rickaby W, Robson A, Bakr F, White J, Rinaldi CA. Recurrent pocket infection due to mycobacterium chelonae at the site of an explanted cardiac implantable electrical device in proximity to a long-standing tattoo.HeartRhythm Case Reports. 2016;2(2):132-134. doi:10.1016/j.hrcr.2015.10.012
vii. Tattoo-associated skin reactions. Tattoo-associated skin reactions | DermNet NZ. https://dermnetnz.org/topics/tattoo-associated-skin-reactions/. Accessed August 14, 2021.
viii. Wollina U. Severe adverse events related to tattooing: an retrospective analysis of 11 years.Indian J Dermatol. 2012;57(6):439-443. doi:10.4103/0019-5154.103062
ix. Tattoo-associated skin reactions. Tattoo-associated skin reactions | DermNet NZ. https://dermnetnz.org/topics/tattoo-associated-skin-reactions/. Accessed August 14, 2021.
x. Tattoo-associated skin reactions. Tattoo-associated skin reactions | DermNet NZ. https://dermnetnz.org/topics/tattoo-associated-skin-reactions/. Accessed August 14, 2021.
xi. Wollina U. Severe adverse events related to tattooing: an retrospective analysis of 11 years.Indian J Dermatol. 2012;57(6):439-443. doi:10.4103/0019-5154.103062
xii. Khunger N, Molpariya A, Khunger A. Complications of Tattoos and Tattoo Removal: Stop and Think Before you ink.J Cutan Aesthet Surg. 2015;8(1):30-36. doi:10.4103/0974-2077.155072
xiii. Bassi A, Campolmi P, Cannarozzo G, et al. Tattoo-associated skin reaction: the importance of an early diagnosis and proper treatment.Biomed Res Int. 2014;2014:354608. doi:10.1155/2014/354608
xiv. Tattoo-associated skin reactions. Tattoo-associated skin reactions | DermNet NZ. https://dermnetnz.org/topics/tattoo-associated-skin-reactions/. Accessed August 14, 2021.






