Authors: Adam Bossert, MD (EM Resident Physician at the Hospital of the University of Pennsylvania); Kevin R. Scott, MD, MSED (EM Attending Physician at the University of Pennsylvania) // Reviewed by: Alex Koyfman, MD (@EMHighAK) and Brit Long, MD (@long_brit)
Case
A 65-year-old male with hypertension presents with left hip pain after a fall from standing 1 day ago. The patient tripped on a curb and fell on his left hip. He is now having difficulty bearing weight and arrived in a wheelchair. His vitals are within normal limits. On exam there is no gross deformity of his lower extremity, but he has point tenderness overlying his left greater trochanter. The patient has intact distal pulses and normal capillary refill in his bilateral lower extremities. His sensation to light touch is also intact. Strength exam in the left lower extremity is limited due to pain with movement of the left hip and knee.
Background
The femur is the longest and strongest bone in the body and typically requires significant force to fracture in young, healthy individuals. Most commonly this force comes from car accidents or other high energy mechanisms. However, femur fractures in the elderly can occur with lower energy mechanisms, such as falls from standing, and are associated with significant morbidity and mortality with 15-30% of elderly individuals dying within 1 year after suffering a hip fracture.1,2 Regardless of the population affected it is important for emergency physicians to recognize and understand femur fractures in order to expeditiously diagnose and treat these injuries to avoid delays in care and potential complications.
The different patterns of femur fractures are associated with varying mechanisms and amounts of force. Fractures sustained in high-speed motor vehicle accidents may be more obvious and can often be identified during an initial trauma evaluation. Classically, when there is an associated displacement of the fracture, the foot on the ipsilateral side will be turned at an abnormal angle giving it the appearance that it is shorter than the contralateral leg. In contrast, fractures from falls or stress fractures may be less obvious on exam, however they also present with pain, especially when bearing weight. Femoral stress fractures occur most often in the extremely active population such as long-distance runners or in patients with decreased bone mineral density (i.e. osteopenia, osteoporosis, medication induced). These injuries tend to develop over time as a result of repeated applied force. This post will emphasize traumatic fractures as these represent a larger percentage of the femoral fractures we will see in the emergency department.
Emergency medicine physicians must be adept at describing fractures in order to effectively relay important information to our surgical colleagues. We recommend reviewing the EMDocs Fracture Terminology post as these terms are used throughout the remainder of this post.
Review of Femur Anatomy
Bony and Muscular Anatomy
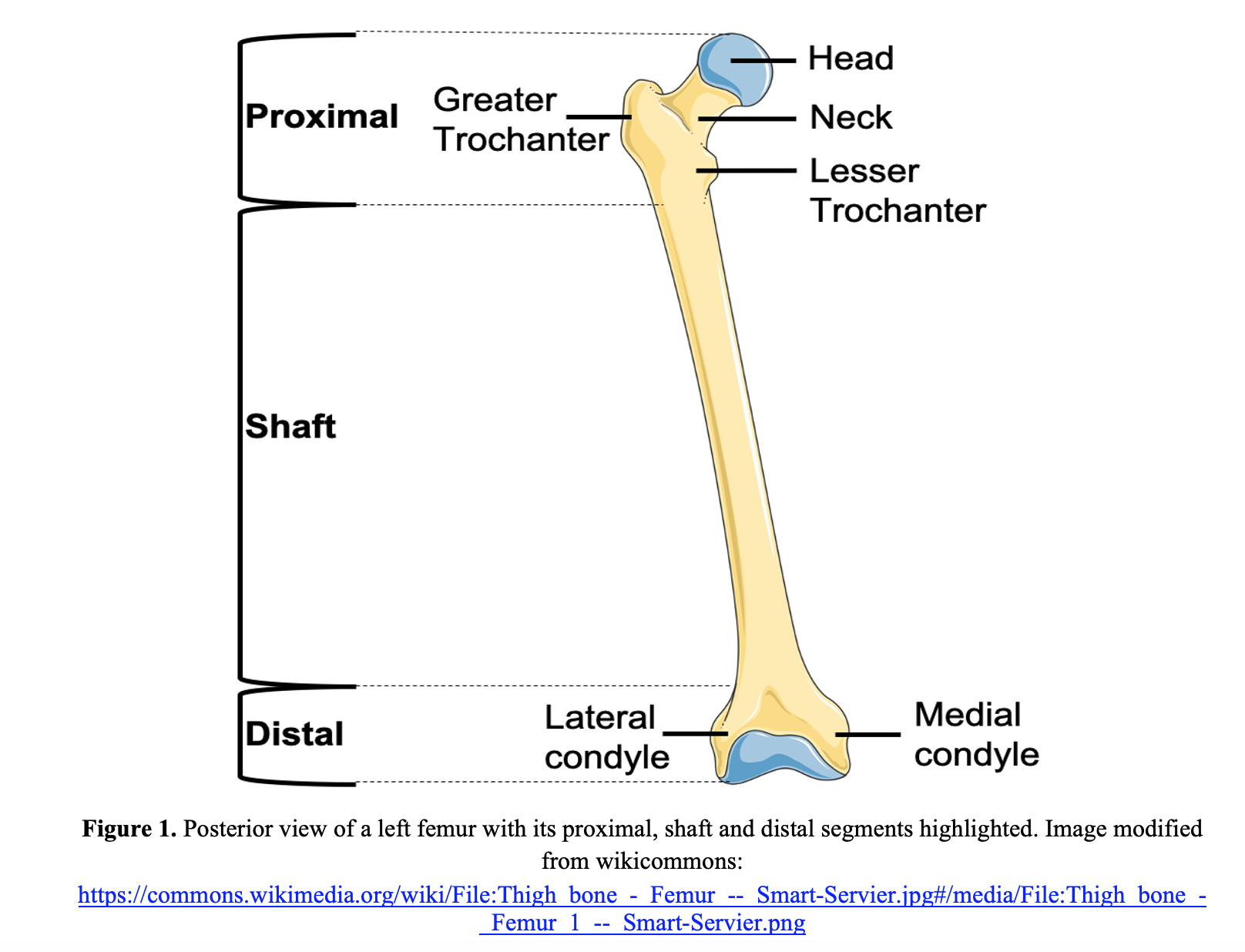
The femur is divided into three parts: proximal aspect, shaft, and the distal aspect (Figure 1). Fractures can occur in any of these areas.
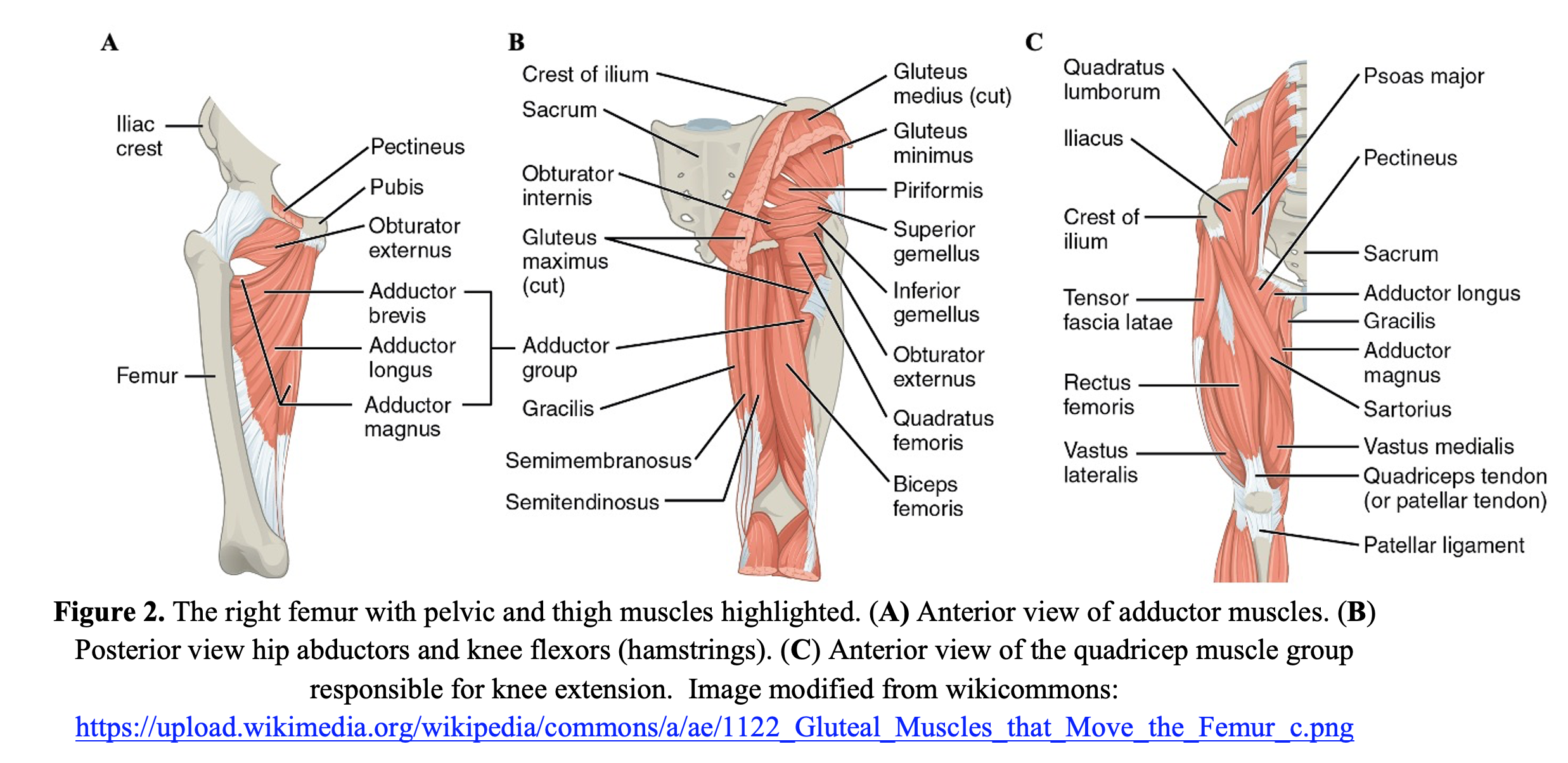
The proximal portion (proximal epiphysis and metaphysis) of the femur is inclusive of the femoral head and neck, which interact with the acetabulum of the pelvis to form the hip joint and the greater and lesser trochanters. The gluteus minimus and medius, piriformis, obturator internus, and vastus lateralis attach to the greater trochanter, while the psoas major and iliopsoas attach to the lesser trochanter (Figure 2B). The intertrochanteric line runs between the two trochanters serving as an attachment for the iliofemoral ligament and the anterior aspect of the hip joint capsule.
The shaft of the femur includes the gluteal tuberosity, which serves as the attachment site for the distal aspect of the gluteus maximus. The adductor muscle group attach to the posterior aspect of the shaft (Figure 2A).
Finally, the distal femur (distal epiphysis and metaphysis) includes the medial and lateral condyles, which articulate with the tibial plateau. The patella articulates with the anterior aspect of the distal femur and is also the insertion site (via the patellar ligament) for the quadricep muscle group: vastus lateralis, vastus magnus, and rectus femoris (Figure 2C). The intercondylar fossa includes the attachment points for the anterior cruciate and posterior cruciate ligaments, while the medial and lateral collateral ligaments attach the medial and lateral epicondyles, respectively.
Neurovascular Anatomy
The blood supply to the femur originates with the femoral artery—a continuation of the external iliac artery (Figure 3A). The proximal femur, including the femoral head and neck which are at highest risk for avascular necrosis, are predominantly supplied (90% of total volume) by branches off the medial circumflex femoral artery.1 Additional support is achieved through anastomoses with branches from the inferior gluteal artery. The deep femoral artery supplies blood to the femoral shaft. The distal femur is well vascularized, receiving its circulation from the popliteal artery, a continuation of the femoral artery, and its genicular branches.
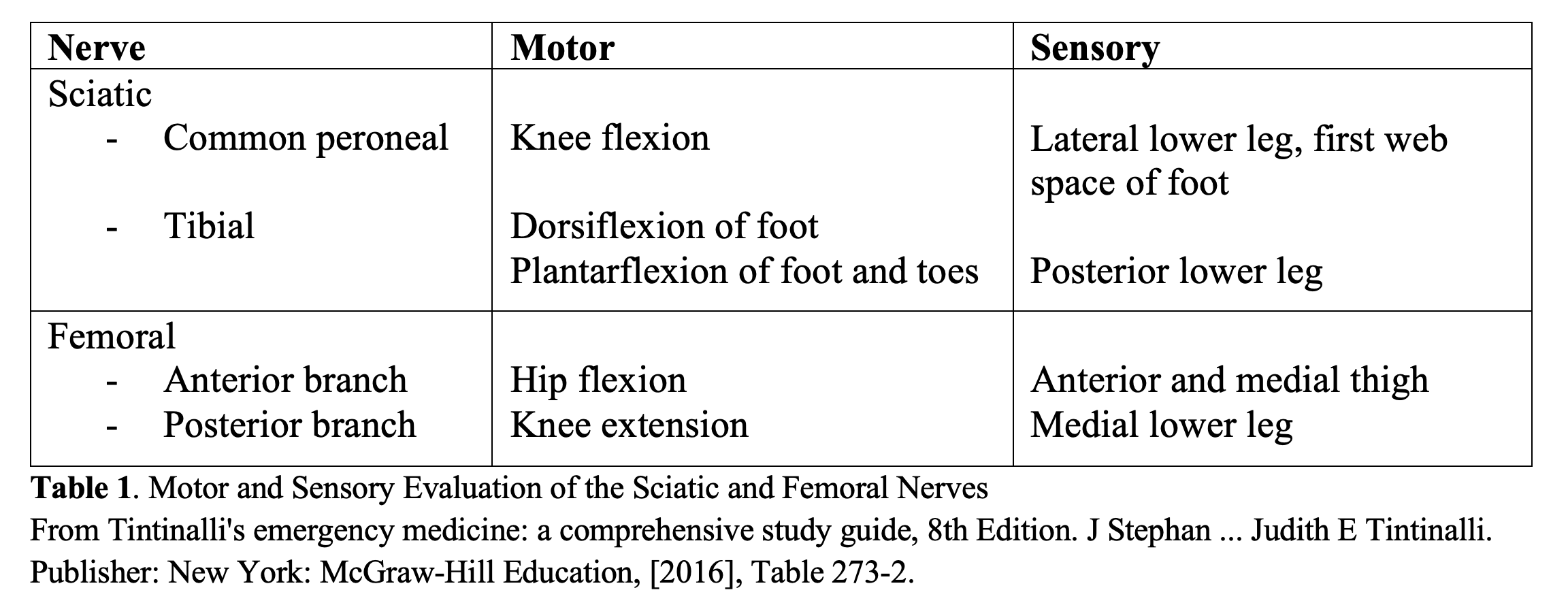
The sciatic nerve courses along the posterior aspect of the femur (Figure 3B). It innervates the muscles responsible for knee flexion, the hamstrings. It branches to form the tibial and popliteal nerves distally with the common peroneal (or common fibular) nerve branching off anterolaterally. These are respectively responsible for foot plantar and dorsi flexion along with sensation of the planter and dorsal aspects of the foot. The adductor muscles of the thigh are innervated by the obturator nerve and the quadriceps muscles responsible for knee extension and hip flexion are innervated by the femoral nerve.

General Approach to Femur Fractures
Exam
In any trauma patient, the primary and secondary exams are vital, but it is also critical to perform a thorough neurovascular exam on patients with a suspected femoral fracture to assess sensation, strength, and distal pulses. Additionally, look for any deformities and examine the hip and knee joints for stability. Expose the entire suspected fracture site to look for open wounds or abrasions that could indicate an open fracture. A baseline neurovascular examination, if available in the electronic medical record, can provide insight into possible pre-existing neurologic or vascular compromise. The neurologic exam is summarized in Table 1.
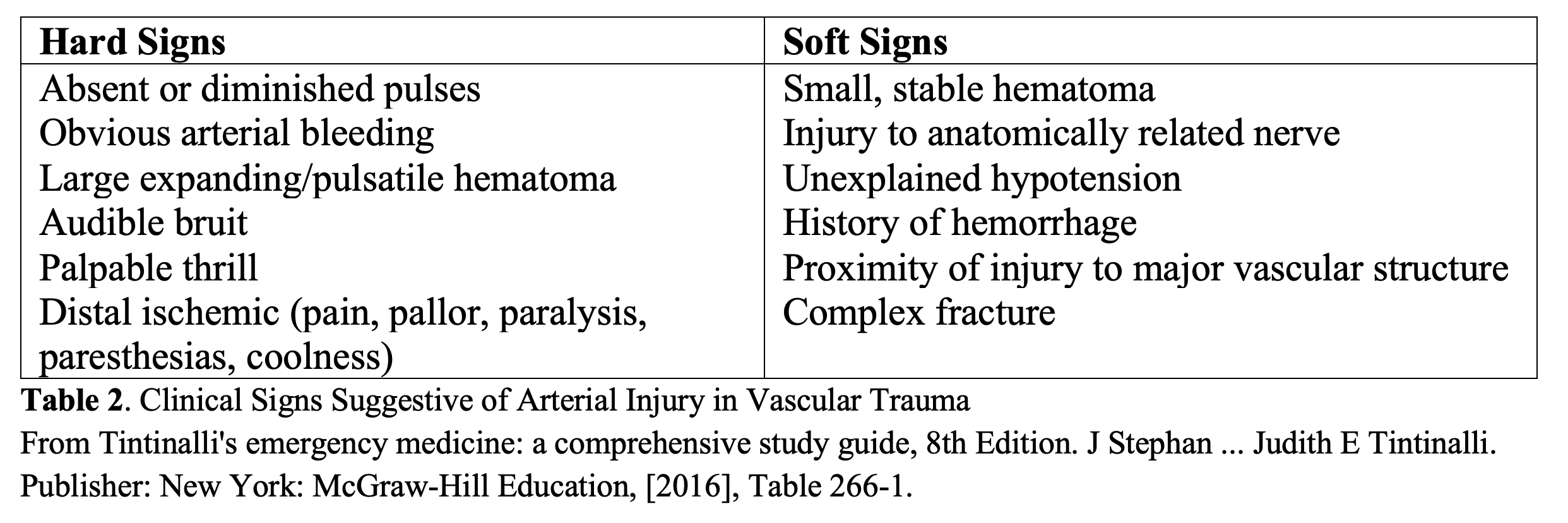
If weak pulses are present, determine the ankle brachial index (ABI) to aid in assessing possible arterial compromise. Ideally, position the patient supine for the ABI measurements and use a manual cuff to compare systolic blood pressures. A value below 0.9 suggests arterial damage with a specificity range of 83% to 99% and sensitivity of 69% to 79% when compared to angiography3. If there are hard signs of an arterial bleed (Table 2), you should acquire CT angiography instead of ABI measurements or go to the operating room if the patient is unstable.
Consider Nonaccidental Trauma
Abuse should be considered in both the elderly and pediatric populations when femur fractures are involved. One study suspected nonaccidental trauma in 31% of children less than 5 years old presenting with a femoral shaft fracture who were ultimately referred to child protective services.4 Be suspicious if the mechanism provided for the injury does not make sense or if there are multiple fractures, especially if they appear to have occurred at different times. Children less than 1 years of age do not have enough mobility to cause a femur fracture on their own. On imaging you can look for epiphyseal and metaphyseal bone avulsions that can result from twisting or pulling at the leg. Consider a full skeletal survey if the patient is less than 2 years of age. Refer to this EMDocs EM Cases to learn more about how to recognize physical abuse.
Imaging
X-rays should be obtained on all patient in whom femur fracture is suspected. An AP pelvic X-ray will likely be obtained if the injury is a result of a trauma. Additional images should be pursued according to clinical suspicion of injury location and should include dedicated AP, lateral and oblique femur views, ideally with the leg internally rotated. For suspected femoral shaft fractures, both the hip and knee joints should be included, obtaining dedicated images of these joints if not possible on a single film. Oblique pelvis views (also known as Judet views) are recommended if there is concern for an associated acetabular fracture. Femoral neck fractures may not be apparent on x-ray for several days and thus advanced imaging may be required for increased sensitivity.1
The prevalence of occult hip fractures not seen on an initial X-ray is likely between 2-8%.5 Higher rates of 39% and 92% are reported in a recent meta-analysis.6 The population was elderly with a mean pooled age of 78.6 years and the highest miss rate of 92% was seen in a population of patients with initial X-ray findings of non-emergent isolated greater trochanteric fractures that were found to have intertrochanteric extension on cross-sectional imaging.6 Thus, while plain radiographs should be the first line imaging modality, more advanced imaging should be pursued if clinical suspicion remains high, such as in elderly patients or when other fractures are seen. MRI is considered the gold standard; however, the literature has competing arguments for CT vs. MRI as the second line imaging modality as many institutions may not have access to MRI or the cost may be prohibitive. The American Association of Orthopedic Surgeons (AAOS) recommends MRI as the second-line test if available within 24 hours, with CT or nuclear medicine bone scan as third-line.7
The data preferring MRI over CT is summarized by a meta-analysis by Kellock et al and in a review by Foex et al with only three available studies that directly compare CT to MRI, with MRI changing diagnoses 61% (27/44 patients), 22% (15/67 patients), and 66% (4/6 patients) of the time.8–12 The available studies are limited by only one being a prospective study, small sample sizes, and very few discrepancies resulting in a change in management. Reports of CT sensitivity for detection of occult proximal femur fractures have varied with Kellock et al stating a sensitivity of 94% while more recently Haj-Mirzaian et al reports a sensitivity of 79%.6,10 Overall, it is reasonable to obtain a CT to assess for occult fracture after negative X-rays, but the policy will vary by institution, with some institutions deciding it may be more cost effective to directly transfer patients to receive definitive MRI imaging in lieu of available CT imaging.13 For more discussion on the approach to diagnosing occult fractures please refer to this EMDocs post.
Management
Stabilize and Resuscitate
Systematically perform the primary and secondary exams to evaluate and stabilize trauma patients.
- If severe bleeding is present, the top priority is to prevent exacerbation of the “lethal triad”: coagulopathy; acidosis; and hypothermia. Control any external bleeding and administer tranexamic acid (TXA) within 3 hours of injury.14,15
- While resuscitation is important, avoid over resuscitation with crystalloid as this can increase the risk of hypothermia and coagulopathy.15
- Consider using the TASH score, which is an externally validated decision-making tool to predict the need for a massive transfusion protocol (MTP). Its calculations include the presence of an open or dislocated femur fracture which has an odds ratio of 2.8 for increased likelihood of requiring a massive transfusion.16 Other tools, such as the ABC Score and the Shock Index, can be used to predict the need for MTP although they do not take femur fractures into account.
Other Interventions
- Patients should be non-weight bearing once a femur fracture is identified.
- Administer antibiotics and a tetanus booster for open fractures. Remove any gross debris to further reduce the risk of infection.
- Pain control
- A fascia iliaca or femoral nerve block can be performed on stable patients which have lower side effects than systemic opioids.17 The fascia iliaca block is thoroughly described in this ACEP Now article.
- If the fracture is a result of a fall the work-up should include non-mechanical causes of falls such as neurologic or cardiac syncope if the cause is not entirely certain.
Proximal Fractures
Background
Also known as hip fractures, these are characterized further by anatomic location: head, neck, and greater and lesser trochanters (see Figure 1). These fractures are also referred to as intracapsular or extracapsular in reference to the joint capsule. The trochanters are outside of the joint space and thus fractures in this location are considered extracapsular. Age is an independent risk factor for femur fractures with proximal fractures being the most common in the elderly population. Therefore, it is important to be suspicious of this injury in these patients.18 These fractures are discussed below but you may also refer to the EM@3AM Proximal Femur Fractures post for a bullet point review.
Femoral Head Fractures
This is the least likely site of fracture, theorized to result from being relatively protected within the hip joint. It is most commonly seen in the younger population associated with high impact traumas and less likely to be caused by a fall.18
Femoral Neck Fractures
These are most common in the elderly population with increased prevalence in elderly females likely due to decreased bone density. Compared to non-falls, fall injuries were 93% more likely to have a neck fracture than femur fractures at other sites.18 Femoral neck fractures can disrupt the medial femoral circumflex artery from supplying blood to the femoral head causing avascular necrosis which is seen more frequently in displaced fractures. These fractures can be further complicated by hip dislocation. For patients age 65 and older, there is a 6% inpatient mortality rate and 1-year mortality rate between 20-30% with the highest risk within the first 6 months.2
Trochanteric Fractures
These fractures are more common in falls as the impact force is directed to the posterolateral greater trochanter. This is the same injury mechanism for femoral neck fractures from falls, but trochanteric fractures are outside of the joint capsule with better vascularization, making them less prone to osteonecrosis. Female sex has been reported as an independent risk factor for trochanteric fractures.18
Management of Proximal Fractures
Should You Use Traction?
- A 2011 Cochrane review found no evidence to support traction devices for proximal femur (hip) fractures.19
- The AAOS also does not recommend the use of traction devices for preoperative management of hip fractures.7
Definitive Surgical Management
According to the AAOS 2018 guidelines, moderate evidence suggests better outcomes with proximal femur (hip) fracture surgery within 48 hours of admission for patients aged 65 years or greater.20 Thus, early surgical consultation is paramount, with significant increased 30-day mortality seen after 24 hours of surgical delay for femoral neck fractures.21 The AAOS consensus statement and guideline outlines 30 various scenarios for the type of surgery indicated. In general, patients are more likely to require surgery with displaced fractures as they are considered unstable, favoring preservation of native femoral head for the younger population while considering total hip arthroplasty for the elderly especially if they have pre-existing arthritis. If conservative management is recommended, patients will be non-weight bearing for at least a month.20,22
Complications of Proximal Fractures
Avascular Necrosis (AVN)
Also known as osteonecrosis, AVN is associated with proximal femur fractures, particularly neck fractures because these more commonly disrupt vasculature (Figure 3A). An additional proposed mechanism in fractures with joint capsule integrity is edema in the joint capsule leading to a tamponade effect on the vascular supply. AVN occurs in 6-30% of femoral neck fractures, with increased prevalence seen in displaced fractures.23 Restoration of the patient’s anatomy, often requiring operative reduction, is associated most strongly with preventing AVN and should be performed as soon as possible.23 Patients who develop AVN will present most commonly with groin pain that radiates to the hip and buttock that is worse on internal rotation of the hip.24 Patients with prior femoral neck fractures who have undergone internal fixation can still develop AVN with a median time of presentation of 1.4 years after surgery in one study.25 The diagnosis can be confirmed with MRI (90-100% sensitivity) after excluding other causes.23,25 AVN is then managed non-operatively if possible, but 80% of symptomatic patients will need a total hip replacement after 2 years.26
Hip Dislocation
The hip is the most stable joint and the hardest to dislocate, thus dislocations require high energy forces that may also result in fracture(s).27 Posterior hip dislocations occur in motor vehicle accidents when the flexed knee hits the dashboard with the hip flexed and adducted, which can be prevented with the use of a seat belt.28 Anterior dislocations are overall less common at about 10% of all traumatic hip dislocations and are associated with falls.28
Head and neck femur fractures are often implicated when a hip dislocation occurs and attempted closed reduction can cause fracture displacement. Thus, when associated with these fractures, open hip reductions in the operating room may be preferable although this remains controversial as discussed in this EMDocs Medical Malpractice Insights Case. A retrospective review in 2019 showed a 73% (16/22 patients) success rate with ED closed reduction of hip dislocations with isolated femoral head fractures, however most patients still required later operative repair.29 Reduction, whether closed or open, should ideally occur within 6 hours to reduce the risk of future AVN; and ensure you perform post-reduction imaging to confirm placement.28
Shaft Fractures
Background
Also known as diaphyseal fractures, shaft fractures most commonly occur during motor vehicle accidents in younger patients with one study finding the average age to be 44 years old compared to an average age of 75 for femur fractures in other locations.18 However, elderly patients who are obese may fit outside this dogma. Obese patients are more likely to sustain shaft fractures from falls compared to patients with lower BMIs likely because of increased fat padding at the hip that protects from proximal fractures while increased weight corresponds to increased fall force that puts the shaft at risk.2 The distribution of fracture is equal between male and female sex. Deformities associated with shaft fractures can be more severe than at other locations and thus vascular damage can be more common, with injury to the femoral artery occurring in 2% of individuals.1
Management of Shaft Fractures
Should You Use Traction?
- Yes! Immobilize shaft fractures. This reduces pain, further surgical interventions, blood transfusions, and hospital length of stay.30
- There are multiple methods: skin traction with devices such as Hare and Sager; skeletal traction with a distal pin; external fixation; and intramedullary nailing, which is the definitive management which should occur within 24 hours.31
- EMS commonly uses skin traction to reduce femur fractures if neurovascular compromise is noted. These devices, when compared to skeletal traction, can be applied more quickly and have similar outcomes.32 Keep in mind these devices may worsen unrecognized injuries or fractures such as hip dislocation, knee fracture or dislocation, and ankle injury which are all absolute contraindications for skin traction.
- In a polytrauma patient, a femoral or tibial skeletal traction pin performed by an orthopedic surgeon is preferred as a damage control measure while awaiting definitive therapy. This can be performed in minutes at the bedside.33
Definitive Surgical Management
Fractures of the femoral shaft in the adult population and in developed countries are treated surgically with intramedullary nailing as the gold standard therapy. This should occur within 24-48 hours. External fixation, if used, is generally a temporary therapy as patients await definitive management. Traction, as discussed above, is important initially but has limited control of the bone alignment and long term has increased risk of deep vein thrombosis and joint stiffness.1
Complications of Shaft Fractures
Hemorrhage
The thigh is estimated to hold 1.5 L of blood. Thus, the classic teaching is that vascular injuries associated with femoral shaft fractures can cause hemorrhagic shock. The deformities associated with shaft fractures are more severe when compared to proximal and distal femur fractures and are the proposed explanation for why shaft fractures are historically associated with higher rates of hemorrhage.31 This is supported by a 1992 study by Lieurance et al that showed an average of 2.5 units of packed red blood cells were required for isolated femur fractures with an average blood loss of 1.2 liters.34 However, a more recent study in 2018 by Wertheimer et al showed transfusions were required in 36% of femoral shaft fractures (median of 2 units) with a mean time of administration of 30.5 hours and occurring post-operatively.35Therefore, alternative causes of shock should be sought during initial resuscitation of a hypotensive polytrauma patient who also happens to have a femoral shaft fracture.
Nerve Injury
Femoral shaft fractures put the sciatic nerve, responsible for knee flexion (Figure 3), at risk of injury. However, sciatic nerve injury is extremely rare occurring in only 0.4% of femoral shaft fractures and most commonly resolves spontaneously.36 The low incidence of sciatic injury is likely due to the protective surrounding musculature (Figures 2, 3B, 4), but when it does present it manifests with weakness of knee flexion and lateral calf numbness (Table 1).36Magnetic resonance neurography should be pursued non-emergently as a diagnostic study and surgical exploration may be required if sciatic nerve palsy persists beyond five months36
Open Fractures and Infection
An open fracture is defined as any break in the skin at the site of fracture. Open femur fractures make up 9–23% of all traumatic femur fractures and are relatively rare compared to open fractures at other anatomic locations with the finger phalanges, tibia, and distal radius being the most common sites of open fractures.37,38 Femoral open fractures most frequently occur at the shaft although they can occur at any location.39,40
According to one population study by Weber et al in 2016, open femur fractures are associated with a higher mortality despite receiving more aggressive resuscitation; the patients requiring massive transfusion are at the greatest risk for sepsis.37 Open fractures are described and classified using the Gustilo Classification system, as summarized in Table 3.41 This system and the general approach for all open fractures is discussed on EMDocs EM@3AM Open Fractures post.
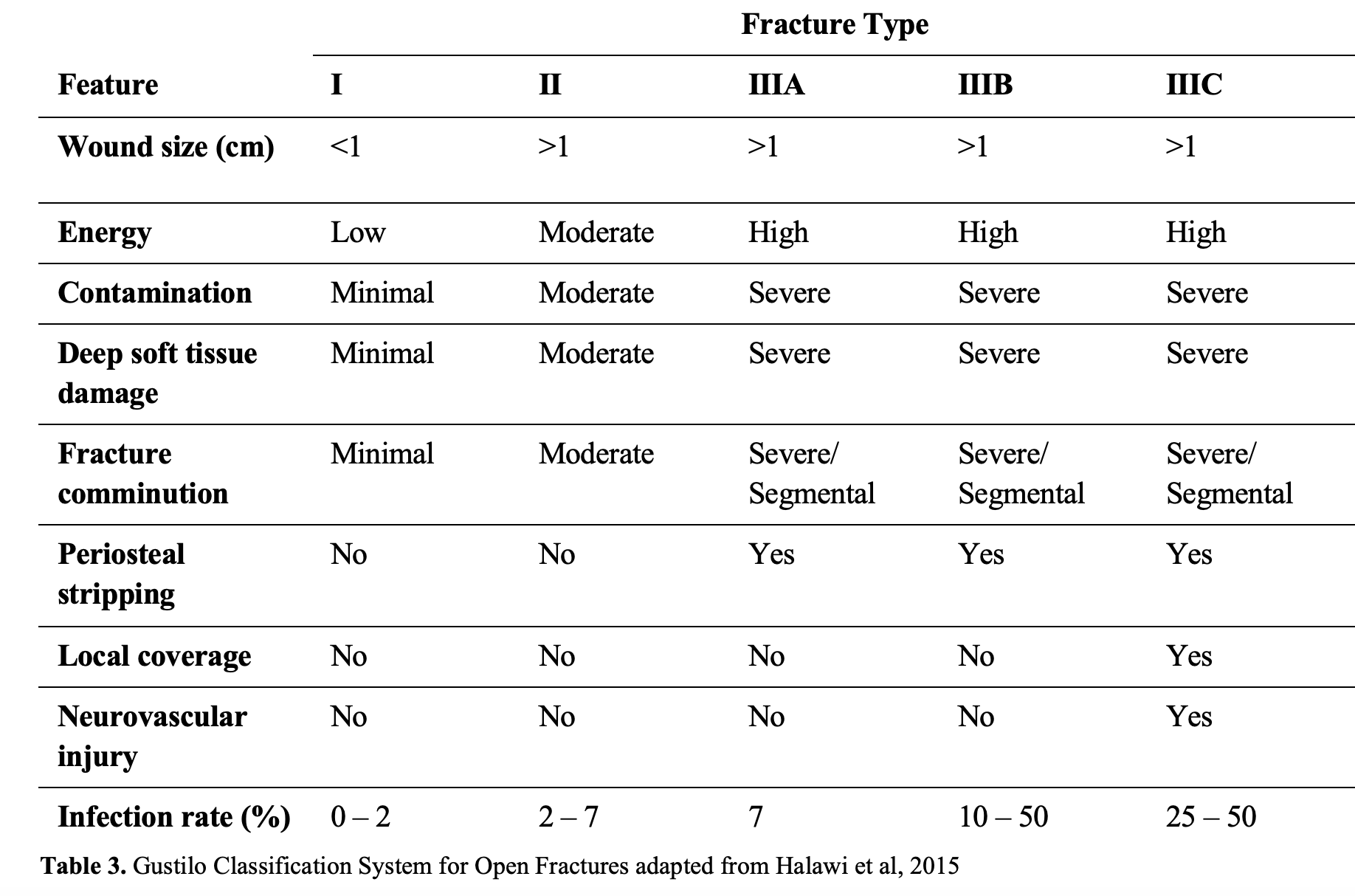
A 2004 Cochrane review showed prophylactic antibiotics to have a relative risk reduction of 43% at preventing subsequent infection of open fractures.42 A first-generation cephalosporin, usually Cefazolin at 100mg/kg with a maximum of 2g/dose every 8 hours, should be administered as soon as possible for 24 hours. If the wound is classified as Gustilo III (see Table 3), a fourth-generation cephalosporin should be used to provide Pseudomonas aeruginosa coverage in these high-risk patients (Gustilo III femur fractures are associated with at least a 17% mortality).37 Tetanus status should also be determined if possible and vaccination should be administered if the patient is not up to date, has not had a booster within 5 years for a severely contaminated wound, or has an unknown status. Place saline soaked gauze over exposed bone and the wound until formal irrigation can be performed in the operating room. The most important step to prevent infection is urgent surgical irrigation and debridement to remove all nonviable tissue.41
Compartment Syndrome
Compartment syndrome is the build-up of pressure inside the muscles caused by bleeding or edema that is confined by the muscle fascia. Acute compartment syndrome is a medical emergency that can cut off vascular supply to the surrounding tissue. This is a rare complication of femur fractures—it is more commonly seen in tibial fractures. In one retrospective study of 28 patients with compartment syndrome of the thigh, 13 (46%) were the result of a femur fracture, with 11 from motor vehicle accidents and 2 from falls.43 The anterior compartment was involved in all patients (Figure 4). Pulselessness and myonecrosis were more commonly seen in patients with femur fractures compared to those without fractures, thus it is important to relieve the pressure as soon as possible. This study did not correlate the incidence with location of femur fracture, but it is likely more common in shaft fractures due to the increased propensity of displacement and subsequent tissue disruption.31,43
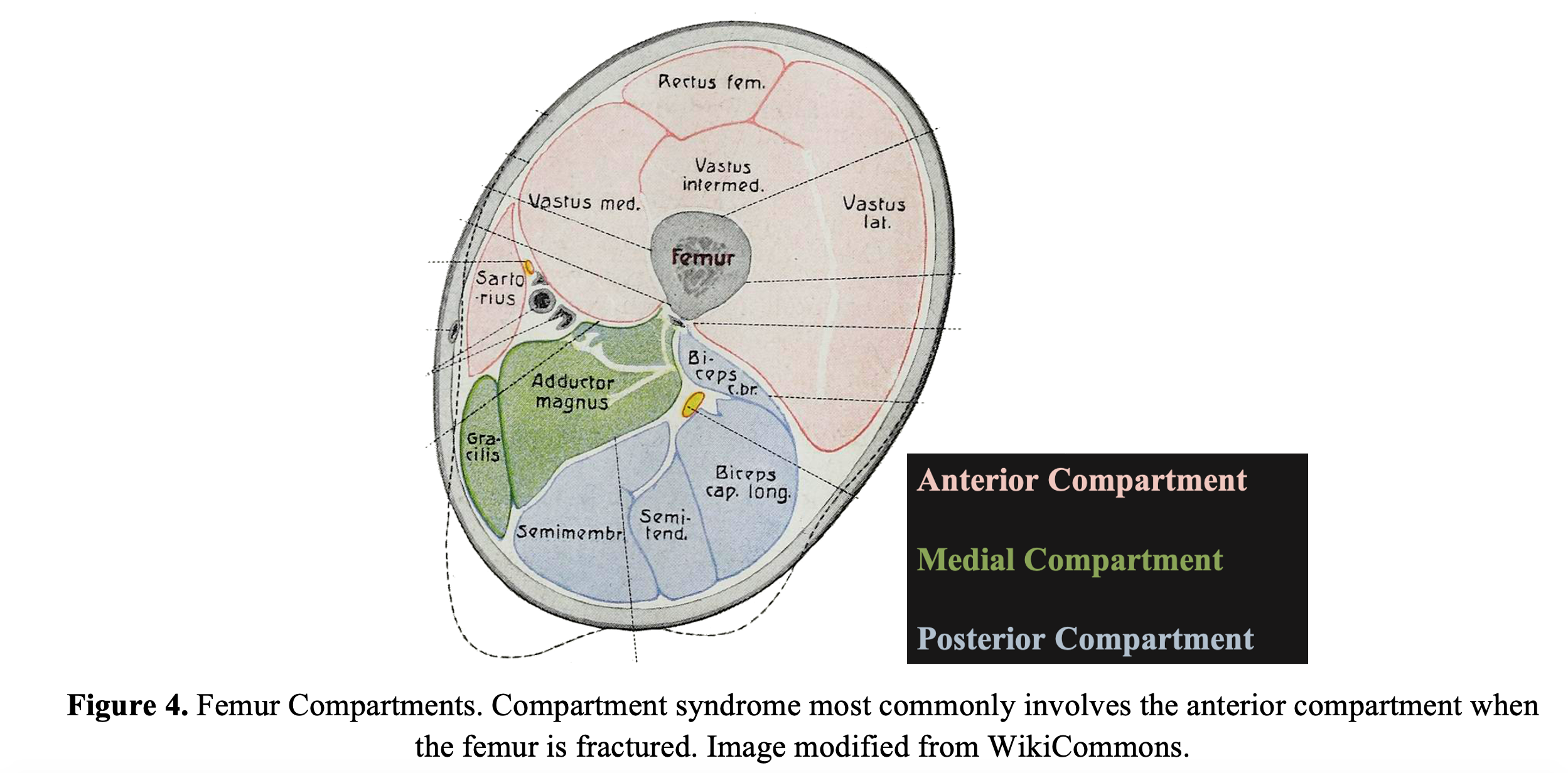
Because they are associated with high energy mechanisms, open fractures are strongly associated with compartment syndrome, and increased incidence is directly associated with higher Gustilo Classifications (Table 3).41 In a 2010 systematic review of 89 cases of thigh compartment syndrome, 49% were associated with femur fractures, of which 22% were open.44 Refer to the EMDocs Compartment Syndrome post for a full review on this complication including diagnosis and management.
Fat Embolism
Fat embolism is the presence of fat globules in the systemic circulation. Potential clinically significant effects may include the classic triad of respiratory distress, neurologic changes, and petechial rash that define fat embolism syndrome (FES). FES is associated most strongly with trauma with an incidence of 0.17% of all fractures; however, the incidence is higher for isolated femur fractures and femur fractures presenting with additional fractures at other locations, with incidences of 0.54% and 1.29%, respectively.45,46 This syndrome most commonly presents 24-72hrs after the associated trauma, so it may not be as relevant in the initial resuscitation phase but should be considered if the patient has a prolonged ED stay due to delayed transfer or admission. This is a clinical diagnosis and treatment is predominately supportive, however the risk is decreased if femoral fracture surgical repair is performed within 24 hours. For a full review on this complication please refer to EMDocs Fat Embolism of Long Bones.
Distal Fractures
Background
Distal femur fractures, also known as supracondylar fractures, make up less than 1% of all orthopedic injuries and compromise 3-6% of all femur fractures.47 These fractures occur most commonly from high impact trauma such as motor vehicle accidents, but they may also occur due to falls in high-risk patients such as the elderly. Patients with distal femur fractures with a median age of 86 years face mortality rates of 29% after 3 months and 35% after 1 year.48 Anatomic considerations include the various muscle groups that span this location, most importantly the quadriceps, adductors, and the gastrocnemius which can cause shortening, varus/valgus, and posterior deformities, respectively, as the muscles pull on loose bone (Figure 2).
Management of Distal Fractures
The goal of therapy for distal femur fractures is to restore the distal articular surface to the femoral shaft while maintaining the proper anatomic alignment. Most repairs are operative, and emergency providers should consult surgical colleagues early as most of these patients will require admission. In the meantime, the femur should be immobilized in a long leg splint.
Orthopedic surgeons may manage nondisplaced fractures conservatively with splinting or casting and non-weight bearing status for 4-6 weeks.49 All fractures involving the articular surface will require surgical repair as healing is often most complicated in the relatively poorly perfused distal shaft compared to periarticular fractures.49 External fixation is often pursued as a damage control measure or definitive therapy if there is serious soft tissue injury, comminuted fractures, or the patient cannot undergo surgery.
Complications of Distal Fractures
Popliteal Artery Injury
When there is displacement of the femur from the knee joint there is a risk of vessel and nerve injury, including popliteal artery injury (Figure 3). Injury to the popliteal artery from extremity trauma is rare (0.2–1%), but amputation rates are high (10–16%).50 This injury is more commonly associated with knee dislocations (see EMDocs post on knee dislocations); however, case series have found that 17% – 24% (4/24 and 17/70 patients) of traumatic popliteal artery injuries were due to distal femur fractures.50,51
Examine the popliteal space in these patients and palpate both the dorsalis pedis and posterior tibial pulses, keeping hard and soft signs of arterial injury in mind (Table 2), pursuing surgical evaluation or CT angiography as indicated, respectively. If possible, assess for foot drop that would indicate a concomitant nerve injury (Table 1). Open vascular repair is generally used over endovascular repair in these patients and there is little evidence on whether or not to pursue bony stabilization prior to vascular repair and therefore the preferred sequence will vary by surgeon.50 Either way, the vascular repair should be performed within 6 hours to reduce the risk of future amputation.51
Case resolution
The patient had stable vital signs and an unremarkable exam (no deformities, no neurovascular deficits) except for his inability to bear weight. His initial x-rays were read as negative (Figure 5A); however, CT imaging was pursued due to a high level of suspicion in this elderly patient with persistent pain that showed a greater trochanteric fracture (Figure 5B). Pre-op labs were drawn, and the patient was made non-weightbearing and admitted to the orthopedic service. Prior to admission, a fascia iliaca block was performed by the ED providers to avoid opioid use. An MRI was performed while inpatient for surgical planning purposes, which found an intertrochanteric fracture with edema extending to the lateral femoral neck (Figure 5C). The fracture was repaired with internal fixation via a sliding hip screw the next day to prevent fracture spread and possible displacement. The patient made an excellent recovery.

Key points
- Mechanisms suggest the location of the fracture
- Fall – high suspicion in the elderly for neck or trochanteric fractures; be concerned for hip dislocation/bone displacement and reduce within 6 hours to decrease the risk of AVN.
- Motor vehicle or other high impact injury – think head, shaft, and distal fractures; more likely to require resuscitation.
- Get cross-sectional imaging if concern for fracture persists after negative X-ray. MRI is preferred, but CT is an acceptable alternative if MRI is not available in a timely manner.
- Early surgical intervention – ideally within 24-48 hours – improves long-term outcomes, reducing risk of AVN and FES.
- Do not use traction devices for proximal femur fractures.
- Do not anchor on a femur fracture as the cause for hemorrhagic shock in trauma patients – look for other causes! Administer TXA within 3 hours and control localized bleeding (in conjunction with ortho colleagues, if possible) with traction for shaft
- Provide prophylactic antibiotics and tetanus to those with open
References
- Reynolds, A. The fractured femur. Radiologic Technology 84, 273–91; quiz p.292-4 (2013).
- Brauer, C. A., Coca-Perraillon, M., Cutler, D. M. & Rosen, A. B. Incidence and Mortality of Hip Fractures in the United States. Jama 302, 1573 (2009).
- Ko, S. H. & Bandyk, D. F. Interpretation and significance of ankle-brachial systolic pressure index. Semin Vasc Surg26, 86–94 (2013).
- Shrader, M. W., Bernat, N. M. & Segal, L. S. Suspected nonaccidental trauma and femoral shaft fractures in children. Orthopedics 34, 360 (2011).
- Deleanu, B. et al. Occult fractures of the proximal femur: imaging diagnosis and management of 82 cases in a regional trauma center. World J Emerg Surg 10, 55 (2015).
- Haj-Mirzaian, A. et al. Use of Advanced Imaging for Radiographically Occult Hip Fracture in Elderly Patients: A Systematic Review and Meta-Analysis. Radiology 296, 521–531 (2020).
- Roberts, K. C., Brox, W. T., Jevsevar, D. S. & Sevarino, K. Management of Hip Fractures in the Elderly. J Am Acad Orthop Sur 23, 131–137 (2015).
- Foex, B. A. & Russell, A. BET 2: CT versus MRI for occult hip fractures. Emerg Med J 35, 645–647 (2018).
- Collin, D., Geijer, M. & Göthlin, J. H. Computed tomography compared to magnetic resonance imaging in occult or suspect hip fractures. A retrospective study in 44 patients. Eur Radiol 26, 3932–3938 (2016).
- Kellock, T. T., Khurana, B. & Mandell, J. C. Diagnostic Performance of CT for Occult Proximal Femoral Fractures: A Systematic Review and Meta-Analysis. Ajr Am J Roentgenol 213, 1324–1330 (2019).
- Lubovsky, O., Liebergall, M., Mattan, Y., Weil, Y. & Mosheiff, R. Early diagnosis of occult hip fractures. Inj 36, 788–792 (2005).
- Haubro, M., Stougaard, C., Torfing, T. & Overgaard, S. Sensitivity and specificity of CT- and MRI-scanning in evaluation of occult fracture of the proximal femur. Inj 46, 1557–1561 (2015).
- Yun, B. J. et al. Diagnostic Imaging Strategies for Occult Hip Fractures: A Decision and Cost–Effectiveness Analysis. Acad Emerg Med 23, 1161–1169 (2016).
- collaborators, C.-2 et al. The importance of early treatment with tranexamic acid in bleeding trauma patients: an exploratory analysis of the CRASH-2 randomised controlled trial. Lancet 377, 1096-1101.e2 (2011).
- Stewart, R., Rotondo, M. F., Henry, S. M. & Drago, M. Advanced Trauma Life Support (ATLS). (American College of Surgeons Committee on Trauma, 2018).
- Yücel, N. et al. Trauma Associated Severe Hemorrhage (TASH)-Score: Probability of Mass Transfusion as Surrogate for Life Threatening Hemorrhage after Multiple Trauma. J Trauma Inj Infect Critical Care 60, 1228–1237 (2006).
- Nagel, E. M., Gantioque, R. & Taira, T. Utilizing Ultrasound-Guided Femoral Nerve Blocks and Fascia Iliaca Compartment Blocks for Proximal Femur Fractures in the Emergency Department. Adv Emerg Nurs J 41, 135–144 (2019).
- Wu, S.-C., Rau, C.-S., Kuo, S. C. H., Chien, P.-C. & Hsieh, C.-H. The influence of ageing on the incidence and site of trauma femoral fractures: a cross-sectional analysis. Bmc Musculoskelet Di 20, 413 (2019).
- Handoll, H. H., Queally, J. M. & Parker, M. J. Pre-operative traction for hip fractures in adults. Cochrane Db Syst RevCD000168 (2011) doi:10.1002/14651858.cd000168.pub3.
- Brox, T. et al. Management of Hip Fractures in The Elderly: Timing of Surgical Intervention. (2018).
- Morrissey, N., Iliopoulos, E., Osmani, A. W. & Newman, K. Neck of femur fractures in the elderly: Does every hour to surgery count? Inj 48, 1155–1158 (2017).
- Directors, A. A. of O. S. B. of. APPROPRIATE USE CRITERIA FOR THE ACUTE TREATMENT OF HIP FRACTURES IN THE ELDERLY. (2015).
- Ehlinger, M. et al. Early prediction of femoral head avascular necrosis following neck fracture. Orthop Traumatology Surg Res Otsr 97, 79–88 (2010).
- Cohen-Rosenblum, A. & Cui, Q. Osteonecrosis of the Femoral Head. Orthop Clin N Am 50, 139–149 (2019).
- Wang, Y. et al. Correlation Between Reduction Quality of Femoral Neck Fracture and Femoral Head Necrosis Based on Biomechanics. Orthop Surg 11, 318–324 (2019).
- Lespasio, M. J., Sodhi, N. & Mont, M. A. Osteonecrosis of the Hip: A Primer. Perm J 23, (2019).
- Schlickewei, W., Elsässer, B., Mullaji, A. B. & Kuner, E. H. Hip dislocation without fracture: traction or mobilization after reduction? Inj 24, 27–31 (1993).
- Sahin, V. et al. Traumatic Dislocation and Fracture-Dislocation of the Hip: A Long-Term Follow-Up Study. J Trauma Inj Infect Critical Care 54, 520–529 (2003).
- Core, M. A. D., Gross, B., Ahn, J., Wallace, S. B. & Starr, A. Clinical and Radiographic Outcomes of Femoral Head Fractures Associated with Traumatic Hip Dislocations. Strategies Trauma Limb Reconstr 14, 6–10 (2019).
- Guerado, E., Bertrand, M. L., Cano, J. R., Cerván, A. M. & Galán, A. Damage control orthopaedics: State of the art. World J Orthop 10, 1–13 (2019).
- Denisiuk, M. & Afsari, A. Femoral Shaft Fractures – StatPearls – NCBI Bookshelf. undefinedhttps://www.ncbi.nlm.nih.gov/books/NBK556057/ (2020).
- Even, J. L. et al. Preoperative Skeletal Versus Cutaneous Traction for Femoral Shaft Fractures Treated Within 24 Hours. J Orthop Trauma 26, e177–e182 (2012).
- Scannell, B. P., Waldrop, N. E., Sasser, H. C., Sing, R. F. & Bosse, M. J. Skeletal traction versus external fixation in the initial temporization of femoral shaft fractures in severely injured patients. J Trauma 68, 633–40 (2010).
- Lieurance, R., Benjamin, J. B. & Rappaport, W. D. Blood Loss and Transfusion in Patients with Isolated Femur Fractures. J Orthop Trauma 6, 175–179 (1992).
- Wertheimer, A., Olaussen, A., Perera, S., Liew, S. & Mitra, B. Fractures of the femur and blood transfusions. Inj 49, 846–851 (2018).
- Emamhadi, M., Saberi, A. & Andalib, S. Sciatic nerve injuries following femoral shaft fractures: Does the time interval from injury to surgery matter? Clin Neurol Neurosurg 147, 6–10 (2016).
- Weber, C. D. et al. Classification of soft-tissue injuries in open femur fractures: Relevant for systemic complications? J Trauma Acute Care 81, 824–833 (2016).
- Enninghorst, N., McDougall, D., Evans, J. A., Sisak, K. & Balogh, Z. J. Population-based epidemiology of femur shaft fractures. J Trauma Acute Care 74, 1516–1520 (2013).
- Kovar, F. M., Jaindl, M., Schuster, R., Endler, G. & Platzer, P. Incidence and analysis of open fractures of the midshaft and distal femur. Wien Klin Wochenschr 125, 396–401 (2013).
- Winkler, D., Goudie, S. T. & Court-Brown, C. M. The changing epidemiology of open fractures in vehicle occupants, pedestrians, motorcyclists and cyclists. Inj 49, 208–212 (2017).
- Halawi, M. J. & Morwood, M. P. Acute Management of Open Fractures: An Evidence-Based Review. Orthopedics 38, e1025–e1033 (2015).
- Gosselin, R. A., Roberts, I. & Gillespie, W. J. Antibiotics for preventing infection in open limb fractures. Cochrane Db Syst Rev CD003764 (2004) doi:10.1002/14651858.cd003764.pub2.
- Mithöfer, K., Lhowe, D. W., Vrahas, M. S., Altman, D. T. & Altman, G. T. Clinical Spectrum of Acute Compartment Syndrome of the Thigh and Its Relation to Associated Injuries. Clin Orthop Relat R 425, 223–229 (2004).
- Ojike, N. I., Roberts, C. S. & Giannoudis, P. V. Compartment syndrome of the thigh: A systematic review. Inj 41, 133–136 (2010).
- STEIN, P. D., YAEKOUB, A. Y., MATTA, F. & KLEEREKOPER, M. Fat Embolism Syndrome. Am J Medical Sci336, 472–477 (2008).
- Rothberg, D. L. & Makarewich, C. A. Fat Embolism and Fat Embolism Syndrome. J Am Acad Orthop Sur 27, e346–e355 (2019).
- Gwathmey, W. F., Jones-Quaidoo, S. M., Kahler, D., Hurwitz, S. & Cui, Q. Distal Femoral Fractures: Current Concepts. Am Acad Orthop Surg 18, 597–607 (2010).
- Loosen, A., Fritz, Y. & Dietrich, M. Surgical Treatment of Distal Femur Fractures in Geriatric Patients. Geriatric Orthop Surg Rehabilitation 10, 215145931986072 (2019).
- Gangavalli, A. K. & Nwachuku, C. O. Management of Distal Femur Fractures in Adults. Orthop Clin N Am 47, 85–96 (2016).
- Fairhurst, P. G. et al. Popliteal vessel trauma: Surgical approaches and the vessel-first strategy. Knee 25, 849–855 (2018).
- Dua, A. et al. Outcome predictors of limb salvage in traumatic popliteal artery injury. Ann Vasc Surg 28, 108–14 (2014).






1 thought on “An Overview of Femur Fractures: Location, Imaging, Complications, and Management”
A succinct and well presented summary of femoral fracture management in the ED. This will definitely improve my approach to taking care of patients with the different types of femoral fractures.
Thank you.