Author: Lloyd Tannenbaum, MD (Emergency Medicine Resident, San Antonio, TX) // Edited by: Jamie Santistevan, MD (@jamie_rae_EMdoc – EM Physician, Presbyterian Hospital, Albuquerque, NM); Manpreet Singh, MD (@MPrizzleER – Assistant Professor of Emergency Medicine / Department of Emergency Medicine – Harbor-UCLA Medical Center); and Brit Long, MD (@long_brit – EM Attending Physician, San Antonio, TX)
Welcome to this edition of ECG Pointers, an emDOCs series designed to give you high yield tips about ECGs to keep your interpretation skills sharp. For a deeper dive on ECGs, we will include links to other great ECG FOAMed!
This week, we have part one of a several part series on concerning ECG findings in patients presenting with syncope.
Before getting started with our ECG and case, let’s define a few terms. The definitions below are taken from the 2017 ACC/AHA/HRS Guidelines for the Evaluation and Management of Patients Presenting with Syncope, a document which has been endorsed by ACEP as guidelines for clinical practice.
Syncope: A symptom that presents with an abrupt, transient, complete loss of consciousness, associated with inability to maintain postural tone, with rapid and spontaneous recovery [1].
Presyncope (also called Near Syncope): The symptoms before syncope. These symptoms could include extreme lightheadedness; visual sensations, such as “tunnel vision” or “graying out”; and variable degrees of altered consciousness without complete loss of consciousness. Presyncope could progress to syncope, or it could abort without syncope [1].
Unexplained syncope (syncope of undetermined etiology): Syncope for which a cause is undetermined after an initial evaluation that is deemed appropriate by the experienced healthcare provider. The initial evaluation includes but is not limited to a thorough history, physical examination, and ECG [1].
Vasovagal Syncope (VVS): The most common form of reflex syncope mediated by the vasovagal reflex. VVS 1) may occur with upright posture (standing or seated or with exposure to emotional stress, pain, or medical settings; 2) typically is characterized by diaphoresis, warmth, nausea, and pallor; 3) is associated with vasodepressor hypotension and/or inappropriate bradycardia; and 4) is often followed by fatigue. Typical features may be absent in older patients (24). VVS is often preceded by identifiable triggers and/or by a characteristic prodrome. The diagnosis is made primarily on the basis of a thorough history, physical examination, and eyewitness observation, if available [1].
Cardiac Syncope: Syncope caused by bradycardia, tachycardia, or hypotension due to low cardiac index, blood flow obstruction, vasodilatation, or acute vascular dissection [1].
Per these guidelines, it is a class one recommendation (the strongest offered) that all patients who present with syncope have a detailed history and physical exam performed. The physical exam should include orthostatic vital signs and a basic neurologic exam looking for any deficits. Obtaining an ECG is also a class one recommendation. This series will talk about what to screen an ECG for to catch cardiac causes of syncope. In my residency program, we were taught the mnemonic: I get my Dairy Queen At HEB [2]. (For those of you tragically not from Texas, HEB is our local grocery store). This stands for:
D: Delta wave (Wolff-Parkinson-White)
Q: QT Prolongation
A: AV nodal blocks
H: HOCM (look for dagger Q waves)
E: Epsilon wave (Arrhymogenic Right Ventricular Dysplasia)
B: Brugada pattern
Over the course of this series, we will explore each of these conditions we screen for to better understand what we are looking for and why they cause syncope.
Case 1:
As a military emergency physician, I think I see more healthy 18-22 year olds who present with a chief complaint of syncope than any other emergency physician on the planet. This ECG comes from a 19-year-old basic trainee who was running on the PT field and passed out. Per the guidelines above, a thorough history and physical exam were performed, and of note, the patient did have an uncle who had drowned swimming when he was a teenager. An ECG was obtained and is shown below:
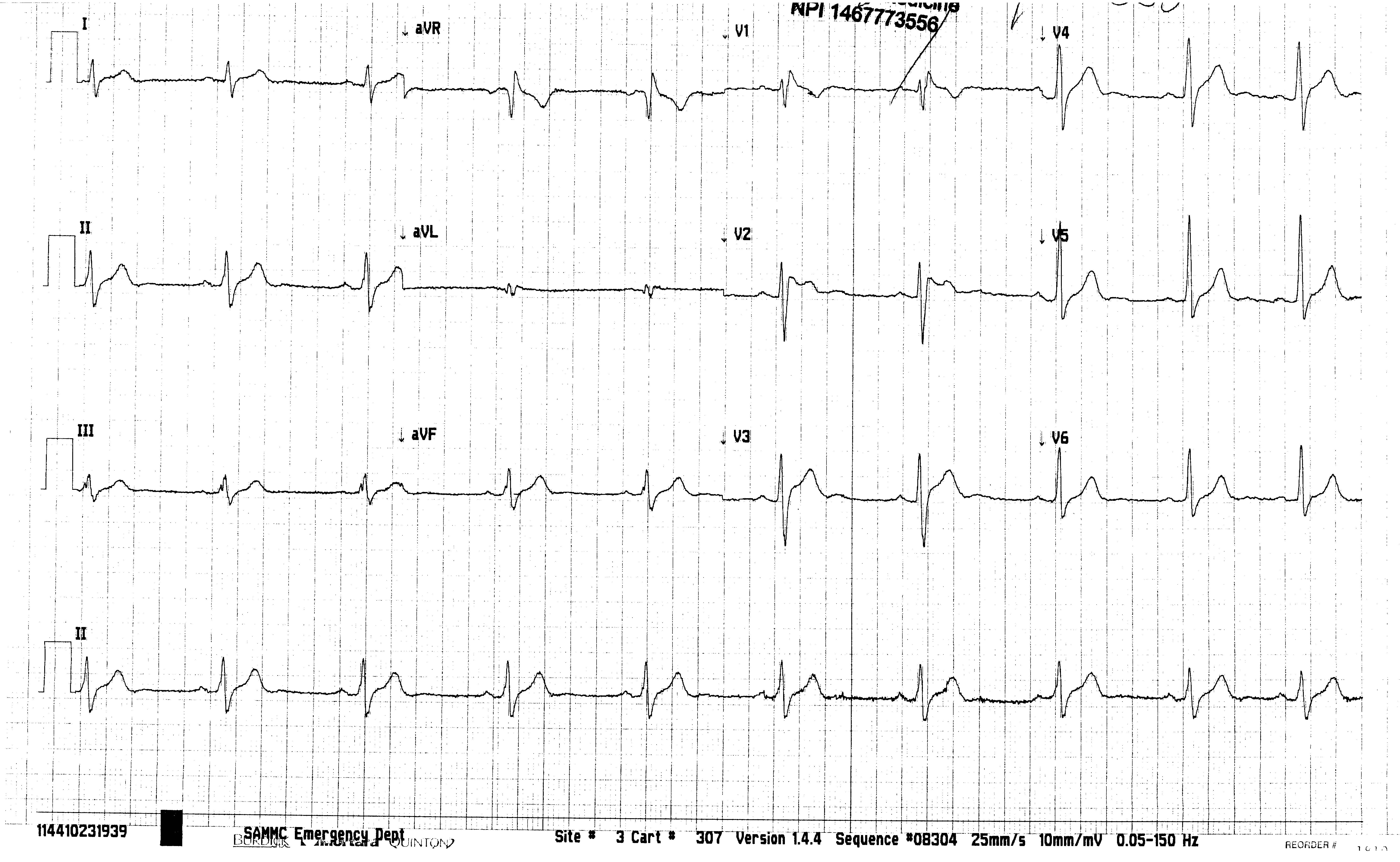
This ECG shows normal sinus rhythm and in V2 an RSR’ pattern with ST segment elevation in a “saddleback” morphology, consistent with Brugada type 2. ECG compliments of Dr. P. Kjell Ballard.
Case 2:
A 53-year-old African American female presents to the ER altered, agitated, and with a core temperature of 105. Her ECG is posted below:
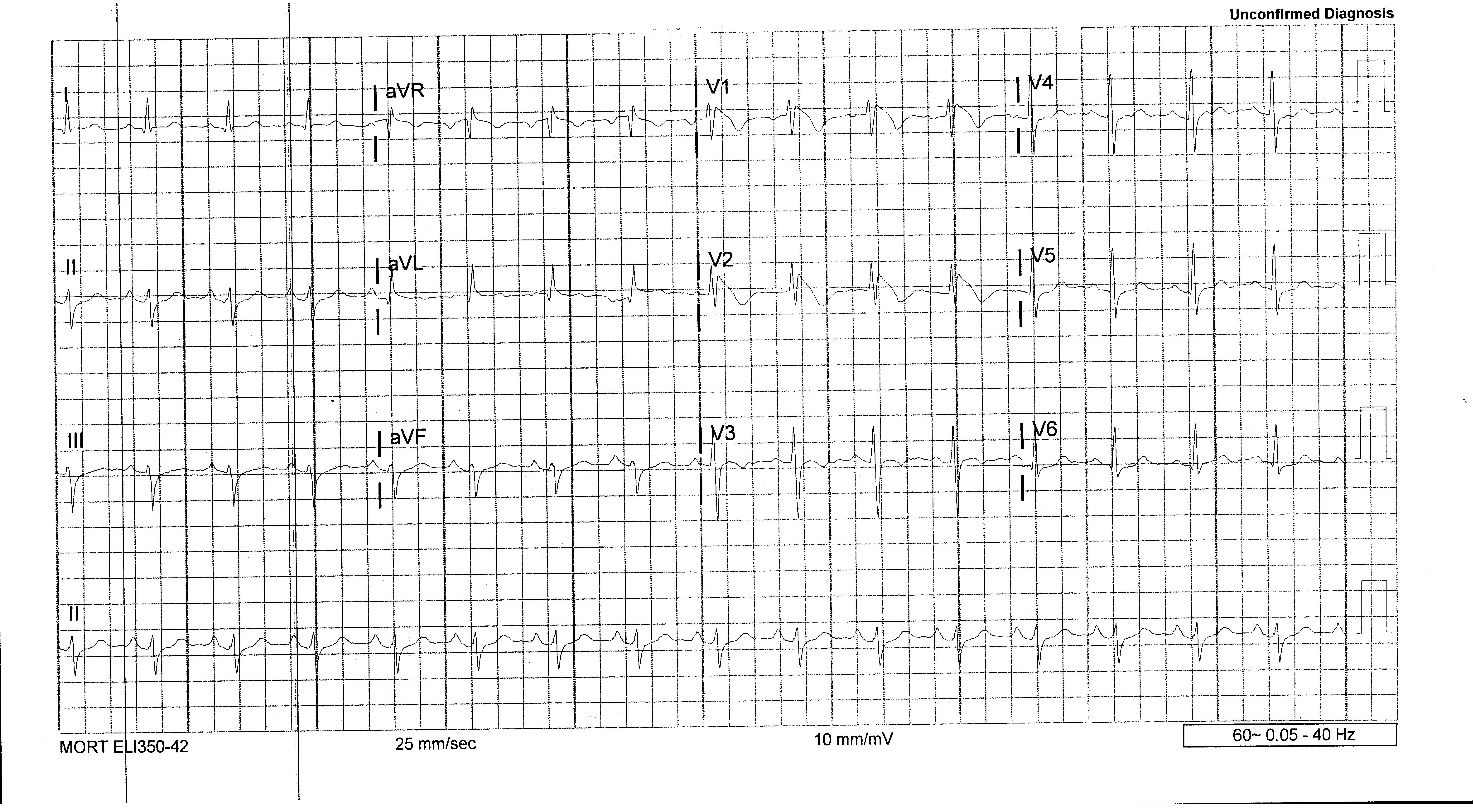
This ECG shows normal sinus rhythm with leads V1-V2 showing RSR’ pattern with ST segment elevation and steep T-wave inversions, consistent with Brugada type 1. ECG compliments of Dr. Garrett Hardy.
Interestingly, after antipyretics and IV Fluid, the ECG was repeated:
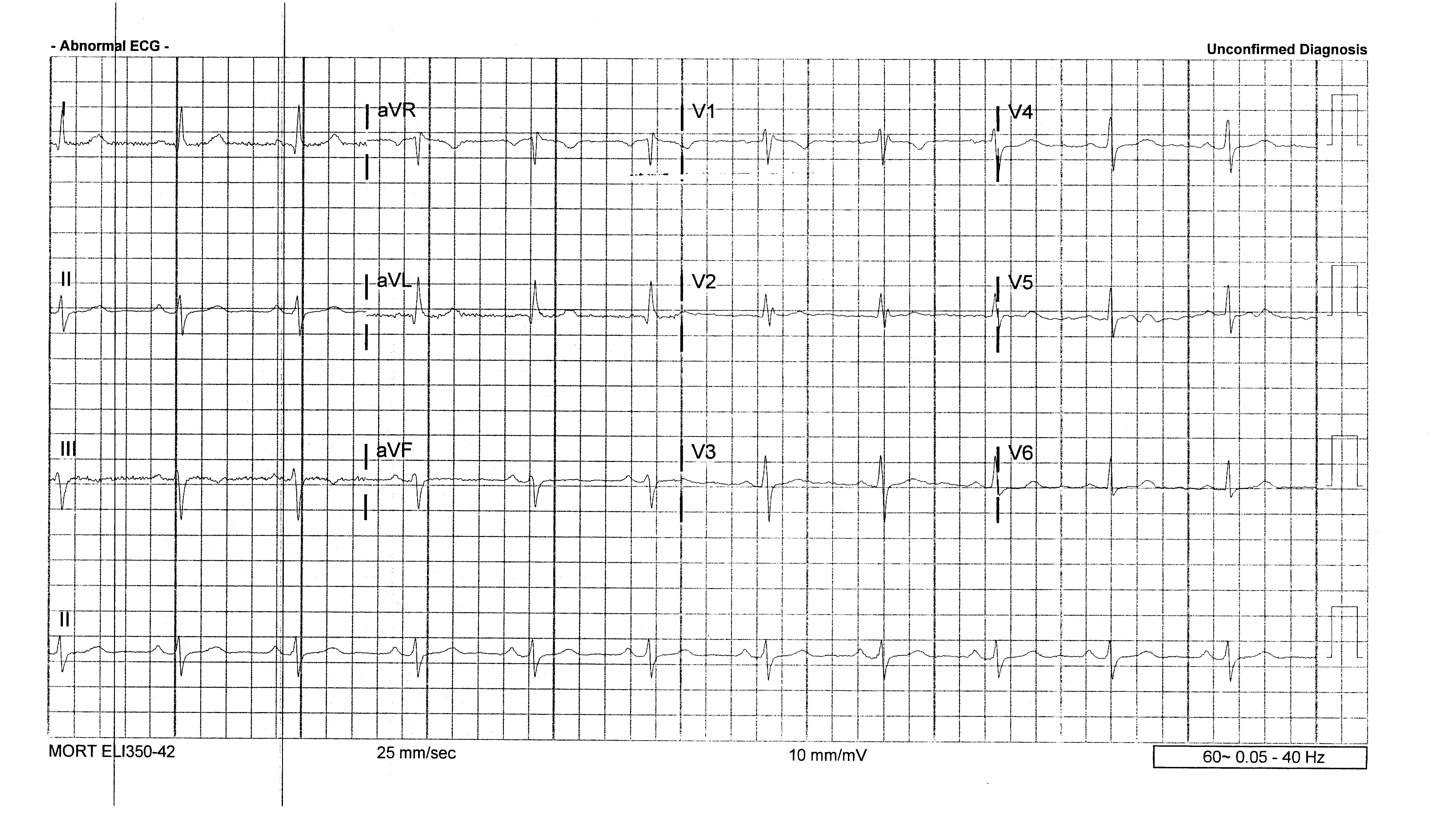
This ECG shows normal sinus rhythm, and the findings concerning for a Brugada pattern have now resolved. ECG compliments of Dr. Garrett Hardy.
What are these Brugada patterns, and why do they cause syncope?
In 1992, two brothers, Dr. Pedro Brugada and Dr. Josep Brugada, described a series of 8 patients who had all been resuscitated from sudden cardiac death and their ECGs all showed similar abnormalities [3]:

These ECGs, taken from [3], show ECG findings consistent with a type 1 Brugada pattern, although at this time, the “Brugada Pattern” did not exist at the time.
At the time that this paper was published, 1992, it was not yet known why these patients went into ventricular tachycardia. All of the patients did have a history of nonprodromal syncope. It was noted that stress seemed to induce arrhythmias, and one patient was admitted for a flu like illness. When this patient would get febrile, he would go into runs of ventricular tachycardia, several of which caused him to arrest requiring CPR and defibrillation. Additionally, several patients in this initial study had a strong family history of sudden death at a young age. The conclusion to this paper was that the current mechanism of arrhythmias is unknown and would require further testing [3].
Five years later, the Brugada brothers were back, this time with a larger study and some interesting results. They found 63 patients from 33 centers around the world with ECG findings similar to their initial 8 patients. All of these 63 patients had a history of nonprodromal syncope, and many had had an episode of aborted sudden cardiac death. Of the 63 patients that they identified, 35 of them had an implantable cardiac defibrillator placed, 15 were on pharmacotherapy with either beta blockers or amiodarone, and 13 received no treatment. What they found was that mortality in the group receiving no treatment was 31%, and mortality in the group with pharmacotherapy was 25%. However, in the group with an implanted defibrillator, mortality was 0%. They concluded that it was still unknown what was causing these patients to go into ventricular tachycardia, but pharmacotherapy did not seem to help. At this time, they recommend an implantable defibrillator to patients with a history of aborted sudden cardiac death and an ECG similar to the ones above [4].
Later that year, in 1998, a team of molecular biologists discovered that mutations in the cardiac sodium channel gene SCN5A was responsible for the ECG changes and the idiopathic runs of ventricular tachycardia. With the mutation identified, patients with a concerning history and ECG pattern consistent with those above can now be tested for this mutation and then diagnosed with Brugada Syndrome [5].
Currently, there are two types of Brugada Syndrome recognized, type 1 and type 2, and over 60 different responsible gene mutations have been identified. There were previously 3 types, but recently, types 2 and 3 have been combined into just type 2. Classic examples of them are shown below [6]:
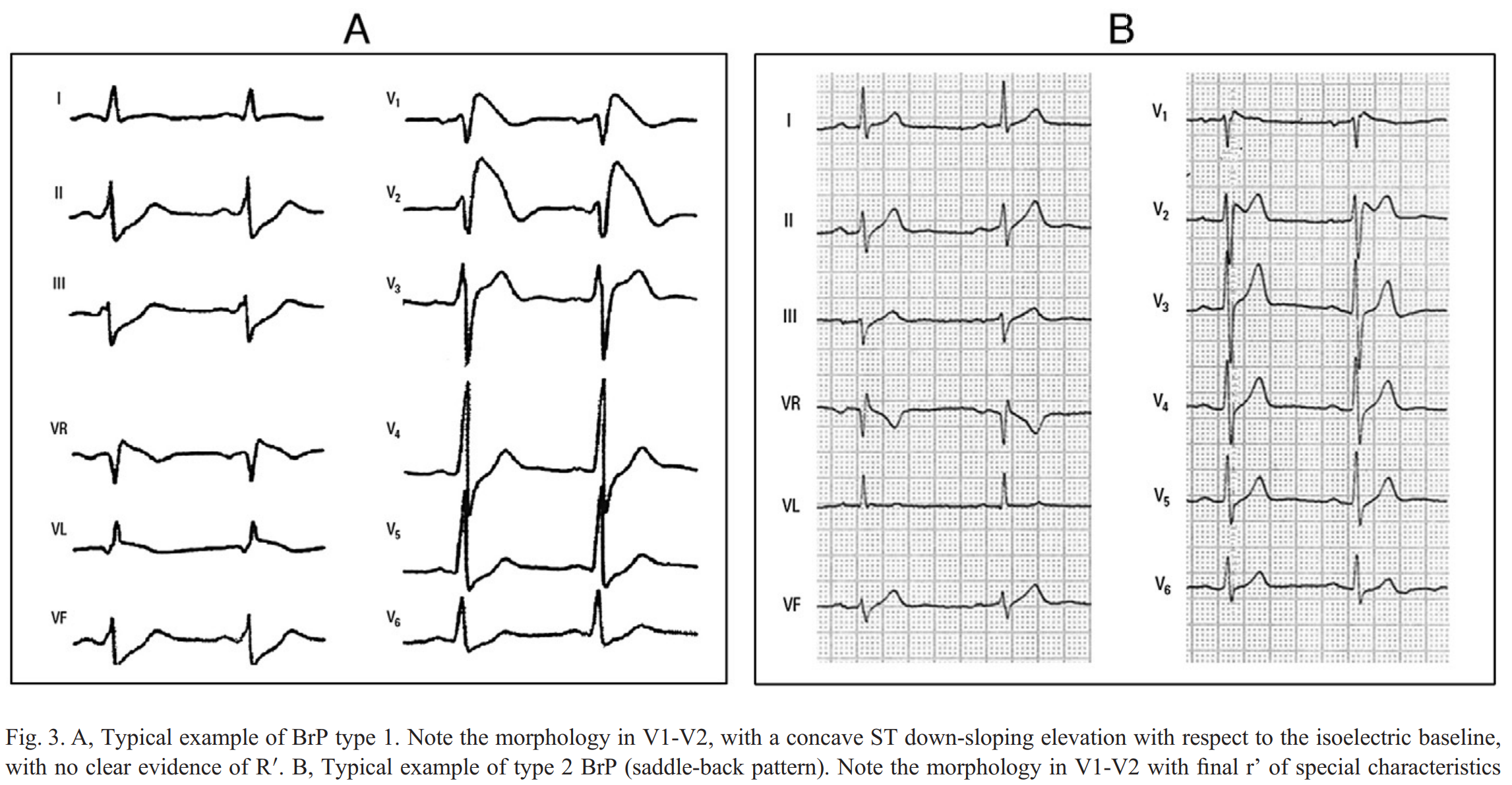
The formal diagnostic criteria are shown in the figure below, but remember, as emergency physicians, our goal is to identify patients at risk of Brugada Syndrome, not diagnose it. Try not to get bogged down in the many specific ECG criteria to formally diagnose it, let the cardiologists do that. It is important to note that other clinical conditions can mimic Brugada pattern on ECG and that diagnosis of Brugada Syndrome requires ECG criteria PLUS at least one clinical criteria:
- Documented ventricular fibrillation (VF) or polymorphic ventricular tachycardia (VT)
- Family history of sudden cardiac death at <45 years old
- Coved-type ECGs in family members
- Inducibility of VT with programmed electrical stimulation
- Syncope
- Nocturnal agonal respiration
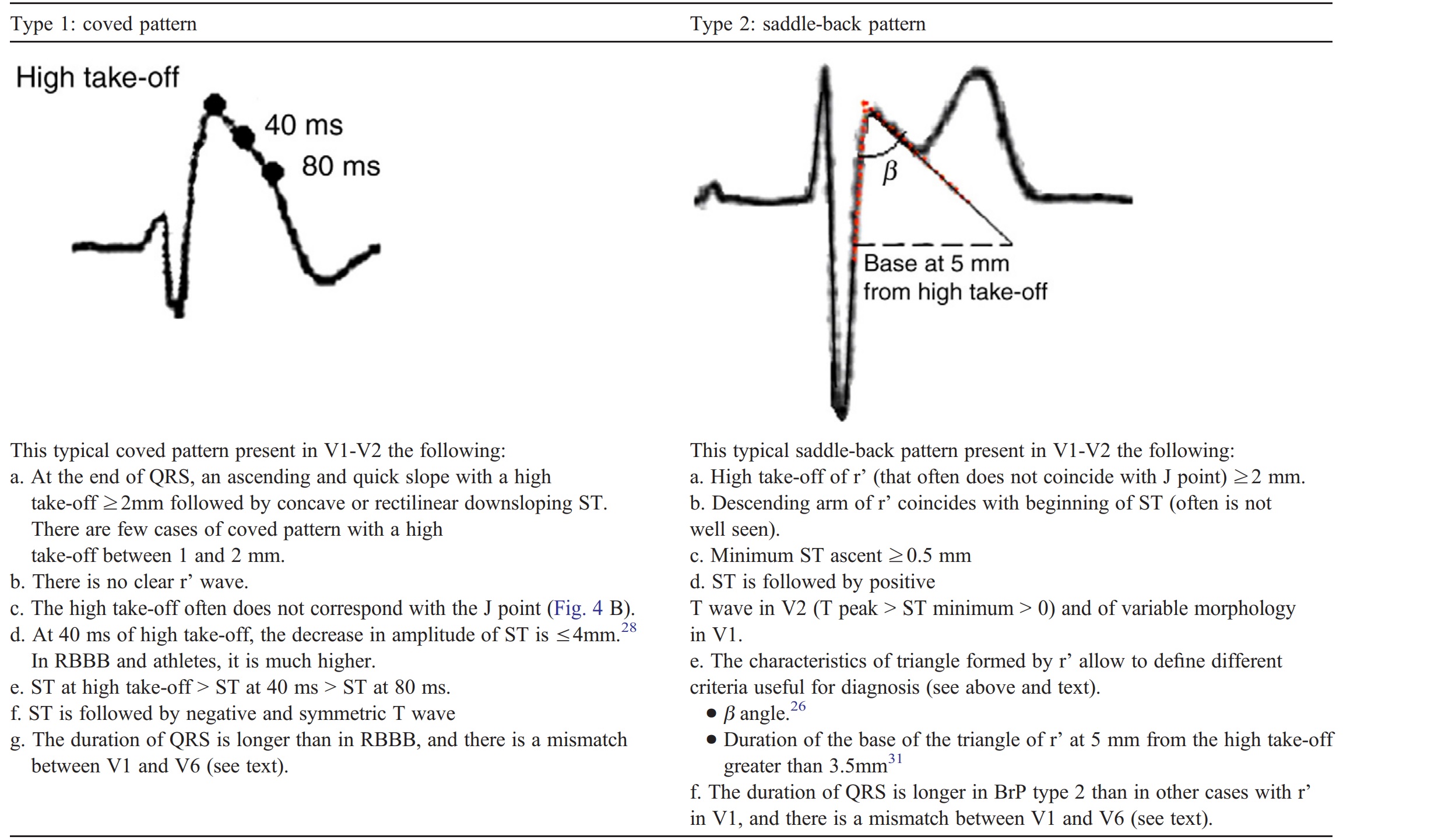 [6]
[6]
From the ED’s perspective, any patient with an ECG concerning for Brugada’s pattern and meets clinical criteria concerning for Brugada Syndrome should have consultation with Cardiology. Even asymptomatic, anyone with an ECG consistent with Brugada’s syndrome has an 8% risk of sudden death over the next 2 years [7]. Implantable defibrillator is the only treatment that has been shown to reduce mortality of Brugada syndrome [4].
Want More FOAM on Brugada?
- Life in the Fast Lane: Brugada Syndrome: https://litfl.com/brugada-syndrome-ecg-library/
- Smith’s ECG Blog does a great discussion on Brugada Syndrome: http://hqmeded-ecg.blogspot.com/search/label/brugada
References:
- Shen W-K, Sheldon RS, Benditt DG, Cohen MI, Forman DE, Goldberger ZD, Grubb BP, Hamdan MH, Krahn AD, Link MS, Olshansky B, Raj SR, Sandhu RK, Sorajja D, Sun BC, Yancy CW, 2017 ACC/AHA/HRS Guideline for the Evaluation and Management of Patients With Syncope, Journal of the American College of Cardiology (2017), doi: 10.1016/j.jacc.2017.03.003.
- Kann, Kristen. Mnemonic Expert.
- Brugada P, Brugada J. Right bundle branch block, persistent ST segment elevation and sudden cardiac death: a distinct clinical and electrocardiographic syndrome: a multicenter report. J Am Coll Cardiol. 1992;20: 1391–1396.
- Brugada J, Brugada R, Brugada P. Right bundle branch block and ST segment elevation in leads V1 through V3: a marker for sudden death in patients without demonstrable structural heart disease. Circulation. 1998; 97:457–460.
- Chen Q, Kirsch GE, Zhang D, Brugada R, Brugada J, Brugada P, Potenza D, Moya A, Borggrefe M, Breithardt G, Ortiz-Lo´pez R, Wang Z, Antzelevitch C, O’Brien RE, Schulze-Bahr E, Keating M, Towbin JA, Wang Q. Genetic basis and molecular mechanisms for idiopathic ventricular fibrillation. Nature. 1998;392:293–296.
- Bayés de Luna, A, Brugada, J, Baranchuk, A, et al. Current electrocardiographic criteria for diagnosis of Brugada pattern: a consensus report. Journal of Electrocardiology. 2012. 45: 433-442.
- Brugada, J, Brugada, R, and Brugada P. Determinants of Sudden Cardiac Death in Individuals With the Electrocardiographic Pattern of Brugada Syndrome and No Previous Cardiac Arrest. Circulation. 17 Nov 2003. 108:3092-3096.







1 thought on “ECG Pointers: Syncope and Brugada Syndrome”
Pingback: Syncope – kardiell – Mind palace of an ER doc