Author: Brit Long, MD (@long_brit, EM Attending Physician, San Antonio, TX) // Reviewed by: Alex Koyfman, MD (@EMHighAK, EM Attending Physician, UTSW / Parkland Memorial Hospital)
Welcome to EM@3AM, an emDocs series designed to foster your working knowledge by providing an expedited review of clinical basics. We’ll keep it short, while you keep that EM brain sharp.
A 39-year-old female presents with severe epigastric pain, nausea, and several episodes of non-bloody, non-bilious emesis. The pain is sharp and radiates to her back. She denies fevers, urinary changes, diarrhea, flank pain, chills, and vaginal bleeding/discharge, but she has no appetite.
On examination, she is tachycardic and tachypneic with diffuse abdominal tenderness, but afebrile. Her lipase returns at 1100 U/L.
What is your next step in evaluation and management?
Answer: Pancreatitis
Anatomy: The pancreas is a retroperitoneal organ with endocrine and exocrine function through production of insulin, glucagon, somatostatin and involvement in digestion.
Background: Pancreatitis is an acute or chronic process with inflammation of the pancreas and surrounding tissue. It may range from mild inflammation with no other organ involvement to necrosis and multiorgan involvement and failure.
Causes: The most common etiology is gallstones (up to 40%), followed by alcohol (30%), hypertriglyceridemia (5-10%), medications (statins, amiodarone, losartan, valproic acid, ATRA, sulfa, furosemide, thiazides, azathioprine, cisplatin, tetracyclines, pentamidine, didanosine, and others), posterior penetrating ulcer, autoimmune (lupus), trauma, postoperative, procedures (ERCP), infection (bacterial, viral, and parasitic), cystic fibrosis, ischemia, hyper Ca, hyperparathyroidism, tumor, scorpion sting, sphincter of Oddi dysfunction, and idiopathic (up to 20% of cases).
Diagnosis: Requires 2 of the following – characteristic abdominal pain, lipase > 3X the upper limit of normal (ULN), characteristic findings on ultrasound (US) or computed tomography (CT).
History:
- Pain most commonly in epigastric or left or right upper quadrant, which can radiate to the back. The pain is usually persistent and sharp.
- Patients may complain of abdominal distension and/or dyspnea.
- Ask about PO tolerance, alcohol intake, history of gallstones, envenomations/intoxications, medications, recent procedures or operations, trauma.
- Ask about other medical conditions, especially connective tissue disorders.
- Obtain family history concerning hypertriglyceridemia (typically autosomal dominant, though there are secondary forms).
Exam:
- Assess vital signs, abdomen, and volume status. Low grade fever is common.
- Patients may have epigastric or diffuse tenderness. Patients with no complications should demonstrate no findings of peritonitis.
- Dehydration with poor capillary refill and dry mucous membranes may be present from vomiting.
- If hemorrhagic pancreatitis is present, patients may demonstrate Cullen or Grey Turner signs.
- Cullen sign with ecchymosis around the periumbilical region is associated with intra-abdominal hemorrhage.
- Grey Turner sign with ecchymosis on the flank is associated with retroperitoneal hemorrhage.
- Patients may by tachypneic and/or hypoxemic.
- Jaundice suggests biliary obstruction and cholangitis.
Differential: Perforation, myocardial ischemia/ACS, hepatitis, aortic dissection, splenic pathology (infarction, rupture, aneurysm), PE, pericarditis/myocarditis, pyelonephritis, pneumonia, liver abscess, bowel obstruction, ingested foreign body, SMA syndrome, cholecystitis, cholangitis, retroperitoneal hematoma, urolithiasis, AAA, mesenteric ischemia, inflammatory bowel disease, appendicitis.
Evaluation:
- Obtain IV access and assess hemodynamic status.
- Obtain ECG, lipase, CBC, renal function, electrolytes, liver function. Lactate and triglycerides should be considered.
- Look for lipase > 3X ULN to diagnose pancreatitis.
- Amylase is not recommended, with less sensitivity and specificity compared to lipase.
- Lipase sensitivity and specificity approximate 90% for diagnosis of pancreatitis.
- Any pancreatic disorder, bowel obstruction, bowel ischemia, perforation, biliary disease, or renal failure can elevate lipase.
- Most conditions that elevate lipase will not reach 3X the ULN.
- Degree of lipase elevation is not associated with patient outcomes.
- Negative lipase cannot exclude chronic pancreatitis.
- Triglyceride level of at least 500 mg/dL (typically > 1000 mg/dL or 11.2 mM) suggests hypertriglyceridemia as the underlying etiology.
- Elevated bilirubin and alkaline phosphatase suggest biliary obstruction and cholangitis, especially in the toxic-appearing patient.
- US is recommended in patients to assess for gallstone pancreatitis. US may demonstrate a swollen pancreas or complication such as pseudocyst or abscess. The size of the common bile duct is the most important finding.
- CT with IV contrast can be diagnostic but is not absolutely necessary in patients with diagnosed pancreatitis via lipase and history/exam. It should be obtained in patients with organ failure, severe pain, SIRS criteria.
- CT is sensitivity and specific for diagnosis, however.
- The primary role for CT in pancreatitis is to assess for complications.
Management:
- Resuscitate to euvolemia and provide analgesia and antiemetics.
- Avoid over resuscitation, which is associated with abdominal compartment syndrome, ARDS, infection, pancreatic necrosis, and mortality. See this PulmCrit post for more.
- 2-4 L over the first day will typically return patients to euvolemia. Start with 250-500 mL/hr if not fluid depleted.
- LR may be reduce inflammation when compared to NS, which is associated with hyperchloremic metabolic acidosis with large volumes of fluid resuscitation.
- Treat underlying cause.
- For gallstone-related pancreatitis, patients will likely need cholecystectomy during admission. The American Gastroenterological Association recommends against routine ERCP in patients with biliary pancreatitis without cholangitis, but it is warranted in patients with cholangitis and may be indicated in those with choledocholithiasis.
- If hypertriglyceridemia is the cause, triglyceride level will need to be lowered, most commonly with insulin infusion/plasmapheresis and gemfibrozil. See this PulmCrit post for more on therapy.
- If medication-induced, stop the offending medication.
- For patients with hypercalcemia, provide IV fluids, bisphosphonate, and other calcium-reducing measures.
- Antibiotics are controversial and only warranted in patients with signs/sources of infection, necrosis, abscess, infected pseudocyst or peripancreatic fluid.
- Meropenem, imipenem-cilastatin, or ciprofloxacin + metronidazole.
- Diet: Early enteral nutrition may improve outcomes including intestinal function and reduce risk of infection and length of stay.
- May start oral diet immediately if PO tolerant, but start slow with small, low-fat meals.
- Monitor for electrolyte abnormalities including hypocalcemia, hypo- or hyperglycemia, and hypoalbuminemia.
- NG tube may be needed if SBO or ileus is present with severe abdominal dissension and other symptoms.
Risk Stratification: There are a variety of scoring systems available that can assist in predicting mortality in pancreatitis.
- Ranson’s criteria was originally developed in the 1970s and consists of 5 immediate lab values that are designed to be evaluated in the ED and 6 more assessed at 48 hours after admission in order to predict mortality (MDCalc).
- Scores of 2 or less are associated with low mortality, but scores 3 or greater have much greater risk (above 15%).

- The BISAP score was developed in 2008 and has several advantages in that there were 18000 patients utilized in derivation and validation and uses fewer variables (MDCalc).
- Patients with a score of 0 have < 1% risk of mortality. Mortality risk increases significant with scores 3 or greater.

- The APACHE II score was developed in 1985 and consists of 12 variables to predict mortality at 24 hours of ICU admission. GCS and renal function are weighted heavily in this score, and it requires PaO2 or A-a gradient (MDCalc).

- The CT Severity index evaluates imaging findings and severity of pancreatic inflammation/necrosis.
- The APACHE II and BISAP scores may be more useful in the ED setting, but these scores were not originally designed for the ED.
Complications: These are broken into local vs. systemic.
- Local: Pancreatic necrosis, pseudocyst, abscess, portal vein thrombosis, abdominal compartment syndrome, hemorrhage.
- Systemic: Hypo- or hyperglycemia, hypocalcemia, pleural effusion, cardiac dysfunction, renal failure, respiratory distress/failure progressing to ARDS, shock.
Disposition:
- Few studies evaluate use of risk scores to safely discharge patients with confirmed pancreatitis.
- Patients with gallstone-induced pancreatitis, severe pain, PO intolerance, end organ damage, and extremes of age should be admitted.
- Patients with pain controlled with oral medication, PO tolerance, normal vital signs, ability to follow up, no major comorbidities, and those without gallstone pancreatitis may be appropriate for discharge.
- If the patient is appropriate for discharge, follow up with GI must be confirmed.
Key Points:
- Pancreatitis is due to pancreatic inflammation.
- Diagnosis is with 2 out of the following 3: upper abdominal pain (clinical), serum lipase or amylase >3x ULN (laboratory), or imaging findings of pancreatic inflammation.
- RUQ US is recommended in the ED. CT is not necessary for diagnosis but can assess for complications.
- Provide analgesics, antiemetics, and IV fluids (LR). Avoid over resuscitation. Start oral diet if PO tolerant.
- Several risk scores are available for use. Discharge may be appropriate in select patients, but the majority of patients will require admission.
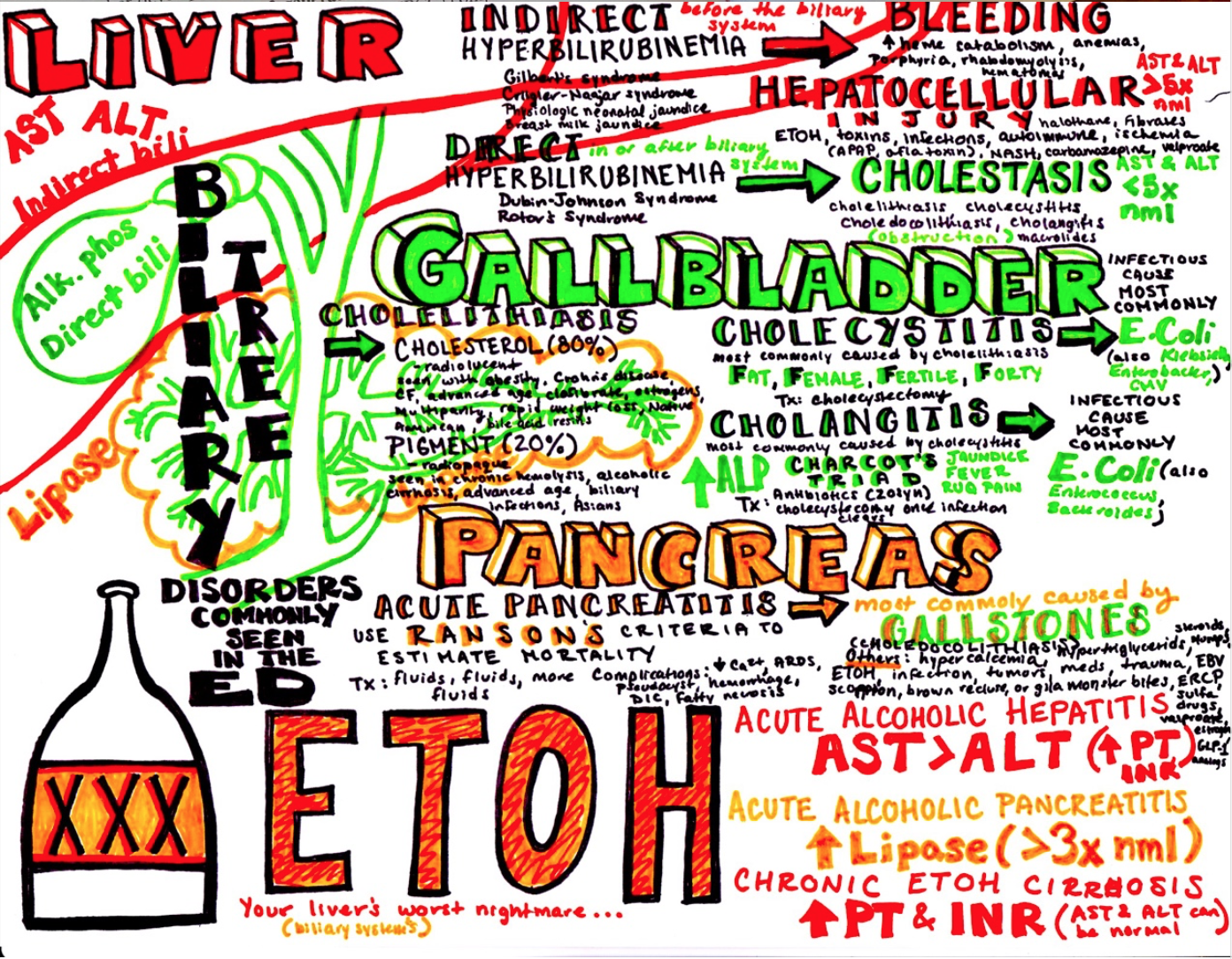
For more on pancreatitis, see these great pieces from Dr. Katy Hanson at www.hansonsanatomy.com


A healthy 40-year-old woman presents to the emergency department with a complaint of acute onset epigastric abdominal pain that started today. She describes it as sharp, radiating to the back, and severe in intensity. She also has associated nausea and anorexia. Laboratory evaluation reveals an alanine aminotransferase of 175 U/L, aspartate aminotransferase of 130 U/L, total bilirubin of 30 mmol/L, lipase of 750 U/L, a hematocrit of 44% and a white blood cell count of 15000/mcL. Which of the following is the next best step in caring for this patient?
A) Admission for IV fluids and pain control
B) Endoscopic retrograde cholangiopancreatography
C) Nasogastric tube insertion and bowel decompression
D) Surgical consult for emergent cholecystectomy
Answer: B
This patient has acute pancreatitis based on her symptoms and markedly elevated lipase. However, given elevated liver enzymes and bilirubin and the acute onset of pain, it is most likely pancreatitis secondary to biliary obstruction and will require endoscopic retrograde cholangiopancreatography for management. In this case, gallstone blockage of the common bile duct causes obstruction and decreased effluence of pancreatic enzymes as well as obstruction of the gall bladder, leading to pain, jaundice and laboratory abnormalities. This obstruction leads to activation of proteolytic enzymes within the pancreas causing local tissue breakdown. It is more common in females, and elevated liver function tests, especially alanine aminotransferase greater than 150 U/L, is highly predictive. These patients need specialist consult for endoscopic retrograde cholangiopancreatography to relieve the obstruction.

Admission for IV fluids and pain control (A) would be indicated for acute pancreatitis in the absence of biliary obstruction. Symptomatic treatment would not relieve the obstruction that is causing this patient’s symptoms. Nasogastric tube and decompression (C) is not necessary in most cases of pancreatitis, rather this would be the treatment for bowel obstruction. Bowel obstruction presents with abdominal pain and distention, and abdominal radiographs show air-fluid levels and dilated loops of small bowel. Emergent cholecystectomy (D) is not indicated for the treatment of gallstone pancreatitis. Cholecystectomy is indicated after recovery from pancreatitis.
Further Reading:
References/Further Reading
- Tenner S, Baillie J, DeWitt J, Vege SS. American College of Gastroenterology guideline: management of acute pancreatitis. The American journal of gastroenterology. 2013;108:1400-1415; 1416.
- Wang GJ, Gao CF, Wei D, Wang C, Ding SQ. Acute pancreatitis: etiology and common pathogenesis. World journal of gastroenterology. 2009;15:1427-1430.
- Cheng CL, Sherman S, Watkins JL, et al. Risk factors for post-ERCP pancreatitis: a prospective multicenter study. The American journal of gastroenterology. 2006;101:139-147.
- Gorelick FS. Alcohol and zymogen activation in the pancreatic acinar cell. 2003;27:305-310.
- Ewald N, Hardt PD, Kloer HU. Severe hypertriglyceridemia and pancreatitis: presentation and management. Current opinion in lipidology. 2009;20:497-504.
- Pandol SJ, Saluja AK, Imrie CW, Banks PA. Acute pancreatitis: bench to the bedside. 2007;132:1127-1151.
- IAP/APA evidence-based guidelines for the management of acute pancreatitis. Pancreatology: official journal of the International Association of Pancreatology (IAP) … [et al.]. 2013;13:e1-15.
- Zaheer A, Singh VK, Qureshi RO, Fishman EK. The revised Atlanta classification for acute pancreatitis: updates in imaging terminology and guidelines. Abdominal imaging. 2013;38:125-136.
- Rompianesi G, Hann A, Komolafe O, Pereira SP, Davidson BR, Gurusamy KS. Serum amylase and lipase and urinary trypsinogen and amylase for diagnosis of acute pancreatitis. The Cochrane database of systematic reviews. 2017;4:CD012010.
- Gumaste VV, Roditis N, Mehta D, Dave PB. Serum lipase levels in nonpancreatic abdominal pain versus acute pancreatitis. The American journal of gastroenterology. 1993;88:2051-2055.
- Chen YT, Chen CC, Wang SS, Chang FY, Lee SD. Rapid urinary trypsinogen-2 test strip in the diagnosis of acute pancreatitis. 2005;30:243-247.
- Gurusamy KS, Davidson C, Gluud C, Davidson BR. Early versus delayed laparoscopic cholecystectomy for people with acute cholecystitis. The Cochrane database of systematic reviews.2013:CD005440.
- Balthazar EJ, Robinson DL, Megibow AJ, Ranson JH. Acute pancreatitis: value of CT in establishing prognosis. 1990;174:331-336.
- Gardner TB, Vege SS, Pearson RK, Chari ST. Fluid resuscitation in acute pancreatitis. Clinical gastroenterology and hepatology: the official clinical practice journal of the American Gastroenterological Association. 2008;6:1070-1076.
- Brown A, Baillargeon JD, Hughes MD, Banks PA. Can fluid resuscitation prevent pancreatic necrosis in severe acute pancreatitis? Pancreatology: official journal of the International Association of Pancreatology (IAP) … [et al.]. 2002;2:104-107.
- Buxbaum JL, Quezada M, Da B, et al. Early Aggressive Hydration Hastens Clinical Improvement in Mild Acute Pancreatitis. The American journal of gastroenterology. 2017;112:797-803.
- Mao EQ, Tang YQ, Fei J, et al. Fluid therapy for severe acute pancreatitis in acute response stage. Chinese medical journal. 2009;122:169-173.
- Mao EQ, Fei J, Peng YB, Huang J, Tang YQ, Zhang SD. Rapid hemodilution is associated with increased sepsis and mortality among patients with severe acute pancreatitis. Chinese medical journal. 2010;123:1639-1644.
- Farkas J. The Myth of Large-Volume resuscitation in Acute Pancreatitis. Vol 2018. PULMCrit2014.
- de-Madaria E, Soler-Sala G, Sanchez-Paya J, et al. Influence of fluid therapy on the prognosis of acute pancreatitis: a prospective cohort study. The American journal of gastroenterology. 2011;106:1843-1850.
- Todd SR, Malinoski D, Muller PJ, Schreiber MA. Lactated Ringer’s is superior to normal saline in the resuscitation of uncontrolled hemorrhagic shock. The Journal of trauma. 2007;62:636-639.
- Wu BU, Hwang JQ, Gardner TH, et al. Lactated Ringer’s solution reduces systemic inflammation compared with saline in patients with acute pancreatitis. Clinical gastroenterology and hepatology: the official clinical practice journal of the American Gastroenterological Association. 2011;9:710-717 e711.
- Singh VK, Wu BU, Bollen TL, et al. Early systemic inflammatory response syndrome is associated with severe acute pancreatitis. Clinical gastroenterology and hepatology: the official clinical practice journal of the American Gastroenterological Association. 2009;7:1247-1251.
- Mofidi R, Duff MD, Wigmore SJ, Madhavan KK, Garden OJ, Parks RW. Association between early systemic inflammatory response, severity of multiorgan dysfunction and death in acute pancreatitis. The British journal of surgery. 2006;93:738-744.
- Forsmark CE, Baillie J. AGA Institute technical review on acute pancreatitis. 2007;132:2022-2044.
- Petrov MS, McIlroy K, Grayson L, Phillips AR, Windsor JA. Early nasogastric tube feeding versus nil per os in mild to moderate acute pancreatitis: a randomized controlled trial. Clinical nutrition (Edinburgh, Scotland). 2013;32:697-703.
- Li JY, Yu T, Chen GC, et al. Enteral nutrition within 48 hours of admission improves clinical outcomes of acute pancreatitis by reducing complications: a meta-analysis. PloS one. 2013;8:e64926.
- Ellery KM, Kumar S, Crandall W, Gariepy C. The Benefits of Early Oral Nutrition in Mild Acute Pancreatitis. The Journal of pediatrics. 2017;191:164-169.
- Ranson JH, Rifkind KM, Roses DF, Fink SD, Eng K, Spencer FC. Prognostic signs and the role of operative management in acute pancreatitis. Surgery, gynecology & obstetrics. 1974;139:69-81.
- Wu BU, Johannes RS, Sun X, Tabak Y, Conwell DL, Banks PA. The early prediction of mortality in acute pancreatitis: a large population-based study. 2008;57:1698-1703.
- Knaus WA, Draper EA, Wagner DP, Zimmerman JE. APACHE II: a severity of disease classification system. Critical care medicine. 1985;13:818-829.
- Sundararajan K, Schoeman T, Hughes L, Edwards S, Reddi B. Predictors and outcomes of acute pancreatitis in critically ill patients presenting to the emergency department of a tertiary referral centre in Australia. Emergency medicine Australasia: EMA. 2017;29:184-191.
- Di MY, Liu H, Yang ZY, Bonis PA, Tang JL, Lau J. Prediction Models of Mortality in Acute Pancreatitis in Adults: A Systematic Review. Annals of internal medicine. 2016;165:482-490.






1 thought on “EM@3AM: Pancreatitis”
Pingback: Quiz 62, February 14th 2020